Abstract
Objective
Our objective was to quantitate the extent of complications and failure rate for apical prolapse repair with transvaginal mesh (TVM) use versus sacrocolpopexy over a minimum of 2 years of follow-up.
Methods
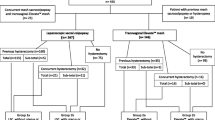
Truven CCAE and Medicare Supplemental databases 2008–2013 were used for analysis. Patients with apical prolapse repair via transvaginal mesh (TVMR), abdominal sacrocolpopexy (ASCP), laparoscopic sacrocolpopexy (LSCP), or native tissue repair (NTR) and continuously enrolled for years were in the study cohort. Surgical failures were identified by reoperation for any prolapse or subsequent use of pessary. SAS® 9.3 was used for analysis.
Results
Mesh removal/revision was reported highest in TVMR (5.1 %), followed by LSCP (1.7 %) and ASCP (1.2 %). In those with concomitant sling, combined rates for mesh/sling revision were high, at 9.0 % in TVMR + sling, 5.6 % in ASCP + sling, and 4.5 % LSCP + sling. Sling-alone cases reported a 3.5 % revision rate. Pelvic pain (16.4–22.7 %) and dyspareunia (5.6–7.5 %) were high in all three approaches for apical prolapse repairs. Reoperation for apical prolapse was more common for TVMR (2.9 %) compared with NTR (2.3 %) [odds ratio (OR) 1.27; confidence interval (CI) 1.1–1.47; p 0.002]. Both ASCP and LSCP were superior to NTR (ASCP 1.5 %, OR 0.63, CI 0.46–0.86; p 0.003) and LSCP 1.8 % (OR 0.79, CI 0.62-1.01; p 0.07). Overall prolapse recurrence, as indicated by any compartment surgery for prolapse and/or pessary use, was also noted highest in TVMR (5.9 % OR 1.23, CI 1.11–1.36; p <0.0001). Laparoscopic sacrocolpopexies were slightly superior at 4.0 % overall recurrence (OR 0.83, CI 0.7–0.98); p 0.03). Failure of incontinence surgery was higher when the initial procedure combined prolapse and sling surgery (1.97 %) versus sling alone (1.6 %).
Conclusions
Reoperation for apical prolapse is more common with TVMR than with sacrocolpopexies and NTR. Incontinence procedures are more likely to fail when performed along with prolapse repair than when performed alone. When mesh is used for repair, mesh revision is highest with TVMR and lowest with ASCP.
Similar content being viewed by others
References
Bjelic-Radisic V, Aigmueller T, Preyer O, Ralph G, Geiss I, Müller G, et al. Vaginal prolapse surgery with transvaginal mesh: results of the Austrian registry. Int Urogynecol J. 2014;25(8):1047-52. doi:10.1007/s00192-014-2333-x.
Kasyan G, Abramyan K, Popov AA, Gvozdev M, Pushkar D. Mesh-related and intraoperative complications of pelvic organ prolapse repair. Cent European J Urol. 2014;67(3):296-301. doi:10.5173/ceju.2014.03.art17.
Nguyen JN, Jakus-Waldman SM, Walter AJ, White T, Menefee SA. Perioperative complications and reoperations after incontinence and prolapse surgeries using prosthetic implants. Obstet Gynecol. 2012;119(3):539–46. doi:10.1097/AOG.0b013e3182479283.
Halaska M, Maxova K, Sottner O, Svabik K, Mlcoch M, Kolarik D, et al. A multicenter, randomized, prospective, controlled study comparing sacrospinous fixation and transvaginal mesh in treating posthysterectomy vaginal vault prolapse. Am J Obstet Gynecol. 2012;207(4):301. doi:10.1016/j.ajog.2012.08.016. e1–301.e7.
Barski D, Otto T, Gerullis H. Systematic review and classification of complications after anterior, posterior, apical, and total vaginal mesh implantation for prolapse repair. Surg Technol Int. 2014;24:217–24. PMID: 24700225.
Kokanali MK, Doğanay M, Aksakal O, Cavkaytar S, Topçu HO, Özer İ. Risk factors for mesh erosion after vaginal sling procedures for urinary incontinence. Eur J Obstet Gynecol Reprod Biol. 2014;177:146–50. doi:10.1016/j.ejogrb.2014.03.039.
Skala C, Renezeder K, Albrich S, Puhl A, Laterza RM, Naumann G, et al. The IUGA/ICS classification of complications of prosthesis and graft insertion: a comparative experience in incontinence and prolapse surgery. Int Urogynecol J. 2011;22(11):1429–35. doi:10.1007/s00192-011–1508-y.
Abbott S, Unger CA, Evans JM, Jallad K, Mishra K, Karram MM, et al. Evaluation and management of complications from synthetic mesh after pelvic reconstructive surgery: a multicenter study. Am J Obstet Gynecol. 2014;210(2):163. doi:10.1016/j.ajog.2013.10.012. e1–8.
Mettu JR, Colaco M, Badlani GH. Evidence-based outcomes for mesh-based surgery for pelvic organ prolapse. Curr Opin Urol. 2014;24(4):370–4. doi:10.1097/MOU.0000000000000063.
Diwadkar GB, Barber MD, Feiner B, Maher C, Jelovsek JE. Complication and reoperation rates after apical vaginal prolapse surgical repair: a systematic review. Obstet Gynecol. 2009;113:367–73.
Jeon MJ, Moon YJ, Jung HJ, Lim KJ, Yang HI, Kim SK, et al. A long-term treatment outcome of abdominal sacrocolpopexy. Yonsei Med J. 2009;50(6):807–13. doi:10.3349/ymj.2009.50.6.807.
Kirby AC, Nager CW. Indications, contraindications, and complications of mesh in the surgical treatment of urinary incontinence. Clin Obstet Gynecol. 2013;56(2):257–75. doi:10.1097/GRF.0b013e31828563d2.
https://www.gov.uk/government/publications/vaginal-mesh-implants-summary-of-benefits-and-risks
Clarhout F, Roovers JP, Lewi P, Verguts J, De Ridder D, Deprest J. Medium-term anatomic and functional results of laparoscopic sacrocolpopexy beyond the learning curve. Int Urogynecol J Pelvic Floor Dysfunct. 2009;20:1119–25.
Nieminen K, Hiltunen R, Takala T, et al. Outcomes after anterior vaginal wall repair with mesh: a randomized, controlled trial with 3 year follow-up. Am J Obstet Gynecol. 2010;203:235e1–e8.
Withagen MI, Milani AL, den Boon J, et al. Trocar-guided mesh compared with conventional vaginal repair in recurrent prolapse: a randomized controlled trial. Obstet Gynecol. 2011;117:242-50.
Altman D, Väyrynen T, Engh ME, et al. Anterior colporrhaphy versus transvaginal mesh for pelvic-organ prolapse. N Engl J Med. 2011;364:1826–36.
Vollebregt A, Fischer K, Gietelink D, et al. Primary surgical repair of anterior vaginal prolapse: a randomised trial comparing anatom-ical and functional outcomes between anterior colporrhaphy and trocar-guided transobturator anterior mesh. Br J Obstet Gynaecol. 2011;118:1518–27.
Carey H, Higgs P, Goh J, et al. Vaginal repair with mesh versus colporrhaphy for prolapse: a randomised controlled trial. Br J Obstet Gynaecol. 2009;116:1380–6.
Lopes ED, Lemos NL, Carramão Sda S, et al. Transvaginal poly-propylene mesh versus sacrospinous ligament fixation for the treat-ment of uterine prolapse: 1-year follow-up of a randomized con-trolled trial. Int Urogynecol J. 2010;21:389–94.
Iglesia CB, Sokol AI, Sokol ER, et al. Vaginal mesh for prolapse: a randomized controlled trial. Obstet Gynecol. 2010;116:293–303.
Maher CF, Feiner B, DeCuyper EM, et al. Laparoscopic sacral colpopexy versus total vaginal mesh for vaginal vault prolapse: a randomized trial. Am J Obstet Gynecol. 2011;204:3603e1–e7.
Hiltunen R, Nieminen K, Takala T, et al. Low-weight polypropyl-ene mesh for anterior vaginal wall prolapse: a randomized con-trolled trial. Obstet Gynecol. 2007;110:455–62.
Sivaslioglu SS, Unlubilgin E, Dolen I. A randomized comparison of polypropylene mesh surgery with site-specific surgery in treating cystocoele. Int Urogynecol J. 2008;19:467–71.
Nguyen JN, Burchette RJ. Outcome after anterior vaginal prolapse repair: a randomized controlled trial. Obstet Gynecol. 2008;111(4):891–8.
Tijdink MM, Vierhout ME, Heesakkers JP, Withagen MIJ. Surgical management of mesh-related complications after prior pelvic floor reconstructive surgery with mesh. Int Urogynecol J. 2011;22:1395–404. doi:10.1007/s00192-011-1476-2.
Barboglio PG, Toler AJ, Triaca V. Robotic sacrocolpopexy for the management of pelvic organ prolapse: a review of midterm surgical and quality of life outcomes. Female Pelvic Med Reconstr Surg. 2014;20(1):38–43. doi:10.1097/SPV.0000000000000047.
Long C-Y, Hsu C-S, Wu C-H, Liu C-M, Wang C-L, Tsai E-M. Three-year outcome of transvaginal mesh repair for the treatment of pelvic organ prolapse. Eur J Obstet Gynecol Reprod Biol. 2012;161(1):105–8. doi:10.1016/j.ejogrb.2011.12.007.
Keys T, Campeau L, Badlani G. Synthetic mesh in the surgical repair of pelvic organ prolapse: current status and future directions. Urology. 2012;80(2):237–43. doi:10.1016/j.urology.2012.04.008.
Landsheere L, Ismail S, Lucot J-P, Deken V, Foidart J-M, Cosson M. Surgical intervention after transvaginal Prolift mesh repair: retrospective single-center study including 524 patients with 3 years’ median follow-up. Am J Obstet Gynecol. 2012;206:83. doi:10.1016/j.ajog.2011.07.040. e1–83.e7.
Kongoasa N, Voralu K, Mokrzycki M. Does prior vaginal prolapse surgery affect synthetic mesh erosion rates? Obstet Gynecol. 2014;123(5):1S. doi:10.1097/01.AOG.0000447041.52027.a6.
Arsene E, Giraudet G, Lucot JP, Rubod C, Cosson M. Sacral colpopexy: long-term mesh complications requiring reoperation(s). Int Urogynecol J. 2014. doi:10.1007/s00192-014-2514-7.
Schierlitz L, Dwyer PL, Rosamilia A, De Souza A, Murray C, Thomas E, et al. Pelvic organ prolapse surgery with and without tension-free vaginal tape in women with occult or asymptomatic urodynamic stress incontinence: a randomised controlled trial. Int Urogynecol J. 2014;25(1):33–40. doi:10.1007/s00192-013-2150-7.
Ellington DR, Richter HE. The role of vaginal mesh procedures in pelvic organ prolapse surgery in view of complication risk. Obstet Gynecol Int. 2013:356960. doi: 10.1155/2013/356960.
Moore RD, Miklos JR. Vaginal mesh kits for pelvic organ prolapse, friend or foe: a comprehensive review. TheScientificWorldJOURNAL. 2009;9:163–89. doi:10.1100/tsw.2009.19.
Shah HN, Badlani GH. Mesh complications in female pelvic floor reconstructive surgery and their management: a systematic review. Indian J Urol. 2012;28(2):129–53. doi:10.4103/0970-1591.98453.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of Interest
Vani Dandolu, MD: Pfizer -Toviaz Advisory Board; Astellas -Independent Investigator Grant; Laborie -Speaker.
Megumi Akiyama, MD, Gayle Allenback, MSOT/L, MPH, GStat, Prathamesh Pathak, BPharm, MS: no conflicts.
Rights and permissions
About this article
Cite this article
Dandolu, V., Akiyama, M., Allenback, G. et al. Mesh complications and failure rates after transvaginal mesh repair compared with abdominal or laparoscopic sacrocolpopexy and to native tissue repair in treating apical prolapse. Int Urogynecol J 28, 215–222 (2017). https://doi.org/10.1007/s00192-016-3108-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00192-016-3108-3