Abstract
Background
The discussion is ongoing about appropriate indications for laparoscopic surgery in trauma patients. As timing and risks of conversion to laparotomy remain unclear, we aimed to elucidate characteristics of and risks for conversion following laparoscopic surgery, using a nationwide database.
Methods
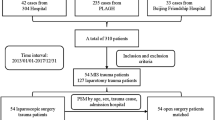
A retrospective observational study was conducted, using Japanese Trauma Data Bank (2004–2018). We included adult trauma patients who underwent laparoscopic surgery as an initial surgical intervention. Conversion to laparotomy was defined as laparotomy at the initial surgery. Patient demographics, mechanism and severity of injury, injured organs, timing of surgery, and clinical outcomes were compared between patients with and without conversion. Risks for conversion were analyzed focusing on indications for laparoscopic surgery, after adjusting patient and institution characteristics.
Results
Among 444 patients eligible for the study, 31 required conversions to laparotomy. The number of laparoscopic surgeries gradually increased over the study period (0.5–4.5% of trauma laparotomy), without changes in conversion rates (5–10%). Patients who underwent conversion had more severe abdominal injuries compared with those who did not (AIS 3 vs 2). While length of hospital stay and in-hospital mortality were comparable, abdominal complications were higher among patients with conversion (12.9 vs. 2.9%), particularly when laparoscopy was performed for peritonitis (OR, 22.08 [5.11–95.39]). A generalized estimating equation model adjusted patient background and identified hemoperitoneum and peritoneal penetration as risks for conversion (OR, 24.07 [7.35–78.75] and 8.26 [1.20– 56.75], respectively).
Conclusions
Trauma laparoscopy for hemoperitoneum and peritoneal penetration were associated with higher incidence of conversion to open laparotomy.



Similar content being viewed by others
Data availability
The data of this study are available from the Japanese Association for Trauma Surgery and the Japanese Association for Acute Medicine, but restrictions apply to the availability of these data, which were used under license for the current study, and so are not publicly available. Data are, however, available from the authors upon reasonable request and with permission of the Japanese Association for Trauma Surgery and the Japanese Association for Acute Medicine.
References
Chang KJ (2019) Laparoscopic foregut surgery and interventions: the future is now. the state-of-the-art and my personal journey. World J Gastroenterol 25:1–41
Mandrioli M, Inaba K, Piccinini A et al (2016) Advances in laparoscopy for acute care surgery and trauma. World J Gastroenterol 22:668–680
Biffl WL, Leppaniemi A (2015) Management guidelines for penetrating abdominal trauma. World J Surg 39:1373–1380
O’Malley E, Boyle E, O’Callaghan A et al (2013) Role of laparoscopy in penetrating abdominal trauma: a systematic review. World J Surg 37:113–122
Di Saverio S, Birindelli A, Podda M et al (2019) Trauma laparoscopy and the six w’s: Why, where, who, when, what, and how? J Trauma Acute Care Surg 86:344–367
Zafar SN, Onwugbufor MT, Hughes K et al (2015) Laparoscopic surgery for trauma: the realm of therapeutic management. Am J Surg 209:627–632
Koganti D, Hazen BJ, Dente CJ et al (2021) The role of diagnostic laparoscopy for trauma at a high-volume level one center. Surg Endosc 35:2667–2670
Parajuli P, Kumar S, Gupta A et al (2018) Role of laparoscopy in patients with abdominal trauma at level-I trauma center. Surg Laparosc Endosc Percutan Tech 28:20–25
Koto MZ, Matsevych OY, Aldous C (2018) Diagnostic laparoscopy for trauma: how not to miss injuries. J Laparoendosc Adv Surg Tech A 28:506–513
Cocco AM, Bhagvan S, Bouffler C et al (2019) Diagnostic laparoscopy in penetrating abdominal trauma. ANZ J Surg 89:353–356
Matsevych O, Koto M, Balabyeki M et al (2018) Trauma laparoscopy: when to start and when to convert? Surg Endosc 32:1344–1352
Li Y, Xiang Y, Wu N et al (2015) A Comparison of laparoscopy and laparotomy for the management of abdominal trauma: a systematic review and meta-analysis. World J Surg 39:2862–2871
Yamamoto R, Suzuki M, Yoshizawa J et al (2021) Physician-staffed ambulance and increased in-hospital mortality of hypotensive trauma patients following prolonged prehospital stay: A nationwide study. J Trauma Acute Care Surg 91:336–343
American College of Surgeons, Committee on Trauma. Advanced trauma life support: student course manual. 10th ed. (2018) American College of Surgeons, Chicago, IL
Bible J, Albert PS, Simons-Morton BG et al (2019) Practical issues in using generalized estimating equations for inference on transitions in longitudinal data: What is being estimated? Stat Med 38:903–916
Kauvar DS, Lefering R, Wade CE (2006) Impact of hemorrhage on trauma outcome: an overview of epidemiology, clinical presentations, and therapeutic considerations. J Trauma 60:S3-11
Moore L, Lavoie A, Abdous B et al (2006) Unification of the revised trauma score. J Trauma 61:718–722
Matsevych OY, Koto MZ, Aldous C (2018) Trauma laparoscopy: A prospect of skills training (cohort study). Int J Surg 55:117–123
Villavicencio RT, Aucar JA (1999) Analysis of laparoscopy in trauma. J Am Coll Surg 189:11–20
Uranues S, Popa DE, Diaconescu B et al (2015) Laparoscopy in penetrating abdominal trauma. World J Surg 39:1381–1388
Bain K, Meytes V, Chang GC et al (2019) Laparoscopy in penetrating abdominal trauma is a safe and effective alternative to laparotomy. Surg Endosc 33:1618–1625
Cirocchi R, Birindelli A, Inaba K et al (2018) Laparoscopy for trauma and the changes in its use from 1990 to 2016: a current systematic review and meta-analysis. Surg Laparosc Endosc Percutan Tech 28:1–12
de Rooij T, van Hilst J, van Santvoort H et al (2019) Minimally invasive versus open distal pancreatectomy (leopard): a multicenter patient-blinded randomized controlled trial. Ann Surg 269:2–9
Di Buono G, Buscemi S, Cocorullo G et al (2021) Feasibility and safety of laparoscopic complete mesocolic excision (cme) for right-sided colon cancer: short-term outcomes. A Randomized Clin Study Ann Surg 274:57–62
Fretland ÅA, Dagenborg VJ, Bjørnelv GMW et al (2018) Laparoscopic versus open resection for colorectal liver metastases: the OSLO-COMET randomized controlled trial. Ann Surg 267:199–207
Cirocchi R, Di Saverio S, Weber DG et al (2017) Laparoscopic lavage versus surgical resection for acute diverticulitis with generalised peritonitis: a systematic review and meta-analysis. Tech Coloproctol 21:93–110
Cherkasov M, Sitnikov V, Sarkisyan B et al (2008) Laparoscopy versus laparotomy in management of abdominal trauma. Surg Endosc 22:228–231
Koto MZ, Matsevych OY, Mosai F et al (2019) Laparoscopy for blunt abdominal trauma: a challenging endeavor. Scand J Surg 108:273–279
Acknowledgements
None
Funding
No funding support in this study.
Author information
Authors and Affiliations
Contributions
RY and RC designed the study. RY performed data collection. JS managed quality control. RY and RC did data analysis and data interpretation. RY, RC, and JS did writing and critical revision. All author revised the manuscript.
Corresponding author
Ethics declarations
Conflicts of interest
The authors have no relevant conflicts of interest to disclose.
Ethical approval
This study was approved by the Institutional Review Board of the Keio University School of Medicine (application number: 20090087). The requirement for informed consent was waived because of the anonymous nature of the data being used.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Yamamoto, R., Cestero, R.F., Kameyama, N. et al. Characteristics of Laparoscopic Surgery for Trauma Patients and Risks of Conversion to Open Laparotomy. World J Surg 46, 2616–2624 (2022). https://doi.org/10.1007/s00268-022-06714-7
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00268-022-06714-7