Abstract
Objective
To evaluate whether apparent diffusion coefficient (ADC) values can predict the status of MGMT of glioblastoma multiforme (GBM) and correlate with overall survival (OS) and progression-free survival (PFS).
Methods
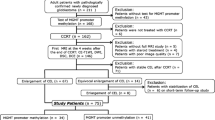
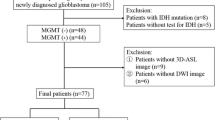
This retrospective study included 47 patients with pathologically proven glioblastoma. All of them underwent MR DWI study before surgery (mean time 1 week) and the status of methylguanine-DNA-methyltransferase (MGMT) promoter methylation was searched for. Minimum apparent diffusion coefficient (ADC) values were evaluated. OS and PSF parameters were calculated, and Student’s t-test, Kaplan-Meier curves, linear and Cox regression were performed.
Results
Twenty-five patients showed positive methylation of the MGMT promoter. Patients showing MGMT promoter methylation had higher minimum ADC values, and they survived longer than those without MGMT promoter methylation. The median ADCmin value of 0.80 represents the cutoff value able to distinguish between methylated and un-methylated patients. Patients showing minimum ADC values higher than 0.80 survived longer than patients with minimum ADC values lower than 0.80. A linear correlation between minimum ADC values vs. the OS and PFS was observed.
Conclusions
Minimum ADC values in glioblastoma multiforme could be used as a preoperative parameter to estimate the status of MGMT promoter methylation and the survival of patients.
Key Points
• Diffusion-weighted MR imaging (DWI) provides new insights into glioblastoma multiforme (GBM)
• DWI ADCmin values can predict the methylation status of MGMT promoter.
• The MGMT promoter methylation group survived longer than the unmethylated group.
• Patients with high ADCmin values survived longer than patients with low values.






Similar content being viewed by others
Abbreviations
- RT:
-
Radiotherapy
- MGMT:
-
Methylguanine-DNA-methyltransferase
- PFS:
-
Progression-free survival
- OS:
-
Overall survival
- ADC:
-
Apparent diffusion coefficient
- DWI:
-
Diffusion-weighted images
- GBM:
-
Glioblastoma multiforme
- TMZ:
-
Temozolomide
- MPRAGE:
-
Magnetisation-prepared rapid acquisition gradient echo
- ROC:
-
Received operating characteristic
- ROI:
-
Region of interest
- FLAIR:
-
Fluid attenuated inversion recovery
- PCR:
-
Polymerase chain reaction
- FA:
-
Fractional anisotropy
References
Hegi E, Diserens AC, Godard S et al (2004) Clinical trial substantiates the predictive value of O-6 methylguanine—DNA methyltransferase promoter methylation in glioblastoma patients treated with temozolomide. Clin Cancer Res 6:1871–1874
Rivera AL, Pelloski CE, Gilbert MR et al (2010) MGMT promoter methylation is predictive of response to radiotherapy and prognostic in the absence of adjuvant alkylating chemotherapy for glioblastoma. Neurooncology 2:116–121
Hegi ME, Diserens AC, Gorlia T et al (2005) MGMT gene silencing and benefit from temozolomide in glioblastoma. N Engl J Med 10:997–1003
Paz MF, Yaya-Tur R, Rojas-Marcos I et al (2004) CpG island hypermethylation of the DNA repair enzyme methyltransferase predicts response to temozolomide in primary gliomas. Clin Cancer Res 10:4933–4938
Idbaih A, Omuro A, Ducray F, Hoang-Xuan K (2007) Molecular genetic markers as predictors of response to chemotherapy in gliomas. Curr Opin Oncol 19:606–611
Eoli M, Menghi F, Bruzzone MG, De Simone T, Valletta L (2007) Methylation of O6-methylguanine DNA methyltransferase and loss of heterozygosity on 19q and/or 17p are overlapping features of secondary glioblastomas with prolonged survival. Clin Cancer Res 9:2606–2613
Hegi ME, Liu L, Herman JG et al (2008) Correlation of O6-methylguanine methyltransferase (MGMT) promoter methylation with clinical outcomes in glioblastoma and clinical strategies to modulate MGMT activity. J Clin Oncol 25:4189–4199
Weller M, Stupp R, Reifenberger G et al (2010) MGMT promoter methylation in malignant gliomas: ready for personalized medicine? Nat Rev Neurol 6:39–51
Arvinda HR, Kesavadas C, Sarma PS et al (2009) Glioma grading: sensitivity, specificity, positive and negative predictive values of diffusion and perfusion imaging. J Neurooncol 94:87–96
Barajas RF, Hodgson G, Chang JS, Vandenberg SR, Yeh RF, Parsa AT (2010) Glioblastoma multiforme regional genetic and cellular expression patterns: Influence on anatomic and physiologic MR imaging. Radiology 2:564–576
Oh J, Henry RG, Pirzkall P et al (2004) Survival analysis in patients with glioblastoma multiforme: predictive value of choline to N-acetylaspartate index, apparent diffusion coefficient, and relative cerebral blood volume. J Magn Reson Imaging 19:546–554
Higano S, Yun X, Kumabe T, Watanabe M, Mugikura S (2006) Malignant astrocytic tumors: clinical importance of apparent diffusion coefficient in prediction of grade and prognosis. Radiology 3:839–846
Moon WJ, Choi JW, Roh HG, Lim SD, Koh YC (2012) Imaging parameters of high grade gliomas in relation to the MGMT promoter methylation status: the CT, diffusion tensor imaging, and perfusion MR imaging. Neuroradiology 54:555–563 y
MacDonald DR, Cascino TL, Schold SC et al (1990) Response criteria for phase II studies of supratentorial malignant glioma. J Clin Oncol 8:1277–1280
Chamberlain MC, Glantz MJ, Chalmers L, Van Horn A, Sloan AE (2007) Early necrosis following concurrent Temodar and radiotherapy in patients with glioblastoma. J Neurooncol 82:81–83
Paz MF, Yaya-Tur R, Rojas-Marcos I et al (2004) CpG island hypermethylation of the DNA repair enzyme methyltransferase predicts response to temozolomide in primary gliomas. Clin Cancer Res 15:4933–4938
Minniti G, Amelio D, Amichetti M et al (2010) Patterns of failure and comparison of different target volume delineations in patients with glioblastoma treated with conformal radiotherapy plus concomitant and adjuvant temozolomide. Radiother Oncol 3:377–381
Rock K, McArdle O, Forde P et al (2012) A clinical review of treatment outcomes in glioblastoma multiforme. The validation in a non-trial population of the results of a randomised phase III clinical trial: has a more radical approach improved survival? Br J Radiol. doi:10.1259/bjr/83796755
Gerson SL (2002) Clinical relevance of MGMT in the treatment of cancer. J Clin Oncol 20:2388–2399
Silber JR, Blank A, Bobola MS et al (1999) O6-Methylguanine-DNA methyltransferase-deficient phenotype in human gliomas: Frequency and time to tumor progression after alkylating agent-based chemotherapy. Clin Cancer Res 5:807–814
Murakami R, Sugahara T, Nakamura H, Hirai T, Kitajima M, Hayashida Y (2007) Malignant supratentorial astrocytoma treated with postoperative radiation therapy: prognostic value of pretreatment quantitative diffusion-weighted MR imaging. Radiology 2:493–499
Bulakbasi N, Guvenc I, Onguru O et al (2004) The added value of the apparent diffusion coefficient calculation to magnetic resonance imaging in the differentiation and grading of malignant brain tumors. J Comput Assist Tomogr 28:735–746
Yang D, Korogi Y, Sugahara T et al (2002) Cerebral gliomas: prospective comparison of multivoxel 2D chemical-shift proton MR spectroscopy, echoplanar perfusion and diffusion-weighted MRI. Neuroradiology 44:656–666
Yamasaki F, Kurisu K, Satoh K et al (2005) Apparent diffusion coefficient of human brain tumors at MR imaging. Radiology 235:985–991
Watanabe T, Katayama Y, Komine C et al (2005) O6-methylguanine-DNA methyltransferase methylation and TP53 mutation in malignant astrocytomas and their relationships with clinical course. Int J Cancer 113:581–587
Brandes AA, Franceschi E, Tosoni A et al (2008) MGMTpromoter methylation status can predict the incidence and outcome of pseudoprogression after concomitant radiochemotherapy in newly diagnosed glioblastoma patients. J Clin Oncol 26:2192–2197
Taal W, Brandsma D, de Bruin HG et al (2008) Incidence of early pseudo-progression in a cohort of malignant glioma patients treated with chemoirradiation with temozolomide. Cancer 113:405–410
Brandes AA, Tosoni A, Spagnolli F et al (2008) Disease progression or pseudoprogression after concomitant radiochemotherapy treatment: pitfalls in neurooncology. J Neurooncol 10:361–367
Drabycz S, Roldán G, De Robles P et al (2010) An analysis of image texture, tumour location, and MGMT promoter methylation in glioblastoma using magnetic resonance imaging. NeuroImage 2:1398–1405
Sugahara T, Korogi Y, Kochi M et al (1999) Usefulness of diffusion-weighted MRI with echo-planar technique in the evaluation of cellularity in gliomas. J Magn Reson Imaging 9:53–60
Gupta RK, Cloughesy TF, Sinha U et al (2000) Relationships between choline magnetic resonance spectroscopy, apparent diffusion coefficient and quantitative histopathology in human glioma. J Neurooncol 50:215–226
Pope WB, Qiao XJ, Kim HJ et al (2012) Apparent diffusion coefficient histogram analysis stratifies progression-free and overall survival in patients with recurrent GBM treated with bevacizumab: a multi-center study. J Neurooncol 108:491–498
Calli C, Kitis O, Yunten N, Yurtseven T, Islekel S et al (2006) Perfusion and diffusion MR imaging in enhancing malignant cerebral tumors. Eur J Radiol 3:394–403
Kono K, Inoue Y, Nakayam K et al (2001) The role of diffusion-weighted imaging in patients with brain tumors. AJNR Am J Neuroradiol 22:1081–1088
Acknowledgement
Beatrice Bozzao, English editing.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Romano, A., Calabria, L.F., Tavanti, F. et al. Apparent diffusion coefficient obtained by magnetic resonance imaging as a prognostic marker in glioblastomas: correlation with MGMT promoter methylation status. Eur Radiol 23, 513–520 (2013). https://doi.org/10.1007/s00330-012-2601-4
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00330-012-2601-4