Abstract
Background
The response of mesothelial cells to surgical trauma and bacterial contamination is poorly defined. We have recently shown that CO2 pneumoperitoneum increases systemic metastasis of neuroblastoma cells in a murine model. Thus, we hypothesized that CO2 alters the morphology and function of mesothelial cells and facilitates transmesothelial tumor cell migration.
Materials and methods
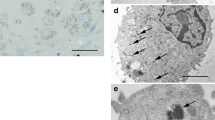
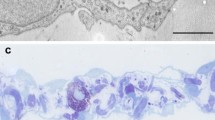
Murine mesothelial cells were exposed to 100% CO2 and 5% CO2 as control. Scanning electron microscopy (SEM) investigations, as well as LPS-induced granulocyte-colony stimulating factor (G-CSF) production and mitochondrial activity (MTT assay) were measured. Transmesothelial migration of neuroblastoma cells (Neuro2a) was determined using a transwell chamber system.
Results
CO2 incubation was associated with a significant destruction of the microvillar formation in SEM. Migration studies showed that the barrier function of the mesothelial monolayer decreased. A significantly increased migration of neuroblastoma cells was identified after 100% CO2 exposure (P < 0.05). Although the conversion of MTT as an indicator of mitochondrial activity was only slightly and not significantly reduced after CO2 incubation, the release of G-CSF induced by LPS was completely blocked during the incubation with 100% CO2 (P < 0.05). The capacity of G-CSF release recovered after the incubation.
Conclusion
We observed that peritoneal mesothelial cells lose their typical cell morphology by CO2 incubation, which is accompanied by facilitated migration of neuroblastoma cells. Moreover, the synthesis of immunological factors is blocked, but this effect is not long lasting. These mechanisms may explain an increased metastasis rate of neuroblastoma cells after CO2 pneumoperitoneum, which was recently observed in a murine model.




Similar content being viewed by others
References
Metzelder ML, Kuebler JF, Shimotakahara A, Glueer S, Grigull L, Ure BM (2007) Role of diagnostic and ablative minimally invasive surgery for pediatric malignancies. Cancer 109:2343–2348
Iwanaka T, Kawashima H, Uchida H (2007) The laparoscopic approach of neuroblastoma. Semin Pediatr Surg 16:259–265
Leclair MD, de Lagausie P, Becmeur F, Varlet F, Thomas C, Valla JS, Petit T, Philippe-Chomette P, Mure PY, Sarnacki S, Michon J, Heloury Y (2008) Laparoscopic resection of abdominal neuroblastoma. Ann Surg Oncol 15:117–124
Chan KW, Lee KH, Tam YH, Yeung CK (2007) Minimal invasive surgery in pediatric solid tumors. J Laparoendosc Adv Surg Tech A 17:817–820
Jacobi CA, Wenger F, Sabat R, Volk T, Ordemann J, Müller JM (1998) The impact of laparoscopy with carbon dioxide versus helium on immunologic function and tumor growth in a rat model. Dig Surg 15:110–116
Cirocco WC, Schwartzman A, Golub RW (1994) Abdominal wall recurrence after laparoscopic colectomy for colon cancer. Surgery 116:842–846
Gleeson NC, Nicosia SV, Mark JE, Hoffman MS, Cavanagh D (1993) Abdominal wall metastases from ovarian cancer after laparoscopy. Am J Obstet Gynecol 169:522–523
Muntz HG, Goff BA, Madsen BL, Yon JL (1999) Port site recurrence after laparoscopic surgery for endometrial carcinoma. Obstet Gynecol 93:807–809
Are C, Talamini MA (2005) Laparoscopy and malignancy. J Laparoendosc Adv Surg Tech A 15:38–47
Bouvy ND, Marquet RL, Hamming JF, Jeekel J, Bonjer HJ (1996) Laparoscopic surgery in the rat: beneficial effect on body weight and tumor take. Surg Endosc 10:490–494
Iwanaka T, Arya G, Ziegler MM (1998) Mechanism and prevention of port-site tumor recurrence after laparoscopy in a murine model. J Pediatr Surg 33:457–461
Maris JM, Hogarty MD, Bagatell R, Cohn SL (2007) Neuroblastoma. Lancet 369:2106–2120
Suita S, Tajiri T, Higashi M, Tanaka S, Kinoshita Y, Takahashi Y, Tatsuta K (2007) Insights into infant neuroblastomas based on an analysis of neuroblastoma detected by mass screening at 6 months of age in Japan. Eur J Pediatr Surg 17:23–28
George RE, Sanda T, Hanna M, Fröhling S, Luther W 2nd, Zhang J, Ahn Y, Zhou W, London WB, McGrady P, Xue L, Zozulya S, Gregor VE, Webb TR, Gray NS, Gilliland DG, Diller L, Greulich H, Morris SW, Meyerson M, Look AT (2008) Activating mutations in ALK provide a therapeutic target in neuroblastoma. Nature 455:975–978
Metzelder M, Kuebler J, Shimotakahara A, Vieten G, von Wasielewski R, Ure BM (2008) CO(2) pneumoperitoneum increases systemic but not local tumor spread after intraperitoneal murine neuroblastoma spillage in mice. Surg Endosc 22:2648–2653 [Epub 13 Feb 2008]
Reismann M, Wehrmann F, Schukfeh N, Kuebler JF, Ure B, Glüer S (2009) Carbon dioxide, hypoxia and low PH lead to overexpression of c-mys and HMGB-1 oncogenes in neuroblastoma cells. Eur J Pediatr Surg 19:224–227 [Epub 22 Apr 2009]
Yung S, Chan TM (2007) Mesothelial cells. Perit Dial Int 27 Suppl 2:S110–S115
Mutsaers SE (2002) Mesothelial cells: their structure, function and role in serosal repair. Respirology 7:171–191
Kimura A, Koga S, Kudoh H, Iitsuka Y (1985) Peritoneal mesothelial cell injury factors in rat cancerous ascites. Cancer Res 45:4330–4333
Ordemann J, Jakob J, Braumann C, Kilian M, Bachmann S, Jacobi CA (2004) Morphology of the rat peritoneum after carbon dioxide and helium pneumoperitoneum: a scanning electron microscopic study. Surg Endosc 18:1389–1393 [Epub 15 Jul 2004]
Thuijls G, de Haan JJ, Derikx JP, Daissormont I, Hadfoune M, Heineman E, Buurman WA (2009) Intestinal cytoskeleton degradation precedes tight junction loss following hemorrhagic shock. Shock 31(2):164–169
Tsukita S, Furuse M, Itoh M (2001) Multifunctional strands in tight junctions. Nat Rev Mol Cell Biol 2:285–293
Fleming S (1991) C. L. Oakley Lecture (1991). Cell adhesion and epithelial differentiation. J Pathol 164:95–100
Rosário MT, Ribeiro U Jr, Corbett CE, Ozaki AC, Bresciani CC, Zilberstein B, Gama-Rodrigues JJ (2006) Does CO2 pneumoperitoneum alter the ultra-structure of the mesothelium? J Surg Res 133:84–88 [Epub 19 Dec 2005]
Ziegler MM, Ishizu H, Nagabuchi E, Takada N, Arya G (1997) A comparative review of the immunology of murine neuroblastoma and human neuroblastoma. Cancer 79:1757–1766
Gebert A, Preiss G (1998) A simple method for the acquisition of high-quality digital images from analog scanning electron microscopes. J Microsc 191:297–302
Shimotakahara A, Kuebler JF, Vieten G, Kos M, Metzelder ML, Ure BM (2008) Carbon dioxide directly suppresses spontaneous migration, chemotaxis, and free radical production of human neutrophils. Surg Endosc 22:1813–1817 [Epub 11 Dec 2007]
Gerlier D, Thomasset N (1986) Use of MTT colorimetric assay to measure cell activation. J Immunol Methods 94:57–63
Gay AN, Chang S, Rutland L, Yu L, Byeseda S, Naik-Mathuria B, Cass DL, Russell H, Olutoye OO (2008) Granulocyte colony stimulating factor alters the phenotype of neuroblastoma cells: implications for disease-free survival of high-risk patients. J Pediatr Surg 43:837–842
Volz J, Köster S, Spacek Z, Paweletz N (1999) Characteristic alterations of the peritoneum after carbon dioxide pneumoperitoneum. Surg Endosc 13:611–614
Volz J, Köster S, Spacek Z, Paweletz N (1999) The influence of pneumoperitoneum used in laparoscopic surgery on an intraabdominal tumor growth. Cancer 86:770–774
Kuebler JF, Kos M, Jesch NK, Metzelder ML, van der Zee DC, Bax KM, Vieten G, Ure BM (2007) Carbon dioxide suppresses macrophage superoxide anion production independent of extracellular pH and mitochondrial activity. J Pediatr Surg 42:244–248
Kos M, Kuebler JF, Jesch NK, Vieten G, Bax NM, van der Zee DC, Busche R, Ure BM (2006) Carbon dioxide differentially affects the cytokine release of macrophage subpopulations exclusively via alteration of extracellular pH. Surg Endosc 20:570–576 [Epub 25 Jan 2006]
Schwartz N, Hosford M, Sandoval RM, Wagner MC, Atkinson SJ, Bamburg J, Molitoris BA (1999) Ischemia activates actin depolymerizing factor: role in proximal tubule microvillar actin alterations. Am J Physiol 276:F544–F551
Kellerman PS, Boqusky RT (1992) Microfilament disruption occurs very early in ischemic proximal tubule cell injury. Kidney Int 42:896–902
Kellerman PS, Clark RA, Hoilien CA, Linas SL, Molitoris BA (1990) Role of microfilaments in the maintenance of proximal tubule structural and functional integrity. Am J Physiol 259:F279–F285
Molitoris BA (1991) Ischemia-induced loss of epithelial polarity: potential role of the actin cytoskeleton. Am J Physiol 260:F769–F778
Molitoris BA (1997) Putting the actin cytoskeleton into perspective: pathophysiology of ischemic alterations. Am J Physiol 272:F430–F433
Faff L, Nolte C (2000) Extracellular acidification decreases the basal motility of cultured mouse microglia via the rearrangement of the actin cytoskeleton. Brain Res 853:22–31
Golenhofen N, Doctor RB, Bacallao R, Mandel LJ (1995) Actin and villin compartmentation during ATP depletion and recovery in renal cultured cells. Kidney Int 48:1837–1845
Jesch NK, Kuebler JF, Nguyen H, Nave H, Bottlaender M, Teichmann B, Braun A, Vieten G, Ure BM (2006) Laparoscopy vs. minilaparotomy and full laparotomy preserves circulatory but not peritoneal and pulmonary immune responses. J Pediatr Surg 41:1085–1092
Polat C, Kahraman A, Yilmaz S, Koken T, Serteser M, Akbulut G, Arikan Y, Dilek ON, Gokce O (2003) A comparison of the oxidative stress response and antioxidant capacity of open and laparoscopic hernia repairs. J Laparoendosc Adv Surg Tech A 13:167–173
Gál I, Róth E, Lantos J, Varga G, Jaberansari MT (1997) Inflammatory mediators and surgical trauma regarding laparoscopic access: free radical mediated reactions. Acta Chir Hung 36:97–99
Seven R, Seven A, Erbil Y, Mercan S, Burçak G (1999) Lipid peroxidation and antioxidant state after laparoscopic and open cholecystectomy. Eur J Surg 165:871–874
Glantzounis GK, Tselepis AD, Tambaki AP, Trikalinos TA, Manataki AD, Galaris DA, Tsimoyiannis EC, Kappas AM (2001) Laparoscopic surgery-induced changes in oxidative stress markers in human plasma. Surg Endosc 15:1315–1319 [Epub 16 Aug 2001]
Acknowledgments
The authors thank Mrs. Renate Schottmann and Mrs. Birgit Teichmann for their excellent technical assistance. The authors also thank Mrs. Clare Boerner for her editorial assistance.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Yu, Y., Kuebler, J., Groos, S. et al. Carbon dioxide modifies the morphology and function of mesothelial cells and facilitates transepithelial neuroblastoma cell migration. Pediatr Surg Int 26, 29–36 (2010). https://doi.org/10.1007/s00383-009-2503-y
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00383-009-2503-y