Abstract
Background
Papillary thyroid cancer (PTC) metastasizes to central lymph node (CLN). CLN metastasis is associated with high risk of locoregional recurrence and distant metastasis. The significance of the number of metastatic CLN has not been addressed. This study was designed to evaluate the clinical implication of the number of metastatic CLN in PTC.
Methods
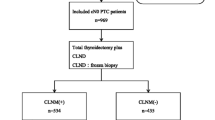
We reviewed the patients who underwent total thyroidectomy and CLN dissection with or without lateral neck dissection due to PTC, from March 2008 to June 2009. The relationships between the number of CLN and risk factors, including age, gender, tumor size, extrathyroidal extension, and lateral lymph node metastasis, were assessed. Patients were divided into three groups according to the number of CLN: group A = 0; group B = 1–2; and group C = ≥3.
Results
Of 258 patients enrolled in this study, 113 were in group A, 73 in group B, and 72 in group C. Extrathyroidal extension and lateral neck lymph node metastasis were related to increased rate of CLN metastasis (P < 0.05). Tumor size increased as the number of CLN increased; group C had the largest tumor size (P < 0.05). When evaluating the distribution of patients with extrathyroidal extension, group C had a significant odds ratio (4.213, P < 0.05). When evaluating the distribution of lateral neck lymph node metastasis, groups B and C had significant odds ratio (14.353, 75.403, respectively, P < 0.05).
Conclusions
The number of CLN metastasis correlated with the negative prognostic factors, including tumor size, extrathyroidal extension, and lateral neck lymph node metastasis. This suggests that the number of CLN has prognostic implication.


Similar content being viewed by others
References
Machens A, Hinze R, Thomusch O et al (2002) Pattern of nodal metastasis for primary and reoperative thyroid cancer. World J Surg 26:22–28
Roh JL, Kim JM, Park CI (2008) Central cervical nodal metastasis from papillary thyroid microcarcinoma: pattern and factors predictive of nodal metastasis. Ann Surg Oncol 15:2482–2486
Shaha AR (1998) Management of the neck in thyroid cancer. Otolaryngol Clin North Am 31:823–831
Cooper DS, Doherty GM, Haugen BR et al (2006) Management guidelines for patients with thyroid nodules and differentiated thyroid cancer. Thyroid 16:109–142
Lundgren CI, Hall P, Dickman PW et al (2006) Clinically significant prognostic factors for differentiated thyroid carcinoma: a population-based, nested case-control study. Cancer 106:524–531
Choi SJ, Kim TY, Lee JC et al (2008) Is routine central neck dissection necessary for the treatment of papillary thyroid microcarcinoma? Clin Exp Otorhinolaryngol 1:41–45
Hughes CJ, Shaha AR, Shah JP et al (1996) Impact of lymph node metastasis in differentiated carcinoma of the thyroid: a matched-pair analysis. Head Neck 18:127–132
White ML, Doherty GM (2007) Level VI lymph node dissection for papillary thyroid cancer. Minerva Chir 62:383–393
Mazzaferri EL, Doherty GM, Steward DL (2009) The pros and cons of prophylactic central compartment lymph node dissection for papillary thyroid carcinoma. Thyroid 19:683–689
Mazzaferri EL (2009) A vision for the surgical management of papillary thyroid carcinoma: extensive lymph node compartmental dissections and selective use of radioiodine. J Clin Endocrinol Metab 94:1086–1088
Greene F (2002) AJCC cancer staging manual. Springer-Verlag, New York
Davidson HC, Park BJ, Johnson JT (2008) Papillary thyroid cancer: controversies in the management of neck metastasis. Laryngoscope 118:2161–2165
Ito Y, Higashiyama T, Takamura Y et al (2007) Risk factors for recurrence to the lymph node in papillary thyroid carcinoma patients without preoperatively detectable lateral node metastasis: validity of prophylactic modified radical neck dissection. World J Surg 31:2085–2091
Ito Y, Miyauchi A, Jikuzono T et al (2007) Risk factors contributing to a poor prognosis of papillary thyroid carcinoma: validity of UICC/AJCC TNM classification and stage grouping. World J Surg 31:838–848
Kim TY, Hong SJ, Kim JM et al (2008) Prognostic parameters for recurrence of papillary thyroid microcarcinoma. BMC Cancer 8:296
Lee BJ, Lee JC, Wang SG et al (2009) Metastasis of right upper para-esophageal lymph nodes in central compartment lymph node dissection of papillary thyroid cancer. World J Surg 33:2094–2098
Camp RL, Rimm EB, Rimm DL (2000) A high number of tumor-free axillary lymph nodes from patients with lymph node negative breast carcinoma is associated with poor outcome. Cancer 88:108–113
Huang CM, Lin BJ, Lu HS et al (2008) Prognostic impact of metastatic lymph node ratio in advanced gastric cancer from cardia and fundus. World J Gastroenterol 14:4383–4388
Nemoto T, Vana J, Bedwani RN et al (1980) Management and survival of female breast cancer: results of a national survey by the American College of Surgeons. Cancer 45:2917–2924
Chatni SS, Thankappan K (2008) Lymph node status cannot be ignored in survival analysis of laryngeal cancer. Arch Otolaryngol Head Neck Surg 134:786 (author reply 786–787)
Schmitz S, Machiels JP, Weynand B et al (2009) Results of selective neck dissection in the primary management of head and neck squamous cell carcinoma. Eur Arch Otorhinolaryngol 266:437–443
Palme CE, Waseem Z, Raza SN et al (2004) Management and outcome of recurrent well-differentiated thyroid carcinoma. Arch Otolaryngol Head Neck Surg 130:819–824
Mazzaferri EL, Jhiang SM (1994) Long-term impact of initial surgical and medical therapy on papillary and follicular thyroid cancer. Am J Med 97:418–428
Simon D, Goretzki PE, Witte J et al (1996) Incidence of regional recurrence guiding radicality in differentiated thyroid carcinoma. World J Surg 20:860–866 (discussion 866)
Noguchi S, Yamashita H, Uchino S et al (2008) Papillary microcarcinoma. World J Surg 32:747–753
Cushing SL, Palme CE, Audet N et al (2004) Prognostic factors in well-differentiated thyroid carcinoma. Laryngoscope 114:2110–2115
Wittekind C, Compton CC, Greene FL et al (2002) TNM residual tumor classification revisited. Cancer 94:2511–2516
Mercante G, Frasoldati A, Pedroni C et al (2009) Prognostic factors affecting neck lymph node recurrence and distant metastasis in papillary microcarcinoma of the thyroid: results of a study in 445 patients. Thyroid 19:707–716
Moo TA, Umunna B, Kato M et al (2009) Ipsilateral versus bilateral central neck lymph node dissection in papillary thyroid carcinoma. Ann Surg 250:403–408
Sadowski BM, Snyder SK, Lairmore TC (2009) Routine bilateral central lymph node clearance for papillary thyroid cancer. Surgery 146:696–703 (discussion 703–695)
Koo BS, Choi EC, Yoon YH et al (2009) Predictive factors for ipsilateral or contralateral central lymph node metastasis in unilateral papillary thyroid carcinoma. Ann Surg 249:840–844
Lin JD, Chao TC, Weng HF et al (1999) Prognostic variables of papillary thyroid carcinomas with local invasion. Endocr J 46:91–98
Andersen PE, Kinsella J, Loree TR et al (1995) Differentiated carcinoma of the thyroid with extrathyroidal extension. Am J Surg 170:467–470
Arora N, Turbendian HK, Scognamiglio T et al (2008) Extrathyroidal extension is not all equal: Implications of macroscopic versus microscopic extent in papillary thyroid carcinoma. Surgery 144:942–947 (discussion 947–948)
Bellantone R, Lombardi CP, Boscherini M et al (1998) Prognostic factors in differentiated thyroid carcinoma: a multivariate analysis of 234 consecutive patients. J Surg Oncol 68:237–241
Ortiz S, Rodriguez JM, Soria T et al (2001) Extrathyroid spread in papillary carcinoma of the thyroid: clinicopathological and prognostic study. Otolaryngol Head Neck Surg 124:261–265
Ito Y, Tomoda C, Uruno T et al (2006) Prognostic significance of extrathyroid extension of papillary thyroid carcinoma: massive but not minimal extension affects the relapse-free survival. World J Surg 30:780–786
Sivanandan R, Soo KC (2001) Pattern of cervical lymph node metastases from papillary carcinoma of the thyroid. Br J Surg 88:1241–1244
Kupferman ME, Patterson M, Mandel SJ et al (2004) Patterns of lateral neck metastasis in papillary thyroid carcinoma. Arch Otolaryngol Head Neck Surg 130:857–860
Noguchi S, Murakami N, Yamashita H et al (1998) Papillary thyroid carcinoma: modified radical neck dissection improves prognosis. Arch Surg 133:276–280
Conflict of interest
None.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Lee, Y.S., Lim, Y.S., Lee, JC. et al. Clinical Implication of the Number of Central Lymph Node Metastasis in Papillary Thyroid Carcinoma: Preliminary Report. World J Surg 34, 2558–2563 (2010). https://doi.org/10.1007/s00268-010-0749-0
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00268-010-0749-0