Abstract
Objectives
Triple-negative (ER-/PR-/HER2-) breast carcinomas (TNBC) are aggressive tumours with underexplored imaging features. This study investigates whether their vascular characteristics as assessed by dynamic contrast-enhanced (DCE) and dynamic susceptibility contrast-enhanced (DSC) MRI are distinct from the prognostically more favourable ER+/PR+/HER2- cancers.
Methods
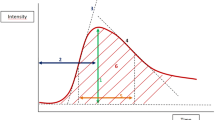
Patients with primary breast cancer underwent MRI before neoadjuvant chemotherapy and were identified as ER-/PR-/HER2- or ER+/PR+/HER2- from core biopsy specimens. MRI parameters reflecting tissue perfusion, permeability, and extracellular leakage space were measured. Values for inflow transfer constant (Ktrans), outflow rate constant (kep), leakage space (ve), area under the gadolinium curve (IAUGC60 ), relative blood volume (rBV) and flow (rBF), and Mean Transit Time (MTT) were compared across receptor status and with known prognostic variables.
Results
Thirty seven patients were assessable in total (16 ER-/PR-/HER2-, 21 ER+/PR+/HER2-). Lower ve (p = 0.001), shorter MTT (p = 0.007) and higher kep values (p = 0.044) were observed in TNBC. ve was lower across all T stages, node-negative (p = 0.004) and low-grade TNBC (p = 0.037). ve was the best predictor of triple negativity (ROC AUC 0.80).
Conclusions
TNBC possess characteristic features on imaging, with lower extracellular space (higher cell density) and higher contrast agent wash-out rate (higher vascular permeability) suggesting a distinctive phenotype detectable by MRI.


Similar content being viewed by others
Abbreviations
- bFGF:
-
Basic fibroblast growth factor
- CALGB:
-
Cancer and Leukemia group B
- DCE-MRI:
-
Dynamic contrast-enhanced MRI
- DSC-MRI:
-
Dynamic susceptibility contrast-enhanced MRI
- ECM:
-
Extracellular matrix
- ER:
-
Oestrogen receptor
- FISH:
-
Fluorescence in-situ hybridisation
- Gd-DTPA:
-
Gadopentetate dimeglumine
- HER2:
-
Human epidermal growth factor receptor-2
- IAUGC60 :
-
Initial area under the gadolinium curve after the first 60 s
- kep :
-
Outflow rate constant
- Ktrans :
-
Inflow transfer constant
- MRI:
-
Magnetic resonance imaging
- MTT:
-
Mean transit time
- NAC:
-
Neoadjuvant chemotherapy
- PET-CT:
-
Positron emission tomography-computed tomography
- PR:
-
Progesterone receptor
- rBF:
-
Relative blood flow
- rBV:
-
Relative blood volume
- ROC:
-
Receiver operating curve characteristic
- TE:
-
Echo time
- TNBC:
-
Triple-negative breast carcinomas
- TNM:
-
Tumour, node, metastasis
- TR:
-
Repetition time
- ve :
-
Leakage space
- VEGF:
-
Vascular endothelial growth factor
References
Irvin WL Jr, Carey LA (2008) What is triple-negative breast cancer? Eur J Cancer 44:2799–2805
Bosch A, Erole P, Zaragoza R, Vina JR, Lluch A (2010) Triple-negative breast cancer: molecular features, pathogenesis, treatment and current lines of research. Cancer Treat Rev 36:206–215
Perou CM, Sorlie T, Eisen MB, van de Rijn M, Jeffrey SS, Rees CA, Pollack JR, Ross DT, Johnsen H, Akslen LA, Fluge O, Pergamenschikov A, Williams C, Zhu SX, Lonning PE, Borresen-Dale A-L, Brown PO, Botstein D (2000) Molecular portraits of human breast tumours. Nature 406:747–752
Sorlie T, Perou CM, Tibshirani R, Aas T, Geisler S, Johnsen H, Hastie T, Eisen MB, van de Rijn M, Jeffrey SS, Thorsen T, Quist H, Matese JC, Brown PO, Botstein D, Eystein Lønning P, Børresen-Dale AL (2001) Gene expression patterns of breast carcinomas distinguish tumor subclasses with clinical implications. Proc Natl Acad Sci USA 98:10869–10874
Rakha EA, Ellis IO (2009) Triple-negative/basal-like breast cancer: a review. Pathology 41(1):40–47
Kreike B, van de Vijver MJ (2007) Are triple-negative tumours and basal-like breast cancer synonymous? Breast Cancer Res 9:405
Collins DJ, Padhani AR (2004) Dynamic magnetic resonance imaging of tumor perfusion. Approaches and biomedical challenges. IEEE Eng Med Biol Mag 23:65–83
Chen JH, Agrawal G, Feig B, Baek HM, Carpenter PM, Mehta RS, Nalcioglu O, Su M-Y (2007) Triple-negative breast cancer: MRI features in 29 patients. Ann Oncol 18:2042–2043, Letters to the editor
Basu S, Chen W, Tchou J, Mavi A, Cermik T, Czerniecki B, Schnall M, Alavi A (2008) Comparison of triple-negative and estrogen receptor-positive/progesterone receptor-positive/HER2-negative breast carcinoma using quantitative fluorine-18 fluorodeoxyglucose/positron emission tomography imaging parameters. Cancer 112:995–1000
Ah-See MW, Makris A, Taylor NJ, Harrison M, Richman PI, Burcombe RJ, Stirling JJ, d’Arcy JA, Collins DJ, Pittam MR, Ravichandran D, Padhani AR (2008) Early changes in functional dynamic magnetic resonance imaging predict for pathologic response to neoadjuvant chemotherapy in primary breast cancer. Clin Cancer Res 14:6580–6589
Sobin LH, Wittekind C (2002) TNM classification of malignant tumours. Wiley-Liss, UICC, New York
Bloom HJG, Richardson WW (1957) Histological grading and prognosis in breast cancer. Br J Cancer 11:359–377
Harvey JM, Clark GM, Osborne CK, Allred DC (1999) Estrogen receptor status by immunohistochemistry is superior to the ligand-binding assay for predicting response to adjuvant endocrine therapy in breast cancer. J Clin Oncol 17:1474–1481
Parker GJM, Suckling J, Tanner SF, Padhani AR, Revell PB, Husband JE, Leach MO (1997) Probing tumor microvascularity by measurement, analysis and display of contrast agent uptake kinetics. JMRI 7:564–574
Galbraith SM, Lodge MA, Taylor NJ, Rustin GJS, Bentzen S, Stirling JJ, Padhani AR (2002) Reproducibility of dynamic contrast-enhanced MRI in human muscles and tumours: comparison of quantitative and semi-quantitative analysis. NMR Biomed 15:132–142
d’Arcy JA, Collins DJ, Padhani AR, Walker-Samuel S, Suckling J, Leach MO (2006) Magnetic resonance imaging workbench (MRIW): dynamic contrast enhanced MRI data analysis and visualisation. Radiographics 26:621–632
Tofts PS, Berkowitz B, Schnall MD (1995) Quantitative analysis of dynamic Gd-DTPA enhancement in breast tumor using a permeability model. Magn Reson Med 33:564–568
Fritz-Hansen T, Rostrup E, Larsson HB, Sondergaard L, Ring P, Henriksen O (1996) Measurement of the arterial concentration of Gd-DTPA using MRI: a step toward quantitative perfusion imaging. Magn Reson Med 36:225–231
Walker-Samuel S, Leach MO, Collins DJ (2006) Evaluation of response to treatment using DCE-MRI: the relationship between initial area under the gadolinium curve (IAUGC) and quantitative pharmacokinetic analysis. Phys Med Biol 51:3593–3602
Walker-Samuel S, Parker C, Leach MO, Collins DJ (2007) Reproducibility of reference tissue quantification of dynamic contrast-enhanced data: comparison with a fixed vascular input function. Phys Med Biol 52:75–89
Livasy CA, Karaca G, Nanda R, Tretiakova MS, Olopade OI, Moore DT, Perou CM (2006) Phenotypic evaluation of the basal-like subtype of invasive breast carcinoma. Mod Pathol 19:264–271
Fulford LG, Easton DF, Reis-Filho JS, Sofronis A, Gillett CE, Lakhani SR, Hanby A (2006) Specific morphological features predictive for the basal phenotype in grade 3 invasive ductal carcinoma of the breast. Histopathology 49:22–34
Gluz O, Liedtke C, Gottschalk N, Pusztai L, Nitz U, Harbeck N (2009) Triple-negative breast cancer-current status and future directions. Ann Oncol 20:1913–1927
Ko ES, Lee BH, Kim HA, Noh WC, Kim MS, Lee SA (2010) Triple-negative breast cancer: correlation between imaging and pathological findings. Eur Radiol 20:1111–1117
Uematsu T, Kasami M, Yuen S (2009) Triple-negative breast cancer: correlation between MR imaging and pathologic findings. Radiology 250:638–647
Tchou J, Wang L-P, Sargen M, Sonnad S, Tomaszewski J, Schnall M (2006) Do triple-negative breast cancers have a distinct imaging phenotype? [abstract]. Breast Cancer Res Treat 100:s128
Miles KA, Williams RE (2008) Warburg revisited: imaging tumour blood flow and metabolism. Cancer Imaging 8:81–86
Bergamaschi A, Tagliabue E, Sorlie T, Naume B, Triulzi T, Orlandi R, Russnes HG, Nesland JM, Tammi R, Auvinen P, Kosma VM, Ménard S, Borresen-Dale AL (2008) Extracellular matrix signature identified breast cancer subgroups with different clinical outcome. J Pathol 214:357–367
Foulkes WD, Brunet JS, Stefansson IM, Straume O, Chappuis PO, Begin LR, Hamel N, Goffin JR, Wong N, Trudel M, Kapusta L, Porter P, Akslen LA (2004) The prognostic implication of the basal-like (cyclin E high/p27 low/p53+/glomeruloid-microvasular proliferation+) phenotype of BRCA1-related breast cancer. Cancer Res 64:830–835
Linderholm BK, Hellborg H, Johansson U, Ellmberger G, Skoog L, Lehtio J, Lewensohn R (2009) Significantly higher levels of vascular endothelial growth factor (VEGF) and shorter survival times for patients with primary operable triple-negative breast cancer. Ann Oncol 20:1639–1646
Linderholm BK, Lindahl T, Holmberg L, Klaar S, Lennerstrand J, Henriksson R, Bergh J (2001) The expression of vascular endothelial growth factor correlates with mutant p53 and poor prognosis in human breast cancer. Cancer Res 61:5407–5414
Greenberg A, Rugo HS (2010) Triple-negative breast cancer: role of antiangiogenic agents. Cancer J 16:33–38
Shi YH, Bingle L, Gong LH, Wang YX, Corke KP, Fang WG (2007) Basic FGF augments hypoxia induced HIF-1 alpha expression and VEGF release in T47D breast cancer cells. Pathology 39:396–400
Raghunand N, Gatenby RA, Gillies RJ (2003) Microenvironmental and cellular consequences of altered blood flow in tumours. Br J Radiol 76:S11–S22
Miles D, Chan A, Romieu G, Dirix LY, Cortes J, Pivot X, Tomczak P, Juozaityte E, Harbeck N, Steger GG, the BO17708 Study Group (2009) Randomized, double-blind, placebo-controlled, phase III study of bevacizumab with docetaxel or docetaxel with placebo as first-line therapy for patients with locally recurrent or metastatic breast cancer (mBC) [abstract]. 32nd San Antonio Breast Cancer Symposium. Available at http://www.sabcs.org/Newsletter/Docs/SABCS_2009_Issue1.pdf. Accessed 23.9.2010
O’Shaughnessy J, Dieras V, Glaspy J, Brufsky A, Miller K, Miles D, Koralewski P, Phan S, Bhattacharya S (2009) Comparison of subgroup analyses of PFS from three phase II studies of bevacizumab in combination with chemotherapy in patients with HER2-negative metastatic breast cancer (MBC) [abstract]. Cancer Res 69:s207
Miller K, Wang M, Gralow J, Dickler M, Cobleigh M, Perez EA, Shenkier T, Cella D, Davidson NE (2007) Paclitaxel plus bevacizumab versus paclitaxel alone for metastatic breast cancer. N Engl J Med 357:2666–2676
Robert N, Dieras V, Glaspy J, Brufsky A, Bondarenko I, Lipatov O, Perez E, Yardley D, Phan S, Bhattacharya S, O’Shaughnessy J (2009) Clinical benefit rate and time to response in RIBBON-1, a randomized, double-blind, phase III trial of chemotherapy with or without bevacizumab (B) for the first-line treatment of HER2-negative locally recurrent or metastatic breast cancer (MBC) [abstract]. Cancer Res 69:s6084
Baltzer PA, Vag T, Dietzel M, Beger S, Freiberg C, Gajda M, Camara O, Kaiser WA (2010) Computer-aided interpretation of dynamic magnetic resonance imaging reflects histopathology of invasive breast cancer. Eur Radiol 20(1):563–571
Dawson SJ, Provenzano E, Caldas C (2009) Triple negative breast cancers: clinical and prognostic implications. Eur J Cancer 45:27–40
Padhani AR, Liu G, Koh DM, Chenevert TL, Thoeny HC, Takahara T, Dzik-Jurasz A, Ross BD, Van Cauteren M, Collins D, Hammoud DA, Rustin GJ, Taouli B, Choyke PL (2009) Diffusion-weighted magnetic resonance imaging as a cancer biomarker: consensus and recommendations. Neoplasia 11:102–125
Li SP, Taylor NJ, Makris A, Ah-See ML, Beresford MJ, Stirling JJ, d’Arcy JA, Collins DJ, Padhani AR (2010) Primary human breast adenocarcinoma: imaging and histologic correlates of intrinsic susceptibility-weighted MR imaging before and during chemotherapy. Radiology 257:643–652, Epub 2010 Sep 21
Acknowledgements
This study was supported by a grant from the Breast Cancer Research Trust, United Kingdom.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Li, S.P., Padhani, A.R., Taylor, N.J. et al. Vascular characterisation of triple negative breast carcinomas using dynamic MRI. Eur Radiol 21, 1364–1373 (2011). https://doi.org/10.1007/s00330-011-2061-2
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00330-011-2061-2