Abstract
Objectives
To investigate if removing DCE from the Vesical Imaging Reporting and Data System (VI-RADS) influences the diagnostic accuracy of muscle-invasive bladder cancer (MIBC). We also explored using different reference standards on the MRI diagnostic performance.
Methods
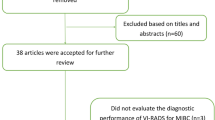
We searched the Cochrane Library, Embase, and PubMed databases to June 26, 2021. Pooled biparametric MRI (bpMRI, T2WI+DWI) and multiparametric MRI (mpMRI, T2WI+DWI+DCE) sensitivities and specificities and the diagnostic performances of these methods for MIBC were compared using different reference standards.
Results
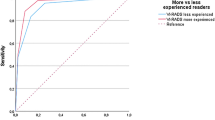
Seventeen studies with 2344 patients were finally included, of which 7 studies, including 1041 patients, reported the diagnostic performance of bpMRI. VI-RADS showed sensitivities and specificities of 0.91 (95% CI 0.87–0.94) and 0.86 (95% CI 0.77–0.91) at cutoff scores of 3, and 0.85 (95% CI 0.77–0.90) and 0.93 (95% CI 0.89–0.96) at cutoff scores of 4. BpMRI showed sensitivities and specificities of 0.90 (95% CI 0.69–0.97) and 0.90 (95% CI 0.81–0.95), and 0.84 (95% CI 0.78–0.88) and 0.97 (95% CI 0.87–0.99), respectively, for cutoff scores of 3 and 4. The sensitivities of bpMRI vs mpMRI for MIBC were not significantly different, but bpMRI was more specific than mpMRI at cutoff scores of 3 (p = 0.02) and 4 (p = 0.02). The VI-RADS studies using primary transurethral resection of bladder tumors (TURBT) as the reference standard had significantly higher sensitivities (p < 0.001) than those using secondary TURBT or radical cystectomy as the reference.
Data conclusion
BpMRI and conventional VI-RADS had similar diagnostic efficacies for MIBC. Since MRI overestimated MIBC diagnoses using primary TURBT as the reference standard, we recommend using secondary TURBT as the reference standard.
Key Points
• Biparametric MRI without DCE had similar diagnostic efficacies for MIBC compared with conventional VI-RADS.
• The sensitivity of VI-RADS was overestimated when referring to the primary TURBT results.
• Biparametric MRI comprised of T2WI and DWI could be used for detecting MIBC in clinical practice.





Similar content being viewed by others
Abbreviations
- AUC:
-
Area under the curve
- BC:
-
Bladder cancer
- BpMRI:
-
Biparametric magnetic resonance imaging
- DCE:
-
Dynamic contrast enhancement
- DWI:
-
Diffusion-weighted imaging
- HsROC:
-
Hierarchical summary receiver operating characteristic curve
- MIBC:
-
Muscle-invasive bladder cancer
- mpMRI:
-
Multiparametric magnetic resonance imaging
- NMIBC:
-
Non-muscle-invasive bladder cancer
- NPV:
-
Negative predictive value
- PPV:
-
Positive predictive value
- QUADAS-2:
-
Quality Assessment of Diagnostic Accuracy Studies-2
- RC:
-
Radical cystectomy
- T2WI:
-
T2-weighted imaging
- TURBT:
-
Transurethral resection of bladder tumor
- VI-RADS:
-
Vesical Imaging Reporting and Data System
References
Sung H, Ferlay J, Siegel RL et al (2021) Global Cancer Statistics 2020: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries. CA Cancer J Clin 71:209–249. https://doi.org/10.3322/caac.21660
Panebianco V, Narumi Y, Altun E et al (2018) Multiparametric magnetic resonance imaging for bladder cancer: development of VI-RADS (Vesical Imaging-Reporting And Data System). Eur Urol 74:294–306. https://doi.org/10.1016/j.eururo.2018.04.029
Valera P, Flavio B, de Haas RJ et al (2016) Improving staging in bladder cancer: the increasing role of multiparametric magnetic resonance imaging. Eur Urol Focus 2:113–121. https://doi.org/10.1016/j.euf.2016.04.010
Panebianco V, De Berardinis E, Barchetti G et al (2017) An evaluation of morphological and functional multi-parametric MRI sequences in classifying non-muscle and muscle invasive bladder cancer. Eur Radiol 27:3759–3766. https://doi.org/10.1007/s00330-017-4758-3
Green DA, Durand M, Gumpeni N et al (2012) Role of magnetic resonance imaging in bladder cancer: current status and emerging techniques. BJU Int 110:1463–1470. https://doi.org/10.1111/j.1464-410X.2012.11129.x
Woo S, Panebianco V, Narumi Y et al (2020) Diagnostic Performance of Vesical Imaging Reporting and Data System for the prediction of muscle-invasive bladder cancer: a systematic review and meta-analysis. Eur Urol Oncol 3:306–315. https://doi.org/10.1016/j.euo.2020.02.007
Divrik RT, Sahin AF, Yildirim U et al (2010) Impact of routine second transurethral resection on the long-term outcome of patients with newly diagnosed pT1 urothelial carcinoma with respect to recurrence, progression rate, and disease-specific survival: a prospective randomised clinical trial. Eur Urol 58:185–190. https://doi.org/10.1016/j.eururo.2010.03.007
Shindo T, Masumori N, Kitamura H et al (2014) Clinical significance of definite muscle layer in TUR specimen for evaluating progression rate in T1G3 bladder cancer: multicenter retrospective study by the Sapporo Medical University Urologic Oncology Consortium (SUOC). World J Urol 32:1281–1285. https://doi.org/10.1007/s00345-013-1205-1
Arita Y, Shigeta K, Akita H et al (2020) Clinical utility of the Vesical Imaging-Reporting and Data System for muscle-invasive bladder cancer between radiologists and urologists based on multiparametric MRI including 3D FSE T2-weighted acquisitions. Eur Radiol. https://doi.org/10.1007/s00330-020-07153-5
See Hyung K (2020) Validation of vesical imaging reporting and data system for assessing muscle invasion in bladder tumor. Abdom Radiol (NY) 45:491–498. https://doi.org/10.1007/s00261-019-02190-1
Hong SB, Lee NK, Kim S et al (2020) Vesical Imaging-Reporting and Data System for multiparametric MRI to predict the presence of muscle invasion for bladder cancer. J Magn Reson Imaging 52:1249–1256. https://doi.org/10.1002/jmri.27141
Wang H, Luo C, Zhang F et al (2019) Multiparametric MRI for bladder cancer: validation of VI-RADS for the detection of detrusor muscle invasion. Radiology 291:668–674. https://doi.org/10.1148/radiol.2019182506
Wang Z, Shang Y, Luan T et al (2020) Evaluation of the value of the VI-RADS scoring system in assessing muscle infiltration by bladder cancer. Cancer Imaging 20:26. https://doi.org/10.1186/s40644-020-00304-3
Delli Pizzi A, Mastrodicasa D, Marchioni M et al (2020) Bladder cancer: do we need contrast injection for MRI assessment of muscle invasion? A prospective multi-reader VI-RADS approach. Eur Radiol. https://doi.org/10.1007/s00330-020-07473-6
Ramalho M, Ramalho J, Burke LM, Semelka RC (2017) Gadolinium retention and toxicity-an update. Adv Chronic Kidney Dis 24:138–146. https://doi.org/10.1053/j.ackd.2017.03.004
Tedeschi E, Caranci F, Giordano F et al (2017) Gadolinium retention in the body: what we know and what we can do. Radiol Med (Torino) 122:589–600. https://doi.org/10.1007/s11547-017-0757-3
Moher D, Shamseer L, Clarke M et al (2015) Preferred reporting items for systematic review and meta-analysis protocols (PRISMA-P) 2015 statement. Syst Rev 4:1. https://doi.org/10.1186/2046-4053-4-1
Whiting PF (2011) QUADAS-2: a revised tool for the quality assessment of diagnostic accuracy studies. Ann Intern Med 155:529. https://doi.org/10.7326/0003-4819-155-8-201110180-00009
Ahn H, Hwang SIL, Lee HJ et al (2020) Quantitation of bladder cancer for the prediction of muscle layer invasion as a complement to the vesical imaging-reporting and data system. Eur Radiol. https://doi.org/10.1007/s00330-020-07224-7
Barchetti G, Simone G, Ceravolo I et al (2019) Multiparametric MRI of the bladder: inter-observer agreement and accuracy with the Vesical Imaging-Reporting and Data System (VI-RADS) at a single reference center. Eur Radiol 29:5498–5506. https://doi.org/10.1007/s00330-019-06117-8
Del Giudice F, Barchetti G, De Berardinis E et al (2020) Prospective Assessment of Vesical Imaging Reporting and Data System (VI-RADS) and its clinical impact on the management of high-risk non-muscle-invasive bladder cancer patients candidate for repeated transurethral resection. Eur Urol 77:101–109. https://doi.org/10.1016/j.eururo.2019.09.029
Liu S, Xu F, Xu T et al (2020) Evaluation of Vesical Imaging-Reporting and Data System (VI-RADS) scoring system in predicting muscle invasion of bladder cancer. Transl Androl Urol 9:445–451. https://doi.org/10.21037/tau.2020.02.16
Makboul M, Farghaly S, Abdelkawi IF (2019) Multiparametric MRI in differentiation between muscle invasive and non-muscle invasive urinary bladder cancer with vesical imaging reporting and data system (VI-RADS) application. Br J Radiol 92:20190401. https://doi.org/10.1259/bjr.20190401
Marchioni M, Primiceri G, Delli Pizzi A et al (2020) Could bladder multiparametric MRI be introduced in routine clinical practice? Role of the new VI-RADS score: results from a prospective study. Clin Genitourin Cancer 18:409–415.e1. https://doi.org/10.1016/j.clgc.2020.03.002
Sakamoto K, Ito M, Ikuta S et al (2020) Detection of muscle-invasive bladder cancer on biparametric MRI using vesical imaging-reporting and data system and apparent diffusion coefficient values (VI-RADS/ADC). Bladder Cancer 6:161–169. https://doi.org/10.3233/BLC-190267
Ueno Y, Tamada T, Takeuchi M et al (2020) Vesicle Imaging and Data Reporting System (VI-RADS): multi-institutional multi-reader diagnostic accuracy and inter-observer agreement study. AJR Am J Roentgenol. https://doi.org/10.2214/AJR.20.23604
Metwally MI, Zeed NA, Hamed EM et al (2021) The validity, reliability, and reviewer acceptance of VI-RADS in assessing muscle invasion by bladder cancer: a multicenter prospective study. Eur Radiol. https://doi.org/10.1007/s00330-021-07765-5
Etxano J, Rodríguez-Vigil B, Pérez F et al (2021) Vesical Imaging-Reporting and Data System (VI-RADS®): experiencia inicial en la clasificación del cáncer de vejiga músculo-infiltrante. Actas Urol Esp 45:320–325. https://doi.org/10.1016/j.acuro.2020.10.004
Akcay A, Yagci AB, Celen S et al (2021) VI-RADS score and tumor contact length in MRI: a potential method for the detection of muscle invasion in bladder cancer. Clin Imaging 77:25–36. https://doi.org/10.1016/j.clinimag.2021.02.026
Soichiro Y, Hiroshi T, Toshiki K et al (2019) Staging accuracy of vesical imaging-reporting and data system (VI-RADS) for bladder cancer. J Urol e1161. https://doi.org/10.1097/01.JU.0000557402.79313.bd
Bandini M, Calareso G, Raggi D et al (2020) The value of multiparametric magnetic resonance imaging sequences to assist in the decision making of muscle-invasive bladder cancer. Eur Urol Oncol 4(5):829–833. https://doi.org/10.1016/j.euo.2020.06.004
Iztok C, Valeria P, Hebert AV et al (2020) MRI of bladder cancer: local and nodal staging. J Magn Reson Imaging 52:649–667. https://doi.org/10.1002/jmri.27090
Patel M, Atyani A, Salameh J-P et al (2020) Safety of intrathecal administration of gadolinium-based contrast agents: a systematic review and meta-analysis. Radiology 297:75–83. https://doi.org/10.1148/radiol.2020191373
Barentsz JO, Jager GJ, van Vierzen PB et al (1996) Staging urinary bladder cancer after transurethral biopsy: value of fast dynamic contrast-enhanced MR imaging. Radiology 201:185–193. https://doi.org/10.1148/radiology.201.1.8816542
Wang H, Pui MH, Guo Y et al (2014) Diffusion-weighted MRI in bladder carcinoma: the differentiation between tumor recurrence and benign changes after resection. Abdom Imaging 39:135–141. https://doi.org/10.1007/s00261-013-0038-0
Nguyen HT, Jia G, Shah ZK et al (2015) Prediction of chemotherapeutic response in bladder cancer using K-means clustering of dynamic contrast-enhanced (DCE)-MRI pharmacokinetic parameters: chemotherapeutic response in bladder cancer. J Magn Reson Imaging 41:1374–1382. https://doi.org/10.1002/jmri.24663
Schrier BP, Peters M, Barentsz JO, Witjes JA (2006) Evaluation of chemotherapy with magnetic resonance imaging in patients with regionally metastatic or unresectable bladder cancer. Eur Urol 49:698–703. https://doi.org/10.1016/j.eururo.2006.01.022
Donaldson SB, Bonington SC, Kershaw LE et al (2013) Dynamic contrast-enhanced MRI in patients with muscle-invasive transitional cell carcinoma of the bladder can distinguish between residual tumour and post-chemotherapy effect. Eur J Radiol 82:2161–2168. https://doi.org/10.1016/j.ejrad.2013.08.008
Barentsz JO, Berger-Hartog O, Witjes JA et al (1998) Evaluation of chemotherapy in advanced urinary bladder cancer with fast dynamic contrast-enhanced MR imaging. Radiology 207:791–797. https://doi.org/10.1148/radiology.207.3.9609906
Babjuk M, Burger M, Compérat EM et al (2019) European association of urology guidelines on non-muscle-invasive bladder cancer (TaT1 and carcinoma in situ) - 2019 update. Eur Urol 76:639–657. https://doi.org/10.1016/j.eururo.2019.08.016
Naselli A, Hurle R, Paparella S et al (2018) Role of restaging transurethral resection for T1 non–muscle invasive bladder cancer: a systematic review and meta-analysis. Eur Urol Focus 4:558–567. https://doi.org/10.1016/j.euf.2016.12.011
Cumberbatch MGK, Foerster B, Catto JWF et al (2018) Repeat transurethral resection in non-muscle-invasive bladder cancer: a systematic review. Eur Urol 73:925–933. https://doi.org/10.1016/j.eururo.2018.02.014
Brausi M, Collette L, Kurth K et al (2002) Variability in the recurrence rate at first follow-up cystoscopy after TUR in stage Ta T1 transitional cell carcinoma of the bladder: a combined analysis of seven EORTC studies. Eur Urol 41:523–531. https://doi.org/10.1016/S0302-2838(02)00068-4
Herr HW (1999) The value of a second transurethral resection in evaluating patients with bladder tumors. J Urol 162:74–76. https://doi.org/10.1097/00005392-199907000-00018
Sugihara T, Yasunaga H, Horiguchi H et al (2014) Comparison of perioperative outcomes including severe bladder injury between monopolar and bipolar transurethral resection of bladder tumors: a population based comparison. J Urol 192:1355–1359. https://doi.org/10.1016/j.juro.2014.05.100
Venkatramani V, Panda A, Manojkumar R, Kekre NS (2014) Monopolar versus bipolar transurethral resection of bladder tumors: a single center, parallel arm, randomized, controlled trial. J Urol 191:1703–1707. https://doi.org/10.1016/j.juro.2013.12.004
Mariappan P, Zachou A, Grigor KM (2010) Detrusor muscle in the first, apparently complete transurethral resection of bladder tumour specimen is a surrogate marker of resection quality, predicts risk of early recurrence, and is dependent on operator experience. Eur Urol 57:843–849. https://doi.org/10.1016/j.eururo.2009.05.047
Dutta SC, Smith JAJ, Shappell SB et al (2001) Clinical under staging of high risk nonmuscle invasive urothelial carcinoma treated with radical cystectomy. J Urol 166:490–493. https://doi.org/10.1097/00005392-200108000-00019
Zhou G, Chen X, Zhang J et al (2014) Contrast-enhanced dynamic and diffusion-weighted MR imaging at 3.0 T to assess aggressiveness of bladder cancer. Eur J Radiol 83:2013–2018. https://doi.org/10.1016/j.ejrad.2014.08.012
Chang KJ, Kamel IR, Macura KJ, Bluemke DA (2008) 3.0-T MR imaging of the abdomen: comparison with 1.5 T. Radiographics 28:1983–1998. https://doi.org/10.1148/rg.287075154
Funding
National Science Foundation of China Youth Fund (No. 31801066)
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflict of interest
The authors of this manuscript declare no relationships with any companies whose products or services may be related to the subject matter of the article.
Statistics and biometry
One of the authors has significant statistical expertise.
Informed consent
Written informed consent was not required for this study because this study was a meta-analysis.
Ethics approval
Institutional Review Board approval was not required because this study was a meta-analysis.
Methodology
• Retrospective
• Diagnostic or prognostic study
• Performed at one institution
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
This study was conducted at West China Hospital, Sichuan University, Chengdu, China.
Supplementary information
ESM 1
(DOCX 465 kb)
Rights and permissions
About this article
Cite this article
Ye, L., Chen, Y., Xu, H. et al. Biparametric magnetic resonance imaging assessment for detection of muscle-invasive bladder cancer: a systematic review and meta-analysis. Eur Radiol 32, 6480–6492 (2022). https://doi.org/10.1007/s00330-022-08696-5
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00330-022-08696-5