Abstract
Background
Device landing zone (DLZ) calcification is an important determinant of procedural success in transcatheter aortic valve implantation (TAVI).
Objective
To evaluate the impact of DLZ calcification on procedural outcome with different types of transcatheter heart valves (THVs).
Methods
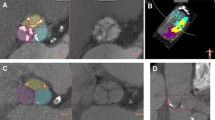
Aortic valve calcium density (AVCdens) was determined by non-contrast-enhanced computed tomography in 1232 patients undergoing transfemoral TAVI. We stratified the outcome data according to the extent of AVCdens (mild, moderate, severe) and compared balloon-expandable (BE) with self-expanding (SE) THV. Moreover, THVs were subdivided according to their radial force (BE: high; SEmod: moderate; SElow: low).
Results
With BE THV, PVR ≥2° (2.1 vs. 7.9%; p < 0.001), post-dilatation (12.3 vs. 36.6%; p < 0.001), malpositioning (8.4 vs. 13.0%; p = 0.01), device embolization (0.4 vs. 2.6%; p = 0.004), and the need for a second valve (1.2 vs. 3.6%; p = 0.01) were less frequent than with SE devices, but mean transaortic gradients at discharge were higher [12.0 mmHg (8.0–15.0) vs. 9.0 mmHg (6.0–11.0); p < 0.001], and aortic root injury was more frequent (2.7 vs. 0.8%; p = 0.01). In cases of severe calcification, differences between BE and SE THV regarding PVR, post-dilatation, and hemodynamics were mostly pronounced, followed by patients with moderate AVCdens. In cases with low AVCdens, the best outcomes with respect to PVR, pacemaker implantation, and hemodynamics were achieved with SElow THV.
Conclusions
In severe and moderate DLZ calcification, BE devices may have advantages, whereas in mild DLZ calcification, SElow THV showed the most favorable profile.

Similar content being viewed by others
References
Leon MB, Smith CR, Mack MJ et al (2016) Transcatheter or surgical aortic-valve replacement in intermediate-risk patients. N Engl J Med 374(17):1609–1620. doi:10.1056/NEJMoa1514616
Mollmann H, Bestehorn K, Bestehorn M et al (2016) 2016 In-hospital outcome of transcatheter vs. surgical aortic valve replacement in patients with aortic valve stenosis: complete dataset of patients treated in 2013in Germany. Clin Res Cardiol 105(6):553–559. doi:10.1007/s00392-016-0962-4
Reardon MJ, Van Mieghem NM, Popma JJ et al (2017) Surgical or transcatheter aortic-valve replacement in intermediate-risk patients. N Engl J Med 376(14):1321–1331. doi:10.1056/NEJMoa1700456
Buellesfeld L, Stortecky S, Heg D et al (2014) Extent and distribution of calcification of both the aortic annulus and the left ventricular outflow tract predict aortic regurgitation after transcatheter aortic valve replacement. EuroIntervention 10(6):732–738. doi:10.4244/EIJV10I6A126
Hansson NC, Norgaard BL, Barbanti M et al (2015) The impact of calcium volume and distribution in aortic root injury related to balloon-expandable transcatheter aortic valve replacement. J Cardiovasc Comput Tomogr 9(5):382–392. doi:10.1016/j.jcct.2015.04.002
John D, Buellesfeld L, Yuecel S et al (2010) Correlation of Device landing zone calcification and acute procedural success in patients undergoing transcatheter aortic valve implantations with the self-expanding CoreValve prosthesis. JACC Cardiovasc Interv 3(2):233–243. doi:10.1016/j.jcin.2009.11.015
Leber AW, Kasel M, Ischinger T et al (2013) Aortic valve calcium score as a predictor for outcome after TAVI using the CoreValve revalving system. Int J Cardiol 166(3):652–657. doi:10.1016/j.ijcard.2011.11.091
Seiffert M, Fujita B, Avanesov M et al (2016) Device landing zone calcification and its impact on residual regurgitation after transcatheter aortic valve implantation with different devices. Eur Heart J Cardiovasc Imaging 17(5):576–584. doi:10.1093/ehjci/jev174
Vahanian A, Alfieri O, Andreotti F et al (2012) Guidelines on the management of valvular heart disease (version 2012). Eur Heart J 33(19):2451–2496. doi:10.1093/eurheartj/ehs109
Kim WK, Praz F, Blumenstein J et al (2016) Transfemoral aortic valve implantation of Edwards SAPIEN 3 without predilatation. Catheter Cardiovasc Interv. doi:10.1002/ccd.26464
Mollmann H, Kim WK, Kempfert J et al (2014) Transfemoral aortic valve implantation of Edwards SAPIEN XT without predilatation is feasible. Clin Cardiol 37(11):667–671. doi:10.1002/clc.22318
Kim WK, Liebetrau C, Renker M et al (2017) Transfemoral aortic valve implantation using a self-expanding transcatheter heart valve without pre-dilation. Int J Cardiol. doi:10.1016/j.ijcard.2017.05.092
Piazza N, Martucci G, Lachapelle K et al (2014) First-in-human experience with the Medtronic CoreValve Evolut R. EuroIntervention 9(11):1260–1263. doi:10.4244/EIJV9I11A215
Manoharan G, Spence MS, Rodes-Cabau J et al (2012) St Jude Medical Portico valve. EuroIntervention 8(Suppl Q):Q97–Q101. doi:10.4244/EIJV8SQA18
Opolski MP, Kim WK, Liebetrau C et al (2015) Diagnostic accuracy of computed tomography angiography for the detection of coronary artery disease in patients referred for transcatheter aortic valve implantation. Clin Res Cardiol 104(6):471–480. doi:10.1007/s00392-014-0806-z
Kim WK, Meyer A, Mollmann H et al (2016) Cyclic changes in area- and perimeter-derived effective dimensions of the aortic annulus measured with multislice computed tomography and comparison with metric intraoperative sizing. Clin Res Cardiol 105(7):622–629. doi:10.1007/s00392-016-0971-3
Clavel MA, Pibarot P, Messika-Zeitoun D et al (2014) Impact of aortic valve calcification, as measured by MDCT, on survival in patients with aortic stenosis: results of an international registry study. J Am Coll Cardiol 64(12):1202–1213. doi:10.1016/j.jacc.2014.05.066
Zamorano JL, Badano LP, Bruce C et al (2011) EAE/ASE recommendations for the use of echocardiography in new transcatheter interventions for valvular heart disease. J Am Soc Echocardiogr 24(9):937–965. doi:10.1016/j.echo.2011.07.003
Athappan G, Patvardhan E, Tuzcu EM et al (2013) Incidence, predictors, and outcomes of aortic regurgitation after transcatheter aortic valve replacement: meta-analysis and systematic review of literature. J Am Coll Cardiol 61(15):1585–1595. doi:10.1016/j.jacc.2013.01.047
Abdel-Wahab M, Mehilli J, Frerker C et al (2014) Comparison of balloon-expandable vs self-expandable valves in patients undergoing transcatheter aortic valve replacement: the CHOICE randomized clinical trial. JAMA 311(15):1503–1514. doi:10.1001/jama.2014.3316
Jilaihawi H, Makkar RR, Kashif M et al (2014) A revised methodology for aortic-valvar complex calcium quantification for transcatheter aortic valve implantation. Eur Heart J Cardiovasc Imaging 15(12):1324–1332. doi:10.1093/ehjci/jeu162
Kodali SK, Williams MR, Smith CR et al (2012) Two-year outcomes after transcatheter or surgical aortic-valve replacement. N Engl J Med 366(18):1686–1695. doi:10.1056/NEJMoa1200384
Moat NE, Ludman P, de Belder MA et al (2011) Long-term outcomes after transcatheter aortic valve implantation in high-risk patients with severe aortic stenosis: the U.K. TAVI (United Kingdom Transcatheter Aortic Valve Implantation) Registry. J Am Coll Cardiol 58(20):2130–2138. doi:10.1016/j.jacc.2011.08.050
Stahli BE, Nguyen-Kim TD, Gebhard C et al (2015) Prosthesis-specific predictors of paravalvular regurgitation after transcatheter aortic valve replacement: impact of calcification and sizing on balloon-expandable versus self-expandable transcatheter heart valves. J Heart Valve Dis 24(1):10–21
Haensig M, Lehmkuhl L, Linke A et al (2016) Aortic valve calcium score for paravalvular aortic insufficiency (AVCS II) study in transapical aortic valve implantation. Heart Surg Forum 19(1):E036–E042. doi:10.1532/hsf.1399
Koos R, Mahnken AH, Dohmen G et al (2011) Association of aortic valve calcification severity with the degree of aortic regurgitation after transcatheter aortic valve implantation. Int J Cardiol 150(2):142–145. doi:10.1016/j.ijcard.2010.03.004
Haensig M, Lehmkuhl L, Rastan AJ et al (2012) Aortic valve calcium scoring is a predictor of significant paravalvular aortic insufficiency in transapical-aortic valve implantation. Eur J Cardiothorac Surg 41(6):1234–1240. doi:10.1093/ejcts/ezr244 (discussion 1240–1231)
Khalique OK, Hahn RT, Gada H et al (2014) Quantity and location of aortic valve complex calcification predicts severity and location of paravalvular regurgitation and frequency of post-dilation after balloon-expandable transcatheter aortic valve replacement. JACC Cardiovasc Interv 7(8):885–894. doi:10.1016/j.jcin.2014.03.007
Schultz C, Rossi A, van Mieghem N et al (2011) Aortic annulus dimensions and leaflet calcification from contrast MSCT predict the need for balloon post-dilatation after TAVI with the Medtronic CoreValve prosthesis. EuroIntervention 7(5):564–572. doi:10.4244/EIJV7I5A92
Barbanti M, Petronio AS, Capodanno D et al (2014) Impact of balloon post-dilation on clinical outcomes after transcatheter aortic valve replacement with the self-expanding CoreValve prosthesis. JACC Cardiovasc Interv 7(9):1014–1021. doi:10.1016/j.jcin.2014.03.009
Barbanti M, Yang TH, Rodes Cabau J et al (2013) Anatomical and procedural features associated with aortic root rupture during balloon-expandable transcatheter aortic valve replacement. Circulation 128(3):244–253. doi:10.1161/CIRCULATIONAHA.113.002947
Abdel-Wahab M, Neumann FJ, Mehilli J et al (2015) 1-year outcomes after transcatheter aortic valve replacement with balloon-expandable versus self-expandable valves: results from the CHOICE Randomized Clinical Trial. J Am Coll Cardiol 66(7):791–800. doi:10.1016/j.jacc.2015.06.026
Webb J, Gerosa G, Lefevre T et al (2014) Multicenter evaluation of a next-generation balloon-expandable transcatheter aortic valve. J Am Coll Cardiol 64(21):2235–2243. doi:10.1016/j.jacc.2014.09.026
Gaede L, Blumenstein J, Kim WK et al (2017) Trends in aortic valve replacement in Germany in 2015: transcatheter versus isolated surgical aortic valve repair. Clin Res Cardiol 106(6):411–419. doi:10.1007/s00392-016-1070-1
Kempfert J, Rastan A, Holzhey D et al (2011) Transapical aortic valve implantation: analysis of risk factors and learning experience in 299 patients. Circulation 124(11 Suppl):S124–S129. doi:10.1161/CIRCULATIONAHA.110.013425
Giannini C, De Carlo M, Tamburino C et al (2017) Transcathether aortic valve implantation with the new repositionable self-expandable Evolut R versus CoreValve system: a case-matched comparison. Int J Cardiol. doi:10.1016/j.ijcard.2017.05.095
Acknowledgements
We thank Elizabeth Martinson, PhD, from the KHFI Editorial Office for her editorial assistance.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
WK and HM are proctors for Symetis SA and St. Jude Medical. All other authors declare that they have no financial disclosure relevant to the content of this manuscript.
Additional information
Won-Keun Kim and Johannes Blumenstein contributed equally to this work.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Kim, WK., Blumenstein, J., Liebetrau, C. et al. Comparison of outcomes using balloon-expandable versus self-expanding transcatheter prostheses according to the extent of aortic valve calcification. Clin Res Cardiol 106, 995–1004 (2017). https://doi.org/10.1007/s00392-017-1149-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00392-017-1149-3