Abstract
Introduction
The purpose of this article is to contribute information to the interpretation of the feasibility and outcomes regarding open, laparoscopic and robotic strategies of radical prostatectomy in patients with previous synthetic mesh inguinal hernia repair.
Materials and methods
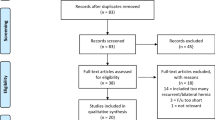
A bibliographic search covering the period from January 1980 to September 2012 was conducted in PubMed, MEDLINE and EMBASE. Database searches yielded 28 references. This analysis is based on the eleven studies that fulfilled the predefined criteria.
Results
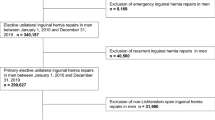
A total of 7,497 patients were included. In the study group, there were 462 patients. The surgical prostatectomy techniques were open in five studies, laparoscopic in three and robotic in the remaining three. The control group consisted in 7,035 patients. The comparison of the open procedure performed in patients with a previous mesh herniorrhaphy and controls shows that the number of lymph nodes removed resulted significantly lower and hospital stay with catheterization time results statistically longer. The comparison of the laparoscopic procedure does not evidence a statistically significant difference in terms of blood loss, operative time and catheterization time, while the comparison with the robotic group could not be performed for the lack of data.
Conclusion
All patients need an adequate informed consent regarding the multitude of aspects which may be influenced by the mesh such as the possibility of hernia recurrence, mesh infection, need for mesh explantation, possibility of mesh erosion into the bowel or bladder, bladder neck contractures or postoperative urinary incontinence and a compromised nodal staging.



Similar content being viewed by others
References
McCormack K, Scott NW, Go PM, Ross S, Grant AM (2011) EU Hernia Trialists Collaboration. Laparoscopic techniques versus open techniques for inguinal hernia repair. Cochrane Database Syst Rev 1:CD001785
Carter J, Duh QY (2011) Laparoscopic repair of inguinal hernias. World J Surg 35:1519–1525
Vijan SS, Wall JC, Greenlee SM, Farley DR (2008) Consequences of endoscopic inguinal hernioplasty with mesh on subsequent open radical prostatectomy. Hernia 12:415–419
Saint-Elie DT, Marshall FF (2010) Impact of laparoscopic inguinal hernia repair mesh on open radical retropubic prostatectomy. Urology 76:1078–1082
Peeters E, Joniau S, Van Poppel H, Miserez M (2012) Case-matched analysis of outcome after open retropubic radical prostatectomy in patients with previous preperitoneal inguinal hernia repair. Br J Surg 99:431–435
Hocaoglu Y, Bastian P, Buchner A et al (2010) Impact of previous mesh hernia repair on the performance of open radical prostatectomy—complications and functional outcome. BJU Int 106:1628–1631
Neff DA, See WA (2011) Laparoscopic mesh herniorrhaphy: impact on outcomes associated with radical retropubic prostatectomy. Urol Oncol 29:66–69
Do HM, Turner K, Dietel A, Wedderburn A, Liatsikos E, Stolzenburg JU (2011) Previous laparoscopic inguinal hernia repair does not adversely affect the functional or oncological outcomes of endoscopic extraperitoneal radical prostatectomy. Urology 77:963–967
Erdorgu T, Teber D, Frede T et al (2005) The effect of previous transperitoneal laparoscopic inguinal herniorrhaphy on transperitoneal laparoscopic radical prostatectomy. J Urol 173:769–772
Tsivian A, Brodsky O, Shtricker A, Tsivian M, Benjamin S, Sidi AA (2009) Urologic pelvic surgery following mesh hernia repair. Hernia 13:523–527
Laungani RG, Kaul S, Muhletaler F, Badani KK, Peabody J, Menon M (2007) Impact of previous inguinal hernia repair on transperitoneal robotic prostatectomy. Can J Urol 14:3635–3639
Lallas CD, Pe ML, Patel JV et al (2009) Transperitoneal robotic assisted laparoscopic prostatectomy after prosthetic mesh herniorrhaphy. JSLS 13:142–147
Siddiqui SA, Krane LS, Bhandari A et al (2010) The impact of previous inguinal or abdominal surgery on outcomes after robotic radical prostatectomy. Urology 75:1079–1082
Harris RP, Helfand M, Woolf SH et al (2001) Methods Work Group, Third US Preventive Services Task Force; Current methods of the US Preventive Services Task Force: a review of the process. Am J Prev Med 20:21–35
Harris R, Atkins D, Berg AO et al (2001) US Preventive Services Task Force Procedure Manual. Agency for Healthcare Research and Quality, Rockville
Moher D, Liberati A, Tetzlaff J, Altman DG, PRISMA Group (2009) Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. PLoS Med 6:e1000097
DerSimonian R, Laird N (1986) Meta-analysis in clinical trials. Control Clin Trials 7:177–188
Katz EE, Patel RV, Sokoloff MH, Vargish T, Brendler CB (2002) Bilateral laparoscopic inguinal hernia repair can complicate subsequent radical retropubic prostatectomy. J Urol 167:637–638
Cook H, Afzal N, Cornaby AJ (2003) Laparoscopic hernia repairs may make subsequent radical retropubic prostatectomy more hazardous. BJU Int 91:729
Cooperberg MR, Downs TM, Carroll PR (2004) Radical retropubic prostatectomy frustrated by prior laparoscopic mesh herniorrhaphy. Surgery 135:452–453
Foley CL, Kirby RS (2003) Re: bilateral laparoscopic inguinal hernia repair can complicate subsequent radical retropubic prostatectomy. J Urol 169:1475
Brown JA, Dahl DM (2004) Transperitoneal laparoscopic radical prostatectomy in patients after laparoscopic prosthetic mesh inguinal herniorrhaphy. Urology 63:380–382
Joseph JV, Madeb R, Wu G, Vicente I, Erturk E (2005) Laparoscopic radical prostatectomy following laparoscopic bilateral mesh hernia repair. JSLS 9:368–369
Rassweiler J, Sentker L, Seemann O et al (2001) Heilbronn laparoscopic radical prostatectomy. Technique and results after 100 cases. Eur Urol 40(1):54–64
Joslyn SA, Konety BR (2006) Impact of extent of lymphadenectomy on survival after radical prostatectomy for prostate cancer. Urology 68:121–125
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Picozzi, S.C.M., Ricci, C., Bonavina, L. et al. Feasibility and outcomes regarding open and laparoscopic radical prostatectomy in patients with previous synthetic mesh inguinal hernia repair: meta-analysis and systematic review of 7,497 patients. World J Urol 33, 59–67 (2015). https://doi.org/10.1007/s00345-014-1282-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00345-014-1282-9