Abstract
Purpose
Epidemiological studies in the Netherlands have reported an excessive gender gap in the risk for non-affective psychotic disorder (NAPD) among immigrants from Morocco with a higher risk elevation in males compared to females. We examined the consistency of these findings and their generalizability to immigrants from the Maghreb (Mauritania, Morocco, Algeria, Tunisia and Libya) in other European countries.
Methods
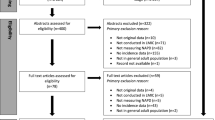
Systematic review and meta-analysis. Medline, PsychINFO and EMBASE databases were searched for publications in the period from January 1970 to April 2014. We included incidence and prevalence studies of non-affective psychotic disorder (NAPD) among migrants from the Maghreb in Europe and studies of subclinical psychotic symptoms (SPS) in representative samples. A meta-analysis was performed on the subgroup of incidence studies.
Results
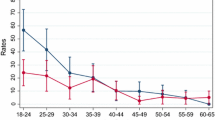
Five incidence and three prevalence studies of NAPD, and two prevalence studies of SPS, conducted in the Netherlands (n=7), Belgium (n=1), France (n=1) and Italy (n=1) met our inclusion criteria. Across all research designs, the risks of NAPD and SPS were consistently increased among male, not female immigrants from the Maghreb. The meta-analysis of incidence studies of NAPD yielded male-to-female risk ratios of 5.1 [95 % confidence interval (CI) 3.1–8.4] for migrants from the Maghreb, 2.0 (95 % CI 1.6–2.5) for other migrant groups, and 1.8 (95 % CI 1.3–2.5) for non-migrant Europeans.
Conclusions
The marked gender gap in psychosis risk among migrants from the Maghreb appears a consistent finding, foremost among the Moroccan-Dutch. The small number of studies limits the strength of conclusions that can be drawn about countries other than the Netherlands. Achievement–expectation mismatch, social marginalization and an increased prevalence of illicit drug use are possible explanations.

Similar content being viewed by others
References
Fearon P, Kirkbride JB, Morgan C, Dazzan P, Morgan K, Lloyd T, Hutchinson G, Tarrant J, Fung WL, Holloway J, Mallett R, Harrison G, Leff J, Jones PB, Murray RM (2006) Incidence of schizophrenia and other psychoses in ethnic minority groups: results from the MRC AESOP study. Psychol Med 36:1541–1550
Bourque F, van der Ven E, Malla A (2011) A meta-analysis of the risk for psychotic disorders among first- and second-generation immigrants. Psychol Med 41:897–910
Aleman A, Kahn RS, Selten JP (2003) Sex differences in the risk of schizophrenia: evidence from meta-analysis. Arch Gen Psychiatry 60:565–571
Cantor-Graae E, Selten JP (2005) Schizophrenia and migration: a meta-analysis and review. Am J Psychiatry 162:12–24
Selten JP, Laan W, Kupka R, Smeets HM, van Os J (2012) Risk of psychiatric treatment for mood disorders and psychotic disorders among migrants and Dutch nationals in Utrecht, The Netherlands. Soc Psychiatry Psychiatr Epidemiol 47:271–278
Selten JP, Sijben N (1994) First admission rates for schizophrenia in immigrants to The Netherlands. The Dutch National Register. Soc Psychiatry Psychiatr Epidemiol 29:71–77
Veling W, Selten JP, Veen N, Laan W, Blom JD, Hoek HW (2006) Incidence of schizophrenia among ethnic minorities in the Netherlands: a four-year first-contact study. Schizophr Res 86:189–193
Coid JW, Kirkbride JB, Barker D, Cowden F, Stamps R, Yang M, Jones PB (2008) Raised incidence rates of all psychoses among migrant groups: findings from the East London first episode psychosis study. Arch Gen Psychiatry 65:1250–1258
Veling W, Hoek HW, Selten JP, Susser E (2011) Age at migration and future risk of psychotic disorders among immigrants in the Netherlands: a 7-year incidence study. Am J Psychiatry 168:1278–1285
Zandi T, Havenaar JM, Smits M, Limburg-Okken AG, van Es H, Cahn W, Algra A, Kahn RS, van den Brink W (2010) First contact incidence of psychotic disorders among native Dutch and Moroccan immigrants in the Netherlands: influence of diagnostic bias. Schizophr Res 119:27–33
Borenstein M (2010) Meta-analysis: computing treatment effects and effect sizes. Wiley, Chichester
Higgins JP, Thompson SG, Deeks JJ, Altman DG (2003) Measuring inconsistency in meta-analyses. BMJ 327:557–560
Adriaanse M, van Domburgh L, Hoek HW, Susser E, Doreleijers TA, Veling W (2015) Prevalence, impact and cultural context of psychotic experiences among ethnic minority youth. Psychol Med 45:637–646
van der Stelt O, Boubakri D, Feltzer M (2013) Migration status, familial risk for mental disorder, and schizotypal personality traits. Eur J Psychol 9:552–571
Vinkers DJ, Selten JP, Hoek HW, Rinne T (2013) Psychotic disorders are more common in ethnic minority than in Dutch native defendants. Soc Psychiatry Psychiatr Epidemiol 48:1399–1404
van der Post L, Visch I, Mulder C, Schoevers R, Dekker J, Beekman A (2012) Factors associated with higher risks of emergency compulsory admission for immigrants: a report from the ASAP study. Int J Soc Psychiatry 58:374–380
de Wit MA, Tuinebreijer WC, van Brussel GH, Selten JP (2012) Ethnic differences in risk of acute compulsory admission in Amsterdam, 1996–2005. Soc Psychiatry Psychiatr Epidemiol 47:111–118
Mulder CL, Koopmans GT, Selten JP (2006) Emergency psychiatry, compulsory admissions and clinical presentation among immigrants to the Netherlands. Br J Psychiatry 188:386–391
Tarricone I, Mimmi S, Paparelli A, Rossi E, Mori E, Panigada S, Carchia G, Bandieri V, Michetti R, Minenna G, Boydell J, Morgan C, Berardi D (2012) First-episode psychosis at the West Bologna Community Mental Health Centre: results of an 8-year prospective study. Psychol Med 42:2255–2264
Tortelli A, Morgan C, Szoke A, Nascimento A, Skurnik N, de Caussade EM, Fain-Donabedian E, Fridja F, Henry M, Ezembe F, Murray RM (2014) Different rates of first admissions for psychosis in migrant groups in Paris. Soc Psychiatry Psychiatr Epidemiol 49:1103–1109
Schrier AC, van de Wetering BJ, Mulder PG, Selten JP (2001) Point prevalence of schizophrenia in immigrant groups in Rotterdam: data from outpatient facilities. Eur Psychiatry 16:162–166
Fossion P, Ledoux Y, Valente F, Servais L, Staner L, Pelc I, Minner P (2002) Psychiatric disorders and social characteristics among second-generation Moroccan migrants in Belgium: an age-and gender-controlled study conducted in a psychiatric emergency department. Eur Psychiatry 17:443–450
Vanheusden K, Mulder CL, van der Ende J, Selten JP, van Lenthe FJ, Verhulst FC, Mackenbach JP (2008) Associations between ethnicity and self-reported hallucinations in a population sample of young adults in The Netherlands. Psychol Med 38:1095–1102
Kelleher I, Cannon M (2011) Psychotic-like experiences in the general population: characterizing a high-risk group for psychosis. Psychol Med 41:1–6
Gerritsen AA, Deville WL (2009) Gender differences in health and health care utilisation in various ethnic groups in the Netherlands: a cross-sectional study. BMC Public Health 9:109
Selten JP, Blom JD, van der Tweel I, Veling W, Leliefeld B, Hoek HW (2008) Psychosis risk for parents and siblings of Dutch and Moroccan-Dutch patients with non-affective psychotic disorder. Schizophr Res 104:274–278
Poulton R, Caspi A, Moffitt TE, Cannon M, Murray R, Harrington H (2000) Children’s self-reported psychotic symptoms and adult schizophreniform disorder: a 15-year longitudinal study. Arch Gen Psychiatry 57:1053–1058
Moussaoui D, Rim S (2011) Epidemiology of schizophrenia and related disorders in the Arab World. Arab J Psychiatry 22:1–9
Nuevo R, Chatterji S, Verdes E, Naidoo N, Arango C, Ayuso-Mateos JL (2012) The continuum of psychotic symptoms in the general population: a cross-national study. Schizophr Bull 38:475–485
Selten JP, Wierdsma A, Mulder N, Burger H (2007) Treatment seeking for alcohol and drug use disorders by immigrants to the Netherlands: retrospective, population-based, cohort study. Soc Psychiatry Psychiatr Epidemiol 42:301–306
Spruit IP (2002) Cannabis 2002 Report. Ministry of Public Health, Brussels, Belgium, pp. 1–142
van Laar MW, Cruts AAN, van Ooyen-Houben MMJ, Meijer RF, Croes EA, Brunt T, Ketelaars APM (2011) NDM annual report 2010, Netherlands national drug monitor. Trimbos Instituut, Utrecht, pp 1–275
Veling W, Mackenbach JP, van Os J, Hoek HW (2008) Cannabis use and genetic predisposition for schizophrenia: a case-control study. Psychol Med 38:1251–1256
Veen N, Selten JP, Hoek HW, Feller W, van der Graaf Y, Kahn R (2002) Use of illicit substances in a psychosis incidence cohort: a comparison among different ethnic groups in the Netherlands. Acta Psychiatr Scand 105:440–443
Lahlah E, van der Knaap LM, Bogaerts S (2013) Dangerous boys or boys in danger? Examining the relationship between ethnicity, child abuse and violent offending. Eur J Criminol 10:641–658
Veling W, Susser E (2011) Migration and psychotic disorders. Expert Rev Neurother 11:65–76
Veling W, Hoek HW, Wiersma D, Mackenbach JP (2010) Ethnic identity and the risk of schizophrenia in ethnic minorities: a case-control study. Schizophr Bull 36:1149–1156
Stevens GWJM, Vollebergh WAM, Pels TVM, Crijnen AAM (2007) Problem behavior and acculturation in Moroccan immigrant adolescents in the Netherlands: effects of gender and parent-child conflict. J Cross Cult Psychol 38:310–317
UNESCO (2010) United Nations educational, scientific, and cultural organization. Institute for Statistics, Statistical tables
Gijsberts M, Huijnk W, Dagevos J (2012) Annual Integration Report 2011. The Netherlands Institute for Social Research, pp. 102–227
Crul M, Doomernik J (2003) The Turkish and Moroccan second generation in the Netherlands: divergent trends between and polarization within the two groups1. Int Migr Rev 37:1039–1064
Kleiner RJ, Parker S (1963) Goal-striving, social status, and mental disorder: a research review. Am Sociol Rev 28:189–203
Reininghaus UA, Morgan C, Simpson J, Dazzan P, Morgan K, Doody GA, Bhugra D, Leff J, Jones P, Murray R, Fearon P, Craig TK (2008) Unemployment, social isolation, achievement-expectation mismatch and psychosis: findings from the AESOP Study. Soc Psychiatry Psychiatr Epidemiol 43:743–751
Blokland A, Grimbergen K, Bernasco W, Nieuwbeerta P (2010) Criminaliteit en etniciteit. Tijdschrift voor Criminologie 2:122–152
de Jong J (2012) Typically Moroccan? A group dynamic explanation of nuisance and criminal behavior. In: Esbensen FA, Maxson CL (eds) Youth gangs in international perspective. Springer, New York, pp 225–236
Pels T (2003) The question of respect: socialisation and misconduct of Moroccan boys in the Netherlands. Neth J Soc Sci 39:126–141
Huijnk W, Dagevos J (2012) Closer together? The socio-cultural position of non-Western migrants in the Netherlands. The Netherlands Institute for Social Research, pp. 128–144
Ouarasse OA, van de Vijver FJR (2005) The role of demographic variables and acculturation attitudes in predicting sociocultural and psychological adaptation in Moroccans in the Netherlands. Int J Intercult Relat 29:251–272
Engbersen G, van der Leun J, de Boom J (2007) The fragmentation of migration and crime in the Netherlands. Crime Justice 35:389–452
Selten JP, van der Ven E, Rutten BP, Cantor-Graae E (2013) The social defeat hypothesis of schizophrenia: an update. Schizophr Bull 39:1180–1186
Selten JP, Cantor-Graae E (2005) Social defeat: risk factor for schizophrenia? Br J Psychiatry 187:101–102
Gevonden M, Booij J, van den Brink W, Heijtel D, Van Os J, Selten JP (2014) Increased release of dopamine in the striata of young adults with hearing impairment and its relevance for the social defeat hypothesis of schizophrenia. JAMA Psychiatry 71:1364–1372
Di Forti M, Morgan C, Dazzan P, Pariante C, Mondelli V, Marques TR, Handley R, Luzi S, Russo M, Paparelli A, Butt A, Stilo SA, Wiffen B, Powell J, Murray RM (2009) High-potency cannabis and the risk of psychosis. Br J Psychiatry 195:488–491
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
van der Ven, E., Veling, W., Tortelli, A. et al. Evidence of an excessive gender gap in the risk of psychotic disorder among North African immigrants in Europe: a systematic review and meta-analysis. Soc Psychiatry Psychiatr Epidemiol 51, 1603–1613 (2016). https://doi.org/10.1007/s00127-016-1261-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00127-016-1261-0