Abstract
Objective
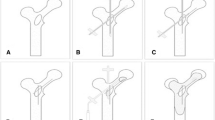
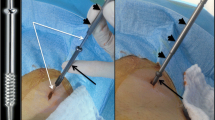
Percutaneous osteosynthesis plus cementoplasty (POPC) is a minimally invasive technique that has never been reported before and that we have prospectively evaluated for patients with impending pathological fracture of the proximal femur.
Methods
We performed POPC in 12 patients (3 males, 9 females) with metastasis of the proximal femur with a high risk of fracture (Mirels’ score ≥8) between February 2010 and July 2011. Patients were not candidates for standard surgical stabilization. We analyzed the feasibility, duration, and complication of the procedure, the risk of fracture, the decrease in pain (Visual Analog Scale, VAS), and length of stay in hospital. Data were prospectively collected in all patients.
Results
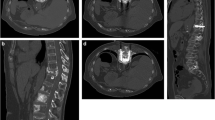
The mean Mirels’ score was 9.8 ± 1.2 (range, 8–11). The technical success was 100%. POPC was performed under general anesthesia (n = 6) or conscious sedation (n = 6). The mean duration was 110 ± 43 (range, 60–180) minutes. All patients stood up and walked the second day after the procedure. The average length of stay in the hospital was 4 ± 1.6 (range, 2–7) days. We experienced two hematomas in two patients and no thromboembolic complication. For symptomatic patients (n = 8), VAS decreased from 6.5/10 (range, 2–9) before treatment to 1/10 (range, 0–3) 1 month after. No fracture occurred after a median follow-up of 145 (range, 12–608) days.
Conclusions
POPC for impending pathological fracture of the proximal femur seems to be a promising alternative for cancer patients who are not candidates for surgical stabilization. Further studies are required to confirm this preliminary experience.



Similar content being viewed by others
References
Ward WG, Holsenbeck S, Dorey FJ et al (2003) Metastatic disease of the femur: surgical treatment. Clin Orthop Relat Res (415 Suppl): S230–S244
Popken F, Schmidt J, Oegur H et al (2002) Treatment outcome after surgical management of osseous breast carcinoma metastases. Preventive stabilization vs. management after pathological fracture. Unfallchirurg 105(4):338–343
Ristevski B, Jenkinson RJ, Stephen DJ et al (2009) Mortality and complications following stabilization of femoral metastatic lesions: a population-based study of regional variation and outcome. Can J Surg 52(4):302–308
Mirels H (1989) Metastatic disease in long bones. A proposed scoring system for diagnosing impending pathologic fractures. Clin Orthop Relat Res (249):256–264
Jawad MU, Scully SP (2010) In brief: classifications in brief: Mirels’ classification: metastatic disease in long bones and impending pathologic fracture. Clin Orthop Relat Res 468(10):2825–2827
Van der Linden YM, Dijkstra PD, Kroon HM et al (2004) Comparative analysis of risk factors for pathological fracture with femoral metastases. J Bone Joint Surg Br 86(4):566–573
Anselmetti GC, Manca A, Ortega C et al (2008) Treatment of extraspinal painful bone metastases with percutaneous cementoplasty: a prospective study of 50 patients. Cardiovasc Interv Radiol 31(6):1165–1173
Dayer R, Peter R (2008) Percutaneous cementoplasty complicating the treatment of a pathologic subtrochanteric fracture: a case report. Injury 39(7):801–804
Chang SW, Murphy KP (2005) Percutaneous CT-guided cementoplasty for stabilization of a femoral neck lesion. J Vasc Interv Radiol 16(6):889–890
Basile A, Giuliano G, Scuderi V et al (2008) Cementoplasty in the management of painful extraspinal bone metastases: our experience. Radiol Med 113(7):1018–1028
Schep NW, Heintjes RJ, Martens EP et al (2004) Retrospective analysis of factors influencing the operative result after percutaneous osteosynthesis of intracapsular femoral neck fractures. Injury 35(10):1003–1009
Conflict of interest
The authors declare that they have no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Deschamps, F., Farouil, G., Hakime, A. et al. Percutaneous Stabilization of Impending Pathological Fracture of the Proximal Femur. Cardiovasc Intervent Radiol 35, 1428–1432 (2012). https://doi.org/10.1007/s00270-011-0330-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00270-011-0330-8