Abstract
Introduction and hypothesis
Information on the prevalence, risk factors and social consequences of pelvic floor dysfunction (PFD) affecting women in 16 low-income and lower middle-income countries is reviewed.
Methods
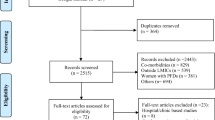
Medline searches were performed for articles dealing with prevalence of PFD.
Results
Thirty studies were identified. The mean prevalence for pelvic organ prolapse was 19.7% (range 3.4–56.4%), urinary incontinence (UI) was 28.7% (range 5.2–70.8%) and faecal incontinence (FI) was 6.9% (range 5.3–41.0%). Risk factors for PFD are similar to those in more affluent countries particularly increased age and parity, but additionally, PFD is associated with other factors including poor nutrition and heavy work. The social consequences of PFD conditions can be devastating.
Conclusions
Pelvic organ prolapse and urinary and faecal incontinence are significant problems in developing countries. Access to health care to manage these conditions is often limited, and women usually have to live with the consequences for the rest of their lives.

Similar content being viewed by others
Abbreviations
- PFD:
-
Pelvic floor dysfunction
- POP:
-
Pelvic organ prolapse
- UI:
-
Urinary incontinence
- FI:
-
Faecal incontinence
- OR:
-
Odds ratio
- CI:
-
Confidence interval
- I&E:
-
Interview and examination
- N:
-
Number
References
Ahmed S, Holtz SA (2007) Social and economic consequences of obstetric fistula: life changed for ever. Int J Gynaecol Obstet 99:S10–S15
Patel DA, Xu X, Thomason AD, Ransom SB, Ivy JS, De Lancey JOL (2006) Childbirth and pelvic floor dysfunction: an epidemiologic approach to the assessment of prevention opportunities at delivery. Am J Obstet Gynecol 195:23–28
Swift S, Woodman P, O'Boyle A, Kahn M, Valley M, Bland D et al (2005) Pelvic Organ Support Study (POSST): the distribution, clinical definition, and epidemiologic condition of pelvic organ support defects. Am J Obstet Gynecol 192:795–806
Subramanian D, Szwarcensztein K, Mauskopf JA, Slack MC (2009) Rate, type, and cost of pelvic organ prolapse surgery in Germany, France, and England. Eur J Obstet Gynecol Reprod Biol 144:177–181
Jelovsek JE, Moher C, Barber MD (2007) Pelvic organ prolapse. Lancet 369:1027–1038
Gunasekera P, Sazaki J, Walker G (2007) Pelvic organ prolapse: don't forget developing countries. Lancet 369:1789–1790
World Bank Country Classification, http://web.worldbank.org/WBSITE/EXTERNAL/DATASTATISTICS/0,,contentMDK:20420458~menuPK:64133156~pagePK:64133150~piPK:64133175~theSitePK:239419,00.html accessed 20 April 2010
Bonetti TR, Erpelding A, Pathak LR (2004) Listening to “felt needs”: investigating genital prolapse in Western Nepal. Reprod Health Matters 12:166–175
Ministry of Health and Population, Nepal, New Era and Macro International Inc. (2007) Nepal Demographic and Health Survey 2006. New Era and Macro International Inc., Kathmandu, Nepal: Ministry of Health and Population
Wusu-Ansah OK, Opare-Addo HS (2008) Pelvic organ prolapse in rural Ghana. Int J Gynaecol Obstet 103:121–124
Sajan F, Fikree FF (2002) Does early age at marriage influence gynaecological morbidities among Pakistani women? J Biosoc Sci 34:407–417
Younis N, Khattab H, Zurayk H, el-Mouelhy M, Amin MF, Farag AM (1993) A community study of gynaecological and related morbidities in rural Egypt. Stud Fam Plann 24:175–185
Bhatia JC, Cleland J, Bhagavan L, Rao NSN (1997) Levels and determinants of gynecological morbidity in a district of south India. Stud Fam Plann 28:95–103
Kumari S, Walia I, Singh A (2000) Self-reported prolapse in a resettlement colony of north India. J Midwifery Women's Health 45:343–350
Garshasbi A, Faghih-Zadeh S, Falah N (2006) The status of pelvic supporting organs in a population of Iranian women 18–68 years of age and possible related factors. Arch Iran Med 9:124–128
Adanu RM, De Lancey JO, Miller JM, Asante A (2006) The physical finding of stress urinary incontinence among African women in Ghana. Int Urogynecol J Pelvic Floor Dysfunct 17:581–585
Andrades M, Paul R, Ambreen A, Dodani S, Dhanani RH, Qidwai W (2004) Distribution of lower urinary tract symptoms (LUTS) in adult women. J Coll Physicians Surg Pak 14:132–135
Rizvi RM, Nazim MH (2005) The frequency of urinary symptoms in women attending gynaecology clinics at the Aga Khan University Hospital Karachi, Pakistan. J Pak Med Assoc 55:489–492
Song YF, Zhang WJ, Song J, Xu B (2005) Prevalence and risk factors of urinary incontinence in Fuzhou Chinese women. Chin Med J (Engl) 118:887–892
Zhang W, Song Y, He X, Xu B, Huang H, He C et al (2005) Prevalence and risk factors of lower urinary tract symptoms in Fuzhou Chinese women. Eur Urol 48:309–313
Zhu L, Lang J, Wang H, Han S, Huang J (2008) The prevalence of and potential risk factors for female urinary incontinence in Beijing, China. Menopause 15:566–569
Zhu L, Li L, Lang J, Xu T, Wong F (2010) Epidemiology of mixed urinary incontinence in China. Int J Gynecol Obstet 109:55–58
Zhu L, Lang J, Liu C, Han S, Huang J, Li X (2009) The epidemiological study of women with urinary incontinence and risk factors for stress incontinence in China. Menopause 15:566–569
Zhu L, Lang J, Liu C, Xu T, Liu X, Li L et al (2010) Epidemiological study of urge urinary incontinence and risk factors in China. Int Urogynecol J 21:589–593
El-Azab AS, Mohamed EM, Sabra HI (2007) The prevalence and risk factors of urinary incontinence and its influence on the quality of life among Egyptian women. Neurourol Urodyn 26:783–788
Sobhgol SS, Charandabee SM (2008) Related factors of urge, stress, mixed urinary incontinence and overactive bladder in reproductive age women in Tabriz, Iran: a cross-sectional study. Int Urogynecol J Pelvic Floor Dysfunct 19:367–373
Shakhatreh FM (2005) Epidemiology of urinary incontinence in Jordanian women. Saudi Med J 26:830–835
Shakhatreh FMH, Mas'ad D (2006) Menopausal symptoms and health problems of women aged 50–65 years in Southern Jordan. Climacteric 9:305–311
Mikou F, Abbassi O, Benjelloun A, Matar N, el Mansouri A (2001) Prevalence of urinary incontinence in Moroccan women. Report of 1, 000 cases. Ann Urol (Paris) 35:280–289
Sakondhavat C, Choosuwan C, Kaewrudee S, Soontrapa S, Louanka K (2007) Prevalence and risk factors of urinary incontinence in Khon Kaen menopausal women. J Med Assoc Thai 90:2553–2558
Manonai J, Poowapirom A, Kittipiboon S, Patrachai S, Udomsubpayakul U, Chittacharoen A (2006) Female urinary incontinence: a cross-sectional study from a Thai rural area. Int Urogynecol J Pelvic Floor Dysfunct 17:321–325
Manonai J, Chittacharoen A, Sarit-apirak S, Udomsubpayakul U, Khanacharoen A, Theppisai U (2004) Lower urinary tract symptoms in Thai women attending the menopause clinic: prevalence and associated factors. J Med Assoc Thai 87:1265–1269
Keskes J, Khairi H, Ben Said A, Hidar M, Pigné A (1988) Stress urinary incontinence in women. Epidemiologic inquiry. Apropos of 500 cases. J Gynecol Obstet Biol Reprod (Paris) 17:453–460
Scherf C, Morison L, Fiander A, Ekpo G, Walraven G (2002) Epidemiology of pelvic organ prolapse in rural Gambia, West Africa. BJOG 109:431–436
Sadeghi-Hassanabadi A, Keshavarz H, Setoudeh-Maram SZ (1998) Prevalence of reproductive morbidity among women of the Qashaq'I tribe, Islamic Republic of Iran. East Mediterr Health J 4:312–318
Al-Qutob R (2001) Menopause-associated problems: types and magnitude. A study in the Ain Al-Basha area, Jordan. J Adv Nurs 33:613–620
Mawajdeh SM, Al-Qutob R, Schmidt A (2003) Measuring reproductive morbidity: a community-based approach, Jordan. Health Care Women Int 24:635–649
National Statistics Office (NSO) [Philippines] and Macro International Inc. (MI) (1994) National Demographic Survey 1993. NSO and MI, Calverton, Maryland
Okonkwo JE, Obionu CO, Obiechina NJ (2001) Factors contributing to urinary incontinence and pelvic prolapse in Nigeria. Int J Gynaecol Obstet 74:301–303
Okonkwo JE, Obionu CN, Okonkwo CV, Obiechina NJ (2002) Anal incontinence among Igbo (Nigerian) women. Int J Clin Pract 56:178–180
Ozel B, Borchelt AM, Cimino FM, Cremer M (2007) Prevalence and risk factors for pelvic floor symptoms in women in rural El Salvador. Int Urogynecol J Pelvic Floor Dysfunct 18:1065–1069
Premachandra ND, Kotalawala SW, Cooray R, Samarasekera DN (2008) Anal incontinence in the aging Sri Lankan population: the results of a pilot study. Ceylon Med J 53:154
Bodner-Adler B, Shrivastava C, Bodner K (2007) Risk factors for uterine prolapse in Nepal. Int Urogynecol J Pelvic Floor Dysfunct 18:1343–1346
Ravindran TK, Savitri R, Bhavani A (1999) Women's experiences of utero-vaginal prolapse: a qualitative study from Tamil Nadu, India. In: Berer M, Sundari TK (eds) Safe motherhood initiatives: critical issues. Blackwell Science, Oxford, pp 166–172
Zhu L, Bian XM, Long Y, Lang JH (2008) Role of different childbirth strategies on pelvic organ prolapse and stress urinary incontinence: a prospective study. Chin Med J (Engl) 121:213–215
Lukman Y (1995) Utero-vaginal prolapse: a rural disability of the young. East Afr Med J 72:2–9
Komorowski L, Chen B (2006) Female urinary incontinence in China: experiences and perspectives. Health Care Women Int 27:169–181
Fernando RJ, Thakar R, Sultan AH, Shah SM, Jones PW (2006) Effect of vaginal pessaries on symptoms associated with pelvic organ prolapse. Obstet Gynecol 108:93–99
Cundiff GW, Weidner AC, Visco AG, Bump RC, Addison WA (2000) A survey of pessary use by members of the American Urogynecologic Society. Obstet Gynecol 95:931–935
Richardson K, Hagen S, Glazener C, Stark D (2009) The role of nurses in the management of women with pelvic organ prolapse. Br J Nurs 18:294–300
Schaaf JM, Dongol A, van der Leeuw-Harmsen (2008) Follow-up of prolapse surgery in rural Nepal. Int Urogynecol J Pelvic Floor Dysfunct 19:851–855
Bhatia MR, Yesudian CAK, Gorter A, Thankappan (2006) Demand side financing for reproductive and child health services in India. Econ Polit Wkly 41:279–284
Zurayk H, Khattab H, Younis N, Kamal O, El-Helw M (1995) Comparing women's reports with medical diagnoses of reproductive morbidity conditions in rural Egypt. Stud Fam Plann 26:14–21
Minassian VA, Drutz HP, Al-Badr A (2003) Urinary incontinence as a worldwide problem. Int J Gynaecol Obstet 82:327–338
Kenton K, Mueller ER (2006) The global burden of female pelvic floor disorders. BJU Int 98(Suppl 1):1–5
Haylen BT, de Ridder D, Freeman RM, Swift SE, Berghmans B, Lee J, Monga A, Petri E et al (2010) International Urogynecological Association; International Continence Society. An International Urogynecological Association (IUGA)/International Continence Society (ICS) joint report on the terminology for female pelvic floor dysfunction. Neurourol Urodyn 29:4–20
Treszezamsky AD, Rascoff L, Shahryarinejad A, Vardy MD (2010) Use of pelvic organ prolapse staging systems in published articles of selected specialized journals. Int Urogynecol J Pelvic Floor Dysfunct 21:359–363
Rizk DE (2009) Minimizing the risk of childbirth-induced pelvic floor dysfunctions in the developing word: “preventive” urogynecology. Int Urogynecol J Pelvic Floor Dysfunct 20:615–617
Conflicts of interest
None.
Author information
Authors and Affiliations
Corresponding author
Additional information
Disclaimer: The views expressed in this article are those of the authors and do not necessarily reflect the views of UNFPA or the United Nations.
Rights and permissions
About this article
Cite this article
Walker, G.J.A., Gunasekera, P. Pelvic organ prolapse and incontinence in developing countries: review of prevalence and risk factors. Int Urogynecol J 22, 127–135 (2011). https://doi.org/10.1007/s00192-010-1215-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00192-010-1215-0