Abstract
Introduction and hypothesis
Our aim was to compare anatomical and functional outcome between vaginal colposuspension and transvaginal mesh.
Methods
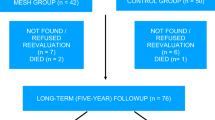
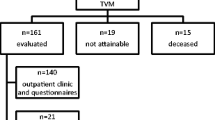
This was a prospective randomized controlled trial in a teaching hospital. Sixty-eight women with stage ≥3 anterior vaginal wall prolapse according to the Pelvic Organ Prolapse Quantification (POP-Q) system were assessed, randomized, and analyzed. Patients were randomized to anterior colporrhaphy with vaginal colposuspension (n = 35) or transvaginal mesh (n = 33). Primary outcome was objective cure rate of the anterior vaginal wall, defined as POP-Q ≤1 at 2 years. Secondary outcomes were functional results, quality-of-life (QoL) scores, mesh-related morbidity, and onset of urinary incontinence.
Results
The anatomical result for point Ba was significantly better at 2 years in the mesh group (−2.8 cm) than in the colposuspension group (−2.4 cm) (p = 0.02). Concerning POP-Q stages, the anatomical success rate at 2 years was 84.4 % for colposuspension and 100 % for mesh (p = 0.05). There were 5 anatomic recurrences (15.6 %) in the colposuspension group. The erosion rate was 6 % (n = 2). No significant difference was noted regarding minor complications. Analysis of QoL questionnaires showed overall improvement in both groups, with no significant difference between them.
Conclusions
The vaginal colposuspension technique of anterior vaginal wall prolapse repair gave good anatomical and functional results at 2 years. Transobturator vaginal mesh gave better 2-year anatomical results than vaginal colposuspension, with overall improvement in QoL in both groups.


Similar content being viewed by others
References
De Boer TA, Slieker-Ten Hove MC, Burger CW, Kluivers KB, Vierhout ME (2011) The prevalence and factors associated with previous surgery for pelvic organ prolapse and/or urinary incontinence in a cross-sectional study in The Netherlands. Eur J Obstet Gynecol Reprod Biol 158:343–349
Weber AM, Walters MD, Piedmonte MR, Ballard LA (2001) Anterior colporrhaphy: a randomized trial of three surgical techniques. Am J Obstet Gynecol 185:1299–1304
Fialkow MF, Newton KM, Weiss NS (2008) Incidence of recurrent pelvic organ prolapse 10 years following primary surgical management: a retrospective cohort study. Int Urogynecol J Pelvic Floor Dysfunct 19:1483–1487
Maher CM, Feiner B, Baessler K, Glazener CMA (2011) Surgical management of pelvic organ prolapse in women: the updated summary version Cochrane review. Int Urogynecol J 22:1445–1457
Jia X, Glazener C, Mowatt G, Jenkinson D, Fraser C, Bain C et al (2010) Systematic review of the efficacy and safety of using mesh in surgery for uterine or vaginal vault prolapse. Int Urogynecol J 21:1413–1431
Altman D, Väyrynen T, Engh ME, Axelsen S, Falconer C (2011) Anterior colporrhaphy versus transvaginal mesh for pelvic-organ prolapse. N Engl J Med 364(19):1826–1836
Stanford EJ, Cassidenti A, Moen MD (2012) Traditional native tissue versus mesh-augmented pelvic organ prolapse repairs: providing an accurate interpretation of current literature. Int Urogynecol J 23(1):19–28
Van Geelen JM, Dwyer PL (2013) Where to for pelvic organ prolapse treatment after the FDA pronouncements? A systematic review of the recent literature. Int Urogynecol J 24(5):707–718
FDA Safety Communication: Update on serious complications associated with transvaginal placement of surgical mesh for pelvic organ prolapse. Issued on 13 July 2011. http://www.fda.gov/medicaldevices/safety/alertsandNotices/ucm262435.htm. Accessed on 12 June 2012
De Tayrac R, Deval B, Fernandez H, Marès P (2007) Development of a linguistically validated French version of two short-form, condition-specific quality of life questionnaires for women with pelvic floor disorders (PFDI-20 and PFIQ-7). J Gynécol Obstét Biol Reprod 36(8):738–748
Dargent D, Mathevet P, Mellier G (2002) Traitement chirurgical des prolapsus génitaux par la voie vaginale. Encycl. Méd. Chir. (Paris France) 41–80, 18p
PERIGEE TM (2004) Instructions for Use. American Medical Systems Minnetonka, Minnesota
Richter K, Dargent D (1986) Spinous fixation (vaginae fixatio sacrospinalis) in the treatment of vaginal prolapse after hysterectomy. J Gynécol Obstét Biol Reprod 15(8):1081–1088
Nieminen K, Hiltunen R, Takala T, Heiskanen E, Merikari M, Niemi K, et al. (2010) Outcomes after anterior vaginal wall repair with mesh: a randomized, controlled trial with a 3 year follow-up. Am J Obstet Gynecol 203(3) 235: e1–8
Menefee SA, Dyer KY, Lukacz ES, Simsiman AJ, Luber KM, Nguyen JN (2011) Colporrhaphy compared with mesh or graft-reinforced vaginal paravaginal repair for anterior vaginal wall prolapse: a randomized controlled trial. Obstet Gynecol 118(6):1337–1344
Carey M, Higgs P, Goh J, Lim J, Leong A, Krause H et al (2009) Vaginal repair with mesh versus colporrhaphy for prolapse: a randomised controlled trial. BJOG 116(10):1380–1386
Rane A, Iyer J, Kannan K, Corstiaans A (2012) Prospective study of the PerigeeTM system for treatment of cystocele - our five-year experience. Aust N Z J Obstet Gynaecol 52(1):28–33
Moore RD, Beyer RD, Jacoby K, Freedman SJ, McCammon KA, Gambla MT (2010) Prospective multicenter trial assessing type I polypropylene mesh placed via transobturator route for the treatment of anterior vaginal prolapse with 2-year follow-up. Int Urogynecol J 21(5):545–552
Chu L-C, Chuang F-C, Kung F-T, Huang K-H (2012) Comparison of short-term outcomes following pelvic reconstruction with Perigee and Apogee systems: hysterectomy or not? Int Urogynecol J 23(1):79–84
Deffieux X, Letouzey V, Savary D, Sentilhes L, Agostini A, Mares P et al (2012) Prevention of complications related to the use of prosthetic meshes in prolapse surgery: guidelines for clinical practice. Eur J Obstet Gynecol Reprod Biol 165(2):170–180
Maher C, Feiner B, Baessler K, Schmid C (2013) Surgical management of pelvic organ prolapse in women. Cochrane Database Syst Rev 4:CD004014. doi:10.1002/14651858.pub5
Baessler K (2012) Do we need meshes in pelvic floor reconstruction? World J Urol 30(4):479–486
Delroy CA, de A Castro R, Dias MM, Feldner PC Jr, Bortolini MAT, Girão MJBC et al (2013) The use of transvaginal synthetic mesh for anterior vaginal wall prolapse repair: a randomized controlled trial. Int Urogynecol J 24(11):1899–1907
Nguyen JN, Jakus-Waldman SM, Walter AJ, White T, Menefee SA (2012) Perioperative complications and reoperations after incontinence and prolapse surgeries using prosthetic implants. Obstet Gynecol 119(3):539–546
Nguyen JN, Burchette RJ (2008) Outcome after anterior vaginal prolapse repair: a randomized controlled trial. Obstet Gynecol 111(4):891–898
Lee U, Wolff EM, Kobashi KC (2012) Native tissue repairs in anterior vaginal prolapse surgery: examining definitions of surgical success in the mesh era. Curr Opin Urol 22(4):265–270
Jacquetin B, Hinoul P, Gauld J, Fatton B, Rosenthal C, Clavé H (2013) Total transvaginal mesh (TVM) technique for treatment of pelvic organ prolapse: a 5-year prospective follow-up study. Int Urogynecol J 24(10):1679–1686
De Tayrac R, Cornille A, Eglin G, Guilbaud O, Mansoor A, Alonso S et al (2013) Comparison between trans-obturator trans-vaginal mesh and traditional anterior colporrhaphy in the treatment of anterior vaginal wall prolapse: results of a French RCT. Int Urogynecol J 24(10):1651–1661
Sivaslioglu AA, Unlubilgin E, Dolen I (2008) A randomized comparison of polypropylene mesh surgery with site-specific surgery in the treatment of cystocele. Int Urogynecol J Pelvic Floor Dysfunct 19(4):467–471
Vollebregt A, Fischer K, Gietelink D, van der Vaart CH (2011) Primary surgical repair of anterior vaginal prolapse: a randomised trial comparing anatomical and functional outcome between anterior colporrhaphy and trocar-guided transobturator anterior mesh. BJOG 118(12):1518–1527
Acknowledgments
This study was supported by Claude Bernard University for financing and Hospices Civils de Lyon, France, for study management.
Conflicts of interest
None.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Lamblin, G., Van-Nieuwenhuyse, A., Chabert, P. et al. A randomized controlled trial comparing anatomical and functional outcome between vaginal colposuspension and transvaginal mesh. Int Urogynecol J 25, 961–970 (2014). https://doi.org/10.1007/s00192-014-2344-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00192-014-2344-7