Abstract
Purpose
To compare PET/CT, MRI and ultrasonography in detecting recurrence of nasopharyngeal carcinoma and identify their benefit in staging, contouring and overall survival (OS).
Methods
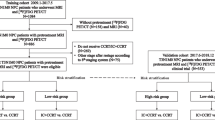
Cohort A included 1453 patients with or without histopathology-confirmed local recurrence, while cohort B consisted of 316 patients with 606 histopathology-confirmed lymph nodes to compare the sensitivities and specificities of PET/CT, MRI and ultrasonography using McNemar test. Cohorts C and D consisted of 273 patients from cohort A and 267 patients from cohort B, respectively, to compare the distribution of PET/CT-based and MRI-based rT-stage and rN-stage and the accuracy of rN-stage using McNemar test. Cohort E included 30 random patients from cohort A to evaluate the changes in contouring with or without PET/CT by related-samples T test or Wilcoxon rank test. The OS of 61 rT3-4N0M0 patients staged by PET/CT plus MRI (cohort F) and 67 MRI-staged rT3-4N0M0 patients (cohort G) who underwent similar salvage treatment were compared by log-rank test and Cox regression.
Results
PET/CT had similar specificity to MRI but higher sensitivity (93.9% vs. 79.3%, P < 0.001) in detecting local recurrence. PET/CT, MRI and ultrasonography had comparable specificities, but PET/CT had greater sensitivity than MRI (90.9% vs. 67.6%, P < 0.001) and similar sensitivity to ultrasonography in diagnosing lymph nodes. According to PET/CT, more patients were staged rT3-4 (82.8% vs. 68.1%, P < 0.001) or rN + (89.9% vs. 69.3%, P < 0.001), and the rN-stage was more accurate (90.6% vs. 73.8%, P < 0.001). Accordingly, the contours of local recurrence were more precise (median Dice similarity coefficient 0.41 vs. 0.62, P < 0.001) when aided by PET/CT plus MRI. Patients staged by PET/CT plus MRI had a higher 3-year OS than patients staged by MRI alone (85.5% vs. 60.4%, P = 0.006; adjusted HR = 0.34, P = 0.005).
Conclusion
PET/CT more accurately detected and staged recurrence of nasopharyngeal carcinoma and accordingly complemented MRI, providing benefit in contouring and OS.



Similar content being viewed by others
Data availability
The dataset generated during and/or analysed during the current study is available from the corresponding author on reasonable request.
References
Ng SH, Liu HM, Ko SF, Hao SP, Chong VF. Posttreatment imaging of the nasopharynx. Eur J Radiol. 2002;44:82–95. https://doi.org/10.1016/s0720-048x(02)00061-x.
Abdel Razek AA, Kandeel AY, Soliman N, El-shenshawy HM, Kamel Y, Nada N, et al. Role of diffusion-weighted echo-planar MR imaging in differentiation of residual or recurrent head and neck tumors and posttreatment changes. AJNR Am J Neuroradiol. 2007;28:1146–52. https://doi.org/10.3174/ajnr.A0491.
Tshering Vogel DW, Zbaeren P, Geretschlaeger A, Vermathen P, De Keyzer F, Thoeny HC. Diffusion-weighted MR imaging including bi-exponential fitting for the detection of recurrent or residual tumour after (chemo)radiotherapy for laryngeal and hypopharyngeal cancers. Eur Radiol. 2013;23:562–9. https://doi.org/10.1007/s00330-012-2596-x.
Vandecaveye V, De Keyzer F, Nuyts S, Deraedt K, Dirix P, Hamaekers P, et al. Detection of head and neck squamous cell carcinoma with diffusion weighted MRI after (chemo)radiotherapy: correlation between radiologic and histopathologic findings. Int J Radiat Oncol Biol Phys. 2007;67:960–71. https://doi.org/10.1016/j.ijrobp.2006.09.020.
Driessen JP, Peltenburg B, Philippens MEP, Huijbregts JE, Pameijer FA, de Bree R, et al. Prospective comparative study of MRI including diffusion-weighted images versus FDG PET-CT for the detection of recurrent head and neck squamous cell carcinomas after (chemo)radiotherapy. Eur J Radiol. 2019;111:62–7. https://doi.org/10.1016/j.ejrad.2018.12.004.
Comoretto M, Balestreri L, Borsatti E, Cimitan M, Franchin G, Lise M. Detection and restaging of residual and/or recurrent nasopharyngeal carcinoma after chemotherapy and radiation therapy: comparison of MR imaging and FDG PET/CT. Radiology. 2008;249:203–11. https://doi.org/10.1148/radiol.2491071753.
Ng SH, Chan SC, Yen TC, Liao CT, Chang JT, Ko SF, et al. Comprehensive imaging of residual/recurrent nasopharyngeal carcinoma using whole-body MRI at 3 T compared with FDG-PET-CT. Eur Radiol. 2010;20:2229–40. https://doi.org/10.1007/s00330-010-1784-9.
Yoon JH, Kim JY, Moon HJ, Youk JH, Son EJ, Kim EK, et al. Contribution of computed tomography to ultrasound in predicting lateral lymph node metastasis in patients with papillary thyroid carcinoma. Ann Surg Oncol. 2011;18:1734–41. https://doi.org/10.1245/s10434-010-1527-9.
Yang WT, Metreweli C, Lam PK, Chang J. Benign and malignant breast masses and axillary nodes: evaluation with echo-enhanced color power Doppler US. Radiology. 2001;220:795–802. https://doi.org/10.1148/radiol.2203001545.
Steppan I, Reimer D, Muller-Holzner E, Marth C, Aigner F, Frauscher F, et al. Breast cancer in women: evaluation of benign and malignant axillary lymph nodes with contrast-enhanced ultrasound. Ultraschall Med. 2010;31:63–7. https://doi.org/10.1055/s-0028-1109847.
Yoon DY, Hwang HS, Chang SK, Rho YS, Ahn HY, Kim JH, et al. CT, MR, US,18F-FDG PET/CT, and their combined use for the assessment of cervical lymph node metastases in squamous cell carcinoma of the head and neck. Eur Radiol. 2009;19:634–42. https://doi.org/10.1007/s00330-008-1192-6.
Pellini R, Manciocco V, Turri-Zanoni M, Vidiri A, Sanguineti G, Marucci L, et al. Planned neck dissection after chemoradiotherapy in advanced oropharyngeal squamous cell cancer: the role of US, MRI and FDG-PET/TC scans to assess residual neck disease. J Craniomaxillofac Surg. 2014;42:1834–9. https://doi.org/10.1016/j.jcms.2014.06.023.
Costantino A, Mercante G, D’Ascoli E, Ferreli F, Di Tommaso L, Franzese C, et al. Accuracy of fine-needle aspiration cytology in detecting cervical node metastasis after radiotherapy: systematic review and meta-analysis. Head Neck. 2021;43:987–96. https://doi.org/10.1002/hed.26536.
Tang LL, Chen YP, Chen CB, Chen MY, Chen NY, Chen XZ, et al. The Chinese Society of Clinical Oncology (CSCO) clinical guidelines for the diagnosis and treatment of nasopharyngeal carcinoma. Cancer Commun (Lond). 2021;41:1195–227. https://doi.org/10.1002/cac2.12218.
Delbeke D, Coleman RE, Guiberteau MJ, Brown ML, Royal HD, Siegel BA, et al. Procedure guideline for tumor imaging with 18F-FDG PET/CT 1.0. J Nucl Med. 2006;47:885–95.
Aiken AH, Farley A, Baugnon KL, Corey A, El-Deiry M, Duszak R, et al. Implementation of a novel surveillance template for head and neck cancer: neck imaging reporting and data system (NI-RADS). J Am Coll Radiol. 2016;13:743-6.e1. https://doi.org/10.1016/j.jacr.2015.09.032.
Aiken AH, Hudgins PA. Neck imaging reporting and data system. Magn Reson Imaging Clin N Am. 2018;26:51–62. https://doi.org/10.1016/j.mric.2017.08.004.
Yen RF, Hung RL, Pan MH, Wang YH, Huang KM, Lui LT, et al. 18-fluoro-2-deoxyglucose positron emission tomography in detecting residual/recurrent nasopharyngeal carcinomas and comparison with magnetic resonance imaging. Cancer. 2003;98:283–7. https://doi.org/10.1002/cncr.11519.
van den Brekel MW, Stel HV, Castelijns JA, Nauta JJ, van der Waal I, Valk J, et al. Cervical lymph node metastasis: assessment of radiologic criteria. Radiology. 1990;177:379–84. https://doi.org/10.1148/radiology.177.2.2217772.
Ng SH, Chang JT, Chan SC, Ko SF, Wang HM, Liao CT, et al. Nodal metastases of nasopharyngeal carcinoma: patterns of disease on MRI and FDG PET. Eur J Nucl Med Mol Imaging. 2004;31:1073–80. https://doi.org/10.1007/s00259-004-1498-9.
Yang SS, Wu YS, Chen WC, Zhang J, Xiao SM, Zhang BY, et al. Benefit of [18F]-FDG PET/CT for treatment-naive nasopharyngeal carcinoma. Eur J Nucl Med Mol Imaging. 2022;49:980–91. https://doi.org/10.1007/s00259-021-05540-8.
Liu YP, Wen YH, Tang J, Wei Y, You R, Zhu XL, et al. Endoscopic surgery compared with intensity-modulated radiotherapy in resectable locally recurrent nasopharyngeal carcinoma: a multicentre, open-label, randomised, controlled, phase 3 trial. Lancet Oncol. 2021;22:381–90. https://doi.org/10.1016/S1470-2045(20)30673-2.
Wei J, Pei S, Zhu X. Comparison of 18F-FDG PET/CT, MRI and SPECT in the diagnosis of local residual/recurrent nasopharyngeal carcinoma: a meta-analysis. Oral Oncol. 2016;52:11–7. https://doi.org/10.1016/j.oraloncology.2015.10.010.
Wang C, Liu L, Lai S, Su D, Liu Y, Jin G, et al. Diagnostic value of diffusion-weighted magnetic resonance imaging for local and skull base recurrence of nasopharyngeal carcinoma after radiotherapy. Medicine (Baltimore). 2018;97: e11929. https://doi.org/10.1097/md.0000000000011929.
Xu JF, Wu XW, Wang WQ, Kong LL, Wu LM, Wang F. Value of diffusion-weighted magnetic resonance imaging on the follow-up of nasopharyngeal carcinoma after radiotherapy. J Xray Sci Technol. 2014;22:605–12. https://doi.org/10.3233/xst-140448.
Piao Y, Cao C, Xu Y, Huang S, Jiang F, Jin T, et al. Detection and staging of recurrent or metastatic nasopharyngeal carcinoma in the era of FDG PET/MR. Eur Arch Otorhinolaryngol. 2022;279:353–9. https://doi.org/10.1007/s00405-021-06779-5.
Chan SC, Yeh CH, Yen TC, Ng SH, Chang JT, Lin CY, et al. Clinical utility of simultaneous whole-body (18)F-FDG PET/MRI as a single-step imaging modality in the staging of primary nasopharyngeal carcinoma. Eur J Nucl Med Mol Imaging. 2018;45:1297–308. https://doi.org/10.1007/s00259-018-3986-3.
Wang P, Hu S, Wang X, Ge Y, Zhao J, Qiao H, et al. Synthetic MRI in differentiating benign from metastatic retropharyngeal lymph node: combination with diffusion-weighted imaging. Eur Radiol. 2022. https://doi.org/10.1007/s00330-022-09027-4.
Funding
This work was supported by the Sun Yat-sen University Clinical Research 5010 Program (2015020).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethics approval
This study was performed in line with the principles of the Declaration of Helsinki. Approval was granted by the Ethics Committee of Sun Yat-sen University Cancer Center (SYSUCC) (No. B2020-222–01 and No. B2020-334–01).
Consent to participate
Informed consent was obtained from all individual participants included in the prospective study but was waved in the retrospective study.
Consent for publication
Not applicable.
Competing interests
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Pu-Yun OuYang, Zhi-Qiao Liu, Qing-Guang Lin, and Yun He are joint first authors.
Yi-Shan Wu, Xu Zhang, Chun-Yan Chen, and Fang-Yun Xie are joint senior authors.
This article is part of the Topical Collection on Oncology - Head and Neck
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
OuYang, PY., Liu, ZQ., Lin, QG. et al. Benefit of [18F] FDG PET/CT in the diagnosis and salvage treatment of recurrent nasopharyngeal carcinoma. Eur J Nucl Med Mol Imaging 50, 881–891 (2023). https://doi.org/10.1007/s00259-022-06020-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00259-022-06020-3