Abstract
Purpose
To investigate the percutaneous endovascular management of visceral aneurysms (VA) and visceral pseudoaneurysms (VPA) treated in three European interventional radiology departments.
Methods
Patient archives from the department’s databases were examined and retrospectively analyzed. Patients diagnosed between 2000 and 2010 with VA and/or VPA, confirmed by computed tomography angiography, magnetic resonance angiography, or digital subtraction angiography and treated exclusively with percutaneous endovascular methods, were included in the study. The study’s primary end points were procedural technical success, target lesion reintervention rate, and periprocedural mortality rate. Secondary end points included major and minor complications rates.
Results
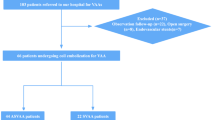
The medical records of 54 patients (41 male, mean age 55 ± 18.1 years) with 58 VAs or VPAs and treated with various percutaneous endovascular therapeutic modalities were analyzed. In total, 21 VAs (mean diameter 49.4 ± 21 mm, range 20–100 mm) and 37 VPAs (mean diameter 25.1 ± 14.6 mm, range 8–60 mm) were treated. Procedural technical success was achieved in 100% of the cases, while target lesion reintervention rate was 6.1% (2 of 33) and 14.2% (3 of 21) in the VPA and VA groups, respectively. Mean clinical follow-up period was 19.1 ± 21.4 months. Overall periprocedural mortality rate was 3% (1 of 33) in the VPA group and 0% (0 of 21) in the VA group.
Conclusion
Percutaneous endovascular treatment of VAs and VPAs is safe and effective with low morbidity and mortality. There is a small but significant reintervention rate, particularly for true aneurysms; dedicated follow-up imaging is recommended. Successful aneurysm exclusion was achieved in all cases with a second procedure.






Similar content being viewed by others
References
Hossain A, Reis ED, Dave SP et al (2001) Visceral artery aneurysms: experience in a tertiary-care center. Am Surg 67:432–437
Bedford PD, Lodge B (1960) Aneurysm of the splenic artery. Gut 1:312–320
Lauschke H, Rudolph J, Textor J et al (2002) Das Visceralarterienaneurysma. Zentralbl Chir 127:538–542
Tulsyan N, Kashyap VS, Greenberg RK et al (2007) The endovascular management of visceral artery aneurysms and pseudoaneurysms. J Vasc Surg 45:276–283
Sachdev-Ost Ulka (2010) Visceral artery aneurysms: review of current management options. Mt Sinai J Med 77:296–303
Hirsch AT, Haskal ZJ, Herztner NR et al (2006) ACC/AHA 2005 guidelines for the management of patients with peripheral arterial disease (lower extremity, renal, mesenteric and aortic). G Am Coll Cardiol 47:1239–1312
Leoni CJ, Potter JE, Rosen MP et al (2001) Classifying complications of interventional procedures: a survey of practicing radiologists. J Vasc Interv Radiol 12:55–59
Carr SC, Pearce WH, Vogelzang RL et al (1996) Current management of visceral artery aneurysms. Surgery 120:627–633
Shanley CJ, Shah NL, Messina LM (1996) Common splanchnic artery aneurysms: splenic, hepatic, and celiac. Ann Vasc Surg 10:315–322
Gabelmann A, Görich J, Merkle EM (2002) Endovascular treatment of visceral artery aneurysms. J Endovasc Ther 9:38–47
Stanley JC, Wakefield TW, Graham LM et al (1986) Clinical importance and management of splanchnic artery aneurysms. J Vasc Surg 3:836–840
Pasha SF, Glolviczki P, Stanson AW, Kamath PS (2007) Splanchnic artery aneurysms. Mayo Clin Proc 82:472–479
Arca MJ, Gagner M, Heniford BT et al (1999) Spenic artery aneurysms: methods of laparoscopic repair. J Vasc Surg 30:184–188
Laganà D, Carrafiello G, Mangini M et al (2006) Multimodal approach to endovascular treatment of visceral artery aneurysms and pseudoaneurysms. Eur J Radiol 59:104–111
Pulli R, Dorigo W, Troisi N et al (2008) Surgical treatment of visceral artery aneurysms: a 25-year experience. J Vasc Surg 48:334–342
Mauro MA, Jacques P (1991) Transcatheter management of pseudoaneurysms complicating pancreatitis. J Vasc Interv Radiol 2:527–532
Marone EM, Mascia D, Kahlberg A et al (2011) Is open repair still the gold standard in visceral artery aneurysm management? Ann Vasc Surg 25:936–946
Ikeda O, Nakasone Y, Tamura Y, Yamashita Y (2010) Endovascular management of visceral artery pseudoaneurysms: transcatheter coil embolization using the isolation technique. Cardiovasc Intervent Radiol 33:1128–1134
Cochennec F, Riga CV, Allaire E et al (2011) Contemporary management of splanchnic and renal artery aneurysms: results of endovascular compared with open surgery from two European vascular centers. Eur J Vasc Endovasc Surg 42(3):340–346
Gabelmann A, Gorich J, Merkle EM (2002) Endovascular treatment of visceral artery aneurysms. J Endovasc Ther 9:38–47
Tessier DJ, Stone WM, Fowl RJ et al (2003) Clinical features and management of splenic artery pseudoaneurysm: case series and cumulative review of literature. J Vasc Surg 38:969–974
Carmo M, Mercandalli G, Rampoldi A et al (2008) Transcatheter thrombin embolization of a giant visceral artery aneurysm. J Cardiovasc Surg (Torino) 49:777–782
Lameris R, du Plessis J, Nieuwoudt M et al (2011) A visceral pseudoaneurysm: management by EUS-guided thrombin injection. Gastrointest Endosc 73:392–395
Bratby MJ, Lehmann ED, Bottomley J et al (2006) Endovascular embolization of visceral artery aneurysms with ethylene-vinyl alcohol (Onyx): a case series. Cardiovasc Intervent Radiol 29:1125–1128
Kawai N, Sato M, Tanihata H et al (2010) Repair of traumatic abdominal aortic pseudoaneurysm using N-butyl-2-cyano-acrylate embolization. Cardiovasc Intervent Radiol 33:406–409
Graham LM, Rubin JR (1994) Visceral arterial aneurysms. In: Strandness DE, van Breda A (eds) Vascular diseases: surgical and interventional therapy. Churchill Livingstone, New York, pp 811–813
Piffaretti G, Tozzi M, Lomazzi C et al (2007) Splenic artery aneurysms: postembolization syndrome and surgical complications. Am J Surg 193:166–170
Larson RA, Solomon J, Carpenter JP (2002) Stent graft repair of visceral artery aneurysms. J Vasc Surg 36:1260–1263
Ruffino M, Rabbia C (2011) Endovascular treatment of visceral artery aneurysms with cardiatis multilayer flow modulator: preliminary results at six-month follow-up. J Cardiovasc Surg (Torino) 52:311–321
Sessa C, Tinelli G, Porcu P et al (2004) Treatment of visceral artery aneurysms: description of a retrospective series of 42 aneurysms in 34 patients. Ann Vasc Surg 18:695–703
Boudghene F, L’Hermine C, Bigot JM (1993) Arterial complications of pancreatitis: diagnostic and therapeutic aspects in 104 cases. J Vasc Interv Radiol 4:551–558
Belli AM, Markose G, Morgan R (2011) The role of interventional radiology in the management of abdominal visceral artery aneurysms. Cardiovasc Intervent Radiol. doi:10.1007/s00270-011-0201-3
Acknowledgment
Supported in part by a CIRSE Foundation Fellowship grant 2011 (to S.S.).
Conflict of interest
The authors declare that they have no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Spiliopoulos, S., Sabharwal, T., Karnabatidis, D. et al. Endovascular Treatment of Visceral Aneurysms and Pseudoaneurysms: Long-term Outcomes from a Multicenter European Study. Cardiovasc Intervent Radiol 35, 1315–1325 (2012). https://doi.org/10.1007/s00270-011-0312-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00270-011-0312-x