Abstract
Introduction and hypothesis
Despite the lack of evidence, antibiotic prophylaxis has been recommended for midurethral sling procedures. The goal of this study was to evaluate the rate of infectious complications in women undergoing midurethral sling procedures without antibiotic prophylaxis.
Methods
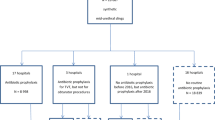
We reviewed the baseline characteristics and postoperative infectious complications of 174 consecutive women who underwent midurethral sling procedures without prophylactic antibiotics from April 2005 to January 2010. Patients undergoing concomitant vaginal surgery were excluded.
Results
The average age, parity, and body mass index of were 51.3 ± 12.6 years, 2.4 ± 1.3, and 30.1 ± 7.4 kg/m2, respectively. There were no wound infections, 2 (1.4%) vaginal mesh exposures and 12 (8%) cases of bacteriuria.
Conclusions
The risk of infections is low when a midurethral sling is performed without antibiotic prophylaxis. Antibiotic prophylaxis does not appear to offer any benefit in midurethral sling procedures.
Similar content being viewed by others
References
Wolf JS Jr, Bennett CJ, Dmochowski RR et al (2008) Urologic surgery antimicrobial prophylaxis best practice policy panel. Best practice policy statement on urologic surgery antimicrobial prophylaxis. J Urol 179:1379–1390
ACOG Committee on Practice Bulletins--Gynecology (2009) ACOG practice bulletin no. 104: antibiotic prophylaxis for gynecologic procedures. Obstet Gynecol 113:1180–1189
Richter HE, Albo ME, Zyczynski HM et al (2010) Retropubic versus transobturator midurethral slings for stress incontinence. N Engl J Med 362:2066–2076
Barber MD, Kleeman S, Karram MM et al (2008) Transobturator tape compared with tension-free vaginal tape for the treatment of stress urinary incontinence. Obstet Gynecol 111:611–621
Ross S, Robert M, Swaby C et al (2009) Transobturator tape compared with tension-free vaginal tape for stress incontinence. Obstet Gynecol 114:1287–1294
Houwert RM, Roovers JPWR, Venema PL et al (2010) Outcome and complications of retropubic and transobturator midurethral slings translated into surgical therapeutic indices. Am J Obstet Gynecol 202:75–77
Persson J, Iosif C, Wolner-Hanssen P (2002) Risk factors for rejection of synthetic suburethral slings for stress urinary incontinence: a case control study. Obstet Gynecol 99:629–634
Harmanli O, Boyer RL, Metz SA et al (2011) Double-blinded randomized trial of preoperative antibiotics in midurethral sling procedures and review of the literature. Int Urogynecol J 22:1249–1253
Ulmsten U, Henriksson L, Johnson P et al (1996) An ambulatory surgical procedure under local anesthesia for treatment of female urinary incontinence. Int Urogynecol J Pelvic Floor Dysfunct 7:81–86
Nygaard I, Brubaker L, Chai TC et al (2011) Risk factors for urinary tract infection following incontinence surgery. Int Urogynecol J 22:1255–1265
Ingber MS, Vasavada SP, Firoozi F et al (2010) Incidence of perioperative urinary tract infection after single-dose antibiotic therapy for midurethal slings. Urology 76:830–834
Swartz M, Ching C, Gill B, Li J et al (2010) Risk of infection after midurethral synthetic sling surgery: are postoperative antibiotics necessary? Urology 75:1305–1308
Conflict of interest
None.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Harmanli, O., Hong, EK., Rubin, R. et al. Is antibiotic prophylaxis necessary for midurethral sling procedures? A series of 174 cases without preoperative antibiotics. Int Urogynecol J 23, 621–623 (2012). https://doi.org/10.1007/s00192-011-1624-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00192-011-1624-8