Abstract.
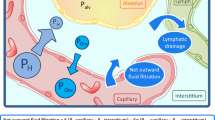
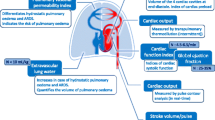
Objectives: The transpulmonary double indicator method uses intra- and extravascular indicators to calculate cardiac output, intrathoracic blood volume, global end-diastolic volume, and extravascular lung water content. Since lung perfusion may be of importance during these measurements, we studied the effects of pulmonary blood flow occlusion on measurements obtained with this method. Setting: Experimental animal facility of a University department. Methods and interventions: In seven pigs, the branch of the pulmonary artery perfusing the lower and middle lobe of the right lung was occluded. Measurements before, during, and after the occlusion were made with a pulmonary artery catheter and a commonly used transpulmonary double indicator catheter and device. Measurements and results: Occlusion of the right lower and middle lobe branch of the pulmonary artery increased mean pulmonary pressure (before occlusion: 24±1, during occlusion: 32±2, after reopening 25±1 mmHg; P<0.05), increased right ventricular end-diastolic volume (172±34, 209±21, 174±32 ml, respectively; P<0.05), decreased intrathoracic blood volume (998±39, 894±48, 1006±49 ml, respectively; P<0.05), and decreased extravascular lung water (7.2±0.5, 4.2±0.4, 6.9±0.4 ml/kg, respectively; P<0.05) without causing significant changes in cardiac output. All changes were reversible upon reopening the vessel. Conclusions: These data show that the transpulmonary double indicator method may underestimate extravascular lung water and right ventricular preload when the perfusion to parts of the lung is obstructed.
Similar content being viewed by others
Author information
Authors and Affiliations
Additional information
Final revision received: 17 August 2001
Electronic Publication
Rights and permissions
About this article
Cite this article
Schreiber, T., Hüter, L., Schwarzkopf, K. et al. Lung perfusion affects preload assessment and lung water calculation with the transpulmonary double indicator method. Intensive Care Med 27, 1814–1818 (2001). https://doi.org/10.1007/s00134-001-1122-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00134-001-1122-4