Abstract
Purpose
To assess the pathological and the oncologic outcomes of the prostate cancer (PCa) missed by 6- and 12-core biopsy protocols by using a reference 21-core scheme.
Materials and methods
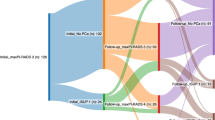
Between 2001 and 2009, all patients who had PCa detected in an initial 21-core TRUS biopsy scheme and were treated by a radical prostatectomy (RP) were included. Patients were sorted in 3 groups according to the diagnosis site: sextant (6 first cores; group 1), peripheral zone (12 first cores; group 2) or midline/transitional zone (after 21 cores; group 3). Demographics, pathological features in biopsy and RP specimens and follow-up after RP were analyzed. The 5-year progression-free survival (PFS) was studied in the 3 groups.
Results
During the study period, 443 patients were included. Among them, 67, 23.7 and 9.2% were, respectively, diagnosed in groups 1, 2 and 3. Among PCa diagnosed in midline/transition zone cores, 42% were intermediate or high risk. Unfavorable disease was more frequently reported in group 1 in terms of extraprostatic extension (P = 0.001), high Gleason score (P = 0.001) and progression (P = 0.001). No significant difference was observed between groups 2 and 3 in terms of pathological features in RP specimens and oncologic outcome. The 5-year PFS was 89.7% and not significantly different in patients diagnosed with a 12-core scheme compared to those diagnosed only with 21-core scheme (P = 0.332).
Conclusions
Our findings emphasize that PCa diagnosed only in a 21-core protocol is at least as aggressive as PCa detected in a 12-core scheme. This study invalidates the widespread idea sustaining that cancers diagnosed by more than 12 biopsies are less aggressive.

Similar content being viewed by others
References
Hodge KK, McNeal JE, Stamey TA (1989) Ultrasound guided transrectal core biopsies of the palpably abnormal prostate. J Urol 142:66–70
Norberg M, Egevad L, Holmberg L et al (1997) The sextant protocol for ultrasound-guided core biopsies of the prostate underestimates the presence of cancer. Urology 50:562–566
Presti JC Jr, O’Dowd GJ, Miller MC et al (2003) Extended peripheral zone biopsy schemes increase cancer detection rates and minimize variance in prostate specific antigen and age related cancer rates: results of a community multi-practice study. J Urol 169:125–129
Scattoni V, Zlotta A, Montironi R et al (2007) Extended and saturation prostatic biopsy in the diagnosis and characterisation of prostate cancer: a critical analysis of the literature. Eur Urol 52:1309–1322
Eichler K, Hempel S, Wilby J et al (2006) Diagnostic value of systematic biopsy methods in the investigation of prostate cancer: a systematic review. J Urol 175:1605–1612
de la Taille A, Antiphon P, Salomon L et al (2003) Prospective evaluation of a 21-sample needle biopsy procedure designed to improve the prostate cancer detection rate. Urology 61:1181–1186
Borboroglu PG, Comer SW, Riffenburgh RH et al (2000) Extensive repeat transrectal ultrasound guided prostate biopsy in patients with previous benign sextant biopsies. J Urol 163:158–162
Djavan B, Remzi M, Marberger M (2003) When to biopsy and when to stop biopsying. Urol Clin N Am 30:253–262
Boccon-Gibod LM, de Longchamps NB, Toublanc M et al (2006) Prostate saturation biopsy in the reevaluation of microfocal prostate cancer. J Urol 176:961–963
Epstein JI, Sanderson H, Carter HB et al (2005) Utility of saturation biopsy to predict insignificant cancer at radical prostatectomy. Urology 66:356–360
Heidenreich A, Bellmunt J, Bolla M et al (2010) EAU guidelines on prostate cancer. Part 1: screening, diagnosis, and treatment of clinically localised disease. Eur Urol 59(1):61–71
Eskew LA, Bare RL, McCullough DL (1997) Systematic 5 region prostate biopsy is superior to sextant method for diagnosing carcinoma of the prostate. J Urol 157:199–202
Eskew LA, Woodruff RD, Bare RL et al (1998) Prostate cancer diagnosed by the 5 region biopsy method is significant disease. J Urol 160:794–796
Guichard G, Larre S, Gallina A et al (2007) Extended 21-sample needle biopsy protocol for diagnosis of prostate cancer in 1000 consecutive patients. Eur Urol 52:430–435
Descazeaud A, Rubin M, Chemama S et al (2006) Saturation biopsy protocol enhances prediction of pT3 and surgical margin status on prostatectomy specimen. World J Urol 24:676–680
Ploussard G, Xylinnas E, Salomon L et al (2009) The role of biopsy core number in selecting prostate cancer patients for active surveillance. Eur Urol 56:891–898
Jones JS, Oder M, Zippe CD (2002) Saturation prostate biopsy with periprostatic block can be performed in office. J Urol 168:2108–2110
Abouassaly R, Tan N, Moussa A et al (2008) Risk of prostate cancer after diagnosis of atypical glands suspicious for carcinoma on saturation and traditional biopsies. J Urol 180:911–914
Terris MK, Wallen EM, Stamey TA (1997) Comparison of mid-lobe versus lateral systematic sextant biopsies in the detection of prostate cancer. Urol Int 59:239–242
Chen ME, Troncoso P, Johnston DA et al (1997) Optimization of prostate biopsy strategy using computer based analysis. J Urol 158:2168–2175
Campos-Fernandes JL, Bastien L, Nicolaiew N et al (2010) Prostate cancer detection rate in patients with repeated extended 21-sample needle biopsy. Eur Urol 55:600–606
Ploussard G, Bastien L, Descazeaud A et al (2010) Extended biopsy protocol decreases prostate cancer incidence and risk of aggressive disease on repeated biopsies compared with initial standard procedure. Urol Int 84:147–152
Scattoni V, Raber M, Abdollah F et al (2010) Biopsy schemes with the fewest cores for detecting 95% of the prostate cancers detected by a 24-core biopsy. Eur Urol 57:1–8
Conflict of interest
None.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Ouzaid, I., Xylinas, E., Campeggi, A. et al. Contemporary pathologic characteristics and oncologic outcomes of prostate cancers missed by 6- and 12-core biopsy and diagnosed with a 21-core biopsy protocol. World J Urol 31, 869–874 (2013). https://doi.org/10.1007/s00345-011-0800-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00345-011-0800-2