Abstract
Background
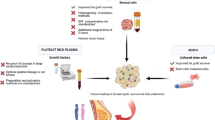
One of the most interesting developments in practical applications of fat grafting in recent years is the use of prosurvival strategies to improve maintenance of volume. Platelet-rich plasma (PRP) plays a decisive role in the repair and regeneration of different tissues via the activation and secretion of a great variety of growth factors and other cytokines stored in the alpha-granules of the platelets. This review aimed to assess the efficacy of PRP mixed-fat grafting as a prosurvival strategy for fat grafts.
Methods
Online searches of the Cochrane Library and MEDLINE until January 2014 were conducted. The review included studies with at least one clinical end point in which the effect of PRP on the absorption and viability of the fat graft could be assessed.
Results
The review comprised 6 preclinical studies with a control group and 9 clinical studies of humans. It also included comparative studies performed with other prosurvival strategies for fat grafts, such as combination with the stromal vascular fraction and second-generation PRP, also called “platelet-rich fibrin.” The results indicate that PRP may have a dose-dependent positive effect on fat grafts and suggest low complication rates.
Conclusions
The development of new growth factor delivery systems or cell therapies to enrich fat grafts is an area that merits further research.
No Level Assigned
This journal requires that authors assign a level of evidence to each submission to which Evidence-Based Medicine rankings are applicable. This excludes Review Articles, Book Reviews, and manuscripts that concern Basic Science, Animal Studies, Cadaver Studies, and Experimental Studies. For a full description of these Evidence-Based Medicine ratings, please refer to the Table of Contents or the online Instructions to Authors www.springer.com/00266.
Similar content being viewed by others
References
Illouz YG (1983) Body contouring by lipolysis: a 5-year experience with over 3,000 cases. Plast Reconstr Surg 72:591–597
Coleman SR (1998) Structural fat grafting. Aesthet Surg J 18:386, 388
Tabit CJ, Slack GC, Fan K et al (2012) Fat grafting versus adipose-derived stem cell therapy: distinguishing indications, techniques, and outcomes. Aesthetic Plast Surg 36:704–713
Newman RE, Yoo D, LeRoux MA et al (2009) Treatment of inflammatory diseases with mesenchymal stem cells. Inflamm Allergy Drug Targets 8:110–123
Rigotti G, Marchi A, Galie M et al (2007) Clinical treatment of radiotherapy tissue damage by lipoaspirate transplant: a healing process mediated by adipose-derived adult stem cells. Plast Reconstr Surg 119:1409–1422 discussion 1423–1424
Serra-Renom JM, Muñoz-Olmo JL, Serra-Mestre JM (2010) Fat grafting in postmastectomy breast reconstruction with expanders and prostheses in patients who have received radiotherapy: formation of new subcutaneous tissue. Plast Reconstr Surg 125:12–18
Phulpin B, Gangloff P, Tran N et al (2009) Rehabilitation of irradiated head and neck tissues by autologous fat transplantation. Plast Reconstr Surg 123:1187–1197
Gir P, Brown SA, Oni G et al (2012) Fat grafting: evidence-based review on autologous fat harvesting, processing, reinjection, and storage. Plast Reconstr Surg 130:249–258
Yoshimura K, Sato K, Aoi N et al (2008) Cell-assisted lipotransfer for cosmetic breast augmentation: Supportive use of adipose-derived stem/stromal cells. Aesthet Plast Surg 32:48–55 discussion 56–57
Hamed S, Egozi D, Kruchevsky D et al (2010) Erythropoietin improves the survival of fat tissue after its transplantation in nude mice. PLoS ONE 5:e13986
Yuksel E, Weinfeld AB, Cleek R et al (2000) Increased free fat-graft survival with the long-term, local delivery of insulin, insulin-like growth factor-I, and basic fibroblast growth factor by PLGA/PEG microspheres. Plast Reconstr Surg 105:1712–1720
Shoshani O, Livne E, Armoni M et al (2005) The effect of interleukin-8 on the viability of injected adipose tissue in nude mice. Plast Reconstr Surg 115:853–859
Marx R, Carlson E, Eichstaedt R et al (1998) Platelet-rich plasma: growth factor enhancement for bone grafts. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 85:638–646
Pierce GF, Mustoe TA, Altrock BW et al (1991) Role of platelet-derived growth factor in wound healing. J Cell Biochem 45:319–326
Eppley BL, Pietrzak WS, Blanton M (2006) Platelet-rich plasma: a review of biology and applications in plastic surgery. Plast Reconstr Surg 118:147
Pires Fraga FM, Nishio RT, Ishikawa RS et al (2010) Increased survival of free fat grafts with platelet-rich plasma in rabbits. J Plast Reconstr Aesthet Surg 63:e818–e822
Oh DS, Cheon YW, Jeon YR et al (2011) Activated platelet-rich plasma improves fat graft survival in nude mice: a pilot study. Dermatol Surg 37:619–625
Nakamura S, Ishihara M, Takikawa M et al (2010) Platelet-rich plasma (PRP) promotes survival of fat grafts in rats. Ann Plast Surg 65:101–106
Rodriguez-Flores J, Palomar-Gallego MA, Enguita-Valls AB et al (2011) Influence of platelet-rich plasma on the histologic characteristics of the autologous fat graft to the upper lip of rabbits. Aesthetic Plast Surg 35:480–486
Por YC, Yeow VK, Louri N et al (2009) Platelet-rich plasma has no effect on increasing free fat graft survival in the nude mouse. J Plast Reconstr Aesthet Surg 62:1030–1034
Liu B, Tan XY, Liu YP et al (2013) The adjuvant use of stromal vascular fraction and platelet-rich fibrin for autologous adipose tissue transplantation. Tissue Eng Part C Methods 19:1–14
Serra-Renom JM, Muñoz del Olmo JL, Gonzalo Caballero C (2006) Use of fat grafts enriched with platelet growth factors for facial lipofiling in ritidectomy. Cir Plas Iberlatinoam 32:191–198
Cervelli V, Gentile P, Scioli MG et al (2009) Application of platelet-rich plasma in plastic surgery: clinical and in vitro evaluation. Tissue Eng Part C Methods 15:625–634
Salgarello M, Visconti G, Rusciani A (2011) Breast fat grafting with platelet-rich plasma: a comparative clinical study and current state of the art. Plast Reconstr Surg 127:2176–2185
Gentile P, Orlandi A, Scioli MG et al (2012) A comparative translational study: the combined use of enhanced stromal vascular fraction and platelet-rich plasma improves fat grafting maintenance in breast reconstruction. Stem Cells Transl Med 1:341–351
Gentile P, Di Pasquali C, Bocchini I et al (2013) Breast reconstruction with autologous fat graft mixed with platelet-rich plasma. Surg Innov 20:370–376
Fiaschetti V, Pistolese CA, Fornari M et al (2013) Magnetic resonance imaging and ultrasound evaluation after breast autologous fat grafting combined with platelet-rich plasma. Plast Reconstr Surg 132:498e–509e
Keyhan SO, Hemmat S, Badri AA et al (2013) Use of platelet-rich fibrin and platelet-rich plasma in combination with fat graft: Which is more effective during facial lipostructure? J Oral Maxillofac Surg 71:610–621
Cervelli V, Bocchini I, Di Pasquali C et al (2013) P R L platelet-rich lipotransfert: our experience and current state of art in the combined use of fat and PRP. Biomed Res Int 2013:434191
Gentile P, De Angelis B, Pasin M et al (2014) Adipose-derived stromal vascular fraction cells and platelet-rich plasma: basic and clinical evaluation for cell-based therapies in patients with scars on the face. J Craniofac Surg 25:267–272
Bennett NT, Schultz GS (1993) Growth factors and wound healing: biochemical properties of growth factors and their receptors. Am J Surg 165:728–737
Sanchez AR, Sheridan PJ, Kupp LI (2003) Is platelet-rich plasma the perfect enhancement factor? a current review. Int J Oral Maxillofac Implants 18:93–103
Anitua E, Andia I, Ardanza B et al (2004) Autologous platelets as a source of proteins for healing and tissue regeneration. Thromb Haemost 91:4–15
Fernandez-Barbero JE, Galindo-Moreno P, Avila-Ortiz G et al (2006) Flow cytometric and morphological characterization of platelet-rich plasma gel. Clin Oral Implants Res 17:687–693
El-Sharkawy H, Kantarci A, Deady J et al (2007) Platelet-rich plasma: growth factors and pro- and antiinflammatory properties. J Periodontol 78:661–669
Eppley BL, Woodell JE, Higgins J (2004) Platelet quantification and growth factor analysis from platelet-rich plasma: implications for wound healing. Plast Reconstr Surg 114:1502–1508
Sommer B, Sattler G (2000) Current concepts of fat graft survival: histology of aspirated adipose tissue and review of the literature. Dermatol Surg 26:1159–1166
Yuksel E, Weinfeld AB, Cleek R et al (2000) Increased free fat-graft survival with the long-term, local delivery of insulin, insulin-like growth factor-I, and basic fibroblast growth factor by PLGA/PEG microspheres. Plast Reconstr Surg 105:1712–1720
Rophael JA, Craft RO, Palmer JA et al (2007) Angiogenic growth factor synergism in a murine tissue engineering model of angiogenesis and adipogenesis. Am J Pathol 171:2048–2057
Craft RO, Rophael J, Morrison WA et al (2009) Effect of local long-term delivery of platelet-derived growth factor (PDGF) on injected fat graft survival in severe combined immunodeficient (SCID) mice. J Plast Reconstr Aesthet Surg 62:235–243
Moya ML, Cheng MH, Huang JJ et al (2010) The effect of FGF-1 loaded alginate microbeads on neovascularization and adipogenesis in a vascular pedicle model of adipose tissue engineering. Biomaterials 31:2816–2826
Zhang J, Middleton KK, Fu FH et al (2013) HGF mediates the antiinflammatory effects of PRP on injured tendons. PLoS ONE 8:e67303
Randelli PS, Arrigoni P, Cabitza P et al (2008) Autologous platelet rich plasma for arthroscopic rotator cuff repair: a pilot study. Disabil Rehabil 30:1584–1589
Mishra A, Pavelko T (2006) Treatment of chronic elbow tendinosis with buffered platelet-rich plasma. Am J Sports Med 34:1774–1778
Peerbooms JC, Sluimer J, Bruijn DJ et al (2010) Positive effect of an autologous platelet concentrate in lateral epicondylitis in a double-blind randomized controlled trial: platelet-rich plasma versus corticosteroid injection with a 1-year follow-up. Am J Sports Med 38:255–262
Everts PA, Devilee RJ, Brown Mahoney C et al (2006) Platelet gel and fibrin sealant reduce allogeneic blood transfusions in total knee arthroplasty. Acta Anaesthesiol Scand 50:593–599
Sanchez M, Anitua E, Azofra J et al (2007) Comparison of surgically repaired Achilles tendon tears using platelet-rich fibrin matrices. Am J Sports Med 35:245–251
Middleton KK, Barro V, Muller B et al (2012) Evaluation of the effects of platelet-rich plasma (PRP) therapy involved in the healing of sports-related soft tissue injuries. Iowa Orthop J 32:150–163
Kakudo N, Minakata T, Mitsui T et al (2008) Proliferation promoting effect of platelet-rich plasma on human adipose-derived stem cells and human dermal fibroblasts. Plast Reconstr Surg 122:1352–1360
Anitua E, Sanchez M, Nurden AT et al (2006) New insights into and novel applications for platelet-rich fibrin therapies. Trends Biotechnol 24:227–234
Kang YH, Jeon SH, Park JY et al (2011) Platelet-rich fibrin is a bioscaffold and reservoir of growth factors for tissue regeneration. Tissue Eng Part A 17:349–359
Wu W, Zhang J, Dong Q et al (2009) Platelet-rich plasma: a promising cell carrier for micro-invasive articular cartilage repair. Med Hypotheses 72:455–457
Eppley BL, Pietrzak WS, Blanton M (2006) Platelet-rich plasma: a review of biology and applications in plastic surgery. Plast Reconstr Surg 118:147e–159e
Marx RE (2004) Platelet-rich plasma: evidence to support its use. J Oral Maxillofac Surg 62:489–496
He L, Lin Y, Hu X et al (2009) A comparative study of platelet-rich fibrin (PRF) and platelet-rich plasma (PRP) on the effect of proliferation and differentiation of rat osteoblasts in vitro. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 108:707–713
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Serra-Mestre, J.M., Serra-Renom, J.M., Martinez, L. et al. Platelet-Rich Plasma Mixed-Fat Grafting: A Reasonable Prosurvival Strategy for Fat GraftS?. Aesth Plast Surg 38, 1041–1049 (2014). https://doi.org/10.1007/s00266-014-0374-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00266-014-0374-7