Abstract
Background
Enhanced recovery after surgery (ERAS) protocols or laparoscopic technique has been applied in various surgical procedures. However, the clinical efficacy of combination of the two methods still remains unclear. Thus, our aim was to assess the role of ERAS protocols in laparoscopic abdominal surgery.
Methods
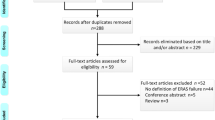
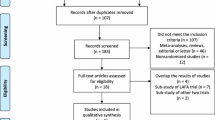
We performed a systematic literature search in various databases from January 1990 to October 2017. The results were analyzed according to predefined criteria.
Results
In the present meta-analysis, the outcomes of 34 comparative studies (15 randomized controlled studies and 19 non-randomized controlled studies) enrolling 3615 patients (1749 in the ERAS group and 1866 in the control group) were pooled. ERAS group was associated with shorter hospital stay (WMD − 2.37 days; 95% CI − 3.00 to − 1.73; P 0.000) and earlier time to first flatus (WMD − 0.63 days; 95% CI − 0.90 to − 0.36; P 0.000). Meanwhile, lower overall postoperative complication rate (OR 0.62; 95% CI 0.51–0.76; P 0.000) and less hospital cost (WMD 801.52 US dollar; 95% CI − 918.15 to − 684.89; P 0.000) were observed in ERAS group. Similar readmission rate (OR 0.73, 95% CI 0.52–1.03, P 0.070) and perioperative mortality (OR 1.33; 95% CI 0.53–3.34; P 0.549) were found between the two groups.
Conclusions
ERAS protocol for laparoscopic abdominal surgery is safe and effective. ERAS combined with laparoscopic technique is associated with faster postoperative recovery without increasing readmission rate and perioperative mortality.




Similar content being viewed by others
References
Bardram LF-JP, Jensen P, Crawford ME, Kehlet H (1995) Recovery after laparoscopic colonic surgery with epidural analgesia, and early oral nutrition and mobilisation. Lancet 345:763–764
Kehlet HWD (2002) Multimodal strategies to improve surgical outcome. Am J Surg 83:630–641
Grant MCYD, Wu CL, Makary MA, Wick EC (2017) Impact of enhanced recovery after surgery and fast track surgery pathways on healthcare-associated infections: results from a systematic review and meta-analysis. Ann Surg 265:68–79
Zhao Y, Qin H, Wu Y et al (2017) Enhanced recovery after surgery program reduces length of hospital stay and complications in liver resection: a PRISMA-compliant systematic review and meta-analysis of randomized controlled trials. Medicine 96:e7628
Deng XCX, Huo Z, Shi Y, Jin Z, Feng H, Wang Y, Wen C, Qian H, Zhao R, Qiu W, Shen B, Peng C (2017) Modified protocol for enhanced recovery after surgery is beneficial for Chinese cancer patients undergoing pancreaticoduodenectomy. Oncotarget 8:47841–47848
Tanaka R, Lee SW, Kawai M et al (2017) Protocol for enhanced recovery after surgery improves short-term outcomes for patients with gastric cancer: a randomized clinical trial. Gastric Cancer 20:861–871
Visioni A, Shah R, Gabriel E et al (2017) Enhanced recovery after surgery for noncolorectal surgery? A systematic review and meta-analysis of major abdominal surgery. Ann Surg 267:57–65
Wang C, Zheng G, Zhang W et al (2017) Enhanced recovery after surgery programs for liver resection: a meta-analysis. J Gastrointest Surg 21:472–486
Jiang L, Yang KH, Guan QL et al (2013) Laparoscopy-assisted gastrectomy versus open gastrectomy for resectable gastric cancer: an update meta-analysis based on randomized controlled trials. Surg Endosc 27:2466–2480
Feng FJG, Li JP, Li XH, Shi H, Zhao ZW, Wu GS, Liu XN, Zhao QC (2013) Fast-track surgery could improve postoperative recovery in radical total gastrectomy patients. World J Gastroenterol 19:3642–3648
Geltzeiler CB, Rotramel A, Wilson C et al (2014) Prospective study of colorectal enhanced recovery after surgery in a community hospital. JAMA Surg 149:955–961
Higgins JP, Altman DG, Gotzsche PC et al (2011) The Cochrane Collaboration’s tool for assessing risk of bias in randomised trials. BMJ 343:d5928
Stang A (2010) Critical evaluation of the Newcastle–Ottawa scale for the assessment of the quality of nonrandomized studies in meta-analyses. Eur J Epidemiol 25:603–605
Recart ADD, White PF, Thomas T, Johnson DB, Cadeddu JA, Recart A, Duchene D, White PF et al (2005) Efficacy and safety of fast-track recovery strategy for patients undergoing laparoscopic nephrectomy. J Endourol 19:1165–1169
Gralla O, Haas F, Knoll N et al (2007) Fast-track surgery in laparoscopic radical prostatectomy: basic principles. World J Urol 25:185–191
Magheli A, Knoll N, Lein M et al (2011) Impact of fast-track postoperative care on intestinal function, pain, and length of hospital stay after laparoscopic radical prostatectomy. J Endourol 25:1143–1147
Vlug MS, Wind J, Hollmann MW et al (2011) Laparoscopy in combination with fast track multimodal management is the best perioperative strategy in patients undergoing colonic surgery: a randomized clinical trial (LAFA-study). Ann Surg 254:868–875
Lee TG, Kang SB, Kim DW et al (2011) Comparison of early mobilization and diet rehabilitation program with conventional care after laparoscopic colon surgery: a prospective randomized controlled trial. Dis Colon Rectum 54:21–28
Kim JW, Kim WS, Cheong J-H et al (2012) Safety and efficacy of fast-track surgery in laparoscopic distal gastrectomy for gastric cancer: a randomized clinical trial. World J Surg 36:2879–2887. https://doi.org/10.1007/s00268-012-1741-7
Chen HJ, Xin JL, Cai L et al (2012) Preliminary experience of fast-track surgery combined with laparoscopy-assisted radical distal gastrectomy for gastric cancer. J Gastrointest Surg 16:1830–1839
Wang Q, Suo J, Jiang J et al (2012) Effectiveness of fast-track rehabilitation vs conventional care in laparoscopic colorectal resection for elderly patients: a randomized trial. Colorectal Dis 14:1009–1013
Wang G, Jiang Z, Zhao K et al (2012) Immunologic response after laparoscopic colon cancer operation within an enhanced recovery program. J Gastrointest Surg 16:1379–1388
Lemanu DP, Singh PP, Berridge K et al (2013) Randomized clinical trial of enhanced recovery versus standard care after laparoscopic sleeve gastrectomy. Br J Surg 100:482–489
Feng F, Li XH, Shi H et al (2014) Fast-track surgery combined with laparoscopy could improve postoperative recovery of low-risk rectal cancer patients: a randomized controlled clinical trial. J Dig Dis 15:306–313
He F, Lin X, Xie F et al (2015) The effect of enhanced recovery program for patients undergoing partial laparoscopic hepatectomy of liver cancer. Clin Transl Oncol 17:694–701
Abdikarim I, Cao XY, Li SZ et al (2015) Enhanced recovery after surgery with laparoscopic radical gastrectomy for stomach carcinomas. World J Gastroenterol 21:13339–13344
Liang X, Ying H, Wang H et al (2016) Enhanced recovery program versus traditional care in laparoscopic hepatectomy. Medicine 95:e2835
Liu G, Jian F, Wang X et al (2016) Fast-track surgery protocol in elderly patients undergoing laparoscopic radical gastrectomy for gastric cancer: a randomized controlled trial. Onco Targets Ther 9:3345–3351
Stoot JH, Van Dam RM, Busch OR et al (2009) The effect of a multimodal fast-track programme on outcomes in laparoscopic liver surgery: a multicentre pilot study. Hpb 11:140–144
Tsikitis VL, Holubar SD, Dozois EJ et al (2010) Advantages of fast-track recovery after laparoscopic right hemicolectomy for colon cancer. Surg Endosc 24:1911–1916
Poon JT, Fan JK, Lo OS et al (2011) Enhanced recovery program in laparoscopic colectomy for cancer. Int J Colorectal Dis 26:71–77
Gouvas N, Gogos-Pappas G, Tsimogiannis K et al (2012) Implementation of fast-track protocols in open and laparoscopic sphincter-preserving rectal cancer surgery: a multicenter, comparative, prospective, non-randomized study. Digestive Surgery 29:301–309
Sanchez-Perez B, Aranda-Narvaez JM, Suarez-Munoz MA et al (2012) Fast-track program in laparoscopic liver surgery: theory or fact? World J Gastrointest Surg 4:246–250
Huibers CJA, de Roos MAJ, Ong KH (2011) The effect of the introduction of the ERAS protocol in laparoscopic total mesorectal excision for rectal cancer. Int J Colorectal Dis 27:751–757
Saar M, Ohlmann CH, Siemer S et al (2013) Fast-track rehabilitation after robot-assisted laparoscopic cystectomy accelerates postoperative recovery. BJU Int 112:E99–E106
Guan X, Liu L, Lei X et al (2014) A comparative study of fast-track versus [corrected] conventional surgery in patients undergoing laparoscopic radical cystectomy and ileal conduit diversion: Chinese experience. Sci Rep 4:6820
Sahoo MRGM, Kumar TA (2014) Early rehabilitation after surgery program versus conventional care during perioperative period in patients undergoing laparoscopic assisted total gastrectomy. J Minim Access Surg 10:132–138
Taupyk Y, Cao X, Zhao Y et al (2015) Fast-track laparoscopic surgery: a better option for treating colorectal cancer than conventional laparoscopic surgery. Oncol Lett 10:443–448
Esteban F, Cerdan FJ, Garcia-Alonso M et al (2014) A multicentre comparison of a fast track or conventional postoperative protocol following laparoscopic or open elective surgery for colorectal cancer surgery. Colorectal Dis 16:134–140
Richardson J, Di Fabio F, Clarke H et al (2015) Implementation of enhanced recovery programme for laparoscopic distal pancreatectomy: feasibility, safety and cost analysis. Pancreatology 15:185–190
Alvarez MP, Foley KE, Zebley DM et al (2015) Comprehensive enhanced recovery pathway significantly reduces postoperative length of stay and opioid usage in elective laparoscopic colectomy. Surg Endosc 29:2506–2511
Vignali A, Elmore U, Cossu A et al (2016) Enhanced recovery after surgery (ERAS) pathway vs traditional care in laparoscopic rectal resection: a single-center experience. Tech Coloproctol 20:559–566
Rege A, Leraas H, Vikraman D et al (2016) Could the use of an enhanced recovery protocol in laparoscopic donor nephrectomy be an incentive for live kidney donation? Cureus 8:e889
Fang F, Gao J, Bi X et al (2016) Effect and clinical significance of fast-track surgery combined with laparoscopic radical gastrectomy on the plasma level of vascular endothelial growth factor in gastric antrum cancer. SpringerPlus 5:50
Pedziwiatr M, Wierdak M, Nowakowski M et al (2016) Cost minimization analysis of laparoscopic surgery for colorectal cancer within the enhanced recovery after surgery (ERAS) protocol: a single-centre, case-matched study. Videosurg Other Miniinvasive Tech 11:14–21
Sugi M, Matsuda T, Yoshida T et al (2017) Introduction of an enhanced recovery after surgery protocol for robot-assisted laparoscopic radical prostatectomy. Urol Int 99:194–200
Zeng WG, Liu MJ, Zhou ZX et al (2017) Enhanced recovery programme following laparoscopic colorectal resection for elderly patients. ANZ J Surg https://doi.org/10.1111/ans.14074. [epub ahead of print]
Tsai TC, Orav EJ, Jha AK (2015) Patient satisfaction and quality of surgical care in US hospitals. Ann Surg 261:2–8
Khorgami Z, Andalib A, Aminian A et al (2016) Predictors of readmission after laparoscopic gastric bypass and sleeve gastrectomy: a comparative analysis of ACS-NSQIP database. Surg Endosc 30:2342–2350
Lyon A, Solomon MJ, Harrison JD (2014) A qualitative study assessing the barriers to implementation of enhanced recovery after surgery. World J Surg 38:1374–1380. https://doi.org/10.1007/s00268-013-2441-7
Bu J, Li N, Huang X et al (2015) Feasibility of fast-track surgery in elderly patients with gastric cancer. J Gastrointest Surg 19:1391–1398
Feroci F, Kroning KC, Lenzi E et al (2011) Laparoscopy within a fast-track program enhances the short-term results after elective surgery for resectable colorectal cancer. Surg Endosc 25:2919–2925
Roulin D, Donadini A, Gander S et al (2013) Cost-effectiveness of the implementation of an enhanced recovery protocol for colorectal surgery. Br J Surg 100:1108–1114
Roulin D, Donadini A, Gander S et al (2015) The Impact of enhanced recovery protocol compliance on elective colorectal cancer resection. Ann Surg 261:1153–1159
Okrainec A, Aarts MA, Conn LG et al (2017) Compliance with urinary catheter removal guidelines leads to improved outcome in enhanced recovery after surgery patients. J Gastrointest Surg 21:1309–1317
Pecorelli N, Hershorn O, Baldini G et al (2017) Impact of adherence to care pathway interventions on recovery following bowel resection within an established enhanced recovery program. Surg Endosc 31:1760–1771
Kennedy RH, Francis EA, Wharton R et al (2014) Multicenter randomized controlled trial of conventional versus laparoscopic surgery for colorectal cancer within an enhanced recovery programme: EnROL. J Clin Oncol 32:1804–1811
van Bree S, Vlug M, Bemelman W et al (2011) Faster recovery of gastrointestinal transit after laparoscopy and fast-track care in patients undergoing colonic surgery. Gastroenterology 141(872–880):e874
Lee SS, Chung HY, Kwon OK et al (2016) Long-term quality of life after distal subtotal and total gastrectomy: symptom- and behavior-oriented consequences. Ann Surg 263:738–744
Bottomley A (2002) The cancer patient and quality of life. Oncologist 7:120–125
Kim YW, Baik YH, Yun YH et al (2008) Improved quality of life outcomes after laparoscopy-assisted distal gastrectomy for early gastric cancer: results of a prospective randomized clinical trial. Ann Surg 248:721–727
Zhang RC, Zhang B, Mou YP et al (2017) Comparison of clinical outcomes and quality of life between laparoscopic and open central pancreatectomy with pancreaticojejunostomy. Surg Endosc 31:4756–4763
Authors’ contributions
Zhengyan Li and Qingchuan Zhao performed the experiment conception and design. Zhengyan Li and Bin Bai performed the research and retrieved the data. Zhengyan Li, Gang Ji, and Yezhou Liu performed the data analysis. Zhengyan Li did the paper writing. All authors read and approved the final manuscript.
Funding
This study was supported by the National Key Basic Research Program of China (No. 2014CBA02002).
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflict of interest
Zhengyan Li, Qingchuan Zhao, Bin Bai, Gang Ji, and Yezhou Liu have no conflicts of interest or financial ties to disclose.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Li, Z., Zhao, Q., Bai, B. et al. Enhanced Recovery After Surgery Programs for Laparoscopic Abdominal Surgery: A Systematic Review and Meta-analysis. World J Surg 42, 3463–3473 (2018). https://doi.org/10.1007/s00268-018-4656-0
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00268-018-4656-0