Abstract
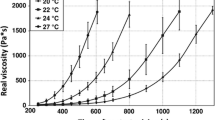
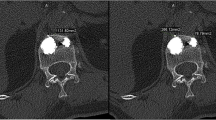
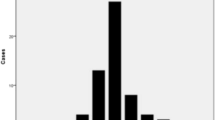
The objective of this study was to simplify the opacifying mixing process of the bone cement and contrast used for percutaneous vertebroplasty (PVP). We performed a biomechanical study of polymethyl methacrylate (PMMA) (CorinplastTM 3) using three different mixtures of PMMA, monomer, and contrast: group I, 2:1; group II, 3:2; group III, 3:2:1 ratio of powder/monomer/iodinated contrast (Omnipaque). In vitro biomechanical testing of ultimate compressive strength was carried out in all samples. Following the conclusion of a proper bone cement mixture regimen drawn from the in vitro study, PVP was performed in 125 patients: 58 with cancer, 12 with hemangioma, and 54 with osteoporotic fracture. The ultimate compressive strength in group III was decreased by 38% compared to groups II and I. Proper fluoroscopic visualization was achieved in all PVP procedures using this mixture. There were no major complications associated with injection of the cement mixture. Complete (CR) and partial response (PR) was obtained in 64% and 32.8%, respectively. No further vertebral collapse occurred during follow-up. The regimen using iodinated contrast for cement visualization during PVP provides a simple and convenient new method for mixing. Although the biomechanical strength is altered by the contrast medium added, it seems insignificant in clinical practice based on the authors’ limited experience.




Similar content being viewed by others
References
P Galibert H Deramond (1990) ArticleTitlePercutaneous acrylic vertebroplasty as a treatment of vertebral angioma as well as painful and debilitating diseases Chirurgie 116 326–334 Occurrence Handle1:STN:280:DyaK3M7itF2htA%3D%3D Occurrence Handle2149096
A Weill J Chiras JM Simon et al. (1996) ArticleTitleSpinal metastases: Indications for and results of percutaneous injection of acrylic surgical cement Radiology 199 241–247 Occurrence Handle1:STN:280:DyaK283gtF2jtA%3D%3D Occurrence Handle10.1148/radiology.199.1.8633152 Occurrence Handle8633152
A Cotten F Dewatre B Cortet et al. (1996) ArticleTitlePercutaneous vertebroplasty for osteolytic metastases and myeloma: Effects of the percentage of lesion filling and the leakage of methyl methacrylate at clinical follow up Radiology 200 525–530 Occurrence Handle1:STN:280:DyaK283psVGqsQ%3D%3D Occurrence Handle10.1148/radiology.200.2.8685351 Occurrence Handle8685351
JD Barr MS Barr TJ Lemley et al. (2000) ArticleTitlePercutaneous vertebroplasty for pain relief and spinal stabilization Spine 25 923–928 Occurrence Handle1:STN:280:DC%2BD3c3jt1Shuw%3D%3D Occurrence Handle10.1097/00007632-200004150-00005 Occurrence Handle10767803
Murphy KJ, Deramond H (2000) Percutaneous vertebroplasty in benign and malignant disease. (Review). Neuroimaging Clin North Am10:535–545
Mathis JM, Wong W (2003) Percutaneous vertebroplasty: technical considerations. J Vasc Intervent Radiol 14:953–960
A Gangi S Guth JP Imbert et al. (2003) ArticleTitlePercutaneous vertebroplasty: indications, technique, and results Radiographics 23 e10 Occurrence Handle10.1148/rg.e10 Occurrence Handle12889460
Evans AJ, Jensen ME, Kip KE, et al. (2003) Vertebral compression fractures: Pain reduction and improvement in functional mobility after percutaneous polymethylmethacrylate vertebroplasty retrospective report of 245 cases. Radiology 22:366–372
Perez-Higueras A, Alvarez L, Rossi RE, et al. (2002) Percutaneous vertebroplasty: long-term clinical and radiological outcome. Neuroradiology 44:950–954
McGraw JK, Lippert JA, Minkus KD, et al. (2002) Prospective evaluation of pain relief in 100 patients undergoing percutaneous vertebroplasty: Results and follow-up. J Vasc Intervent Radiol 13:883–886
World Health Organization (WHO) (1990) Cancer Pain Relief and Palliative Care: Report of a WHO Expert Committee. WHO, Geneva
McGraw JK, Cardella J, Barr JD, et al. (2003) Society of Interventional Radiology quality improvement guidelines for percutaneous vertebroplasty. J Vasc Intervent Radiol 14:827–831
Belkoff S, Deramond H, Mathis J, et al. (2000) Vertebroplasty: the biomechanical effect of cement volume (abstract). Trans Orthop Res Soc 25:356
SM Belkoff M Maroney DC Fenton et al. (1999) ArticleTitleAn in vitro biomechanical evaluation of bone cements used in percutaneous vertebroplasty Bone 25 23S–26S Occurrence Handle1:STN:280:DyaK1MzosFCmsw%3D%3D Occurrence Handle10.1016/S8756-3282(99)00128-3 Occurrence Handle10458269
Mathis JM, Barr JD, Belkoff SM, et al. (2001) Percutaneous vertebroplasty: a developing standard of care for vertebral compression fractures. AJNR 22:373–381
C Vasconcelos P Gailloud NJ Beauchamp et al. (2002) ArticleTitleIs percutaneous vertebroplasty without pretreatment venography safe? Evaluation of 205 consecutives procedures AJNR Am J Neuroradiol 23 913–917 Occurrence Handle12063215
Hierholzer J, Anselmetti G, Fuchs H, et al. (2003) Percutaneous osteoplasty as a treatment for painful malignant bone lesions of the pelvis and femur. J Vasc Intervent Radiol 14:773–777
WC Peh La Gilula DD Peck (2002) ArticleTitlePercutaneous vertebroplasty for severe osteoporotic vertebral body compression fractures Radiology 223 121–126 Occurrence Handle10.1148/radiol.2231010234 Occurrence Handle11930056
Chiras J., Depriester C, Weill A, et al. (1997) Percutaneous vertebral surgery: techniques and indications. J Neuroradiol 24:45–52
Acknowledgments
The authors thank Dr. Robert F. Jeffery from Dartmouth-Hitchcock Medical Center for his effort on manuscript revision. This study is supported by grant H2014 from the Jiangsu Health Key Project and grant 20024074 from the Nanjing Science and Technique Research Foundation.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Teng, GJ., He, SC., Deng, G. et al. A Simplified Method of Opacifying and Mixing Acrylic Cement for Percutaneous Vertebroplasty: A Clinical and In Vitro Study. Cardiovasc Intervent Radiol 28, 570–577 (2005). https://doi.org/10.1007/s00270-004-0126-1
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00270-004-0126-1