Abstract
Purpose
Blood pressure (BP) monitoring is an essential procedure in intensive care. There is controversy about the reliability of non-invasive BP measurements in very preterm infants. This prospective trial compared non-invasive BP monitoring with BP monitoring via an umbilical arterial catheter (UAC) in this population.
Methods
Preterm infants born at less than 32 weeks gestation requiring a UAC for clinical management were eligible. Enrolled infants had up to three BP measurements on the right arm (RA) and right leg (RL) when in a resting state. UAC-BP measurements were noted immediately after the non-invasive BP was displayed on the monitor. Measurements were analysed in subgroups according to birth weight: no greater than 750 g, 751–1,000 g, above 1,000 g. Statistical analysis reports median, range, and Bland–Altman analysis.
Results
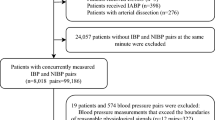
Sixty infants were included. Median (range) gestational age was 26.4 weeks (23.6, 31.2); birth weight 924 g (581, 1,518). A total of 1,865 measurements were performed (RA: 935, RL: 930). Mean difference (95% limits of agreement) for infants no greater than 750 g: RA 2.53 mmHg (−11.18, 16.24), RL −0.804 mmHg (−12.65, 11.04); for infants 751–1,000 g: RA 3.535 mmHg (−9.6, 16.7), RL −1.239 mmHg (–13.14, 10.66); for infants above 1,000 g: RA −1.65 mmHg (−13.47, 10.17), RL −4.101 mmHg (−14.17, 5.96).
Conclusions
Although the average differences between invasive and non-invasive BP measurements are acceptable, the range of under- and overestimation of non-invasive BP measurements is large and not consistent, making reliance on non-invasive modalities to guide circulatory management problematic. If arterial BP monitoring is not available, our results suggest measuring non-invasive BP on the leg in preterm infants with a birth weight no greater than 1,000 g.






Similar content being viewed by others
References
Kluckow M, Evans N (2000) Superior vena cava flow in newborn infants: a novel marker of systemic blood flow. Arch Dis Child Fetal Neonatal Ed 82:F182–F187
Kluckow M, Evans N (2000) Low superior vena cava flow and intraventricular haemorrhage in preterm infants. Arch Dis Child Fetal Neonatal Ed 82:F188–F194
Hunt RW, Evans N, Rieger I, Kluckow M (2004) Low superior vena cava flow and neurodevelopment at 3 years in very preterm infants. J Pediatr 145:588–592
Osborn DA, Evans N, Kluckow M (2004) Clinical detection of low upper body blood flow in very premature infants using blood pressure, capillary refill time, and central-peripheral temperature difference. Arch Dis Child Fetal Neonatal Ed 89:F168–F173
Kluckow M, Evans N (2001) Low systemic blood flow and hyperkalemia in preterm infants. J Pediatr 139:227–232
Miall-Allen VM, de Vries LS, Whitelaw AG (1987) Mean arterial blood pressure and neonatal cerebral lesions. Arch Dis Child 62:1068–1069
Watkins AM, West CR, Cooke RW (1989) Blood pressure and cerebral haemorrhage and ischaemia in very low birthweight infants. Early Hum Dev 19:103–110
Low JA, Froese AB, Galbraith RS, Smith JT, Sauerbrei EE, Derrick EJ (1993) The association between preterm newborn hypotension and hypoxemia and outcome during the first year. Acta Paediatr 82:433–437
Goldstein RF, Thompson RJ Jr, Oehler JM, Brazy JE (1995) Influence of acidosis, hypoxemia, and hypotension on neurodevelopmental outcome in very low birth weight infants. Pediatrics 95:238–243
Cunningham S, Symon AG, Elton RA, Zhu C, McIntosh N (1999) Intra-arterial blood pressure reference ranges, death and morbidity in very low birthweight infants during the first seven days of life. Early Hum Dev 56:151–165
Al-Aweel I, Pursley DM, Rubin LP, Shah B, Weisberger S, Richardson DK (2001) Variations in prevalence of hypotension, hypertension, and vasopressor use in NICUs. J Perinatol 21:272–278
Synnes AR, Chien LY, Peliowski A, Baboolal R, Lee SK (2001) Variations in intraventricular hemorrhage incidence rates among Canadian neonatal intensive care units. J Pediatr 138:525–531
Martens SE, Rijken M, Stoelhorst GM, van Zwieten PH, Zwinderman AH, Wit JM, Hadders-Algra M, Veen S (2003) Is hypotension a major risk factor for neurological morbidity at term age in very preterm infants? Early Hum Dev 75:79–89
Fanaroff JM, Wilson-Costello DE, Newman NS, Montpetite MM, Fanaroff AA (2006) Treated hypotension is associated with neonatal morbidity and hearing loss in extremely low birth weight infants. Pediatrics 117:1131–1135
Batton B, Zhu X, Fanaroff J, Kirchner HL, Berlin S, Wilson-Costello D, Walsh M (2009) Blood pressure, anti-hypotensive therapy, and neurodevelopment in extremely preterm infants. J Pediatr 154:351–357 357 e351
Dempsey EM, Barrington KJ (2007) Treating hypotension in the preterm infant: when and with what: a critical and systematic review. J Perinatol 27:469–478
Dempsey EM, Al Hazzani F, Barrington KJ (2009) Permissive hypotension in the extremely low birthweight infant with signs of good perfusion. Arch Dis Child Fetal Neonatal Ed 94:F241–F244
Logan JW, O’Shea TM, Allred EN, Laughon MM, Bose CL, Dammann O, Batton DG, Engelke SC, Leviton A (2011) Early postnatal hypotension and developmental delay at 24 months of age among extremely low gestational age newborns. Arch Dis Child Fetal Neonatal Ed 96:F321–F328
Hermansen MC, Hermansen MG (2005) Intravascular catheter complications in the neonatal intensive care unit. Clin Perinatol 32:141–156 vii
Diprose GK, Evans DH, Archer LN, Levene MI (1986) Dinamap fails to detect hypotension in very low birthweight infants. Arch Dis Child 61:771–773
Chia F, Ang AT, Wong TW, Tan KW, Fung KP, Lee J, Khin K (1990) Reliability of the Dinamap non-invasive monitor in the measurement of blood pressure of ill Asian newborns. Clin Pediatr (Phila) 29:262–267
Dannevig I, Dale HC, Liestol K, Lindemann R (2005) Blood pressure in the neonate: three non-invasive oscillometric pressure monitors compared with invasively measured blood pressure. Acta Paediatr 94:191–196
O’Shea J, Dempsey EM (2009) A comparison of blood pressure measurements in newborns. Am J Perinatol 26:113–116
Raab E, Seri I (2006) Diagnosis and treatment of the hypotensive very low birth weight infant during postnatal transition. J Perinatol 26:657–659
Dempsey EM, Barrington KJ (2009) Evaluation and treatment of hypotension in the preterm infant. Clin Perinatol 36:75–85
Meyer S, Sander J, Graber S, Gottschling S, Gortner L (2010) Agreement of invasive versus non-invasive blood pressure in preterm neonates is not dependent on birth weight or gestational age. J Paediatr Child Health 46:249–254
Papadopoulos G, Mieke S, Elisaf M (1999) Assessment of the performances of three oscillometric blood pressure monitors for neonates using a simulator. Blood Press Monit 4:27–33
Weindling AM (1989) Blood pressure monitoring in the newborn. Arch Dis Child 64:444–447
Kunk R, McCain GC (1996) Comparison of upper arm and calf oscillometric blood pressure measurement in preterm infants. J Perinatol 16:89–92
Acknowledgments
The study investigators would like to thank all the families for their cooperation and all NICU nurses for the excellent support in conducting this study.
Author information
Authors and Affiliations
Corresponding author
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
König, K., Casalaz, D.M., Burke, E.J. et al. Accuracy of non-invasive blood pressure monitoring in very preterm infants. Intensive Care Med 38, 670–676 (2012). https://doi.org/10.1007/s00134-012-2499-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00134-012-2499-y