Abstract
Introduction
The decision to perform a relaparotomy in patients with secondary peritonitis is based on “clinical judgment” with inherent variability among surgeons. Our objective was to review the literature on prognostic variables for ongoing abdominal infection. Predictive variables for positive findings at relaparotomy can generate more objective criteria to support the decision whether to perform a relaparotomy in patients with secondary peritonitis.
Methods
Multiple databases were searched for studies assessing the prognostic value of clinical variables predicting outcome of relaparotomy or general outcome in patients with secondary peritonitis. Data on the methodologic quality of the study as well as statistical strength of predictors and validity of individual variables were extracted and scored. A cumulative score was calculated from these three scores, and the variables were ranked.
Results
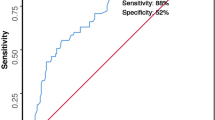
A total of 37 of 197 retrieved articles were included for final assessment. The median score for methodologic quality of individual articles was 36 (range 19–54). After calculation of the combined scores, 76 individual variables (patient, peritonitis, surgery, clinical, and laboratory variables) were identified from which the top 10 were eventually selected. These variables were age, concomitant disease, upper gastrointestinal source of peritonitis, generalized peritonitis, elimination of the focus, bilirubin, creatinine, lactate, PaO2/FiO2 ratio, and albumin. This set of variables proved to be moderately predictive for positive findings during relaparotomy in a retrospective cohort of 219 patients operated on for secondary peritonitis (receiver operator curve 0.75, with 95% confidence interval 0.68–0.82).
Conclusions
This review generated a hierarchy (weighted ranking) of published variables that could play a role in the decision to perform a relaparotomy in patients with secondary peritonitis. The top sixtile of ranked variables (10 variables) showed promising results in the discrimination between patients having a positive and negative relaparotomy when tested on a peritonitis patient database. This ranking of variables provides evidence for potential inclusion of variables in future predictive scores, although improvement in overall predictive strength of a set of variables in such a score is needed.


Similar content being viewed by others
References
Lamme B, Boermeester MA, Reitsma JB, et al. Meta-analysis of relaparotomy for secondary peritonitis. Br J Surg 2002;89:1516–1524
Hinsdale JG, Jaffe BM. Re-operation for intra-abdominal sepsis: indications, results in modern critical care setting. Ann Surg 1984; 199:31–36
Machiedo GW, Tikellis J, Suval W, et al. Reoperation for sepsis. Am Surg 1985;51:149–154
Beal AL, Cerra FB. Multiple organ failure syndrome in the 1990s: systemic inflammatory response and organ dysfunction. JAMA 1994;271:226–233
Ferraris VA. Exploratory laparotomy for potential abdominal sepsis in patients with multiple-organ failure. Arch Surg 1983;118:1130–1133
Fry DE, Garrison RN, Heitsch RC, et al. Determinants of death in patients with intraabdominal abscess. Surgery 1980;88:517–523
Koperna T, Schulz F. Relaparotomy in peritonitis: prognosis and treatment of patients with persisting intraabdominal infection. World J Surg 2000;24:32–37
Pacelli F, Doglietto GB, Alfierri S, et al. Prognosis in intra-abdominal infections: multivariate analysis on 604 patients. Arch Surg 1996;131:641–645
Wickel DJ, Cheadle WG, Mercer-Jones MA, et al. Poor outcome from peritonitis is caused by disease acuity and organ failure, not recurrent peritoneal infection. Ann Surg 1997;225:744–753
Altman DG. Systematic reviews of evaluations of prognostic variables. BMJ 2001;323:224–228
Chalmers TC, Smith H, Blackburn B, et al. A method for assessing the quality of a randomized control trial. Control Clin Trials 1981;2:31–49
Evans M, Pollock AV. A score system for evaluating random control clinical trials of prophylaxis of abdominal surgical wound infection. Br J Surg 1985;72:256–260
Fletcher B, Sackett DL. Canadian Task Force on the periodic health examination: the periodic health examination. CMAJ 1979;121:1193–1254
Lamme B, Boermeester MA, Belt EJ, et al. Mortality and morbidity of planned relaparotomy versus relaparotomy on demand for secondary peritonitis. Br J Surg 2004;91:1046–1054
Teichmann W, Wittmann DH, Andreone PA. Scheduled reoperations (etappenlavage) for diffuse peritonitis. Arch Surg 1986;121:147–152
Penninckx FM, Kerremans RP, Filez L. Planned relaparotomies for advanced, established peritonitis from colonic origin. Acta Chir Belg 1990;90:269–274
Ohmann C. Prognostic scores and design of clinical studies. Infection 1998;26:342–344
Jiffry BA, Sebastian MW, Amin T, et al. Multiple laparotomies for severe intra-abdominal infection. Aust N Z J Surg 1998;68:139–142
Billing A, Frohlich D, Schildberg FW. Prediction of outcome using the Mannheim peritonitis index in 2003 patients: Peritonitis Study Group. Br J Surg 1994;81:209–213
Oberholzer A, Keel M, Zellweger R, et al. Incidence of septic complications and multiple organ failure in severely injured patients is sex specific. J Trauma 2000;48:932–937
Spence PA, Mathews RE, Khanna R, et al. indications for operation when peritonitis occurs in patients on chronic ambulatory peritoneal dialysis. Surg Gynecol Obstet 1985;161:450–452
Bohnen JM, Schouten BD. Predicting the need for reoperation for abdominal infection. New Horiz 1998;6:S89–S96
Velmahos GC, Degiannis E, Souter I. Relaparotomies for abdominal sepsis—why, when, how? A collective review. S Afr J Surg 1998;36:52–56
Krause R. Reintervention in abdominal surgery. World J Surg 1987;11:226–232
Dellinger EP. Use of scoring systems to assess patients with surgical sepsis. Surg Clin North Am 1988;68:123–145
van Goor H. Interventional management of abdominal sepsis: when and how. Langenbecks Arch Surg 2002;387:191–200
Holzheimer R, Dralle H. Paradigm change in 30 years peritonitis treatment: a review on source control. Eur J Med Res 2001;6:161–168
Bohnen JM, Mustard RA. A critical look at scheduled relaparotomy for secondary bacterial peritonitis. Surg Gynecol Obstet 1991;172(Suppl):25–29
Pusajo JF, Bumaschny E, Doglio GR, et al. Postoperative intra-abdominal sepsis requiring reoperation: value of a predictive index. Arch Surg 1993;128:218–222
Sinanan M, Maier RV, Carrico CJ. Laparotomy for intra-abdominal sepsis in patients in an intensive care unit. Arch Surg 1984;119:652–658
Mustard RA, Bohnen JM, Rosati C, et al. Pneumonia complicating abdominal sepsis: an independent risk factor for mortality. Arch Surg 1991;126:170–175
Ohmann C, Hau T. Prognostic indices in peritonitis. Hepatogastroenterology 1997;44:937–946
Ohmann C, Wittmann DH, Wacha H. Prospective evaluation of prognostic scoring systems in peritonitis: Peritonitis Study Group. Eur J Surg 1993;159:267–274
Dellinger EP, Wertz MJ, Meakins JL, et al. Surgical infection stratification system for intra-abdominal infection: multicenter trial. Arch Surg 1985;120:212–219
Pine RW, Wertz MJ, Lennard ES, et al. Determinants of organ malfunction or death in patients with intra-abdominal sepsis: a discriminant analysis. Arch Surg 1983;118:242–249
Zer M, Dux S, Dintsman M. The timing of relaparotomy and its influence on prognosis: a 10 year survey. Am J Surg 1980;139:338–343
Wacha H, Hau T, Dittmer R, et al. Risk factors associated with intraabdominal infections: a prospective multicenter study; Peritonitis Study Group. Langenbecks Arch Surg 1999;384:24–32
Koperna T, Schulz F. Prognosis and treatment of peritonitis: do we need new scoring systems? Arch Surg 1996;131:180–186
Makela J, Kairaluoma MI. Relaparotomy for postoperative intra-abdominal sepsis in jaundiced patients. Br J Surg 1988;75:1157–1159
Meisner M, Tschaikowsky K, Palmaers T, et al. Comparison of procalcitonin (PCT) and C-reactive protein (CRP) plasma concentrations at different SOFA scores during the course of sepsis and MODS. Crit Care (Lond) 1999;3:45–50
Gotzinger P, Gebhard B, Wamser P, et al. [Revision of diffuse peritonitis: planned versus on demand.] Langenbecks Arch Chir 1996;381:343–347
Grunau G, Heemken R, Hau T. Predictors of outcome in patients with postoperative intra-abdominal infection. Eur J Surg 1996;162:619–625
Hau T, Ohmann C, Wolmershauser A, et al. Planned relaparotomy vs relaparotomy on demand in the treatment of intra-abdominal infections: The Peritonitis Study Group of the Surgical Infection Society–Europe. Arch Surg 1995;130:1193–1196
Bunt TJ. Urgent relaparotomy: the high-risk, no-choice operation. Surgery 1985;98:555–560
Bunt TJ. Non-directed relaparotomy for intra-abdominal sepsis: a futile procedure. Am Surg 1986;52:294–298
Butler JA, Huang J, Wilson SE. Repeated laparotomy for postoperative intra-abdominal sepsis: an analysis of outcome predictors. Arch Surg 1987;122:702–706
Bohnen JM, Mustard RA, Oxholm SE, et al. APACHE II score and abdominal sepsis: a prospective study. Arch Surg 1988;123:225–229
Bosscha K, Reijnders K, Hulstaert PF, et al. Prognostic scoring systems to predict outcome in peritonitis and intra-abdominal sepsis. Br J Surg 1997;84:1532–1534
Christou NV, Barie PS, Dellinger EP, et al. Surgical Infection Society intra-abdominal infection study: prospective evaluation of management techniques and outcome. Arch Surg 1993;128:193–198
Makela J, Kiviniemi H, Laitinen S. Prevalence of perforated sigmoid diverticulitis is increasing. Dis Colon Rectum 2002;45:955–961
Mulier S, Penninckx F, Verwaest C, et al. Factors affecting mortality in generalized postoperative peritonitis: multivariate analysis in 96 patients. World J Surg 2003;27:379–384
Ozguc H, Yilmazlar T, Gurluler E, et al. Staged abdominal repair in the treatment of intra-abdominal infection: analysis of 102 patients. J Gastrointest Surg 2003;7:646–651
Holzheimer RG, Gathof B. Re-operation for complicated secondary peritonitis: how to identify patients at risk for persistent sepsis. Eur J Med Res 2003;8:125–134
Cerra FB, Negro F, Abrams J. APACHE II score does not predict multiple organ failure or mortality in postoperative surgical patients. Arch Surg 1990;125:519–522
Bohnen JM, Christou NV, Maclean LD, et al. Predicting postoperative complications. Br J Surg 1983;70:128
McCrory C, Crowley K. Is repeat laparotomy of value in patients with suspected intra-abdominal sepsis in the intensive care unit? Ir J Med Sci 1997;166:88–91
Marshall JC, Maier RV, Jimenez M, et al. Source control in the management of severe sepsis and septic shock: an evidence-based review. Crit Care Med 2004;32:S513–S526
Dupont H, Paugam-Burtz C, Muller-Serieys C, et al. Predictive factors of mortality due to polymicrobial peritonitis with Candida isolation in peritoneal fluid in critically ill patients. Arch Surg 2002;137:1341–1346
Berard A, Andreu N, Tetrault J, et al. Reliability of Chalmers’ scale to assess quality in meta-analyses on pharmacological treatments for osteoporosis. Ann Epidemiol 2000;10:498–503
Linder MM, Wacha H, Feldmann U, et al. [The Mannheim peritonitis index: an instrument for the intraoperative prognosis of peritonitis.] Chirurg 1987;58:84–92
Marshall JC, Cook DJ, Christou NV, et al. Multiple organ dysfunction score: a reliable descriptor of a complex clinical outcome. Crit Care Med 1995;23:1638–1652
Vincent JL, Moreno R, Takala J, et al. The SOFA (Sepsis-related Organ Failure Assessment) score to describe organ dysfunction/failure: on behalf of the Working Group on Sepsis-Related Problems of the European Society of Intensive Care Medicine. Intensive Care Med 1996;22:707–710
Ohmann C, Yang Q, Hau T, et al. Prognostic modelling in peritonitis: Peritonitis Study Group of the Surgical Infection Society Europe. Eur J Surg 1997;163:53–60
Knaus WA, Draper EA, Wagner DP, et al. APACHE II: a severity of disease classification system. Crit Care Med 1985;13:818–829
Copeland GP, Jones D, Walters M. POSSUM: a scoring system for surgical audit. Br J Surg 1991;78:355–360
Moreno R, Vincent JL, Matos R, et al. The use of maximum SOFA score to quantify organ dysfunction/failure in intensive care: results of a prospective, multicentre study; Working Group on Sepsis Related Problems of the ESICM. Intensive Care Med 1999;25:686–696
Acknowledgment
The present study was supported by a grant from The Center for Clinical Guidelines of the Academic Medical Center, Amsterdam.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Lamme, B., Mahler, C.W., van Ruler, O. et al. Clinical Predictors of Ongoing Infection in Secondary Peritonitis: Systematic Review. World J. Surg. 30, 2170–2181 (2006). https://doi.org/10.1007/s00268-005-0333-1
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00268-005-0333-1