Abstract
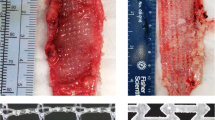
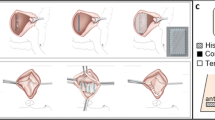
The aims of this study were dual. First, to evaluate the feasibility of a sheep model as an animal model for vaginal surgery with meshes. Second, to compare host response to two low-weight polypropylene (PP) meshes, a noncoated (Soft Prolene™, Gynecare, Ethicon) and a coated mesh with an absorbable hydrophilic film (Ugytex™, Sofradim). Thirty-six 20×20 mm polypropylene meshes (18 coated and 18 noncoated) were surgically implanted by the vaginal route in 12 adult ewes. Meshes were implanted in the anterior (n=12) and the posterior vaginal compartments (n=24). Animals were killed 1 (n=6) and 12 (n=6) weeks after surgery. Postimplantation evaluation included macroscopical examination, histological and immunohistochemical analysis and histomorphometrical measures of the distance between the meshes and the vaginal epithelium. The experimental procedure was feasible in all cases. Vaginal erosions were observed twice as frequently with the noncoated-PP meshes (6/18, 33.3%) as with the coated-PP meshes (3/18, 16.7%), even if that difference was not significant (p=0.4). However, no differences were observed between the two meshes in terms of shrinkage, tissue ingrowth, inflammatory response, and position of the mesh in the vaginal wall. The mechanism involved in the reduction of vaginal erosion could be due to the lesser adhesion of the coated mesh on the vaginal wound during the early postoperative period.





Similar content being viewed by others
References
MacLennan AH, Taylor AW, Wilson DH, Wilson D (2000) The prevalence of pelvic floor disorders and their relationship to gender, age, parity and mode of delivery. Br J Obstet Gynaecol 107:1460–1470
Olsen AL, Smith VJ, Bergstrom JO, Colling JC, Clark AL (1997) Epidemiology of surgically managed pelvic organ prolapse and urinary incontinence. Obstet Gynecol 89:501–506
Shull BL, Capen CV, Riggs MW, Kuehl TJ (1992) Preoperative and postoperative analysis of site-specific pelvic support defects in 81 women treated with sacrospinous ligament suspension and pelvic reconstruction. Am J Obstet Gynecol 166(6 Pt 1):1764–1768
Kohli N, Sze EHM, Roat TW, Karram MM (1996) Incidence of recurrent cystocele after anterior colporrhaphy with or without concomitant transvaginal needle suspension. Am J Obstet Gynecol 175:1476–1482
Benson J, Lucente V, McClellan E (1996) Vaginal versus abdominal reconstructive surgery for the treatment of pelvic support defects: a prospective randomized study with long-term outcome evaluation. Am J Obstet Gynecol 175:1418–1422
Bellon JM, Contreras LA, Bujan J, Palomares D, Carrera-San Martin A (1998) Tissue response to polypropylene meshes used in the repair of abdominal wall defects. Biomaterials 19:669–675
Desai VB (1987) Marlex mesh prosthesis for massive vaginal vault prolapse. Int Surg 72:160–162
Scales JT (1953) Materials for hernia repair. Proc R Soc Med 46:647–652
Cervigni M, Natale F (2001) The use of synthetics in the treatment of pelvic organ prolapse. Curr Opin Urol 11:429–435
Rackley RR, Abdelmalak JB, Tchetgen MB, Madjar S, Jones S, Noble M (2001) Tension-free vaginal tape and percutaneous vaginal tape sling procedures. Tech Urol 7:90–100
Aliabadi-Wahle S, Cnota M, Choe E, Jacob JT, Flint LM, Ferrara JJ (1998) Comparison of novel synthetic materials with traditional methods to repair exposed abdominal wall fascial defects. J Invest Surg 11:97–104
Klosterhalfen B, Klinge U, Henze U, Bhardwaj R, Conze J, Schumpelick V (1997) Morphologic correlation of functional abdominal wall mechanics after mesh implantation. Langenbecks Arch Chir 382:87–94
Amid PK (1997) Classification of biomaterials and their related complications in abdominal wall hernia surgery. Hernia 1:15–21
McGinty JJ, Hogle NJ, McCarthy H, Fowler DL (2005) A comparative study of adhesion formation and abdominal wall ingrowth after laparoscopic ventral hernia repair in a porcine model using multiple types of mesh. Surg Endosc 19(6):786–790
Boulanger L, Boukerrou M, Lambaudie E, Defossez A, Cosson M (2005) Tissue integration and tolerance to meshes used in gynecologic surgery: an experimental study. Eur J Obstet Gynecol Reprod Biol
Robinson TN, Clarke JH, Schoen J, Walsh MD (2005) Major mesh-related complications following hernia repair events reported to the Food and Drug Administration. Surg Endosc 19(12):1556–1560
Kayaoglu HA, Ozkan N, Hazinedaroglu SM, Ersoy OF, Erkek AB, Koseoglu RD (2005) Comparison of adhesive properties of five different prosthetic materials used in hernioplasty. J Invest Surg 18(2):89–95
Goldenberg A, Matone J, Marcondes W, Mardiros Herbella FA, de Matteos Farah JF (2005) Comparative study of inflammatory response and adhesions formation after fixation of different meshes for inguinal hernia repair in rabbits. Acta Cir Bras 20(5):
Konstantinovic ML, Lagae P, Zheng F, Verbeken EK, De Ridder D, Deprest JA (2005) Comparison of host response to polypropylene and non-cross-linked porcine small intestine serosal-derived collagen implants in a rat model. Br J Obstet Gynaecol 112:1554–1560
Klinge U, Junge K, Stumpf M, Öttinger AP, Klosterhalfen B (2002) Functional and morphological evaluation of a low-weight monofilament polypropylene mesh for hernia repair. J Biomed Mater Res Appl Biomater 63:129–136
Shmidbauer S, Ladurner R, Hallfeldt KK, Mussack T (2005) Heavy-weight versus low-weight polypropylene meshes for open sublay mesh repair of incisional hernia. Eur J Med Res 10(6):247–253
Acknowledgements
We wish to thank the technicians from Biomatech animal facility for their excellent technical assistance.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
de Tayrac, R., Alves, A. & Thérin, M. Collagen-coated vs noncoated low-weight polypropylene meshes in a sheep model for vaginal surgery. A pilot study. Int Urogynecol J 18, 513–520 (2007). https://doi.org/10.1007/s00192-006-0176-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00192-006-0176-9