Abstract
Purpose
Defining an optimal imaging modality for assessment of therapy and the best time of evaluation are pivotal for ideal patient’s management.
Methods
223Ra (Xofigo®, formerly Alpharadin) has been approved by the FDA and European Medicines Agency for treatment of metastatic castration-resistant prostate cancer with painful osseous involvement.
Results
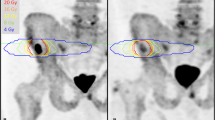
PET/CT imaging using various radiotracers such as 18F–FDG, 18F–FCH, 68Ga-PSMA and 18F–NaF have been investigated to mitigate the limitations of conventional imaging modalities. Diagnostic radiotracers that have properties similar to a therapeutic radiotracer will precisely assess of the possibility and efficacy of a treatment; this is the theranostic concept. An example of a diagnostic test employed for selecting targeted therapy is the combined use of 18F–fluoride PET/CT for evaluation of possible therapy with 223Ra.
Conclusion
This review examines the most recent publications related to this topic.







Similar content being viewed by others
References
Center MM, Jemal A, Lortet-Tieulent J, Ward E, Ferlay J, Brawley O, et al. International variation in prostate cancer incidence and mortality rates. Eur Urol. 2012;61:1079–92. doi:10.1016/j.eururo.2012.02.054.
McMurtry CT, McMurtry JM. Metastatic prostate cancer: complications and treatment. J Am Geriatr Soc. 2003;51:1136–42.
Yu KK, Hawkins RA. The prostate: diagnostic evaluation of metastatic disease. Radiol Clin N Am. 2000;38:139–57. ix
Cabrera ME, Rey PM, Carrio I, Montes A, Lopez DA. Response to 223Ra-dichloride in castration-resistant prostate cancer with bone metastasis: a case report. Oncol Lett. 2016;12:1323–8. doi:10.3892/ol.2016.4762.
Vali R, Loidl W, Pirich C, Langesteger W, Beheshti M. Imaging of prostate cancer with PET/CT using (18)F-Fluorocholine. Am J Nucl Med Mol Imaging. 2015;5:96–108.
Damle NA, Bal C, Bandopadhyaya GP, Kumar L, Kumar P, Malhotra A, et al. The role of 18F-fluoride PET-CT in the detection of bone metastases in patients with breast, lung and prostate carcinoma: a comparison with FDG PET/CT and 99mTc-MDP bone scan. Jpn J Radiol. 2013;31:262–9. doi:10.1007/s11604-013-0179-7.
National Comprehensive Cancer Network (NCCN): NCCN Guidelines for Supportive Care: Adult cancer pain. Version 2.2013.
Hamdy NA, Papapoulos SE. The palliative management of skeletal metastases in prostate cancer: use of bone-seeking radionuclides and bisphosphonates. Semin Nucl Med. 2001;31:62–8.
Apolo AB, Lindenberg L, Shih JH, Mena E, Kim JW, Park JC, et al. Prospective study evaluating Na18F PET/CT in predicting clinical outcomes and survival in advanced prostate cancer. J Nucl Med: Off Publ, Soc Nucl Med. 2016;57:886–92. doi:10.2967/jnumed.115.166512.
Pandit-Taskar N, Larson SM, Carrasquillo JA. Bone-seeking radiopharmaceuticals for treatment of osseous metastases, part 1: alpha therapy with 223Ra-dichloride. J Nucl Med. 2014;55:268–74. doi:10.2967/jnumed.112.112482.
Parker C, Nilsson S, Heinrich D, Helle SI, O’Sullivan JM, Fossa SD, et al. Alpha emitter radium-223 and survival in metastatic prostate cancer. N Engl J Med. 2013;369:213–23. doi:10.1056/NEJMoa1213755.
Kairemo K, Joensuu T, Rasulova N, Kiljunen T, Kangasmaki A. Evaluation of alpha-therapy with radium-223-dichloride in castration resistant metastatic prostate cancer-the role of gamma Scintigraphy in Dosimetry and pharmacokinetics. Diagnostics. 2015;5:358–68. doi:10.3390/diagnostics5030358.
Harrison MR, Wong TZ, Armstrong AJ, George DJ. Radium-223 chloride: a potential new treatment for castration-resistant prostate cancer patients with metastatic bone disease. Cancer Manag Res. 2013;5:1–14. doi:10.2147/CMAR.S25537.
Kairemo K, Joensuu T. Radium-223-dichloride in castration resistant metastatic prostate cancer-preliminary results of the response evaluation using F-18-fluoride PET/CT. Diagnostics. 2015;5:413–27. doi:10.3390/diagnostics5040413.
Love C, Din AS, Tomas MB, Kalapparambath TP, Palestro CJ. Radionuclide bone imaging: an illustrative review. Radiogr: Rev Publ Radiol Soc North Am, Inc. 2003;23:341–58. doi:10.1148/rg.232025103.
Pyka T, Okamoto S, Dahlbender M, Tauber R, Retz M, Heck M, et al. Comparison of bone scintigraphy and 68Ga-PSMA PET for skeletal staging in prostate cancer. Eur J Nucl Med Mol Imaging. 2016; doi:10.1007/s00259-016-3435-0.
Castellucci P, Jadvar H. PET/CT in prostate cancer: non-choline radiopharmaceuticals. Quart J Nucl Med Mol Imaging: Off Publ Ital Assoc Nucl Med. 2012;56:367–74.
Beauregard JM, Blouin AC, Fradet V, Caron A, Fradet Y, Lemay C, et al. FDG-PET/CT for pre-operative staging and prognostic stratification of patients with high-grade prostate cancer at biopsy. Cancer Imaging: Off Publ Int Cancer Imaging Soc. 2015;15:2. doi:10.1186/s40644-015-0038-0.
Effert PJ, Bares R, Handt S, Wolff JM, Bull U, Jakse G. Metabolic imaging of untreated prostate cancer by positron emission tomography with 18fluorine-labeled deoxyglucose. J Urol. 1996;155:994–8.
Liu IJ, Zafar MB, Lai YH, Segall GM, Terris MK. Fluorodeoxyglucose positron emission tomography studies in diagnosis and staging of clinically organ-confined prostate cancer. Urology. 2001;57:108–11.
Jadvar H, FDG PET in Prostate Cancer. PET Clin. 2009;4:155–61. doi:10.1016/j.cpet.2009.05.002.
Jadvar H. Prostate cancer: PET with 18F-FDG, 18F- or 11C-acetate, and 18F- or 11C-choline. J Nucl Med. 2011;52:81–9. doi:10.2967/jnumed.110.077941.
Oyama N, Akino H, Suzuki Y, Kanamaru H, Ishida H, Tanase K, et al. FDG PET for evaluating the change of glucose metabolism in prostate cancer after androgen ablation. Nucl Med Commun. 2001;22:963–9.
Iagaru A, Mosci C, Keu K, Mittra E, Hancock S, Pachynski R, et al. Combined NaF/FDG PET/CT evaluation of prostate cancer patients. J Nucl Med. 2014;55(supplement 1):1654.
Simoncic U, Perlman S, Liu G, Staab MJ, Straus JE, Jeraj R. Comparison of NaF and FDG PET/CT for assessment of treatment response in castration-resistant prostate cancers with osseous metastases. Clin Genitour Cancer. 2015;13:e7–e17. doi:10.1016/j.clgc.2014.07.001.
Tu Z, Mach RH. C-11 radiochemistry in cancer imaging applications. Curr Top Med Chem. 2010;10:1060–95.
Beheshti M, Vali R, Waldenberger P, Fitz F, Nader M, Hammer J, et al. The use of F-18 choline PET in the assessment of bone metastases in prostate cancer: correlation with morphological changes on CT. Mol Imaging Biol: MIB: Off Publ Acad Mol Imaging. 2009;11:446–54. doi:10.1007/s11307-009-0217-0.
Beheshti M, Imamovic L, Broinger G, Vali R, Waldenberger P, Stoiber F, et al. 18F choline PET/CT in the preoperative staging of prostate cancer in patients with intermediate or high risk of extracapsular disease: a prospective study of 130 patients. Radiology. 2010;254:925–33. doi:10.1148/radiol.09090413.
Beheshti M, Vali R, Langsteger W. [18F]fluorocholine PET/CT in the assessment of bone metastases in prostate cancer. Eur J Nucl Med Mol Imaging. 2007;34:1316–1317; author reply 8–9. doi:10.1007/s00259-007-0401-x.
Beheshti M, Vali R, Waldenberger P, Fitz F, Nader M, Loidl W, et al. Detection of bone metastases in patients with prostate cancer by 18F fluorocholine and 18F fluoride PET-CT: a comparative study. Eur J Nucl Med Mol Imaging. 2008;35:1766–74. doi:10.1007/s00259-008-0788-z.
Challapalli A, Barwick T, Tomasi G. M OD, contractor K, Stewart S, et al. exploring the potential of [11C]choline-PET/CT as a novel imaging biomarker for predicting early treatment response in prostate cancer. Nucl Med Commun. 2014;35:20–9. doi:10.1097/MNM.0000000000000014.
Langsteger W, Balogova S, Huchet V, Beheshti M, Paycha F, Egrot C, et al. Fluorocholine (18F) and sodium fluoride (18F) PET/CT in the detection of prostate cancer: prospective comparison of diagnostic performance determined by masked reading. Quart J Nucl Med Mol Imaging: Off Publ Ital Assoc Nucl Med. 2011;55:448–57.
Miyazaki KS, Kuang Y, Kwee SA. Changes in skeletal tumor activity on (18)F-choline PET/CT in patients receiving (223)radium radionuclide therapy for metastatic prostate cancer. Nucl Med Mol Imaging. 2015;49:160–4. doi:10.1007/s13139-014-0314-0.
Lee J, Sato MM, Coel MN, Lee KH, Kwee SA. Prediction of PSA progression in castration-resistant prostate cancer based on treatment-associated change in tumor burden quantified by 18F-Fluorocholine PET/CT. J Nucl Med. 2016;57:1058–64. doi:10.2967/jnumed.115.169177.
Demirkol MO, Acar O, Ucar B, Ramazanoglu SR, Saglican Y, Esen T. Prostate-specific membrane antigen-based imaging in prostate cancer: impact on clinical decision making process. Prostate. 2015;75:748–57. doi:10.1002/pros.22956.
Mease RC, Foss CA, Pomper MG. PET imaging in prostate cancer: focus on prostate-specific membrane antigen. Curr Top Med Chem. 2013;13:951–62.
Jadvar H, PSMA PET in Prostate Cancer. J Nucl Med. 2015;56:1131–2. doi:10.2967/jnumed.115.157339.
Baum RP, Kulkarni HR, Schuchardt C, Singh A, Wirtz M, Wiessalla S, et al. 177Lu-labeled prostate-specific membrane antigen Radioligand therapy of metastatic castration-resistant prostate cancer: safety and efficacy. J Nucl Med. 2016;57:1006–13. doi:10.2967/jnumed.115.168443.
Bouchelouche K, Choyke PL, Capala J. Prostate specific membrane antigen- a target for imaging and therapy with radionuclides. Discov Med. 2010;9:55–61.
Lutje S, Heskamp S, Cornelissen AS, Poeppel TD, van den Broek SA, Rosenbaum-Krumme S, et al. PSMA ligands for radionuclide imaging and therapy of prostate cancer: clinical status. Theranostics. 2015;5:1388–401. doi:10.7150/thno.13348.
Weineisen M, Schottelius M, Simecek J, Baum RP, Yildiz A, Beykan S, et al. 68Ga- and 177Lu-labeled PSMA I&T: optimization of a PSMA-targeted Theranostic concept and first proof-of-concept human studies. J Nucl Med. 2015;56:1169–76. doi:10.2967/jnumed.115.158550.
Maurer T, Eiber M, Schwaiger M, Gschwend JE. Current use of PSMA-PET in prostate cancer management. Nat Rev Urol. 2016;13:226–35. doi:10.1038/nrurol.2016.26.
Afshar-Oromieh A, Haberkorn U, Eder M, Eisenhut M, Zechmann CM. [68Ga]gallium-labelled PSMA ligand as superior PET tracer for the diagnosis of prostate cancer: comparison with 18F-FECH. Eur J Nucl Med Mol Imaging. 2012;39:1085–6. doi:10.1007/s00259-012-2069-0.
Afshar-Oromieh A, Malcher A, Eder M, Eisenhut M, Linhart HG, Hadaschik BA, et al. PET imaging with a [68Ga]gallium-labelled PSMA ligand for the diagnosis of prostate cancer: biodistribution in humans and first evaluation of tumour lesions. Eur J Nucl Med Mol Imaging. 2013;40:486–95. doi:10.1007/s00259-012-2298-2.
Afshar-Oromieh A, Zechmann CM, Malcher A, Eder M, Eisenhut M, Linhart HG, et al. Comparison of PET imaging with a (68)Ga-labelled PSMA ligand and (18)F-choline-based PET/CT for the diagnosis of recurrent prostate cancer. Eur J Nucl Med Mol Imaging. 2014;41:11–20. doi:10.1007/s00259-013-2525-5.
Lavalaye J, Kaldeway P, van Melick HH. Diffuse bone metastases on (68)Ga-PSMA PET-CT in a patient with prostate cancer and normal bone scan. Eur J Nucl Med Mol Imaging. 2016;43:1563–4. doi:10.1007/s00259-016-3398-1.
Thomas L, Balmus C, Ahmadzadehfar H, Gaertner F, Bundschuh R. Comparison of 99mTc-MDP bone scintigraphy (visual and automatic analysis with Exini) and 68Ga-PSMA PET/CT for staging of bone metastases in patients with prostate carcinoma undergoing therapy with 223Ra-dichlorid. J Nucl Med. 2016;57(no. supplement 2).
Giesel F, Kratochwil C, Fiedler H, Afshar-Oromieh A, Debus J, Haberkorn U, et al. Impact of 68Ga-PSMA-PET-CT to the radiotherapeutic management of prostate cancer patients. J Nucl Med. 2015; 56(supplement 3).
Agrawal A, Natarajan A, Bakshi G, Prakash G, Mahantshetty U, Murthy V, et al. Evaluation of skeletal metastases of prostate cancer with 68Ga PSMA PET/CT and 18F- NaF PET/CT and its comparison. J Nucl Med. 2016;57(supplement 2):559.
Soydal C, Ozkan E, Kaya B, Kucuk ON. Demonstration of response to androgen deprivation therapy by 68Ga-PSMA PET/CT. Clin Nucl Med. 2016; doi:10.1097/RLU.0000000000001316.
Uprimny C, Kroiss A, Nilica B, Buxbaum S, Decristoforo C, Horninger W, et al. (68)Ga-PSMA ligand PET versus (18)F-NaF PET: evaluation of response to (223)Ra therapy in a prostate cancer patient. Eur J Nucl Med Mol Imaging. 2015;42:362–3. doi:10.1007/s00259-014-2922-4.
Costeas A, Woodard HQ, Laughlin JS. Depletion of 18F from blood flowing through bone. J Nucl Med: Off Publ, Soc Nucl Med. 1970;11:43–5.
Schiepers C, Nuyts J, Bormans G, Dequeker J, Bouillon R, Mortelmans L, et al. Fluoride kinetics of the axial skeleton measured in vivo with fluorine-18-fluoride PET. J Nucl Med: Off Publ, Soc Nucl Med. 1997;38:1970–6.
Glendenning J, Cook G. Imaging breast cancer bone metastases: current status and future directions. Semin Nucl Med. 2013;43:317–23. doi:10.1053/j.semnuclmed.2013.02.002.
Beheshti M, Langsteger W. (18)F NaF PET/CT in the assessment of metastatic bone disease: comparison with specific PET tracers. PET Clin. 2012;7:303–14. doi:10.1016/j.cpet.2012.04.002.
Bortot DC, Amorim BJ, Oki GC, Gapski SB, Santos AO, Lima MC, et al. (1)(8)F-fluoride PET/CT is highly effective for excluding bone metastases even in patients with equivocal bone scintigraphy. Eur J Nucl Med Mol Imaging. 2012;39:1730–6. doi:10.1007/s00259-012-2195-8.
Even-Sapir E, Metser U, Mishani E, Lievshitz G, Lerman H, Leibovitch I. The detection of bone metastases in patients with high-risk prostate cancer: 99mTc-MDP planar bone scintigraphy, single- and multi-field-of-view SPECT, 18F-fluoride PET, and 18F-fluoride PET/CT. J Nucl Med: Off Publ, Soc Nucl Med. 2006;47:287–97.
Hillner BE, Siegel BA, Hanna L, Duan F, Quinn B, Shields AF. 18F-fluoride PET used for treatment monitoring of systemic cancer therapy: results from the National Oncologic PET registry. J Nucl Med: Off Publ, Soc Nucl Med. 2015;56:222–8. doi:10.2967/jnumed.114.150391.
Etchebehere EC, Araujo JC, Fox PS, Swanston NM, Macapinlac HA, Rohren EM. Prognostic factors in patients treated with 223Ra: the role of skeletal tumor burden on baseline 18F-fluoride PET/CT in predicting overall survival. J Nucl Med: Off Publ, Soc Nucl Med. 2015;56:1177–84. doi:10.2967/jnumed.115.158626.
Yu EY, Duan F, Muzi M, Deng X, Chin BB, Alumkal JJ, et al. Castration-resistant prostate cancer bone metastasis response measured by 18F-fluoride PET after treatment with dasatinib and correlation with progression-free survival: results from American College of Radiology Imaging Network 6687. J Nucl Med: Off Publ, Soc Nucl Med. 2015;56:354–60. doi:10.2967/jnumed.114.146936.
Nome R, Hernes E, Bogsrud TV, Bjoro T, Fossa SD. Changes in prostate-specific antigen, markers of bone metabolism and bone scans after treatment with radium-223. Scand J Urol. 2015;49:211–7. doi:10.3109/21681805.2014.982169.
Cook G Jr, Parker C, Chua S, Johnson B, Aksnes AK, Lewington VJ. 18F-fluoride PET: changes in uptake as a method to assess response in bone metastases from castrate-resistant prostate cancer patients treated with 223Ra-chloride (Alpharadin). EJNMMI Res. 2011;1:4. doi:10.1186/2191-219X-1-4.
Ahmadzadehfar H, Azgomi K, Hauser S, Wei X, Yordanova A, Gaertner F, et al. 68Ga-PSMA-11 PET as a gate-keeper for the treatment of metastatic prostate cancer with radium-223: proof of concept. J Nucl Med: Off Publ, Soc Nucl Med. 2016; doi:10.2967/jnumed.116.178533.
Nakajima K, Nakajima Y, Horikoshi H, Ueno M, Wakabayashi H, Shiga T, et al. Enhanced diagnostic accuracy for quantitative bone scan using an artificial neural network system: a Japanese multi-center database project. EJNMMI Res. 2013;3:83. doi:10.1186/2191-219X-3-83.
Poulsen MH, Rasmussen J, Edenbrandt L, Hoilund-Carlsen PF, Gerke O, Johansen A, et al. Bone scan Index predicts outcome in patients with metastatic hormone-sensitive prostate cancer. BJU Int. 2016;117:748–53. doi:10.1111/bju.13160.
Anand A, Morris MJ, Larson SM, Minarik D, Josefsson A, Helgstrand JT, et al. Automated bone scan Index as a quantitative imaging biomarker in metastatic castration-resistant prostate cancer patients being treated with enzalutamide. EJNMMI Res. 2016;6:23. doi:10.1186/s13550-016-0173-z.
Uemura K, Miyoshi Y, Kawahara T, Yoneyama S, Hattori Y, Teranishi J, et al. Prognostic value of a computer-aided diagnosis system involving bone scans among men treated with docetaxel for metastatic castration-resistant prostate cancer. BMC Cancer. 2016;16:109. doi:10.1186/s12885-016-2160-1.
Anand A, Morris MJ, Kaboteh R, Reza M, Tragardh E, Matsunaga N, et al. A Preanalytic validation study of automated bone scan Index: effect on accuracy and reproducibility due to the procedural Variabilities in bone scan image acquisition. J Nucl Med: Off Publ, Soc Nucl Med. 2016;57:1865–71. doi:10.2967/jnumed.116.177030.
Rohren EM, Etchebehere EC, Araujo JC, Hobbs BP, Swanston NM, Everding M, et al. Determination of skeletal tumor burden on 18F-fluoride PET/CT. J Nucl Med: Off Publ, Soc Nucl Med. 2015;56:1507–12. doi:10.2967/jnumed.115.156026.
Etchebehere EC, Araujo JC, Milton DR, Erwin WD, Wendt RE 3rd, Swanston NM, et al. Skeletal tumor burden on baseline 18F-fluoride PET/CT predicts bone marrow failure after 223Ra therapy. Clin Nucl Med. 2016;41:268–73. doi:10.1097/RLU.0000000000001118.
Muzahir S, Jeraj R, Liu G, Hall LT, Rio AM, Perk T, et al. Differentiation of metastatic vs degenerative joint disease using semi-quantitative analysis with (18)F-NaF PET/CT in castrate resistant prostate cancer patients. Am J Nucl Med Mol Imaging. 2015;5:162–8.
Sabbah N, Jackson T, Mosci C, Jamali M, Minamimoto R, Quon A, et al. 18F-sodium fluoride PET/CT in oncology: an atlas of SUVs. Clin Nucl Med. 2015;40:e228–31. doi:10.1097/RLU.0000000000000633.
Kurdziel KA, Shih JH, Apolo AB, Lindenberg L, Mena E, McKinney YY, et al. The kinetics and reproducibility of 18F-sodium fluoride for oncology using current PET camera technology. J Nucl Med: Off Publ, Soc Nucl Med. 2012;53:1175–84. doi:10.2967/jnumed.111.100883.
Oldan JD, Hawkins AS, Chin BB. (18)F sodium fluoride PET/CT in patients with prostate cancer: quantification of normal tissues, benign degenerative lesions, and malignant lesions. World J Nucl Med. 2016;15:102–8. doi:10.4103/1450-1147.172301.
Lin C, Bradshaw T, Perk T, Harmon S, Eickhoff J, Jallow N, et al. Repeatability of quantitative 18F-NaF PET: a multicenter study. J Nucl Med: Off Publ, Soc Nucl Med. 2016;57:1872–9. doi:10.2967/jnumed.116.177295.
Oldan JD, Turkington TG, Choudhury K, Chin BB. Quantitative differences in [(18)F] NaF PET/CT: TOF versus non-TOF measurements. Am J Nucl Med Mol Imaging. 2015;5:504–14.
Brito A, Santos A, Sasse AD, Cabello C, Oliveira P, Mosci C, Souza T, Amorim B, Lima M, Ramos CD, Etchebehere E. 18F–Fluoride PET/CT tumor burden quantification predicts survival in breast cancer Oncotarget. 2017 (article in press).
Piccardo A, Puntoni M, Morbelli S, Massollo M, Bongioanni F, Paparo F, et al. 18F-FDG PET/CT is a prognostic biomarker in patients affected by bone metastases from breast cancer in comparison with 18F-NaF PET/CT. Nuklearmedizin Nucl Med. 2015;54:163–72. doi:10.3413/Nukmed-0727-15-02.
Abikhzer G, Srour S, Fried G, Drumea K, Kozlener E, Frenkel A, et al. Prospective comparison of whole-body bone SPECT and sodium 18F-fluoride PET in the detection of bone metastases from breast cancer. Nucl Med Commun. 2016;37:1160–8. doi:10.1097/MNM.0000000000000568.
Minamimoto R, Loening A, Jamali M, Barkhodari A, Mosci C, Jackson T, et al. Prospective comparison of 99mTc-MDP Scintigraphy, combined 18F-NaF and 18F-FDG PET/CT, and whole-body MRI in patients with breast and prostate cancer. J Nucl Med: Off Publ, Soc Nucl Med. 2015;56:1862–8. doi:10.2967/jnumed.115.162610.
Gerety EL, Lawrence EM, Wason J, Yan H, Hilborne S, Buscombe J, et al. Prospective study evaluating the relative sensitivity of 18F-NaF PET/CT for detecting skeletal metastases from renal cell carcinoma in comparison to multidetector CT and 99mTc-MDP bone scintigraphy, using an adaptive trial design. Ann Oncol: Off J Eur Soc Med Oncol. 2015;26:2113–8. doi:10.1093/annonc/mdv289.
Kruger S, Buck AK, Mottaghy FM, Hasenkamp E, Pauls S, Schumann C, et al. Detection of bone metastases in patients with lung cancer: 99mTc-MDP planar bone scintigraphy, 18F-fluoride PET or 18F-FDG PET/CT. Eur J Nucl Med Mol Imaging. 2009;36:1807–12. doi:10.1007/s00259-009-1181-2.
Rao L, Zong Z, Chen Z, Wang X, Shi X, Yi C, et al. 18F-labeled NaF PET-CT in detection of bone metastases in patients with preoperative lung cancer. Medicine. 2016;95:e3490. doi:10.1097/MD.0000000000003490.
Subbiah V, Anderson P, Rohren E. Alpha Emitter radium 223 in high-risk osteosarcoma: first clinical evidence of response and blood–brain barrier penetration. JAMA Oncol. 2015;1:253–5. doi:10.1001/jamaoncol.2014.289.
Tateishi U, Morita S, Taguri M, Shizukuishi K, Minamimoto R, Kawaguchi M, et al. A meta-analysis of (18)F-fluoride positron emission tomography for assessment of metastatic bone tumor. Ann Nucl Med. 2010;24:523–31. doi:10.1007/s12149-010-0393-7.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
All authors declare that they have no conflicts of interest.
Ethical approval
Ethical approval is not applicable. This article does not contain any studies with human participants performed by any of the authors.
Rights and permissions
About this article
Cite this article
Etchebehere, E., Brito, A.E., Rezaee, A. et al. Therapy assessment of bone metastatic disease in the era of 223radium. Eur J Nucl Med Mol Imaging 44 (Suppl 1), 84–96 (2017). https://doi.org/10.1007/s00259-017-3734-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00259-017-3734-0