Abstract
Background
This manuscript is a review of different surgical techniques to manage perforated colon diverticulitis.
Objective
This study was conducted to compare the benefits and disadvantages of different surgical treatments for Hinchey III or IV type of colon diverticulitis.
Methods
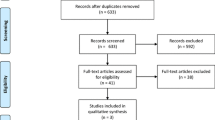
A systematic search was conducted in Medline, Embase, Cochrane Central Register of Controlled Trials, and the Science Citation Index (1990 and 2011). A total of 1,809 publications were identified and 14 studies with 1,041 patients were included in the study. Any surgical treatment was considered in this review. Mortality was considered the primary outcome, whereas hospital stay and reoperation rate were considered secondary outcomes.
Results
Primary resection with anastomosis has a significant advantage in terms of lower mortality rate with respect to Hartmann’s procedure (P = 0.02). The postoperative length of hospitalization was significantly shorter in the resection with anastomosis group (P < 0.001). Different findings have emerged from studies of patients with the primary resection with anastomosis vs laparoscopic peritoneal lavage and subsequent resection: overall surgical morbidity and hospital stay were lower in the laparoscopic peritoneal lavage group compared to the primary resection and anastomosis group (P < 0.001).
Conclusions
Despite numerous published articles on operative treatments for patients with generalized peritonitis from perforated diverticulitis, we found a marked heterogeneity between included studies limiting the possibility to summarize in a metanalytical method the data provided and make difficult to synthesize data in a quantitative fashion. The advantages in the group of colon resection with primary anastomosis in terms of lower mortality rate and postoperative stay should be interpreted with caution because of several limitations. Future randomized controlled trials are needed to further evaluate different surgical treatments for patients with generalized peritonitis from perforated diverticulitis.


Similar content being viewed by others
References
Weizman AV, Nguyen GC (2011) Diverticular disease: epidemiology and management. Can J Gastroenterol 25:385–389
Vermeulen J, Lange JF (2010) Treatment of perforated diverticulitis with generalized peritonitis: past, present, and future. World J Surg 34:587–593
Hughes ES, Cuthbertson AM, Carden AB (1963) The surgical management of acute diverticulitis. Med J Aust 50(1):780–782
Hinchey EJ, Schaal PG, Richards GK (1978) Treatment of perforated diverticular disease of the colon. Adv Surg 12:85–109
Killingback M (1983) Management of perforative diverticulitis. Surg Clin North Am 63:97–115
Krukowski ZH, Matheson NA (1984) Emergency surgery for diverticular disease complicated by generalized and faecal peritonitis: a review. Br J Surg 71:921–927
Aydin HN, Tekkis PP, Remzi FH, Constantinides V, Fazio VW (2006) Evaluation of the risk of a nonrestorative resection for the treatment of diverticular disease: the Cleveland Clinic diverticular disease propensity score. Dis Colon Rectum 49:629–639
Kaiser AM, Jiang JK, Lake JP, Ault G, Artinyan A, Gonzalez-Ruiz C et al (2005) The management of complicated diverticulitis and the role of computed tomography. Am J Gastroenterol 100:910–917
Smithwick RH (1942) Experiences with the surgical management of diverticulitis of the sigmoid. Ann Surg 115:969–985
Lockhart-Mummery JP (1938) Late results of diverticulitis. Lancet 2:1401–1404
Greif JM, Fried G, McSherry CK (1980) Surgical treatment of perforated diverticulitis of the sigmoid colon. Dis Colon Rectum 23:483–487
Banerjee S, Leather AJ, Rennie JA, Samano N, Gonzalez JG, Papagrigoriadis S (2005) Feasibility and morbidity of reversal of Hartmann's. Colorectal Dis 7:454–459
Toorenvliet BR, Bakker RF, Breslau PJ, Merkus JW, Hamming JF (2010) Colonic diverticulitis: a prospective analysis of diagnostic accuracy and clinical decision-making. Colorectal Dis 12:179–186
White SI, Frenkiel B, Martin PJ (2010) A ten-year audit of perforated sigmoid diverticulitis: highlighting the outcomes of laparoscopic lavage. Dis Colon Rectum 53:1537–1541
Kohler L, Sauerland S, Neugebauer E (1999) Diagnosis and treatment of diverticular disease: results of a consensus development conference. The Scientific Committee of the European Association for Endoscopic Surgery. Surg Endosc 13:430–436
Lee EC, Murray JJ, Coller JA, Roberts PL, Schoetz DJ Jr (1997) Intraoperative colonic lavage in nonelective surgery for diverticular disease. Dis Colon Rectum 40:669–674
Biondo S, Pares D, Kreisler E, Rague JM, Fraccalvieri D, Ruiz AG et al (2005) Anastomotic dehiscence after resection and primary anastomosis in left-sided colonic emergencies. Dis Colon Rectum 48:2272–2280
Tabbara M, Velmahos GC, Butt MU, Chang Y, Spaniolas K, Demoya M et al (2010) Missed opportunities for primary repair in complicated acute diverticulitis. Surgery 148:919–924
Moher D, Liberati A, Tetzlaff J, Altman DG (2009) Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. PLoS Med 6:e1000097
Higgins J, Green S (eds) (2011) Cochrane handbook for systematic reviews of interventions. Wiley, Chichester
Liberati A, Altman DG, Tetzlaff J, Mulrow C, Gotzsche PC, Ioannidis JP et al (2009) The PRISMA statement for reporting systematic reviews and meta-analyses of studies that evaluate health care interventions: explanation and elaboration. PLoS Med 6:e1000100
Greenland S, Robins JM (1985) Estimation of a common effect parameter from sparse follow-up data. Biometrics 41:55–68
Mantel N, Haenszel W (1959) Statistical aspects of the analysis of data from retrospective studies of disease. J Natl Cancer Inst 22:719–748
Friedman HP, Goldberg JD (1996) Meta-analysis: an introduction and point of view. Hepatology 23:917–928
SIGN guidelines. Available at: http://www.sign.ac.uk/guidelines/fulltext/50/checklist3. Accessed 20 Mar 2009
Rangel SJ, Kelsey J, Colby CE, Anderson J, Moss RL (2003) Development of a quality assessment scale for retrospective clinical studies in pediatric surgery. J Pediatr Surg 38:390–396, discussion −6
Jadad AR, Moore RA, Carroll D, Jenkinson C, Reynolds DJ, Gavaghan DJ et al (1996) Assessing the quality of reports of randomized clinical trials: is blinding necessary? Control Clin Trials 17:1–12
Chalmers TC, Smith H Jr, Blackburn B, Silverman B, Schroeder B, Reitman D et al (1981) A method for assessing the quality of a randomized control trial. Control Clin Trials 2:31–49
Egger M (1997) Davey Smith G, Schneider M, Minder C. Bias in meta-analysis detected by a simple, graphical test. BMJ 315:629–634
Fegiz G, Tonelli F, Rossi P, Di Paola M, De Masi E, Simonetti G (1976) Preservation of the superior hemorrhoidal artery in resection of the colon and rectum. Surg Gynecol Obstet 143:919–925
Napolitano AM, Napolitano L, Costantini R, Ucchino S (1996) Innocenti P [Skeletization of the inferior mesenteric artery in colorectal surgery. Current considerations]. G Chir 17:185–189
Gooszen AW, Tollenaar RA, Geelkerken RH, Smeets HJ, Bemelman WA, Van Schaardenburgh P et al (2001) Prospective study of primary anastomosis following sigmoid resection for suspected acute complicated diverticular disease. Br J Surg 88:693–697
Hoemke M, Treckmann J, Schmitz R, Shah S (1999) Complicated diverticulitis of the sigmoid: a prospective study concerning primary resection with secure primary anastomosis. Dig Surg 16:420–424
Messinetti S, Giacomelli L, Manno A, Finizio R, Fabrizio G, Granai AV et al (1998) Preservation and peeling of the inferior mesenteric artery in the anterior resection for complicated diverticular disease. Ann Ital Chir 69:479–482, discussion 82–3
Urbanavicius L, Pattyn P, de Putte DV, Venskutonis D (2011) How to assess intestinal viability during surgery: a review of techniques. World J Gastrointest Surg 3:59–69
Binda GA, Arezzo A, Serventi A, Bonelli L, Facchini M, Prandi M et al (2012) Multicentre observational study of the natural history of left-sided acute diverticulitis. Br J Surg 99:276–285
Gooszen AW, Gooszen HG, Veerman W, Van Dongen VM, Hermans J, Klien Kranenbarg E et al (2001) Operative treatment of acute complications of diverticular disease: primary or secondary anastomosis after sigmoid resection. Eur J Surg 167:35–39
Hold M, Denck H, Bull P (1990) Surgical management of perforating diverticular disease in Austria. Int J Colorectal Dis 5:195–199
Regenet N, Pessaux P, Hennekinne S, Lermite E, Tuech JJ, Brehant O et al (2003) Primary anastomosis after intraoperative colonic lavage vs. Hartmann's procedure in generalized peritonitis complicating diverticular disease of the colon. Int J Colorectal Dis 18:503–507
Richter S, Lindemann W, Kollmar O, Pistorius GA, Maurer CA, Schilling MK (2006) One-stage sigmoid colon resection for perforated sigmoid diverticulitis (Hinchey stages III and IV). World J Surg 30:1027–1032
Schilling MK, Maurer CA, Kollmar O, Buchler MW (2001) Primary vs. secondary anastomosis after sigmoid colon resection for perforated diverticulitis (Hinchey Stage III and IV): a prospective outcome and cost analysis. Dis Colon Rectum 44:699–703, discussion −5
Trenti L, Biondo S, Golda T, Monica M, Kreisler E, Fraccalvieri D et al (2011) Generalized peritonitis due to perforated diverticulitis: Hartmann's procedure or primary anastomosis? Int J Colorectal Dis 26:377–384
Finlay IG, Carter DC (1987) A comparison of emergency resection and staged management in perforated diverticular disease. Dis Colon Rectum 30:929–933
Karoui M, Champault A, Pautrat K, Valleur P, Cherqui D, Champault G (2009) Laparoscopic peritoneal lavage or primary anastomosis with defunctioning stoma for Hinchey 3 complicated diverticulitis: results of a comparative study. Dis Colon Rectum 52:609–615
Nagorney DM, Adson MA, Pemberton JH (1985) Sigmoid diverticulitis with perforation and generalized peritonitis. Dis Colon Rectum 28:71–75
Vermeulen J, Akkersdijk GP, Gosselink MP, Hop WC, Mannaerts GH, van der Harst E et al (2007) Outcome after emergency surgery for acute perforated diverticulitis in 200 cases. Dig Surg 24:361–366
Zingg U, Pasternak I, Dietrich M, Seifert B, Oertli D, Metzger U (2010) Primary anastomosis vs Hartmann's procedure in patients undergoing emergency left colectomy for perforated diverticulitis. Colorectal Dis 12:54–60
Zeitoun G, Laurent A, Rouffet F, Hay J, Fingerhut A, Paquet J et al (2000) Multicentre, randomized clinical trial of primary versus secondary sigmoid resection in generalized peritonitis complicating sigmoid diverticulitis. Br J Surg 87:1366–1374
Kronborg O (1993) Treatment of perforated sigmoid diverticulitis: a prospective randomized trial. Br J Surg 80:505–507
Perathoner A, Klaus A, Muhlmann G, Oberwalder M, Margreiter R, Kafka-Ritsch R (2010) Damage control with abdominal vacuum therapy (VAC) to manage perforated diverticulitis with advanced generalized peritonitis—a proof of concept. Int J Colorectal Dis 25:767–774
Pasternak I, Dietrich M, Woodman R, Metzger U, Wattchow DA, Zingg U (2010) Use of severity classification systems in the surgical decision-making process in emergency laparotomy for perforated diverticulitis. Int J Colorectal Dis 25:463–470
Krukowski ZH (2009) Diverticular disease. In: Phillips RKS (ed) Colorectal surgery: a companion to specialist surgical practice, 3rd edn. Saunders, Edinburgh, p 107–124
Practice parameters for sigmoid diverticulitis (2000) The Standards Task Force, American Society of Colon and Rectal Surgeons. Surg Laparosc Endosc Percutan Tech 10:142–148.
Mayo WJ, Wilson LB, Griffin HZ (1907) Acquired diverticulitis of the large intestine. Surg Gynecol Obstet 5:8–15
Bauer VP (2009) Emergency management of diverticulitis. Clin Colon Rectal Surg 22:161–168
Constantinides VA, Tekkis PP, Athanasiou T, Aziz O, Purkayastha S, Remzi FH et al (2006) Primary resection with anastomosis vs. Hartmann's procedure in nonelective surgery for acute colonic diverticulitis: a systematic review. Dis Colon Rectum 49:966–981
Afshar S, Kurer MA (2012) Laparoscopic peritoneal lavage for perforated sigmoid diverticulitis. Colorectal Dis 14:135–142
Naraynsingh V, Maharaj R, Hassranah D, Hariharan S, Dan D, Zbar AP (2011) Perforated left-sided diverticulitis with faecal peritonitis: is the Hinchey classification the best guide for surgical decision making? Tech Coloproctol 15:199–203
Mueller MH, Karpitschka M, Renz B, Kleespies A, Kasparek MS, Jauch KW et al (2011) Co-morbidity and postsurgical outcome in patients with perforated sigmoid diverticulitis. Int J Colorectal Dis 26:227–234
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Cirocchi, R., Trastulli, S., Desiderio, J. et al. Treatment of Hinchey stage III–IV diverticulitis: a systematic review and meta-analysis. Int J Colorectal Dis 28, 447–457 (2013). https://doi.org/10.1007/s00384-012-1622-4
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00384-012-1622-4