Abstract
Purpose
The risk factors for acquiring an infection with multidrug-resistant (MDR) bacteria in patients with anastomotic leakage after colorectal cancer surgery are poorly understood. We evaluated the risk factors associated with the initial acquisition of MDR pathogens in patients with anastomotic leakage after colorectal cancer surgery.
Methods
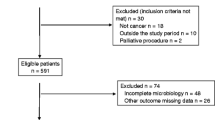
This study was a retrospective review of prospectively collected data at a university affiliated-tertiary referral hospital in South Korea. From January 2009 to April 2013, a total of 6767 consecutive patients with colorectal cancer who underwent surgery were registered. Of these patients, 190 (2.8 %) were diagnosed with anastomotic leakage. Finally, 143 (2.1 %) patients with culture test results were included in this study.
Results
Of the 143 enrolled patients, 46 (32.2 %) were classified in the MDR group. The use of antibiotics for more than 5 days before diagnosis of anastomosis site leakage (p = 0.016) and diabetes mellitus (p = 0.028) was identified as independent risk factors for MDR acquisition by multivariate analysis. The rate of adequate initial empirical antibiotic therapy in the MDR group was lower than in the non-MDR group (35 vs. 75 %, p < 0.001). Furthermore, the duration of antibiotic administration after the leak was longer in the MDR group (p = 0.013). Patients in the MDR group also had a longer hospital stay (p = 0.012).
Conclusions
The length of antibiotic administration before the diagnosis of anastomotic leakage and diabetes mellitus were risk factors associated with the acquisition of MDR bacteria in patients with anastomotic leakage after colorectal cancer surgery.
Similar content being viewed by others
References
Roehrborn A, Thomas L, Potreck O, Ebener C, Ohmann C, Goretzki PE, Roher HD (2001) The microbiology of postoperative peritonitis. Clin Infect Dis 33:1513–1519
Riche FC, Dray X, Laisne MJ, Mateo J, Raskine L, Sanson-Le Pors MJ, Payen D, Valleur P, Cholley BP (2009) Factors associated with septic shock and mortality in generalized peritonitis: comparison between community-acquired and postoperative peritonitis. Crit Care 13:R99
Frye J, Bokey EL, Chapuis PH, Sinclair G, Dent OF (2009) Anastomotic leakage after resection of colorectal cancer generates prodigious use of hospital resources. Color Dis 11:917–920
Augustin P, Kermarrec N, Muller-Serieys C, Lasocki S, Chosidow D, Marmuse JP, Valin N, Desmonts JM, Montravers P (2010) Risk factors for multidrug resistant bacteria and optimization of empirical antibiotic therapy in postoperative peritonitis. Crit Care 14:R20
Matthiessen P, Hallbook O, Andersson M, Rutegard J, Sjodahl R (2004) Risk factors for anastomotic leakage after anterior resection of the rectum. Color Dis 6:462–469
Eckmann C, Kujath P, Schiedeck TH, Shekarriz H, Bruch HP (2004) Anastomotic leakage following low anterior resection: results of a standardized diagnostic and therapeutic approach. Int J Color Dis 19:128–133
Caulfield H, Hyman NH (2013) Anastomotic leak after low anterior resection: a spectrum of clinical entities. JAMA Surg 148:177–182
Kumar A, Roberts D, Wood KE, Light B, Parrillo JE, Sharma S, Suppes R, Feinstein D, Zanotti S, Taiberg L, Gurka D, Kumar A, Cheang M (2006) Duration of hypotension before initiation of effective antimicrobial therapy is the critical determinant of survival in human septic shock. Crit Care Med 34:1589–1596
Gold HS, Moellering RC Jr (1996) Antimicrobial-drug resistance. N Engl J Med 335:1445–1453
Montravers P, Gauzit R, Muller C, Marmuse JP, Fichelle A, Desmonts JM (1996) Emergence of antibiotic-resistant bacteria in cases of peritonitis after intraabdominal surgery affects the efficacy of empirical antimicrobial therapy. Clin Infect Dis 23:486–494
Solomkin JS, Mazuski JE, Baron EJ, Sawyer RG, Nathens AB, DiPiro JT, Buchman T, Dellinger EP, Jernigan J, Gorbach S, Chow AW, Bartlett J (2003) Guidelines for the selection of anti-infective agents for complicated intra-abdominal infections. Clin Infect Dis 37:997–1005
Christou NV, Turgeon P, Wassef R, Rotstein O, Bohnen J, Potvin M (1996) Management of intra-abdominal infections. The case for intraoperative cultures and comprehensive broad-spectrum antibiotic coverage. The Canadian Intra-abdominal Infection Study Group. Arch Surg 131:1193–1201
Magiorakos AP, Srinivasan A, Carey RB, Carmeli Y, Falagas ME, Giske CG, Harbarth S, Hindler JF, Kahlmeter G, Olsson-Liljequist B, Paterson DL, Rice LB, Stelling J, Struelens MJ, Vatopoulos A, Weber JT, Monnet DL (2012) Multidrug-resistant, extensively drug-resistant and pandrug-resistant bacteria: an international expert proposal for interim standard definitions for acquired resistance. Clin Microbiol Infect 18:268–281
Seguin P, Laviolle B, Chanavaz C, Donnio PY, Gautier-Lerestif AL, Campion JP, Malledant Y (2006) Factors associated with multidrug-resistant bacteria in secondary peritonitis: impact on antibiotic therapy. Clin Microbiol Infect 12:980–985
Seguin P, Fedun Y, Laviolle B, Nesseler N, Donnio PY, Malledant Y (2010) Risk factors for multidrug-resistant bacteria in patients with post-operative peritonitis requiring intensive care. J Antimicrob Chemother 65:342–346
Burnett RJ, Haverstock DC, Dellinger EP, Reinhart HH, Bohnen JM, Rotstein OD, Vogel SB, Solomkin JS (1995) Definition of the role of Enterococcus in intraabdominal infection: analysis of a prospective randomized trial. Surgery 118:716–721, discussion 721–713
Montravers P, Andremont A, Massias L, Carbon C (1994) Investigation of the potential role of Enterococcus faecalis in the pathophysiology of experimental peritonitis. J Infect Dis 169:821–830
Sitges-Serra A, Lopez MJ, Girvent M, Almirall S, Sancho JJ (2002) Postoperative enterococcal infection after treatment of complicated intra-abdominal sepsis. Br J Surg 89:361–367
Walker AP, Nichols RL, Wilson RF, Bivens BA, Trunkey DD, Edmiston CE Jr, Smith JW, Condon RE (1993) Efficacy of a beta-lactamase inhibitor combination for serious intraabdominal infections. Ann Surg 217:115–121
Cohn SM, Lipsett PA, Buchman TG, Cheadle WG, Milsom JW, O'Marro S, Yellin AE, Jungerwirth S, Rochefort EV, Haverstock DC, Kowalsky SF (2000) Comparison of intravenous/oral ciprofloxacin plus metronidazole versus piperacillin/tazobactam in the treatment of complicated intraabdominal infections. Ann Surg 232:254–262
Ohlin B, Cederberg A, Forssell H, Solhaug JH, Tveit E (1999) Piperacillin/tazobactam compared with cefuroxime/ metronidazole in the treatment of intra-abdominal infections. Eur J Surg 165:875–884
Krobot K, Yin D, Zhang Q, Sen S, Altendorf-Hofmann A, Scheele J, Sendt W (2004) Effect of inappropriate initial empiric antibiotic therapy on outcome of patients with community-acquired intra-abdominal infections requiring surgery. Eur J Clin Microbiol Infect Dis 23:682–687
Dellinger RP, Levy MM, Carlet JM, Bion J, Parker MM, Jaeschke R, Reinhart K, Angus DC, Brun-Buisson C, Beale R, Calandra T, Dhainaut JF, Gerlach H, Harvey M, Marini JJ, Marshall J, Ranieri M, Ramsay G, Sevransky J, Thompson BT, Townsend S, Vender JS, Zimmerman JL, Vincent JL (2008) Surviving sepsis campaign: international guidelines for management of severe sepsis and septic shock: 2008. Crit Care Med 36:296–327
Montravers P, Lepape A, Dubreuil L, Gauzit R, Pean Y, Benchimol D, Dupont H (2009) Clinical and microbiological profiles of community-acquired and nosocomial intra-abdominal infections: results of the French prospective, observational EBIIA study. J Antimicrob Chemother 63:785–794
Dellinger RP, Levy MM, Rhodes A, Annane D, Gerlach H, Opal SM, Sevransky JE, Sprung CL, Douglas IS, Jaeschke R, Osborn TM, Nunnally ME, Townsend SR, Reinhart K, Kleinpell RM, Angus DC, Deutschman CS, Machado FR, Rubenfeld GD, Webb SA, Beale RJ, Vincent JL, Moreno R (2013) Surviving sepsis campaign: international guidelines for management of severe sepsis and septic shock: 2012. Crit Care Med 41:580–637
Funding/support
None.
Financial disclosure
None.
Conflict of interest
The authors declared no financial conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Lee, DS., Ryu, JA., Chung, C.R. et al. Risk factors for acquisition of multidrug-resistant bacteria in patients with anastomotic leakage after colorectal cancer surgery. Int J Colorectal Dis 30, 497–504 (2015). https://doi.org/10.1007/s00384-015-2161-6
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00384-015-2161-6