Abstract
Introduction and hypothesis
The beneficial effect of pelvic organ prolapse (POP) surgery on urge urinary incontinence (UI) is well described in the literature, while effect on preoperative stress UI (SUI) is still unclear. The aim of this study was to investigate changes concerning UUI following POP surgery without concomitant anti-incontinence procedures and to identify possible factors influencing the changes.
Methods
We conducted a retrospective study of 678 women with prolapse surgery using native tissue repair during a 3-year period. Patients completed three prolapse questions from the International Consultation on Incontinence–Vaginal Symptoms (ICIQ-VS) questionnaire and the International Consultation on Incontinence Questionnaire–Urinary Incontinence Short Form (ICIQ-UI SF) before undergoing surgery and 3 months postoperatively. Patients who scored >0 on the ICIQ-UI SF before surgery were included in the study.
Results
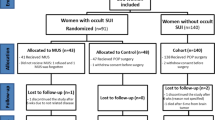
A total of 379 patients (55.9%) with POP had concomitant UI. At 3 months’ follow-up, 174 patients (46%) became continent compared with 205 patients (54%) with UI. Patients with remaining UI had statistically significant higher mean preoperative ICIQ-UI SF score than patients who became dry. The risk of remaining UI after POP surgery was greater in patients with previous anti-incontinence repair. UI type was not a risk factor for its persistance.
Conclusion
Almost half of the patients with UI before POP surgery became completely dry after prolapse surgery alone. Severity of incontinence and previous anti-incontinence surgery were identified as risk factors for persisting UI after POP surgery. We found a reduction of incontinence after an operation in any of the three compartments.




Similar content being viewed by others
References
Samuelsson EC, Victor FT, Tibblin G, Svärdsudd KF. Signs of genital prolapse in a Swedish population of women 20 to 59 years of age and possible related factors. Am J Obstet Gynecol. 1999;180(2 Pt 1):299–305.
Almousa S, Bandin van Loon A. The prevalence of urinary incontinence in nulliparous adolescent and middle-aged women and the associated risk factors: a systematic review. Maturitas. 2018;107:78–83.
Bump RC, Fantl JA, Hurt WG. The mechanism of urinary continence in women with severe uterovaginal prolapse: results of barrier studies. Obstet Gynecol. 1988;72(3 Pt 1):291–5.
Lensen EJ, Withagen MI, Kluivers KB, Milani AL, Vierhout ME. Urinary incontinence after surgery for pelvic organ prolapse. Neurourol Urodyn. 2013;32(5):455–9.
Bai SW, Jeon MJ, Kim JY, Chung KA, Kim SK, Park KH. Relationship between stress urinary incontinence and pelvic organ prolapse. Int Urogynecol J Pelvic Floor Dysfunct. 2002;13(4):256–60.
Ramanah R, Ballester M, Chereau E, Rouzier R, Daraï E. Effects of pelvic organ prolapse repair on urinary symptoms: a comparative study between the laparoscopic and vaginal approach. Neurourol Urodyn. 2012;31(1):126–31.
Digesu GA, Salvatore S, Chaliha C, et al. Do overactive bladder symptoms improve after repair of anterior vaginal wall prolapse? Int Urogynecol J Pelvic Floor Dysfunct. 2007;18:1439–43.
Fletcher SG, Haverkorn RM, Yan J, et al. Demographic and urodynamic factors associated with persistent OAB after anterior compartment prolapse repair. Neurourol Urodyn. 2010;29:1414–8.
Foster RTS, Barber MD, Parasio MF, et al. A prospective assessment of overactive bladder symptoms in a cohort of elderly women who underwent transvaginal surgery for advanced pelvic organ prolapse. Am J Obstet Gynecol. 2007;197(82):e1–4.
de Boer TA, Salvatore S, Cardozo L, et al. Pelvic organ prolapse and overactive badder. Neurourol Urodyn. 2010;29:30–9.
de Boer TA, Kluivers KB, Withagen MI, Milani AL, Vierhout ME. Predictive factors for overactive bladder symptoms after pelvic organ prolapse surgery. Int Urogynecol J. 2010;21(9):1143–9.
Nguyen JK, Bahatia NN. Resolution of motor urge incontinence after surgical repair of pelvic organ prolapse. J Urol. 2001;166:2263–6.
Miranne JM, Lopes V, Carberry CL, Sung VW. The effect of pelvic organ prolapse severity on improvement in overactive bladder symptoms after pelvic reconstructive surgery. Int Urogynecol J. 2013;24(8):1303–8.
Kim MS, Lee GH, Na ED, Jang JH, Kim HC. The association of pelvic organ prolapse severity and improvement in overactive bladder symptoms after surgery for pelvic organ prolapse. Obstet Gynecol Sci. 2016;59(3):214–9.
Costantini E, Lazzeri M, Zucchi A, Mearini L, Fragalà E, Del Zingaro M, et al. Urgency, detrusor overactivity and posterior vault prolapse in women who underwent pelvic organ prolapse repair. Urol Int. 2013;90(2):168–73.
Wei JT, Nygaard I, Richter HE, Nager CW, Barber MD, Kenton K, et al. Pelvic floor disorders network. A midurethral sling to reduce incontinence after vaginal prolapse repair. N Engl J Med. 2012;366(25):2358–67.
Brubaker L, Cundiff GW, Fine P, Nygaard I, Richter HE, Visco AG, et al. Pelvic floor disorders network. Abdominal sacrocolpopexy with Burch colposuspension to reduce urinary stress incontinence. N Engl J Med. 2006;354(15):1557–66.
Liapis A, Bakas P, Georgantopoulou C, Creatsas G. The use of the pessary test in preoperative assessment of women with severe genital prolapse. Eur J Obstet Gynecol Reprod Biol. 2011;155(1):110–3.
van der Ploeg JM, van der Steen A, Oude Rengerink K, van der Vaart CH, Roovers JP. Prolapse surgery with or without stress incontinence surgery for pelvic organ prolapse: a systematic review and meta-analysis of randomized trials. BJOG. 2014;121(5):537–47.
Baessler K, Maher C. Pelvic organ prolapse surgery and bladder function. Int Urogynecol J. 2013;24(11):1843–52.
Borstad E, Abdelnoor M, Staff AC, Kulseng-Hanssen S. Surgical strategies for women with pelvic organ prolapse and urinary stress incontinence. Int Urogynecol J. 2010;21(2):179–86.
Ennemoser S, Schönfeld M, von Bodungen V, Dian D, Friese K, Jundt K. Clinical relevance of occult stress urinary incontinence (OSUI) following vaginal prolapse surgery: long-term follow-up. Int Urogynecol J. 2012;23(7):851–855.
Jundt K, Wagner S, von Bodungen V, Friese K, Peschers UM. Occult incontinence in women with pelvic organ prolapse - does it matter? Eur J Med Res. 2010;15(3):112.
Guldberg R, Brostrøm S, Hansen JK, Kærlev L, Gradel KO, Nørgård BM, et al. The Danish Urogynecological database: establishment, completeness and validity. Int Urogynecol J. 2013;24:983–90.
Haylen BT, Maher CF, Barber MD, Camargo S, Dandolu V, Digesu A, et al. An international Urogynecological association (IUGA)/international continence society (ICS) joint report on the terminology for female pelvic organ prolapse (POP). Int Urogynecol J. 2016;27(4):655–84.
Price N, Jackson SR, Avery K, Brookes ST, Abrams P. Development and psychometric evaluation of the ICIQ vaginal symptoms questionnaire: the ICIQ-VS. BJOG. 2006;113(6):700–12.
Abrams P, Avery K, Gardener N, Donovan J. ICIQ advisory board. The international consultation on incontinence modular questionnaire: www.iciq.net. J Urol. 2006;175:1063–6.
Brading AF. A myogenic basis for the overactive bladder. Urology. 1997;50(6A Suppl):57–67. discussion 68-73
Ugianskiene A, Kjærgaard N, Inger Lindquist AS, Larsen T, Glavind K. Retrospective study on de novo postoperative urinary incontinence after pelvic organ prolapse surgery. Eur J Obstet Gynecol Reprod Biol. 2017;219:10–4.
King AB, Goldman HB. Stress incontinence surgery at the time of prolapse surgery: mandatory or forbidden? World J Urol. 2015;33:1257–62.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
None.
Rights and permissions
About this article
Cite this article
Ugianskiene, A., Kjærgaard, N., Larsen, T. et al. What happens to urinary incontinence after pelvic organ prolapse surgery?. Int Urogynecol J 30, 1147–1152 (2019). https://doi.org/10.1007/s00192-018-3677-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00192-018-3677-4