Abstract
Introduction
The purpose of this article is to study whether the newly designed whole-process total hip arthroplasty (THA) robotic arm can improve the accuracy of prosthesis placement in THA.
Method
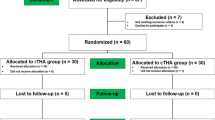
In this study, 72 patients undergoing THA were prospectively included and randomly divided into two groups. The experimental group was treated with THA assisted by a newly designed robotic arm. The control group received THA with conventional surgical methods. The imaging data were compared after operation.
Result
Compared with the conventional operation, the whole-process robotic arm can more accurately place the acetabular prosthesis in the anteversion safe zone of 5 ~ 25°, but in terms of the inclination angle, whether the reference is the safe zone of 30 ~ 50° or 30 ~ 45°, there is no statistical difference between the two groups. The average lower limb length discrepancy (LLLD) in the experimental group was 3.77 ± 8.31 mm longer than contralateral side, while the counterpart in the control group was 8.39 ± 9.11 mm, with significant difference (P = 0.029). The femoral prosthesis was fixed in neutral position in 35 (100%) cases in the experimental group and only 30 (83.3%) in the control group (P = 0.036). There was no significant difference in the recovery of hip offset, femoral anteversion, and canal fill ratio (CFR) between the two groups.
Conclusion
Robotic arm can improve the accuracy of anteversion of acetabular cup, restore the consistency of the length of lower limbs, and more accurately implant the femoral prosthesis to the neutral position in the coronal position.
Clinical trial registration number
ChiCTR2100044124 (date of registration: 2021–3-11).




Similar content being viewed by others
References
Ledford CK et al (2019) What are the contemporary etiologies for revision surgery and revision after primary, noncemented total hip arthroplasty? J Am Acad Orthop Surg 27(24):933–938
Elson L et al (2015) Precision of acetabular cup placement in robotic integrated total hip arthroplasty. Hip Int 25(6):531–536
Seagrave KG et al (2017) Acetabular cup position and risk of dislocation in primary total hip arthroplasty. Acta Orthop 88(1):10–17
Hodge WA, Andriacchi TP, Galante JO (1991) A relationship between stem orientation and function following total hip arthroplasty. J Arthroplasty 6(3):229–235
Belzunce MA et al (2020) Uncemented femoral stem orientation and position in total hip arthroplasty: a CT study. J Orthop Res 38(7):1486–1496
Widmer KH (2020) The impingement-free, prosthesis-specific, and anatomy-adjusted combined target zone for component positioning in THA depends on design and implantation parameters of both components. Clin Orthop Relat Res 478(8):1904–1918
Barrack RL et al (2013) Accuracy of acetabular component position in hip arthroplasty. J Bone Joint Surg Am 95(19):1760–1768
Callanan MC et al (2011) The John Charnley Award: risk factors for cup malpositioning: quality improvement through a joint registry at a tertiary hospital. Clin Orthop Relat Res 469(2):319–329
Kayani B et al (2021) The learning curve of robotic-arm assisted acetabular cup positioning during total hip arthroplasty. Hip Int 31(3):311–319
Kim HS et al (2022) Distribution and outliers of anteversion of short-length cementless stem. Int Orthop 46(4):725–732
Konyves A, Bannister GC (2005) The importance of leg length discrepancy after total hip arthroplasty. J Bone Joint Surg Br 87:155e7. https://doi.org/10.1302/0301-620X.87B2.14878
Bonnin MP et al (2012) Do we medialise the hip centre of rotation in total hip arthroplasty? Influence of acetabular offset and surgical technique. Hip Int 22(4):371–378
Peng Y et al (2018) In vivo sliding distance on the metal-on-polyethylene total hip arthroplasty articulation using patient-specific gait analysis. J Orthop Res 36(12):3151–3160
Xu S et al (2020) Robotic-arm assisted direct anterior total hip arthroplasty; improving implant accuracy. Surg Technol Int 38:347–352
Ries C et al (2019) Femoral stem subsidence in cementless total hip arthroplasty: a retrospective single-centre study. Int Orthop 43(2):307–314
D’Ambrosio A et al (2020) Influence of femoral morphology and canal fill ratio on early radiological and clinical outcomes of uncemented total hip arthroplasty using a fully coated stem. Bone Joint Res 9(4):182–191
Leiss F et al (2022) Differences in femoral component subsidence rate after THA using an uncemented collarless femoral stem: full weight-bearing with an enhanced recovery rehabilitation versus partial weight-bearing. Arch Orthop Trauma Surg 142(4):673–680
McGoldrick NP et al (2022) Can we predict fracture when using a short cementless femoral stem in the anterior approach? J Arthroplasty S0883–5403(22):00338–2
Desai AS, Dramis A, Board TN (2013) Leg length discrepancy after total hip arthroplasty: a review of literature. Curr Rev Musculoskelet Med 6(4):336–341
Waibel FWA et al (2021) Symptomatic leg length discrepancy after total hip arthroplasty is associated with new onset of lower back pain. Orthop Traumatol Surg Res 107(1):102761
Iversen MD et al (2011) Influence of self-reported limb length discrepancy on function and satisfaction 6 years after total hip replacement. J Geriatr Phys Ther 34(3):148–152
O’brien S, Kernohan G, Fitzpatrick C et al (2010) Perception of imposed leg length inequality in normal subjects. Hip Int 20(4):505–511
Robinson M et al (2012) Effect of restoration of combined offset on stability of large head THA. Hip Int 22(3):248–253
Worlicek M et al (2020) Restoration of leg length and offset correlates with trochanteric pain syndrome in total hip arthroplasty. Sci Rep 10(1):7107
Mahmood SS et al (2016) Association between changes in global femoral offset after total hip arthroplasty and function, quality of life, and abductor muscle strength. A prospective cohort study of 222 patients. Acta Orthop 87(1):36–41
Sato H et al (2020) Effect of femoral offset and limb length discrepancy on hip joint muscle strength and gait trajectory after total hip arthroplasty. Gait Posture 77:276–282
Flecher X, Ollivier M, Argenson JN (2016) Lower limb length and offset in total hip arthroplasty. Orthop Traumatol Surg Res 102(1 Suppl):S9-20
Tezuka T et al (2019) Functional safe zone is superior to the Lewinnek safe zone for total hip arthroplasty: why the Lewinnek safe zone is not always predictive of stability. J Arthroplasty 34(1):3–8
Tang H et al (2022) Conversion of the sagittal functional safe zone to the coronal plane using a mathematical algorithm: the reason for failure of the lewinnek safe zone. J Bone Joint Surg Am 00:1–8
Gavaskar A et al (2021) Choice of surgical approach influences the combined anteversion needed for a stable and impingement-free total hip arthroplasty. Eur J Orthop Surg Traumatol 31(6):1023–1028
Li L et al (2020) A specific anteversion of cup and combined anteversion for total hip arthroplasty using lateral approach. Orthop Surg 12(6):1663–1673
Author information
Authors and Affiliations
Contributions
WW wrote the paper. CL, YL, and XL collected the data and participated in writing and revising the paper. HZ, HX, ZZ, GW, and CR performed THA procedures. HNZ designed the whole study. All authors have read and approved the final manuscript.
Corresponding author
Ethics declarations
Ethics approval
This study was performed in line with the principles of the Declaration of Helsinki. Approval was granted by the Ethics Committee of the Affiliated Hospital of Qingdao University (Ethical approval No. QYFYEC2020-01701).
Consent to participate
Informed consent was obtained from all individual participants included in the study.
Consent for publication
Not applicable.
Competing interests
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Wang, W., Zhang, Z., Wang, G. et al. Prospective randomized controlled trial on the accuracy of prosthesis positioning in total hip arthroplasty assisted by a newly designed whole-process robotic arm. International Orthopaedics (SICOT) 47, 413–419 (2023). https://doi.org/10.1007/s00264-022-05501-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00264-022-05501-2