Abstract
Purpose
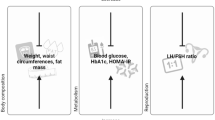
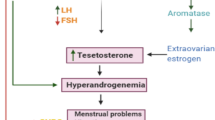
Polycystic ovary syndrome (PCOS) is a common endocrine disorder among reproductive-age women. Insulin resistance and dyslipidemia are linked to PCOS. l-Carnitine supplementation as a management strategy for women with PCOS has been proposed. The effect of l-carnitine supplementation on insulin resistance, sex hormone-binding globulin (SHBG) and lipid profile in overweight/obese women with PCOS was investigated.
Methods
This randomized, double-blind, controlled clinical trial, was conducted on 62overweight/obese women with PCOS. Participants were randomly assigned into two groups to receive 1000 mg/day l-carnitine or placebo (1000 mg starch) for 12 weeks.
Results
l-Carnitine supplementation compared to the placebo showed a significant improvement in insulin [− 0.7 (− 7.3 to 4.0) vs. 0.7 (− 3.0 to 5.2); P = 0.001], homeostatic model assessment for insulin resistance [− 0.4 (− 1.7 to 1.1) vs. 0.0 (− 0.7 to 1.3); P = 0.002], quantitative insulin sensitivity check index (+ 0.01 ± 0.02 vs. − 0.01 ± 0.01; P = 0.02) and a non-significant change toward improvement in SHBG (+ 11.5 ± 40.2 vs. − 3.2 ± 40.2; P = 0.2). However, there was no significant differences between the two groups in serum levels of fasting plasma glucose, total cholesterol, triglyceride, low density lipoprotein-cholesterol and high density lipoprotein cholesterol (P > 0.05).
Conclusion
12-week l-carnitine supplementation in overweight or obese women with PCOS ameliorate insulin resistance, but has no effect on SHBG and lipid profile. Studies with higher dosages and duration of l-carnitine intake are required. The trial was registered on 30 December 2019 at Iranian Registry of Clinical Trials IRCT20191016045131N1.
Trial registration
Registered on 30th December 2019 at Iranian Registry of Clinical Trials (IRCT20191016045131N1).

Similar content being viewed by others
Abbreviations
- Acyl-CoA:
-
Acyl-coenzyme A
- AES:
-
Androgen Excess Society
- ASRM:
-
American Society for Reproductive Medicine
- BMI:
-
Body mass index
- CVD:
-
Cardiovascular disease
- DHEA:
-
Dehydroepiandrosterone
- ESHRE:
-
European Society of Human Reproduction and Embryology
- FAI:
-
Free androgen index
- FPG:
-
Fasting plasma glucose
- HC:
-
Hip circumference
- HDL-c:
-
High density lipoprotein-cholesterol
- HOMA-IR:
-
Homeostatic model assessment for insulin resistance
- IPAQ:
-
International physical activity questionnaire
- LDL-c:
-
Low-density lipoprotein-cholesterol
- LH:
-
Luteinizing hormone
- MET-h:
-
Metabolic equivalent task hours
- NAFLD:
-
Nonalcoholic fatty liver disease
- NIH:
-
National Institutes of Health
- PCOS:
-
Polycystic ovary syndrome
- QUICKI:
-
Quantitative insulin sensitivity check index
- SHBG:
-
Sex hormone-binding globulin
- T2DM:
-
Type 2 diabetes mellitus
- TC:
-
Total cholesterol
- TG:
-
Triglyceride
- VLDL:
-
Very low-density lipoprotein
- WC:
-
Waist circumference
References
Condorelli RA, Calogero AE, Di Mauro M, Mongioi’ LM, Cannarella R, Rosta G et al (2018) Androgen excess and metabolic disorders in women with PCOS: beyond the body mass index. J Endocrinol Invest 41(4):383–388
Azziz R, Carmina E, Chen Z, Dunaif A, Laven JSE, Legro RS et al (2016) Polycystic ovary syndrome. Nat Rev Dis Primers 2:16057
Harris HR, Terry KL (2016) Polycystic ovary syndrome and risk of endometrial, ovarian, and breast cancer: a systematic review. Fertil Res Pract 2:14
Knochenhauer ES, Key TJ, Kahsar-Miller M, Waggoner W, Boots LR, Azziz R (1998) Prevalence of the polycystic ovary syndrome in unselected black and white women of the Southeastern United States: a prospective study. J Clin Endocrinol Metab 83(9):3078–3082
Kauffman RP, Baker VM, DiMarino P, Gimpel T, Castracane VD (2002) Polycystic ovarian syndrome and insulin resistance in white and Mexican American women: a comparison of two distinct populations. Am J Obstet Gynecol 187(5):1362–1369
Amato MC, Galluzzo A, Finocchiaro S, Criscimanna A, Giordano C (2008) The evaluation of metabolic parameters and insulin sensitivity for a more robust diagnosis of the polycystic ovary syndrome. Clin Endocrinol (Oxf) 69(1):52–60
Azziz R, Carmina E, Dewailly D, Diamanti-Kandarakis E, Escobar-Morreale HF, Futterweit W et al (2009) The Androgen Excess and PCOS Society criteria for the polycystic ovary syndrome: the complete task force report. Fertil Steril 91(2):456–488
Teede HJ, Misso ML, Costello MF, Dokras A, Laven J, Moran L et al (2018) Recommendations from the international evidence-based guideline for the assessment and management of polycystic ovary syndrome. Hum Reprod 110(3):364–379
Carmina E (2004) Diagnosis of Polycystic ovary syndrome: from NIH criteria to ESHRE-ASRM guidelines. Minerva Ginecol 56(1):1–6
Rotterdam ESHRE/ASRM-Sponsored PCOS Consensus Workshop Group (2004) Revised 2003 consensus on diagnostic criteria and long-term health risks related to polycystic ovary syndrome. Fertil Steril 81(1):19–25
Wild RA, Rizzo M, Clifton S, Carmina E (2011) Lipid levels in polycystic ovary syndrome: systematic review and meta-analysis. Fertil Steril 95(3):1073–1079
Goodarzi MO, Dumesic DA, Chazenbalk G, Azziz R (2011) Polycystic ovary syndrome: etiology, pathogenesis and diagnosis. Nat Rev Endocrinol 7(4):219–231
Barber TM, Dimitriadis GK, Andreou A, Franks S (2016) Polycystic ovary syndrome: insight into pathogenesis and a common association with insulin resistance. Clin Med (Lond) 16(3):262–266
Goodman NF, Cobin RH, Futterweit W, Glueck JS, Legro RS, Carmina E (2015) American association of clinical endocrinologists, American college of endocrinology, and androgen excess and pcos society disease state clinical review: guide to the best practices in the evaluation and treatment of polycystic ovary syndrome—Part 1. Endocr Pract 21(11):1291–1300
Steiber A, Kerner J, Hoppel CL (2004) Carnitine: a nutritional, biosynthetic, and functional perspective. Mol Aspects Med 25(5–6):455–473
El-Hattab AW, Scaglia F (2015) Disorders of carnitine biosynthesis and transport. Mol Genet Metab 116(3):107–112
Stephens FB, Constantin-teodosiu D, Greenhaff PL (2007) New insights concerning the role of carnitine in the regulation of fuel metabolism in skeletal muscle. J Physiol 581(Pt 2):431–444
Evans AM, Fornasini G (2003) Pharmacokinetics of L-carnitine. Clin Pharmacokinet 42(11):941–967
Demarquoy C, Demarquoy J (2019) Autism and carnitine: a possible link. World J Biol Chem 10(1):7–16
Ruggenenti P, Cattaneo D, Loriga G, Ledda F, Motterlini N, Gherardi G et al (2009) Ameliorating hypertension and insulin resistance in subjects at increased cardiovascular risk: effects of acetyl-l-carnitine therapy. Hypertension 54(3):567–574
Power RA, Hulver MW, Zhang JY, Dubois J, Marchand RM, Ilkayeva O et al (2007) Carnitine revisited: potential use as adjunctive treatment in diabetes. Diabetologia 50(4):824–832
Ferrari R, Merli E, Cicchitelli G, Mele D, Fucili A, Ceconi C (2004) Therapeutic effects of L-carnitine and propionyl-L-carnitine on cardiovascular diseases: a review. Ann N Y Acad Sci 1033:79–91
Barzegar A, Alipour B, Panahi F, Karamzad N (2013) Effect of L-Carnitine supplementation on serum adipokines (Leptin and Visfatin) levels in obese type II diabetes mellitus women with Hypocaloric diet. Life Sci J 10:359–365
Malek Mahdavi A, Mahdavi R, Kolahi S, Zemestani M, Vatankhah AM (2015) L-Carnitine supplementation improved clinical status without changing oxidative stress and lipid profile in women with knee osteoarthritis. Nutr Res 35(8):707–715
Askarpour M, Hadi A, Miraghajani M, Symonds ME, Sheikhi A, Ghaedi E (2020) Beneficial effects of L-carnitine supplementation for weight management in overweight and obese adults: an updated systematic review and dose-response meta-analysis of randomized controlled trials. Pharmacol Res 151:104554
Ringseis R, Keller J, Eder K (2012) Role of carnitine in the regulation of glucose homeostasis and insulin sensitivity: evidence from in vivo and in vitro studies with carnitine supplementation and carnitine deficiency. Eur J Nutr 51(1):1–18
Emami Naini A, Moradi M, Mortazavi M, Amini Harandi A, Hadizadeh M, Shirani F et al (2012) Effects of oral L-carnitine supplementation on lipid profile, anemia, and quality of life in chronic renal disease patients under hemodialysis: a randomized, double-blinded, placebo-controlled trial. J Nutr Metab. https://doi.org/10.1155/2012/510483
Zayed EA, AinShoka AA, El Shazly KA, Abd El Latif HA (2018) Improvement of insulin resistance via increase of GLUT4 and PPARγ in metabolic syndrome-induced rats treated with omega-3 fatty acid or l-carnitine. J Biochem Mol Toxicol 32(11):e22218
Agarwal A, Sengupta P, Durairajanayagam D (2018) Role of L-carnitine in female infertility. Reprod Biol Endocrinol 16(1):5
Dunning KR, Robker RL (2012) Promoting lipid utilization with l-carnitine to improve oocyte quality. Anim Reprod Sci 134(1–2):69–75
Ghanbarzadeh S, Garjani A, Ziaee M, Khorrami A (2014) CoQ10 and L-Carnitine attenuate the effect of high LDL and oxidized LDL on spermatogenesis in male rats. Drug Res (Stuttg) 64(10):510–515
Zhu J, Chen Z, Feng W, Long S, Mo ZC (2019) Sex hormone-binding globulin and polycystic ovary syndrome. Clin Chim Acta 499:142–148
Hammond GL, Wu TS, Simard M (2012) Evolving utility of sex hormone-binding globulin measurements in clinical medicine. Curr Opin Endocrinol Diabetes Obes 19(3):183–189
Fenkci SM, Fenkci V, Oztekin O, Rota S, Karagenc N (2008) Serum total L-carnitine levels in non-obese women with polycystic ovary syndrome. Hum Reprod 23(7):1602–1606
Ismail AM, Hamed AH, Saso S, Thabet HH (2014) Adding L-carnitine to clomiphene resistant PCOS women improves the quality of ovulation and the pregnancy rate. A randomized clinical trial. Eur J Obstet Gynecol Reprod Biol 180:148–152
Samimi M, Jamilian M, Ebrahimi FA, Rahimi M, Tajbakhsh B, Asemi Z (2016) Oral carnitine supplementation reduces body weight and insulin resistance in women with polycystic ovary syndrome: a randomized, double-blind, placebo-controlled trial. Clin Endocrinol (Oxf) 84(6):851–857
Maleki V, Jafari-Vayghan H, Kashani A, Moradi F, Vajdi M, Kheirouri S et al (2019) Potential roles of carnitine in patients with polycystic ovary syndrome: a systematic review. Gynecol Endocrinol 35(6):463–469
Salehpour S, Nazari L, Hoseini S, Moghaddam PB, Gachkar L (2019) Effects of L-carnitine on polycystic ovary syndrome. JBRA Assist Reprod 23(4):392–395
Huang H, Song L, Zhang H, Zhang H, Zhang J, Zhao W (2014) Influence of L-carnitine supplementation on serum lipid profile in hemodialysis patients: a systematic review and meta-analysis. Kidney Blood Press Res 38(1):31–41
Lee BJ, Lin JS, Lin YC, Lin PT (2016) Effects of L-carnitine supplementation on lipid profiles in patients with coronary artery disease. Lipids Health Dis 15:107
Malaguarnera M, Vacante M, Avitabile T, Malaguarnera M, Cammalleri L, Motta M (2009) L-Carnitine supplementation reduces oxidized LDL cholesterol in patients with diabetes. Am J Clin Nutr 89(1):71–76
Askarpour M, Hadi A, Symonds ME, Miraghajani M, Sadeghi O, Sheikhi A et al (2019) Efficacy of L-carnitine supplementation for management of blood lipids: a systematic review and dose-response meta-analysis of randomized controlled trials. Nutr Metab Cardiovasc Dis 29(11):1151–1167
Montjean D, Entezami F, Lichtblau I, Belloc S, Gurgan T, Menezo Y (2012) Carnitine content in the follicular fluid and expression of the enzymes involved in beta oxidation in oocytes and cumulus cells. J Assist Reprod Genet 29(11):1221–1225
Longo N, Frigeni M (1863) Pasquali M (2016) Carnitine transport and fatty acid oxidation. Biochim Biophys Acta 10:2422–2435
Sirtori CR, Calabresi L, Ferrara S, Pazzucconi F, Bondioli A, Baldassarre D et al (2000) L-carnitine reduces plasma lipoprotein(a) levels in patients with hyper Lp(a). Nutr Metab Cardiovasc Dis 10(5):247–251
Hoppel C (2003) The role of carnitine in normal and altered fatty acid metabolism. Am J Kidney Dis 41(Suppl4):S4–S12
Acknowledgements
We acknowledge the contribution of the co-researchers. We also thank the participants for their cooperation throughout recruitment and data collection processes.
Funding
Shahid Sadoughi University of Medical Sciences and Health Services, Yazd, Iran supported this study. This was a financial support for student thesis process including laboratory works, and provide kits as well as supplements.
Author information
Authors and Affiliations
Contributions
FP and MH: conducted the study; AG: provided material and technical support, AS: interpreted the finding and drafted the manuscript; MH and AN: critically revised the manuscript; HF: carried out the statistical analysis; and MH: supervised the study. The final version of the manuscript was approved by all authors.
Corresponding author
Ethics declarations
Conflict of interests
The authors have declared no competing interests.
Ethical approval
The research council of Nutrition and Food Security Research Center, Shahid Sadoughi University of Medical Sciences and Health Services approved the study protocol. The ethical committee of Shahid Sadoughi University of Medical Sciences and Health Services in Yazd approved the written informed consent (code number: IR.SSU.SPH.REC.1397.014).
Informed consent
Written informed consent was obtained from all participants before the data collection.
Consent for publication
Not applicable.
Data availability
The data and materials of the current study is available from the corresponding author on reasonable request.
Rights and permissions
About this article
Cite this article
Sangouni, A.A., Pakravanfar, F., Ghadiri-Anari, A. et al. The effect of l-carnitine supplementation on insulin resistance, sex hormone-binding globulin and lipid profile in overweight/obese women with polycystic ovary syndrome: a randomized clinical trial. Eur J Nutr 61, 1199–1207 (2022). https://doi.org/10.1007/s00394-021-02659-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00394-021-02659-0