Abstract
Purpose
To evaluate the factors influencing the baseline Knee Injury and Osteoarthritis Outcome Score (KOOS) in patients with knee cartilage defects and planned cartilage repair surgery and to provide baseline KOOS data from a large patient population.
Material and methods
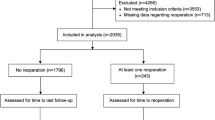
Between October 2013 and April 2017, a total of 2815 patients assigned for cartilage repair surgery were included into the German Cartilage Registry (KnorpelRegister DGOU) and their data were analyzed for the present study. Multivariate regression model and ANOVA were used to detect patient- and defect-specific factors with an influence on baseline KOOS. In addition, KOOS baseline data was calculated and compared according to these parameters.
Results
Sex, age, body mass index (BMI), and smoking status were revealed as patient-specific factors, and defect location and the number of previous knee and cartilage operations were revealed as defect-specific factors with a significant influence on baseline KOOS. Most subscores were affected in accordance with the total KOOS. Interestingly, defect ICRS grade, defect size, and symptom duration had no significant influence. The mean baseline KOOS was 56.7 (± 17.9). Men had significantly higher mean overall KOOS (60 ± 17.3 vs. 51.8 ± 17.6, p < 0.001) than women, and patients with a BMI over 30 and smokers scored significantly lower (58.07 ± 17.67 vs. 50.32 ± 17.29, p < 0.001; 57.64 ± 17.86 vs. 53.59 ± 18.06, p < 0.001). Patients with two or more previous knee operations as well as patients with more than one previous cartilage procedure also showed significantly lower overall KOOS (57.19 ± 17.89 vs. 54.56 ± 17.58, p < 0.001; 57.68 ± 18.01 vs. 52.72 ± 17.58, p < 0.001).
Conclusion
Several factors influencing baseline KOOS data in patients with knee cartilage defects assigned for cartilage repair surgery could be detected. Their individual influence in the multivariate linear regression model was not very strong. Baseline data according to these criteria is presented in this paper.
Similar content being viewed by others
References
Widuchowski W, Widuchowski J, Trzaska T (2007) Articular cartilage defects: study of 25,124 knee arthroscopies. Knee 14(3):177–182
Hjelle K et al (2002) Articular cartilage defects in 1,000 knee arthroscopies. Arthroscopy 18(7):730–734
Niemeyer P et al (2013) Autologous chondrocyte implantation (ACI) for cartilage defects of the knee: a guideline by the Working Group “Tissue Regeneration” of the German Society of Orthopaedic Surgery and Traumatology (DGOU). Z Orthop Unfall 151(1):38–47
Cole BJ, Pascual-Garrido C, Grumet RC (2009) Surgical management of articular cartilage defects in the knee. J Bone Joint Surg Am 91(7):1778–1790
Vaquero J, Forriol F (2012) Knee chondral injuries: clinical treatment strategies and experimental models. Injury 43(6):694–705
Heir S et al (2010) Focal cartilage defects in the knee impair quality of life as much as severe osteoarthritis: a comparison of knee injury and osteoarthritis outcome score in 4 patient categories scheduled for knee surgery. Am J Sports Med 38(2):231–237
Walczak BE, McCulloch PC, Kang RW, Zelazny A, Tedeschi F, Cole BJ (2008) Abnormal findings on knee magnetic resonance imaging in asymptomatic NBA players. J Knee Surg 21(1):27–33
Niethammer TR, Holzgruber M, Gülecyüz MF, Weber P, Pietschmann MF, Müller PE (2017) Matrix based autologous chondrocyte implantation in children and adolescents: a match paired analysis in a follow-up over three years post-operation. Int Orthop 41(2):343–350
Volz M, Schaumburger J, Frick H, Grifka J, Anders S (2017) A randomized controlled trial demonstrating sustained benefit of autologous matrix-induced chondrogenesis over microfracture at five years. Int Orthop 41(4):797–804
Brix M, Kaipel M, Kellner R, Schreiner M, Apprich S, Boszotta H, Windhager R, Domayer S, Trattnig S (2016) Successful osteoconduction but limited cartilage tissue quality following osteochondral repair by a cell-free multilayered nano-composite scaffold at the knee. Int Orthop 40(3):625–632
Roessler PP, Pfister B, Gesslein M, Figiel J, Heyse TJ, Colcuc C, Lorbach O, Efe T, Schüttler KF (2015) Short-term follow up after implantation of a cell-free collagen type I matrix for the treatment of large cartilage defects of the knee. Int Orthop 39(12):2473–2479
Roos EM, Lohmander LS (2003) Knee injury and Osteoarthritis Outcome Score (KOOS): from joint injury to osteoarthritis. Health Qual Life Outcomes 1:64
Roos EM, Engelhart L et al (2011) ICRS recommendation document: patient-reported outcome instruments for use in patients with articular cartilage defects. Cartilage 2(2):122–136
Bekkers JE, de Windt TS, Raijmakers NJ, Dhert WJ, Saris DB (2009) Validation of the Knee Injury and Osteoarthritis Outcome Score (KOOS) for the treatment of focal cartilage lesions. Osteoarthr Cartil 17(11):1434–1439
Roos EM et al (1998) Knee Injury and Osteoarthritis Outcome Score (KOOS) -development of a self-administered outcome measure. J Orthop Sports Phys Ther 28(2):88–96
Tegner Y, Lysholm J (1985) Rating systems in the evaluation of knee ligament injuries. Clin Orthop Relat Res (198):43–49
Collins NJ, Prinsen CA, Christensen R, Bartels EM, Terwee CB, Roos EM (2016) Knee Injury and Osteoarthritis Outcome Score (KOOS): systematic review and meta-analysis of measurement properties. Osteoarthr Cartil 24(8):1317–1329
Cameron KL, Thompson BS, Peck KY, Owens BD, Marshall SW, Svoboda SJ (2013) Normative values for the KOOS and WOMAC in a young athletic population: history of knee ligament injury is associated with lower scores. Am J Sports Med 41(3):582–589
Paradowski PT, Bergman S, Sundén-Lundius A, Lohmander LS, Roos EM (2006) Knee complaints vary with age and gender in the adult population. Population-based reference data for the Knee injury and Osteoarthritis Outcome Score (KOOS). BMC Musculoskelet Disord 7:38
Røtterud JH, Sivertsen EA, Forssblad M, Engebretsen L, Arøen A (2013) Effect of meniscal and focal cartilage lesions on patient-reported outcome after anterior cruciate ligament reconstruction: a nationwide cohort study from Norway and Sweden of 8476 patients with 2-year follow-up. Am J Sports Med 41(3):535–543
Cox CL, Huston LJ, Dunn WR et al (2014) Are articular cartilage lesions and meniscus tears predictive of IKDC, KOOS, and Marx activity level outcomes after ACL reconstruction? A 6-year multicenter cohort study. Am J Sports Med 42(5):1058–1067
Jaiswal PK, Macmull S, Bentley G, Carrington RW, Skinner JA, Briggs TW (2009) Does smoking influence outcome after autologous chondrocyte implantation?: a case-controlled study. J Bone Joint Surg Br 91(12):1575–1578
Jaiswal PK, Bentley G, Carrington RW, Skinner JA, Briggs TW (2012) The adverse effect of elevated body mass index on outcome after autologous chondrocyte implantation. J Bone Joint Surg Br 94(10):1377–1381
Illingworth KD, El Bitar Y, Siewert K, Scaife SL, El-Amin S, Saleh KJ (2014) Correlation of WOMAC and KOOS scores to tibiofemoral cartilage loss on plain radiography and 3 tesla MRI: data from the osteoarthritis initiative. Knee Surg Sports Traumatol Arthrosc 22(7):1649–1658
Michalitsis S, Vlychou M, Malizos KN, Thriskos P, Hantes ME (2015) Meniscal and articular cartilage lesions in the anterior cruciate ligament-deficient knee: correlation between time from injury and knee scores. Knee Surg Sports Traumatol Arthrosc 23(1):232–239
Maurer J, Grotejohann B, Jenkner C, Schneider C, Flury T, Tassoni A, Angele P, Fritz J, Albrecht D, Niemeyer P (2016) A registry for evaluation of efficiency and safety of surgical treatment of cartilage defects: the German Cartilage Registry (KnorpelRegister DGOU). JMIR Res Protoc 29;5(2):e122
Engen CN, Engebretsen L, Årøen A (2010) Knee cartilage defect patients enrolled in randomized controlled trials are not representative of patients in orthopedic practice. Cartilage 1(4):312–319
Imam MA, Barke S, Stafford GH, Parkin D, Field RE (2014) Loss to follow-up after total hip replacement: a source of bias in patient reported outcome measures and registry datasets? Hip Int 24(5):465–472
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
The study was registered at the DRKS website (DRKS Number: DRKS00005617) and approved by the ethical committee (Approval Number 105/13 (Freiburg University). Informed consent was given by all patients.
Conflict of interest
The authors declare that they have no conflict of interest.
Rights and permissions
About this article
Cite this article
Hochrein, A., Zinser, W., Spahn, G. et al. What parameters affect knee function in patients with untreated cartilage defects: baseline data from the German Cartilage Registry . International Orthopaedics (SICOT) 43, 1107–1112 (2019). https://doi.org/10.1007/s00264-018-4125-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00264-018-4125-2