Abstract
Background
Prevalence of diabetes in surgical patients is 10–40%. It is well recognized that they have higher rates of complications, and longer stays in hospital compared to patients without diabetes. Enhanced recovery after surgery (ERAS) is an evidence-based multimodal surgical care pathway that improves postoperative complications and length of stay in patients without diabetes. This review evaluates the evidence on whether individuals with diabetes would benefit from ERAS implementation.
Methods
MEDLINE, Cochrane Central Register of Controlled Trials (CENTRAL) and EMBASE searched with no language restrictions applied. Conference proceedings and bibliographies were reviewed. Experts in the field were contacted, and www.clinicaltrials.gov searched for ongoing trials.
Selection criteria
Randomized controlled trials (RCT) looking at individuals with diabetes undergoing surgery randomized to ERAS® or conventional care. Non-randomized controlled trials, controlled before–after studies, interrupted time series, and cohort studies with concurrent controls were also considered. Two authors independently screened studies.
Results
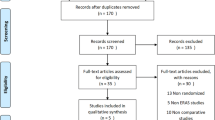
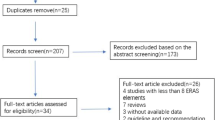
The electronic search yielded 437 references. After removing duplicates, 376 were screened for eligibility. Conference proceedings and bibliographies identified additional references. Searching www.clinicaltrials.gov yielded 59 references. Contacting experts in the field identified no further studies. Fourteen full articles were assessed and subsequently excluded for the following reasons: used an intervention other than ERAS®, did not include patients with diabetes, or used an uncontrolled observational design.
Conclusions
To date, the effects of ERAS® on patients with diabetes have not been rigorously evaluated. This review highlights the lack of evidence in this area and provides guidance on design for future studies.

Similar content being viewed by others
References
International Diabetes Federation (2015) IDF Diabetes Atlas, 7th edn. International Diabetes Federation, Brussels, Belgium. http://www.diabetesatlas.org
Clement S, Braithwaite SS, Magee MF et al (2004) Management of diabetes and hyperglycemia in hospitals. Diabetes Care 27:553–591
Smiley DD, Umpierrez GE (2006) Perioperative glucose control in the diabetic or nondiabetic patient. South Med J 99:580–589
Hoffman RL, Bartlett EK, Ko C et al (2014) Early discharge and readmission following colorectal resection. J Surg Res 190:579–586
Awad S, Carter S, Purkayastha S et al (2014) Enhanced recovery after bariatric surgery (ERABS): clinical outcomes from a tertiary referral bariatric centre. Obes Surg 24:753–758
Dogan K, Kraaij L, Aarts EO et al (2015) Fast-track bariatric surgery improves perioperative care and logistics compared to conventional care. Obes Surg 25:28–35
Hahl T, Tarkiainen P, Knutar O et al (2016) Outcome of laparoscopic gastric bypass (LRYGB) with a Program for Enhanced Recovery After Surgery (ERAS). Obes Surg 26:505–511
Malone DL, Genuit T, Tracy JK et al (2002) Surgical site infections: reanalysis of risk factors. J Surg Res 103:89–95
Bower WF, Jin L, Underwood MJ et al (2010) Overt diabetes mellitus adversely affects surgical outcomes of noncardiovascular patients. Surgery 147:670–675
Korol E, Johnston K, Waser N et al (2013) A systematic review of risk factors associated with surgical site infections among surgical patients. PLoS ONE 8:e83743
Fearon KC, Ljungqvist O, Von Meyenfeldt M et al (2005) Enhanced recovery after surgery: a consensus review of clinical care for patients undergoing colonic resection. Clin Nutr 24:466–477
History of the ERAS Society. Retrieved June 24 2016 from http://www.erassociety.org/index.php/about-us/history
Sammour T, Zargar-Shoshtari K, Bhat A et al (2010) A programme of enhanced recovery after surgery is a cost-effective intervention in elective colonic surgery. J N Z Med Assoc 123:61–70
Varadhan KK, Neal KR, Dejong CH et al (2010) The enhanced recovery after surgery (ERAS) pathway for patients undergoing major elective open colorectal surgery: a meta-analysis of randomized controlled trials. Clin Nutr 29:434–440
Lv L, Shao YF, Zhou YB (2012) The enhanced recovery after surgery (ERAS) pathway for patients undergoing colorectal surgery: an update of meta-analysis of randomized controlled trials. Int J Colorectal Dis 7:1549–1554
Gustafsson UO, Scott MJ, Schwenk W et al (2013) Guidelines for perioperative care in elective colonic surgery: enhanced recovery after surgery (ERAS) society recommendations. World J Surg 37:259–284. doi:10.1007/s00268-012-1772-0
Nygren J, Thacker J, Carli F et al (2013) Guidelines for perioperative care in elective rectal/pelvic surgery: Enhanced Recovery After Surgery (ERAS) Society recommendations. World J Surg 37:285–305. doi:10.1007/s00268-012-1787-6
Greco M, Capretti G, Beretta L et al (2014) Enhanced recovery program in colorectal surgery: a meta-analysis of randomized controlled trials. World J Surg 38:1531–1541. doi:10.1007/s00268-013-2416-8
Guyatt GH, Oxman AD, Vist GE et al (2008) GRADE: an emerging consensus on rating quality of evidence and strength of recommendations. BMJ 336:924–926
Gustafsson UO, Scott MJ, Schwenk W et al (2012) Enhanced Recovery After Surgery Society. Guidelines for perioperative care in elective colonic surgery: Enhanced Recovery After Surgery (ERAS®) Society recommendations. Clin Nutr 31:783–800
Gustafsson U, Hausel J, Thorell A et al (2011) Adherence to the enhanced recovery after surgery protocol and outcomes after colorectal cancer surgery. Arch Surg 146:571–577
Søreide E, Eriksson LI, Hirlekar G, et al (Task Force on Scandinavian Pre-operative Fasting Guidelines, Clinical Practice Committee Scandinavian Society of Anaesthesiology and Intensive Care Medicine) (2005) Pre-operative fasting guidelines: an update. Acta Anaesthesiol Scand 49:1041–1047
Farrukh A, Higgins A, Singh B et al (2014) Can pre-operative carbohydrate loading be used in diabetic patients undergoing colorectal surgery? Br J Diabetes Vasc Dis 14:102–104
Dhatariya K, Levy N, Kilvert A, Watson B et al (2012) NHS Diabetes guideline for the perioperative management of the adult patient with diabetes. Diabet Med 29:420–433
Laffin MR, Quigley P, Brisebois R et al (2015) Assessment of pre-operative carbohydrate loading and blood glucose concentration in patients with diabetes. Can J Surg 58:S183
Camilleri M (2007) Clinical practice. Diabetic gastroparesis. N Engl J Med 356:820–829
Vittal H, Farrugia G, Gomez G et al (2007) Mechanisms of disease: the pathological basis of gastroparesis—a review of experimental and clinical studies. Nat Clin Pract Gastroenterol Hepatol 4:336
Horváth VJ, Izbéki F, Lengyel C et al (2014) Diabetic gastroparesis: functional/morphologic background, diagnosis, and treatment options. Curr Diab Rep 14:527
Fraser R, Horowitz M, Dent J (1991) Hyperglycaemia stimulates pyloric motility in normal subjects. Gut 32:475–478
Kashyap P, Farrugia G (2010) Diabetic gastroparesis: what we have learned and had to unlearn in the past 5 years. Gut 59:1716–1726
Frisch A, Chandra P, Smiley D et al (2010) Prevalence and clinical outcome of hyperglycemia in the perioperative period in noncardiac surgery. Diabetes Care 33:1783–1788
King JT Jr, Goulet JL, Perkal MF et al (2011) Glycemic control and infections in patients with diabetes undergoing noncardiac surgery. Ann Surg 253:158–165
Blondet JJ, Beilman GJ (2007) Glycemic control and prevention of perioperative infection. Curr Opin Crit Care 13:421–427
Reeves BC, Deeks JJ, Higgins JPT, Wells GA. Chapter 13: Including non-randomized studies. In: Higgins JPT, Green S (editors), Cochrane Handbook for Systematic Reviews of Interventions Version 5.1.0 (updated March 2011). The Cochrane Collaboration, 2011. www.cochrane-handbook.org
Effective Practice and Organisation of Care (EPOC) (2013) How to prepare a risk of bias table for reviews that include more than one study design. EPOC Resources for review authors. Norwegian Knowledge Centre for the Health Services, Oslo. http://epoc.cochrane.org/epoc-specific-resources-review-authors. Accessed 24 June 2016
Higgins JPT, Altman DG, Sterne JAC (eds). Chapter 8: Assessing risk of bias in included studies. In: Higgins JPT, Green S (eds). Cochrane handbook for systematic reviews of interventions version 5.1.0 (updated March 2011). The Cochrane Collaboration, 2011. www.cochrane-handbook.org
Effective Practice and Organisation of Care (EPOC) (2015) Suggested risk of bias criteria for EPOC reviews. EPOC Resources for review authors. Norwegian Knowledge Centre for the Health Services, Oslo. http://epoc.cochrane.org/epoc-specific-resources-review-authors. Accessed 24 June 2016
Moher D, Liberati A, Tetzlaff J et al (2009) Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. J Clin Epidemiol 62:1006–1012
Haverkamp MP, de Roos MA, Ong KH (2012) The ERAS protocol reduces the length of stay after laparoscopic colectomies. Surg Endosc 26:361–367
Roulin D, Donadini A, Gander S et al (2013) Cost-effectiveness of the implementation of an enhanced recovery protocol for colorectal surgery. Br J Surg 100:1108–1114
Juul AB, Wetterslev J, Kofoed-Enevoldsen A (2004) Long term postoperative mortality in diabetic patients undergoing major non-cardiac surgery. Eur J Anaesth 21:523–529
Bolognesi MP, Marchant MH Jr, Viens NA et al (2008) The impact of diabetes on perioperative patient outcomes after total hip and total knee arthroplasty in the United States. J Arthroplast 23:92–98
Gil-Bona J, Sabaté A, Pi A et al (2009) Mortality risk factors in surgical patients in a tertiary hospital: a study of patient records in the period 2004–2006. Cir Esp 85:229–237
Jämsen E, Nevalainen P, Eskelinen A et al (2012) Obesity, diabetes, and preoperative hyperglycemia as predictors of periprosthetic joint infection: a single-center analysis of 7181 primary hip and knee replacements for osteoarthritis. J Bone Joint Surg Am 94:e101
Fei Q, Li J, Lin J et al. (2016) Risk factors for surgical site infection following spinal surgery: a meta-analysis. World Neurosurg 95:507–515
Martin ET, Kaye KS, Knott C et al (2016) Diabetes and risk of surgical site infection: a systematic review and meta-analysis. Infect Control Hosp Epidemiol 37:88–99
Luther A, Panteleimonitis S, Kang P, et al (2012) Diabetic patients take longer to recover than non-diabetics within an Enhanced Recovery Programme. In: Poster abstracts. Colorectal Disease 14:12–40
Jorgensen C, Madsbad S, Kehlet H, on behalf of the Lundbeck Foundation Centre for Fast-track Hip and Knee Replacement Collaborative Group (2015) Postoperative morbidity and mortality in type-2 diabetics after fast-track primary total hip and knee arthroplasty. Anesth Analg 120:230–238
Loo FD, Palmer DW, Soergel KH et al (1984) Gastric emptying in patients with diabetes mellitus. Gastroenterology 86:485–494
Wright RA, Clemente R, Wathen R (1985) Diabetic gastroparesis: an abnormality of gastric emptying of solids. Am J Med Sci 289:240–242
Camilleri M, Parkman HP, Shafi MA et al (2013) Clinical guideline: management of gastroparesis. Am J Gastroenterol 108:18–37
Choung RS, Locke GR 3rd, Schleck CD et al (2012) Risk of gastroparesis in subjects with type 1 and 2 diabetes in the general population. Am J Gastroenterol 107:82–88
Kong MF, Horowitz M, Jones KL et al (1999) Natural history of diabetic gastroparesis. Diabetes Care 22:503–507
Horowitz M, Wishart JM, Jones KL et al (1996) Gastric emptying in diabetes: an overview. Diabetes Med 13:S16–S22
Parkman HP, Yates K, Hasler WL et al (2011) Similarities and differences between diabetic and idiopathic gastroparesis. Clin Gastroenterol Hepatol 9:1056–1064
Jones KL, Horowitz M, Wishart MJ et al (1995) Relationships between gastric emptying, intragastric meal distribution and blood glucose concentrations in diabetes mellitus. J Nucl Med 36:2220–2228
Gustafsson UO, Nygren J, Thorell A et al (2008) Pre-operative carbohydrate loading may be used in type 2 diabetes patients. Acta Anaesthesiol Scand 52:946–951
Tryba M, Zenz M, Mlasowsky B et al (1983) Does a stomach tube enhance regurgitation during general anaesthesia? Anaesthesist 32:407–409
Ljungqvist O, Søreide E (2003) Preoperative fasting. Br J Surg 90:400–406
ERAS Compliance Group (2015) The impact of enhanced recovery protocol compliance on elective colorectal cancer resection: results from an international registry. Ann Surg 261:1153–1159
Chand M, Tatterton M, Heetun A, et al (2014) Diabetic patients undergoing laparoscopic surgery for colorectal. In: Poster Abstracts. Colorectal Disease 16:37–105
Jia Y, Jin G, Guo S et al (2014) Fast-track surgery decreases the incidence of postoperative delirium and other complications in elderly patients with colorectal carcinoma. Langenbecks Arch Surg 399:77–84
Kobayashi S, Ooshima R, Koizumi S et al (2014) Perioperative care with fast-track management in patients undergoing pancreaticoduodenectomy. World J Surg 38:2430–2437. doi:10.1007/s00268-014-2548-5
Lassen K, Soop M, Nygren J et al (2009) Consensus review of optimal perioperative care in colorectal surgery: Enhanced Recovery After Surgery (ERAS) Group recommendations. Arch Surg 144:961–969
Ahmed J, Khan S, Lim M et al (2012) Enhanced recovery after surgery protocols—compliance and variations in practice during routine colorectal surgery. Colorectal Dis 14:1045–1051
Vlug MS, Bartels SA, Wind J et al (2012) Which fast track elements predict early recovery after colon cancer surgery? Colorectal Dis 14:1001–1008
Nicholson A, Lowe MC, Parker J et al (2014) Systematic review and meta-analysis of enhanced recovery programmes in surgical patients. Br J Surg 101:172–188
Oppelstrup H, Ljungqvist O, Thorell A et al (2015) Adherence to the ERAS protocol and 5-year survival after colorectal cancer surgery: a retrospective cohort study [abstract]. J Anesth 62:683–720
American Diabetes Association (2016) 13. Diabetes care in the hospital. Diabetes Care 39(Suppl 1):S99–104
Buchleitner AM, Martínez-Alonso M, Hernández M et al (2012) Perioperative glycaemic control for diabetic patients undergoing surgery. Cochr Database Syst Rev 9: CD007315
Umpierrez GE, Smiley D, Hermayer K et al (2013) Randomized study comparing a basal-bolus with a basal plus correction insulin regimen for the hospital management of medical and surgical patients with type 2 diabetes: basal plus trial. Diabetes Care 36:2169–2174
Umpierrez GE, Smiley D, Jacobs S et al (2011) Randomized study of basal-bolus insulin therapy in the inpatient management of patients with type 2 diabetes undergoing general surgery (RABBIT 2 surgery). Diabetes Care 34:256–261
Joslin Diabetes Center (2015) Joslin Diabetes Center and Joslin Clinic Guideline for Inpatient Management of Surgical and ICU Patients with Diabetes (Pre-Peri- and Postoperative Care). https://www.joslin.org/docs/Inpatient-management-of-surgical-patients-with-diabetes-_12-30-2015.pdf. Accessed 23 October 2016
Shadish WR, Cook TD, Campbell DT (2001) Experimental and quasi-experimental designs for generalized causal inference. Houghton Mifflin, Boston, xxi: 623p
Kontopantelis E, Doran T, Springate DA (2015) Regression based quasi-experimental approach when randomisation is not an option: interrupted time series analysis. BMJ 350:h2750
Goodacre S (2015) Uncontrolled before-after studies: discouraged by Cochrane and EMJ. Emerg Med J 32:507–508
Acknowledgements
We would like to thank Linda Slater, librarian at the University of Alberta, for her assistance in developing the search strategy for this review.
Authors’ contributions
Authors who contributed to the development of this review’s strategy, design, and analysis include ZA, FM, LG, and PS. The two independent reviewers were ZA and ML; FM was the third reviewer who resolved any disagreement. Additional expert opinion on ERAS in reviewing the manuscript was provided by LG. All authors reviewed and agreed on the final manuscript prior to submission.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
All authors declare that they have no conflict of interest.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Albalawi, Z., Laffin, M., Gramlich, L. et al. Enhanced Recovery After Surgery (ERAS®) in Individuals with Diabetes: A Systematic Review. World J Surg 41, 1927–1934 (2017). https://doi.org/10.1007/s00268-017-3982-y
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00268-017-3982-y