Abstract
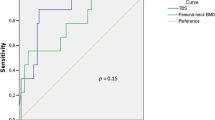
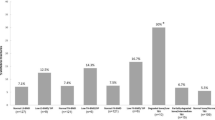
Ankylosing spondylitis (AS) patients have a high risk of osteoporotic fractures. The aim of this study was to evaluate the usefulness of trabecular bone score (TBS) in assessing fracture risk in patients with AS. 67 patients meeting the ASAS classification criteria were enrolled in the study. Fracture risk for each patient was assessed based on a lumbar spine exam encompassing bone mineral density (BMD), and TBS through a dual-energy X-ray absorptiometry (DXA) exam. In addition, each patient had an X-ray taken of their lumbar and thoracic spine to determine the presence of syndesmophytes and bony bridges, as well as spinous process and vertebral body fractures. Moreover, each patient's medical history was analyzed for other osteoporotic fractures. A major osteoporosis fracture (MOF) was found in 11 (16%) patients in total, of which 7 (10%) were vertebral body fractures. The mean TBS in patients with MOF and no MOF were, respectively, 1.12 and 1.29 (p < 0.001). No significant differences were found in BMD scores between the two groups. Syndesmophytes and bony bridges occurred more frequently in patients with MOF (p = 0.02). Age of 50 or more (RR = 9.86, p = 0.002), TBS score ≤ 1.31 (RR = 2.07, p < 0.0001), and presence of syndesmophytes and bony bridges (RR = 2.14, p = 0.04) were considered a relative risk (RR) increasing factors. TBS is a markedly more sensitive method of identifying patients with a high fracture risk compared to BMD measurement in a DXA exam in patients with AS.



Similar content being viewed by others
Open data sharing statement
Primary data of the study are available from the corresponding author upon reasonable request.
References
Østergaard M, Lambert RGW (2012) Imaging in ankylosing spondylitis. Ther Adv Musculoskelet Dis 4:301–311. https://doi.org/10.1177/1759720X11436240
Kekl AS, Corr M, Weisman MH (2016) Enthesitis. New insights into pathogenesis, diagnostic modalities, and treatment. Arthritis Rheumatol 68:312–322. https://doi.org/10.1002/art.39458
Sieper J, Braun J, Rudwaleit M, Boonen A, Zink A (2002) Ankylosing spondylitis: an overview. Ann Rheum Dis 61(Suppl 3):iii8–iii18. https://doi.org/10.1136/ard.61.suppl_3.iii8
Sun L, Rui W, Xue Q, Wang F, Lu P (2016) Risk factors of uveitis in ankylosing spondylitis. Medicine (Baltimore) 95:e4233. https://doi.org/10.1097/md.0000000000004233
Zhu W, He X, Cheng K, Chen D, Wang X, Qiu G, Cao X, Weng X (2019) Ankylosing spondylitis: etiology, pathogenesis, and treatments. Bone Res 7:22. https://doi.org/10.1038/s41413-019-0057-8
Kang KY, Kim IJ, Park SH, Hong YS (2018) Associations between trabecular bone score and vertebral fractures in patients with axial spondyloarthritis. Rheumatology (Oxford) 57:1033–1040. https://doi.org/10.1093/rheumatology/key027
Hans D, Goertzen A, Krieg MA, Leslie WD (2011) Bone microarchitecture assessed by TBS predicts osteoporotic fractures independent of bone density: the Manitoba study. J Bone Miner Res 26:2762–2769. https://doi.org/10.1002/jbmr.499
Gran TJ, Husby G (1993) The epidemiology of ankylosing spondylitis. Semin Arthritis Rheum 22:319–334. https://doi.org/10.1016/s0049-0172(05)80011-3
Richards C, Hans D, Leslie WD (2020) Trabecular Bone Score (TBS) predicts fracture in ankylosing spondylitis: the Manitoba BMD Registry. J Clin Densitom 23:543–548. https://doi.org/10.1016/j.jocd.2020.01.003
2019 ISCD Official Positions—Adult. https://iscd.org/wp-content/uploads/2021/09/2019-Official-Positions-Adult-1.pdf. Accessed 01 Mar 2022
Nam SW, Sung YK, Kim D, Cho SK, Song Y, Choi YY et al (2021) The usefulness of trabecular bone score in patients with ankylosing spondylitis. Korean J Intern Med 36:1211–1220. https://doi.org/10.3904/kjim.2020.065
Buehring B, Thomas J, Wittkämper T, Baraliakos X, Braun J (2020) Evaluation of the trabecular bone score (TBS) in routine clinical care of patients with inflammatory rheumatic and non-inflammatory diseases: correlation with conventional bone mineral density measurement and prevalence of vertebral fractures. Z Rheumatol 79:1067–1074. https://doi.org/10.1007/s00393-020-00764-9
Lim MIJ, Kang KY (2020) A contemporary view of the diagnosis of osteoporosis in patients with axial spondyloarthritis. Front Med (Lausanne) 7:569449. https://doi.org/10.3389/fmed.2020.569449
Nowakowska-Płaza A, Wroński J, Sudoł-Szopińska I, Głuszko P (2021) Trabecular Bone Score (TBS) in patients with early ankylosing spondylitis—limited utility. J Clin Med 10:5373. https://doi.org/10.3390/jcm10225373
Rudwaleit M, van der Heijde D, Landewe R, Listing K, Akkoc N, Brandt J et al (2009) The development of Assessment of SpondyloArthritis international Society classification criteria for axial spondyloarthritis (part II): validation and final selection. Ann Rheum Dis 68:777–783
Genant HK, Wu CY, van Kiujk X, Nevitt MC (1993) Vertebral fracture assessment using a semiquantitative technique. J Bone Miner Res 8:1137–1148. https://doi.org/10.1002/jbmr.5650080915
Chaudhary SB, Hullinger H, Vives MJ (2011) Management of acute spinal fractures in ankylosing spondylitis. ISRN Rheumatol 2011:150484. https://doi.org/10.5402/2011/150484
Lee SY, Song R, Hi Y, Chung SW, Lee YA, Hong SJ et al (2021) The bone bridge significantly affects the decrease in bone mineral density measured with quantitative computed tomography in ankylosing spondylitis. PLoS ONE 16:e0249578. https://doi.org/10.1371/journal.pone.0249578
Fatemi G, Gensler LS, Learch TJ, Weisman MH (2014) Spine fractures in ankylosing spondylitis: a case report and review of imaging as well as predisposing factors to falls and fractures. Semin Arthritis Rheum 44:20–24. https://doi.org/10.1016/j.semarthrit.2014.03.007
Zhao S, Thong D, Miller N, Duffield SJ, Hughes DM, Chadwick L et al (2018) The prevalence of depression in axial spondyloarthritis and its association with disease activity: a systematic review and meta-analysis. Arthritis Res Ther 20:140. https://doi.org/10.1186/s13075-018-1644-6
Hopkins C, Moulton C (2016) The prevalence of depression and its correlates in ankylosing spondylitis: a systematic review and meta-analysis. Eur Psychiatry 33:S166. https://doi.org/10.1016/j.eurpsy.2016.01.264
Kerr C, Bottomley C, Shingler S, Giangregorio L, de Freitas HM, Patel C et al (2017) The importance of physical function to people with osteoporosis. Osteoporos Int 28:1597–1607. https://doi.org/10.1007/s00198-017-3911-9
Lim MJ, Kang KY (2020) A contemporary view of the diagnosis of osteoporosis in patients with axial spondyloarthritis. Front Med (Lausanne) 7:569449. https://doi.org/10.3389/fmed.2020.569449
Sambrook PN, Geusens P (2012) The epidemiology of osteoporosis and fractures in ankylosing spondylitis. Ther Adv Musculoskelet Dis 4:287–292. https://doi.org/10.1177/1759720x12441276
Klingberg E, Lorentzon M, Göthlin J, Mellström D, Geijer M, Ohlsson C et al (2013) Bone microarchitecture in ankylosing spondylitis and the association with bone mineral density, fractures, and syndesmophytes. Arthritis Res Ther 15(6):R179. https://doi.org/10.1186/ar4368
Fauny M, Morizot C, Allado E, Verhoeven F, Albuisson E, Semaan M et al (2020) Consequences of spinal ankylosis on bone trabecular fragility assessed on CT scans in patients with ankylosing spondylitis. A retrospective study. Jt Bone Spine 87:625–631. https://doi.org/10.1016/j.jbspin.2020.05.009
Leslie WD, Aubry-Rozier B, Lamy O, Hans D (2013) TBS (trabecular bone score) and diabetes-related fracture risk. J Clin Endocrinol Metab 98:602–609. https://doi.org/10.1210/jc.2012-3118
Silva BC, Bilezikian JP (2014) Trabecular bone score: perspectives of an imaging technology coming of age. Arq Bras Endocrinol Metabol 58:493–503. https://doi.org/10.1590/0004-2730000003456
Caparbo VF, Furlam P, Saad CGS, Alvarenga JC, Aubry-Rozier B, Hans D et al (2019) Assessing bone impairment in ankylosing spondylitis (AS) using the trabecular bone score (TBS) and high-resolution peripheral quantitative computed tomography (HR-pQCT). Bone 122:8–13. https://doi.org/10.1016/j.bone.2019.01.024
Mann C, Ziegler K, Mews J, Plaschke M, Issever AS (2018) Bone mineral density assessment using iterative reconstruction compared with quantitative computed tomography as the standard of reference. Sci Rep 8:15095. https://doi.org/10.1038/s41598-018-33444-5
Fernandes BM, Garcia S, Ganhão S, Rato M, Pinheiro F, Bernardes M, Costa L (2020) Spondyloarthritis and fracture risk: does DXA really have an impact in the risk of fracture estimated by frax? Ann Rheum Dis 79:1181–1182
Funding
None.
Author information
Authors and Affiliations
Contributions
PZ study design, data collection, statistical analysis, data interpretation, manuscript preparation, literature search. MD study design, data collection, data interpretation, manuscript preparation, literature search. DJ data collection, manuscript preparation, literature search. MW-J data interpretation, manuscript preparation, literature search.
Corresponding author
Ethics declarations
Compliance with ethical standards
The study was approved by the bioethical commission: Uniwersytet Mikołaja Kopernika w Toruniu, Collegium Medicum im. L. Rydygiera w Bydgoszczy, Komisja Bioetyczna (study number: KB 771/2018, date of approval: 20/NOV/2018).
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Żuchowski, P., Dura, M., Jeka, D. et al. The applicability of trabecular bone score for osteoporosis diagnosis in ankylosing spondylitis. Rheumatol Int 42, 839–846 (2022). https://doi.org/10.1007/s00296-022-05109-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00296-022-05109-0