Abstract
Aims/hypothesis
The imbalance between maternal insulin resistance and a relative lack of insulin secretion underlies the pathogenesis of gestational diabetes mellitus (GDM). Alterations in T cell subtypes and increased levels of circulating proinflammatory cytokines have been proposed as potential mechanisms underlying the pathophysiology of insulin resistance in GDM. Since oestrogen modulates T cell immunity, we hypothesised that oestrogen plays a homeostatic role in visceral adipose tissue by coordinating T cell immunity through oestrogen receptor α (ERα) in T cells to prevent GDM.
Methods
Female CD4-cre ERαfl/fl (KO) mice on a C57BL/6 background with ERα ablation specifically in T cells, and ERαfl/fl (ERα-floxed [FL]) mice were fed 60 kJ% high-fat diet (HFD) for 4 weeks. Female mice mated with male BALB/c mice to achieve allogenic pregnancy and were maintained on an HFD to generate the GDM model. Mice were divided into four experimental groups: non-pregnant FL, non-pregnant KO, pregnant FL (FL-GDM) and pregnant KO (KO-GDM). GTTs and ITTs were performed on day 12.5 or 13.5 and 16.5 after breeding, respectively. On day 18.5 after breeding, mice were killed and T cell subsets in the gonadal white adipose tissue (gWAT) and spleen were analysed using flow cytometry. Histological examination was also conducted and proinflammatory gene expression in gWAT and the liver was evaluated.
Results
KO mice that mated with BALB/c mice showed normal fertility rates and fetal weights as compared with FL mice. Body and tissue weights were similar between FL and KO mice. When compared with FL-GDM mice, KO-GDM mice showed decreased insulin secretion (serum insulin concentration 15 min after glucose loading: 137.3 ± 18.3 pmol/l and 40.1 ± 36.5 pmol/l, respectively; p < 0.05), impaired glucose tolerance (glucose AUC in GTT: 2308.3 ± 54.0 mmol/l × min and 2620.9 ± 122.1 mmol/l × min, respectively; p < 0.05) and increased numbers of T helper (Th)17 cells in gWAT (0.4 ± 0.0% vs 0.8 ± 0.1%; p < 0.05). However, the contents of Th1 and regulatory T cells (Tregs) in gWAT remained similar between FL-GDM and KO-GDM. Glucose-stimulated insulin secretion was similar between isolated islets derived from FL and KO mice, but was reduced by IL-17A treatment. Moreover, the levels of proinflammatory gene expression, including expression of Emr1 and Tnfa in gWAT, were significantly higher in KO-GDM mice than in FL-GDM mice (5.1-fold and 2.7-fold, respectively; p < 0.01 for both). Furthermore, KO-GDM mice showed increased expression of genes encoding hepatokines, Ahsg and Fgf21 (both were 2.4-fold higher vs FL-GDM mice; p < 0.05 and p = 0.09, respectively), with no changes in inflammatory gene expression (e.g., Tnfa and Ifng) in the liver compared with FL-GDM mice.
Conclusions/interpretation
Deletion of ERα in T cells caused impaired maternal adaptation of insulin secretion, changes in hepatokine profiles, and enhanced chronic inflammation in gWAT alongside an abnormal increase in Th17 cells. These results suggest that the ERα-mediated oestrogen signalling effects in T cells regulate T cell immunity and contribute to glucose homeostasis in pregnancy.
Graphical abstract

Similar content being viewed by others

Introduction
Gestational diabetes mellitus (GDM) is defined as glucose intolerance with an onset or first recognition during pregnancy and its presence indicates an increased risk of future diabetes in the mother [1]. According to the International Diabetes Federation (IDF) in 2017, approximately 14% of pregnant women worldwide are estimated to have GDM [2] and its incidence increases with elevated maternal age [3]. The imbalance between maternal insulin resistance and the relative lack of insulin secretion due to beta cell dysfunction is regarded as the central pathophysiology of GDM; however, the underlying mechanisms remain unclear [4, 5].
Maternal insulin resistance is an important mechanism that promotes the partitioning of nutrients to the fetus [4] and is affected by maternal metabolic conditions, such as obesity and chronic inflammation in adipose tissue [4]. Circulating levels of proinflammatory cytokines have been shown to increase in GDM [5, 6]. Furthermore, alterations in immune cells in peripheral blood, such as increased numbers of proinflammatory T helper (Th)17 cells, and decreased numbers of regulatory T cells (Treg) or a reduction in their immunosuppressive activities, have been reported [7, 8], and these changes may contribute to the progression of insulin resistance in GDM. However, the underlying mechanisms for these immunological changes in GDM remain unknown. Moreover, model mice that reflect immune changes in human GDM have not yet been developed.
Oestrogen increases during pregnancy and plays important roles in reproductive function, including the maintenance of pregnancy [9]. A cardinal effect of oestrogen is the regulation of reproductive immunity by controlling immune tolerance during pregnancy, mainly by differentiating naive T cells into Tregs and accumulating them around the uterus [10]. Oestrogen also modulates the differentiation of inflammatory Th1 and Th17 cells [11, 12], suggesting that it possesses a wide range of immunoregulatory functions. Regarding receptor expression, CD4+ T cells express higher levels of oestrogen receptor α (ERα) than oestrogen receptor β (ERβ), whereas very low, but similar levels of both oestrogen receptors are expressed in CD8+ T cells [13]. Therefore, most of the immunoregulatory effects of oestrogens in T cells are suggested to be mediated via ERα [14]. Serum concentrations of oestrogen are indistinguishable between women with GDM and healthy pregnant women [15]. However, it currently remains unclear whether insufficient effects of oestrogen in T cells are related to the immune disturbance observed in GDM.
Physiological levels of oestrogen enhance insulin sensitivity in various tissues, including adipose tissue, skeletal muscles and the liver, through ERα [16, 17]. Oestrogen contributes to the adaptation of beta cell mass and function to counteract maternal insulin resistance during pregnancy [18]. To examine the effects of oestrogen in T cells during pregnancy, we generated a GDM model using T cell-specific ERα-deleted mice. We investigated glucose metabolism and immune abnormalities during pregnancy in these mice and clarified the impact of T cell-specific ERα deletion on chronic inflammation in visceral adipose tissue in order to shed light on the pathophysiology of GDM.
Methods
Animals and experimental protocols
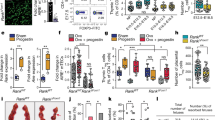
All experimental procedures used in the present study were approved by the Committee of Animal Experiments at the University of Toyama, Toyama, Japan (approval number for animal experiments: A2013PHA15 and A2017PHA-16; approval number for recombinant DNA experiments: G2013PHA-7 and G2018PHA-2). The experiments were conducted with careful consideration of mice welfare. ERα-floxed (ERαfl/fl [FL]) mice were provided by P. Chambon at the Institut de Génétique et de Biologie Moléculaire et cellulaire (IGBMC; Illkirch-Graffenstaden, France) [19]. ERα-floxed mice on a C57BL/6 background were crossed with CD4-cre mice (STOCK Tg(Cd4-cre)1Cwi/BfluJ; Jackson Laboratory, USA; www.jax.org/strain/17336) to generate CD4-cre ERαfl/fl (KO) mice with ablated ERα specifically in T cells. Female KO mice and their littermate controls (FL mice) were fed PicoLab Rodent Diet 20 (chow 14.4 kJ/g; PMI Nutrition International, USA) until they were 8 weeks old, after which they were fed a 60 kJ% high-fat diet (HFD; 21.9 kJ/g; D12492; Research Diets, USA) for 4 weeks. Following this, breeding was conducted overnight between female KO or FL mice and male BALB/c mice in a 1:1 ratio to achieve allogenic pregnancy. Mating was confirmed the following morning (day 0.5 after breeding) by the presence of a vaginal mucous plug. Mice were divided into four experimental groups, non-pregnant FL, non-pregnant KO, pregnant FL (FL-GDM) and pregnant KO (KO-GDM), and were maintained on an HFD. The 2 h GTT (0–120 min) was conducted on day 13.5 after breeding by an intraperitoneal injection of glucose (11.1 mmol [2 g]/kg body weight) after 6 h of fasting, and the ITT was performed on day 16.5 after breeding by an intraperitoneal injection of insulin (0.75 U/kg body weight) after 4 h of fasting, as described previously [20, 21]. In addition, on day 12.5 after breeding, another individual mouse was used for a 0–15 min GTT to evaluate insulin secretion. Mice were killed on day 18.5 after breeding. An outline of the experimental protocol is shown in Fig. 1a. Serum insulin levels during GTT and oestradiol levels at the time of death were measured using ELISA kits (Morinaga, Japan and Cayman, USA, respectively). The fertility rate was calculated from the numbers of pregnant mice per vaginal mucous plug-positive mice after breeding. Mice were maintained in the animal laboratory at the University of Toyama. Mice were housed on a 12:12 h light–dark cycle (lights on at 7:00 hours) in a temperature-controlled colony room (23 ± 3°C) and were allowed free access to food and water. Mice with premature delivery (n = 1) and growth failure due to abnormal tooth formation (n = 2) were excluded from data analysis. All other mice represented normal growth and pregnancy. Besides this, animals were excluded from analysis if we noted an inadequate injection of glucose or insulin. All measurements were taken from distinct samples. Randomisation were not conducted; blinding of samples was carried out in histological analysis, serum measurements and real-time PCR. The deviation in sample numbers among mice groups in each experiment was derived from the fact that more KO mice were prepared for experiments than FL mice because of our initial concerns about possible miscarriage and lower mating rate in KO mice.
Experimental protocol for GDM mouse models and the efficiency of ERα knockout in different types of leucocytes. (a) Female CD4-cre ERαfl/fl (KO) mice and ERαfl/fl (FL) mice on a C57BL/6 J background, aged 8–9 weeks, were fed a 60 kJ% high-fat diet (HFD) for 4 weeks and then mated with male BALB/c mice. Mice were killed and analysed on day 18.5 after mating. (b–f) Relative mRNA expression of Esr1 (gene encoding ERα) in CD4+ T cells (b; n = 6–9), CD8+ T cells (c; n = 6–9; FL vs KO, p = 0.09), macrophages (d; n = 8–11), B cells (e; n = 4–5) and NK cells (f; n = 6–8) isolated from the spleens of unmated female FL and KO mice. Cell gating in flow cytometry for each cell type is shown in ESM Fig. 1. Data are shown as means ± SEM. **p < 0.01; unpaired Student’s t test
Flow cytometry
Cells of the stromal-vascular fraction (SVF) of gonadal white adipose tissue (gWAT), splenocytes, thymus and uterus were prepared using the collagenase digestion method, and then incubated with purified rat anti-mouse CD16/CD32 (BD Biosciences, San Jose, CA, USA) for 15 min. Cells were then stained with an anti-CD45 antibody, antibodies corresponding to immune cell type and isotype controls at 4°C for 30 min. Subsequently, cells were rinsed and incubated with 7-amino-actinomycin D (7AAD; BD Biosciences) and then subjected to flow cytometry analysis, as described previously [22,23,24,25]. SVF cells obtained from two mice in the same group were analysed as one sample when the amounts from one mouse were not enough. For the analysis of Emr1 expression in various leucocytes, CD4+, CD8+, F4/80+, CD3-B220/CD45R+ or CD3-NK1.1+ cells gated on CD45+7AAD− cells were isolated from the spleen of unmated female FL and KO mice using the FACSAria II cell sorting system (BD Biosciences); their gating is shown in electronic supplementary material (ESM) Fig. 1. In the analysis of Tregs in splenocytes, thymus and uterus, cells were stained with anti-mouse CD45–APC, CD4–FITC, CD8–APC-cyanine7 (Cy7) and CD25–phycoerythrin (PE) at 4°C for 30 min, incubated with 7-amino-actinomycin D (7-AAD; BD Biosciences, Japan) for 15 min, fixed and permeabilised at 4°C overnight using the Foxp3/Transcription Factor Staining Buffer Set (eBioscience, USA) and then stained with forkhead box P 3 (FOXP3)–PE–Cy7 for 30 min. In the analysis of Tregs in gWAT, SVF cells were stained with LIVE-DEAD–APC–Cy7 and with CD45–PE–Cy7, CD4–Brilliant Violet 421 (BV421), CD25–APC and FOXP3–PE using the same protocol described above. In the analysis of Th1 and Th17, splenocytes and SVF cells were stimulated with phorbol 12-myristate 13-acetate (PMA), ionomycin and Brefeldin A Solution (protein transport inhibitor) for 4 h. Cells were then stained with LIVE-DEAD–APC–Cy7, CD45–PE–Cy7, CD4–BV421, IFNγ–APC, and IL-17A–PE. Stained cells were analysed by FACSCanto II or FACSAria II (BD Biosciences). Data were analysed by FACS Diva 6.1.2 (BD Bioscience) and Flow Jo (Treestar, Ashland, OR, USA). Antibodies used in the present study are listed in the ESM Table 1.
RNA isolation and real-time PCR
Total RNA in gWAT, liver and sorted leucocytes was purified using TRIsure (Nippon Genetics, Tokyo, Japan) or TRIzol (Thermo Fisher, Tokyo, Japan). Real-time PCR was performed using SYBR green (Takara Bio, Japan), as described previously [21, 24, 25]. The relative expression of target mRNAs was calculated as a ratio of 18S ribosomal RNA. Primer sequences are listed in ESM Table 2.
Histological analysis and immunohistochemistry
Isolated pancreases, gWAT and livers were fixed in 4% (wt/vol.) paraformaldehyde for 24 h and embedded in paraffin. Following on, 6 μm-thick sections were H&E stained and then used for subsequent analysis. In immunohistochemistry analyses, paraffin-embedded sections were stained with anti-F4/80, anti-CD11c, anti-CD3, anti-insulin or anti-glucagon antibodies overnight, followed by the corresponding secondary antibody for 1 h (see ESM Table 1 for antibody details) [24]. DAPI (Vector, USA) was used for nuclear counter staining. Photomicrographs were captured using the microscopes BZX800 (Keyence, Osaka, Japan) or BX61 (Olympus, Tokyo, Japan), and images were analysed using the BZX analyser or ImageJ 1.45s software (National Institutes of Health [NIH], USA; https://imagej.nih.gov/ij/) [24]. Approximately 10–30 islets were observed in the pancreas per mouse and a representative islet was selected for photomicrographs. The size of beta cells was analysed as previously reported [26].
Insulin secretion from isolated pancreatic islet
Insulin secretion from isolated pancreatic islet was measured as described previously [27]. In brief, collagenase (Sigma-Aldrich, USA) in HEPES-added Krebs-Ringer bicarbonate buffer (HKRB) supplemented with 5.6 mmol/l glucose and 0.1% (wt/vol.) BSA was injected into the common bile duct of mice and the pancreas was digested. Islets were hand collected under a microscope and were cultured overnight in RPMI-1640 medium with or without 100 ng/ml murine recombinant IL-17A (Peprotech, USA). Five islets were seeded in one well and stimulated with 2.5 mmol/l or 13.5 mmol/l glucose for 45 min in the absence or presence of recombinant IL-17A, according to the culture conditions, and insulin secretion in the culture media was measured using ELISA kits (Morinaga).
IL-17A secretion from gWAT
IL-17A secretion from gWAT was measured using a previously reported protocol for assessment of IL-1β secretion [24] with minor modification. In brief, 300 μg of gWAT was cultured in serum-free DMEM for 6 h, after which IL-17A secretion in the culture media was determined by ELISA (Fujifilm, Japan).
TNF-α secretion from hepatic nonparenchymal cells
The liver was minced and digested with collagenase at 37°C for 50 min. Samples were passed through a mesh, suspended in RPMI-1640 medium and centrifuged at 500 g for 4 min. Pellets were suspended in 33% (vol./vol.) Percoll (GE Healthcare, IL, USA) and centrifuged at 800 g at 25°C for 30 min. Pellets were incubated with ammonium-chloride-potassium (ACK) lysing buffer. Subsequently, 7.5 × 106 hepatic nonparenchymal cells (NPCs) were seeded in 24-well plates and incubated in serum-free RPMI-1640 medium for 6 h. TNF-α secretion in the culture media was determined by ELISA (Fujifilm).
Statistical analysis
Data are expressed as means ± SEM. Statistical analyses were performed using the unpaired Student’s t test between two groups or a two-way ANOVA followed by the Bonferroni test for multiple comparisons, using the software JSTAT (M. Sato, Japan; http://toukeijstat.web.fc2.com/EnglishPage.html) or StatView5.0. (Bioz, USA). Measurements over time were evaluated by a two-way repeated-measures ANOVA followed by the Bonferroni test for multiple comparisons using the software StatView5.0. A value of p < 0.05 was considered to be significant.
Results
ERα knockout efficiency in various leucocytes of KO mice
Changes in T cell subtypes towards cells that produce proinflammatory cytokines are considered to be causative mechanisms of insulin resistance in GDM [7]. In the present study, we aimed to investigate whether ERα-mediated oestrogen effects are involved in alterations in CD4+ T cell phenotypes in GDM using CD4-cre ERafl/fl (KO) mice. We initially characterised the knockout efficiency of Esr1 (gene encoding ERα) in various types of leucocytes isolated from the spleen because a low level of CD4 expression has been suggested in some types of leucocytes, such as macrophages [28]. Expression of Esr1 was almost completely deleted in CD4+ and CD8+ T cells (Fig. 1b,c; p < 0.01 and p = 0.09 for KO vs FL mice, respectively). In contrast, a reduction was not observed in macrophages, B cells or natural killer (NK cells) (Fig. 1d–f). Therefore, the T cell-specific ablation of Esr1 was verified in KO mice.
T cell ERα-deficient mice have a normal fertility rate and basal profiles
The maternal immune system plays a crucial role in the maintenance of pregnancy [10]. Nevertheless, the fertility rate estimated by the proportion of pregnant mice to vaginal mucous plug-positive mice on the morning after breeding was not significantly different between FL and KO mice (Fig. 2a). Furthermore, fetal and maternal weights and number of litters were not significantly different between FL and KO mice (Fig. 2b–d). Serum oestradiol levels were significantly higher in pregnant mice vs the same genotypes of non-pregnant mice, but did not significantly change between the genotypes (Fig. 2e). Although the liver weights of pregnant mice were heavier than those of non-pregnant mice of the same genotype, no marked differences were observed in the weights of the spleen, gWAT, and liver between FL and KO mice (Fig. 2f–h).
Effects of the maternal T cell ERα deletion on fertility rate, fetal weight and body and tissue weights in mice. (a) Fertility rate in FL-GDM and KO-GDM mice (n = 14–22). (b) Fetal weights during dissection (n = 70–116). (c) Body weight transition of mice (FL, n = 12; KO, n = 11; FL-GDM, n = 9; KO-GDM, n = 17). (d) Number of litters (n = 18–27). (e) Serum oestradiol levels on day 18.5 after breeding (n = 5–6). (f–h) Spleen (f), gWAT (g) and liver (h) weights during dissection (n = 9–18). Data are shown as means ± SEM. *p < 0.05, **p < 0.01, difference between the same genotypes of non-pregnant and pregnant mice assessed by two-way ANOVA followed by Bonferroni test
T cell ERα-deficient mouse models of GDM show deterioration of glucose tolerance and insulin secretion
We investigated glucose metabolism in each group of mice. Blood glucose levels in mice with random-fed status were indistinguishable between genotypes both before and after mating, although the glucose levels were significantly elevated on day 8.5 after breeding in pregnant mice vs non-pregnant mice of the same genotype (ESM Table 3). The glucose AUC during GTTs were indistinguishable between non-pregnant FL and non-pregnant KO mice, but were significantly higher in KO-GDM mice (2620.9 ± 122.1 mmol/l × min) than in FL-GDM mice (2308.3 ± 54.0 mmol/l × min) (p < 0.05; Fig. 3a). In contrast, the glucose AUC during ITTs was higher in FL-GDM than in FL mice, whereas no marked changes were observed between genotypes (Fig. 3b).
Effects of maternal T cell ERα deletion on glucose metabolism. (a) GTT performed on day 13.5 after breeding (n = 11–27). The time course of changes in blood glucose levels after glucose loading is shown, alongside the glucose AUC. (b) ITT performed on day 16.5 after breeding (n = 12–22). The time course of changes in blood glucose levels after insulin injection is shown, alongside the glucose AUC. (c) Serum insulin levels during 0–15 min of the GTT (GTT15) on day 12.5 after breeding (n = 5–6). At 5 min, p = 0.07 for FL-GDM vs KO-GDM. Data are shown as means ± SEM. *p < 0.05, **p < 0.01, FL vs FL-GDM; §§p < 0.01, KO vs KO-GDM; ‡‡p < 0.01, FL vs KO; †p < 0.05, ††p < 0.01, FL-GDM vs KO-GDM; assessed by two-way ANOVA followed by Bonferroni
Insufficient insulin secretion in maternal adaptation is a factor in developing GDM [4, 5]. Serum insulin levels at 30 min in the GTT did not change significantly among the four mice groups (ESM Fig. 2). To further evaluate insulin secretion in these mice, we analysed insulin levels after 0, 5 and 15 min of glucose loading (GTT15). Serum insulin levels and the insulin:glucose ratio as an indicator of insulin secretion did not change before glucose loading but were slightly lower in KO-GDM mice than in FL-GDM mice 5 min (p = 0.07) and 15 min (p < 0.05) after glucose administration (Fig. 3c, ESM Table 4). Specifically, serum insulin levels in FL-GDM and KO-GDM mice 15 min post glucose administration were 137.3 ± 18.3 pmol/l and 40.1 ± 36.5 pmol/l, respectively (p < 0.05).
T cell ERα-deficient GDM mice show similar increase in beta cell mass, but insufficient insulin secretion
We next investigated morphological changes in pancreatic beta cells because KO-GDM mice showed decreased adaptive insulin secretion. The size of the islets of Langerhans and mean beta cell size became larger under pregnant conditions as compared with non-pregnant mice of the same genotype, but was indistinguishable between FL-GDM and KO-GDM mice (Fig. 4a–d). Interestingly, the integrated density of insulin in beta cells was significantly lower in KO-GDM mice than that in FL-GDM mice (Fig. 4e). Elevated glucose levels in GDM mice may affect beta cell function; therefore, we isolated pancreatic islets from FL and KO mice and the glucose-stimulated insulin secretion was compared within each genotype (Fig. 4f,g). Insulin secretion was similar between genotypes, but glucose-stimulated (13.5 mmol/l) insulin secretion was significantly attenuated by IL-17A treatment in both genotypes. We further examined infiltration of F4/80+ macrophages and CD3+ T cells in pancreatic islet by immunostaining; however, no apparent changes in these immune cells were observed among the four mice groups (ESM Fig. 3).
Effects of maternal T cell ERα deletion on beta cells. (a, b) Representative photomicrographs of H&E-stained sections (a; FL, FL-GDM and KO-GDM, n = 9; KO, n = 7) and immunofluorescence staining for insulin and glucagon (b) in the pancreas. Scale bars, 30 μm. (c) Percentage of islet area per pancreas area. (d) Quantified beta cell size (μm2). (e) Integrated density of insulin staining in beta cells. Data are shown as means ± SE (n = 7–9). *p < 0.05, **p < 0.01, difference between the same genotypes of non-pregnant and pregnant mice; †p < 0.05, as indicated; assessed by two-way ANOVA followed by Bonferroni test. (f, g) Glucose-stimulated insulin secretion from isolated islets treated with or without 100 ng/ml IL-17A. Data are shown as means ± SEM (n = 5–6). *p < 0.05, **p < 0.01, vs 2.5 mmol/l glucose in the absence or presence of IL-17A; †p < 0.05, ††p < 0.01, as indicated; assessed by two-way ANOVA followed by Bonferroni test
T cell ERα-deficient GDM mice show enhanced chronic inflammation with increased Th17 and unaltered Th1 and Treg numbers in gWAT
Obesity-associated chronic inflammation, including the altered distribution of proinflammatory T cell subsets in visceral adipose tissue, is closely associated with glucose metabolism [29]. To investigate the impact of the deletion of ERα in T cells on T cell subset distribution, we analysed Treg, Th1 and Th17 content in gWAT by flow cytometry. Representative dot plots of these CD4+ T cells are shown in ESM Fig. 4. The contents of total CD4+ T cells in gWAT did not significantly change among the four groups of mice (Fig. 5a). Treg contents were also unaltered among the four groups (Fig. 5b). The content of IFNγ+ Th1 cells significantly decreased in GDM mice compared with non-pregnant mice of the same genotype, and no significant differences were observed between FL-GDM and KO-GDM (Fig. 5c). In contrast, Th17 contents in FL-GDM and KO-GDM mice were 0.4 ± 0.0% and 0.8 ± 0.1%, and they were significantly higher in KO-GDM than in FL-GDM mice (p < 0.05; Fig. 5d). The spontaneous secretion of IL-17A from gWAT in culture media was slightly higher in KO-GDM than in FL-GDM, although the difference was not statistically significant (ESM Fig. 5). Similar differences were not noted between the Treg, Th1 or Th17 cell content in the spleen of each mouse group (Fig. 5e–h), suggesting that the change in proportions of T cell subsets was gWAT-specific. Treg content in the thymus was significantly increased in GDM mice compared with non-pregnant mice of the same genotype and an increase was also observed between KO-GDM and FL-GDM mice (ESM Fig. 6a). Interestingly, the increase in the actual number of uterus Tregs (not the ratio of Tregs) that was observed in FL-GDM mice vs non-pregnant mice of the same genotype, was not seen in KO-GDM (ESM Fig. 6c).
Effects of maternal T cell ERα deletion on the proportion of T cell subsets in gWAT and the spleen. Cumulative flow cytometric analysis of CD4+ T cell subsets in gWAT (a–d) and the spleen (e–h). Representative dot plots are shown in ESM Fig. 4. (a, e) CD4+ T cells (n = 5–15), (b, f) CD4+CD25+FOXP3+ Tregs (n = 5–15), (c, g) IFNγ+ Th1 cells (n = 7–12) and (d, h) IL-17A+ Th17 cells (n = 7–12). Data are shown as means ± SEM. **p < 0.01, difference between the same genotypes of non-pregnant and pregnant mice; †p < 0.05, as indicated; assessed by two-way ANOVA followed by Bonferroni test
To further characterise gWAT, we analysed adipocyte sizes using H&E-stained specimens (Fig. 6a,b). Adipocytes were slightly larger in KO mice than in FL mice under non-pregnant and GDM conditions, although this finding was not statistically significant. A cell size histogram analysis also showed a rightward shift in both non-pregnant and KO-GDM mice (ESM Fig. 7). We next examined the expression of proinflammatory genes in gWAT. The expression of Emr1 (encoding F4/80, a macrophage marker) was significantly increased by 5.1-fold in KO-GDM mice compared with FL-GDM mice (p < 0.01; Fig. 6c). Similarly, the expression of Itgax (encoding CD11c, an inflammatory M1-macrophage marker) was increased in KO-GDM mice vs non-pregnant KO mice (Fig. 6d). Consequently, Tnfa expression in gWAT was significantly increased by 2.7-fold in KO-GDM mice compared with FL-GDM mice (p < 0.01; Fig. 6e). Moreover, the expression of Ifng was also increased (p = 0.051) in KO-GDM mice compared with FL-GDM mice (Fig. 6g). No significant differences were observed in Il10 expression among the four groups (Fig. 6f).
Effects of maternal T cell ERα deletion on adipocyte size and proinflammatory gene expression in gWAT. (a, b) Representative photomicrographs of H&E-stained sections of gWAT (a) and the average size of adipocytes (b). For (a), four photomicrographs per mouse were taken from five animals per group and representative images were selected. Scale bar, 50 μm. (c–g) mRNA levels of Emr1 (c), Itgax (d), Tnfa (e), Il10 (f) and Ifng (g; FL-GDM vs KO-GDM, p = 0.051). Data are shown as means ± SEM (n = 4–12). *p < 0.05, **p < 0.01, difference between the same genotypes of non-pregnant and pregnant mice; †† p < 0.01, as indicated; assessed by two-way ANOVA followed by Bonferroni test
T cell-specific ERα-deficient GDM mice do not show hepatic chronic inflammation but altered hepatokine expression
We examined the liver phenotypes of mice. In histological analyses, the livers of non-pregnant FL and KO mice showed mild steatosis or almost normal histological findings (Fig. 7a). In contrast, the livers of FL-GDM and KO-GDM mice exhibited significant lipid accumulation observed as small vacuolar changes; however, the degree of steatosis was similar between the two groups (Fig. 7a). We next evaluated chronic inflammation in the liver. TNF-α secretion from hepatic NPCs did not differ between FL-GDM and KO-GDM mice (Fig. 7b). In addition, the number of F4/80+ Kupffer cells and macrophages in the liver sections were comparable between FL-GDM and KO-GDM mice, although these cell numbers were slightly increased when compared with respective non-pregnant controls (ESM Fig. 8a,b). Consistently, hepatic expression of Emr1, Itgax, Tnfa and Ifng did not differ between the mouse groups (Fig. 7c–f). Finally, we analysed the expression of hepatokines related to glucose metabolism and GDM in the liver. Expression of both Ahsg, encoding Fetuin A, and Fgf21 in KO-GDM mice was 2.4-fold higher compared with FL-GDM mice (p < 0.05 and p = 0.09, respectively; Fig. 7g,h). In constant, no such difference was observed in Sepp1 and Lect2 expressions (ESM Fig. 8c,d).
Effects of maternal T cell ERα deletion on histology, chronic inflammation and gene expressions in the liver. (a) Representative photomicrographs of H&E-stained sections of the liver. Three photomicrographs were taken at medium magnification from each group of mice (FL, n = 9; KO and FL-GDM, n = 7; KO-GDM, n = 12), and the representative hepatic lobule was selected. Scale bar, 50 μm. (b) Levels of spontaneously secreted TNF-α in culture medium of hepatic NPCs (n = 8–9). (c–h) mRNA levels of Emr1 (c), Itgax (d), Tnfa (e), Ifng (f), Ahsg (g) and Fgf21 (h; FL-GDM vs KO-GDM, p = 0.09). Data are shown as means ± SEM (n = 12–14). *p < 0.05, difference between the same genotypes of non-pregnant and pregnant mice; †p < 0.05, as indicated; assessed by two-way ANOVA followed by Bonferroni test
Discussion
Insulin resistance and insufficient insulin secretion have been proposed as contributors towards the pathophysiology of GDM; however, their underlying mechanisms currently remain unknown [4]. In the present study, we aimed to investigate the impact of the deletion of ERα in T cells on GDM phenotype. KO-GDM mice exhibited the deterioration of glucose tolerance due to decreased insulin secretion, and increased Th17 cell number with increased proinflammatory gene expression in gWAT as compared with FL-GDM mice. In addition, KO-GDM mice showed increased expression of the hepatokine-encoding Ahsg and Fgf21 genes compared with FL-GDM mice, although hepatic steatosis and chronic inflammation were indistinguishable between the genotypes. Therefore, the effects of oestrogen on T cells are involved in maternal adaptive insulin secretion, the attenuation of chronic inflammation in adipose tissue and hepatokine expressions, all of which contribute to the maintenance of glucose metabolism during pregnancy. Increased numbers of Th17 cells and expression of Ahsg and Fgf21 have been reported in individuals with GDM [7], suggesting that a similar pathophysiology exists in KO-GDM mice and humans.
Insulin secretion was similar between FL and KO mice in the non-pregnant condition, but it was decreased in KO-GDM mice when compared with FL-GDM mice (Fig. 3c). Therefore, KO mice showed impaired maternal beta cell adaptation as a main cause of impaired glucose tolerance in KO-GDM mice. The underlying mechanisms of beta cell dysfunction in KO-GDM mice need to be elucidated. Type 1 diabetes is caused by autoreactive T cell-mediated beta cell destruction, and Tregs are considered to regulate the immune reaction [30]. In addition, islet-reactive T cells have been suggested to be involved in the development of beta cell dysfunction in a certain proportion of individuals with type 2 diabetes [31]. Therefore, we initially assumed the involvement of immune disturbance in beta cell dysfunction following T cell-specific ERα deletion. However, the numbers of infiltrated macrophages and T cells in pancreatic islet were not altered in KO mice (ESM Fig. 3); thus, no obvious islet inflammation was observed in KO-GDM mice. It is of note that KO-GDM mice showed impaired maternal adaptation in regard to beta cell function but not proliferation in the pancreas as sizes of islets and beta cells increased to a similar extent during pregnancy in both genotypes (Fig. 4a–d). Alternatively, since resident Tregs have been suggested to regulate tissue homeostasis and insulin secretion in the pancreas [32, 33], a change in the pancreatic microenvironment, including resident Treg function, may affect insulin secretion capacity in KO-GDM mice. In addition, glucose-stimulated insulin secretion was similar between isolated islets derived from FL and KO mice, but was reduced by IL-17A treatment (Fig. 4f,g), suggesting that the immunological background of KO-GDM mice may affect beta cell function in vivo. Elucidation of the molecular mechanisms of maternal beta cell adaptation by oestrogen signalling via T cells would provide further insights into the pathophysiology of GDM and approaches for GDM prevention.
Tregs are a subset of CD4+ T cells that regulate excessive immune responses [34]. Since Tregs are potentially able to alleviate obesity-associated chronic inflammation in adipose tissue, they also contribute to the maintenance of glucose homeostasis [35]. Oestrogen has been shown to promote the differentiation of naive T cells into Tregs [36, 37]; therefore, we initially hypothesised that KO-GDM mice exhibit enhanced chronic inflammation caused by impaired Treg induction. However, the abundance of Tregs did not significantly differ in the thymus (ESM Fig. 6), spleen, or visceral adipose tissue between the mouse genotypes (Fig. 5b,f). These results indicate that oestrogen is not significantly involved in the normal differentiation of Tregs in the thymus, spleen and adipose tissue. This is consistent with previous findings showing that ERα is not essential for the differentiation of Tregs [38]. In contrast, the number of Tregs in the uterus was significantly elevated in FL-GDM vs non-pregnant mice of the same genotype, but not in KO-GDM mice (ESM Fig. 6). Since Tregs contribute to fetal tolerance during pregnancy and their number increases in healthy pregnant woman [10, 39,40,41,42], the effects of oestrogen via the ERα appear to play an important role in the induction of uterine Tregs during pregnancy. However, the pregnancy rate of T cell-specific ERα-deficient mice was not significantly different from that of FL mice during allogenic pregnancy under the present experimental conditions (Fig. 2a). Therefore, ERα-mediated oestrogen effects on T cells are not essential for maintaining allogenic pregnancy. On the other hand, the immunosuppressive ability of Tregs has been reported to decrease with the deletion of ERα in vitro [43]. Assuming that the suppressive activity of Tregs is possibly reduced in KO-GDM mice in vivo, enhanced chronic inflammation in the gWAT of KO-GDM mice may be partly explained by dysfunction of ERα-deficient Tregs (Fig. 6c–g). KO-GDM mice exhibited higher expression levels of Emr1, Tnfa, and Ifng (p = 0.051) in gWAT vs FL-GDM mice, despite the lack of significant changes in body- and gWAT weights.
Th17 cells are a subset of inflammatory CD4+ T cells that are specifically related to autoimmunity [44]. Oestrogen attenuates their differentiation by directly suppressing the expression of retinoic acid receptor-related orphan receptor γt (RORγt), a transcription factor that is important for Th17 differentiation [45]. In contrast, a previous study demonstrated that the number of Th17 in the peripheral blood of humans increased in association with glucose levels at 1 h and 2 h during GTT [7] and serum IL-17 levels slightly increased with GDM, suggesting a role for Th17 in the pathology of GDM [46]. In addition, Th17 cells are involved in chronic inflammation in obesity because their differentiation is promoted in obese mice and individuals [47]. A recent study indicated that a high glucose condition, per se, drives Th17 differentiation through a reactive oxygen species-dependent TGFβ activation mechanism [48]. In this context, IL-17-deficient mice showed decreased IL-6 and IFNγ levels with improved glucose and lipid metabolism [49, 50]. In the present study, the number of Th17 cells in visceral fat was significantly higher in KO-GDM mice than in FL-GDM mice (Fig. 5d). The secretion of IL-17A from gWAT ex vivo was slightly higher in KO-GDM than in FL-GDM, although this did not reach statistical significance (ESM Fig. 5). IL-17 is known to act in a paracrine manner in the microenvironment of certain disease conditions [51, 52], and IL-17-differentiated macrophages are shown to express higher levels of Toll-like receptor 4 (TLR4) and have a greater inflammatory ability [53]. Since IL-17 causes inflammation, the observed increase in Th17 cells could be an upstream event for deteriorating chronic inflammation in the gWAT of KO-GDM mice (Fig. 6c–g).
The pathophysiology of GDM is affected by fluctuating hepatokines. Increased serum Fetuin A is associated with the induction of insulin resistance, whereas increased fibroblast growth factor 21 (FGF21) is thought to antagonise maternal insulin resistance in women with GDM [54,55,56], although the precise induction mechanism is unknown. Similar to the reports in individuals with GDM, the genetic expression of these hepatokines was increased in KO-GDM mice compared with FL-GDM mice (although the difference was not significant for Fgf21; Fig. 7g,h). Since the levels of these hepatokines in non-pregnant FL mice were as low as those in KO mice, the observed increases in KO-GDM mice may be due to the secondary influence of the GDM condition rather than the direct effect of ERα deletion in T cells. In contrast, hepatic steatosis was more prominent in pregnant mice than in non-pregnant mice but was similar between genotypes (Fig. 7a). Similarly, the expression of proinflammatory genes and proteins was indistinguishable among mouse groups (Fig. 7b–f). It currently remains unclear why chronic inflammation in KO-GDM mice was only aggravated in gWAT and remained unchanged in the liver. We speculate that an adipose tissue-specific Th17 infiltration mechanism or relatively abundant resident Kupffer cells in the liver affected the phenotype.
In summary, oestrogen contributes to the maintenance of glucose metabolism through signalling via ERα in T cells under high oestrogen conditions in pregnancy. The disruption of ERα signalling in T cells affects maternal adaptative insulin secretion, as well as function and distribution of T cell subsets under GDM conditions, particularly Th17 cells, causing chronic inflammation in visceral adipose tissue and impairing glucose metabolism.
Data availability
Data presented in this manuscript are available upon request from the corresponding authors.
Abbreviations
- 7AAD:
-
7-amino-actinomycin D
- BV421:
-
Brilliant Violet 421
- Cy7:
-
Cyanine7
- ERα:
-
Oestrogen receptor α
- FOXP3:
-
Forkhead box P 3
- FL:
-
ERα-floxed (mice)
- FL-GDM:
-
Pregnant ERαfl/fl (mice)
- GDM:
-
Gestational diabetes mellitus
- gWAT:
-
Gonadal white adipose tissue
- HFD :
-
High-fat diet
- KO:
-
CD4-cre ERαfl/fl (mice)
- KO-GDM:
-
Pregnant CD4-cre ERαfl/fl (mice)
- NK:
-
Natural killer
- NPC:
-
Nonparenchymal cells
- PE:
-
Phycoerythrin
- SVF:
-
Stromal-vascular fraction
- Th:
-
T helper
- Treg:
-
Regulatory T cell
References
Rayanagoudar G, Hashi AA, Zamora J, Khan KS, Hitman GA, Thangaratinam S (2016) Quantification of the type 2 diabetes risk in women with gestational diabetes: a systematic review and meta-analysis of 95,750 women. Diabetologia 59(7):1403–1411. https://doi.org/10.1007/s00125-016-3927-2
International Diabetes Federation (ed) (2017) IDF diabetes atlas 8th ed. International Diabetes Federation, Brussels, Belgium
Shirazian N, Emdadi R, Mahboubi M et al (2009) Screening for gestational diabetes: usefulness of clinical risk factors. Arch Gynecol Obstet 280(6):933–937. https://doi.org/10.1007/s00404-009-1027-y
Plows JF, Stanley JL, Baker PN, Reynolds CM, Vickers MH (2018) The pathophysiology of gestational diabetes mellitus. Int J Mol Sci 19(11):3342. https://doi.org/10.3390/ijms19113342
Fasshauer M, Blüher M, Stumvoll M (2013) Adipokines in gestational diabetes. Lancet Diabetes Endocrinol 2(6):488–499. https://doi.org/10.1016/S2213-8587(13)70176-1
Ategbo JM, Grissa O, Yessoufou A et al (2006) Modulation of adipokines and cytokines in gestational diabetes and macrosomia. J Clin Endocrinol Metab 91(10):4137–4143. https://doi.org/10.1210/jc.2006-0980
Sheu A, Chan Y, Ferguson A et al (2018) A proinflammatory CD4+ T cell phenotype in gestational diabetes mellitus. Diabetologia 61(7):1633–1643. https://doi.org/10.1007/s00125-018-4615-1
Schober L, Radnai D, Spratte J et al (2014) The role of regulatory T cell (Treg) subsets in gestational diabetes mellitus. Clin Exp Immunol 177(1):76–85. https://doi.org/10.1111/cei.12300
Wang X, Wu SP, DeMayo FJ (2017) Hormone dependent uterine epithelial-stromal communication for pregnancy support. Placenta 60(Suppl 1):S20–S26. https://doi.org/10.1016/j.placenta.2017.07.003
Samstein RM, Josefowicz SZ, Arvey A, Treuting PM, Rudensky AY (2012) Extrathymic generation of regulatory T cells in placental mammals mitigates maternal-fetal conflict. Cell 150(1):29–38. https://doi.org/10.1016/j.cell.2012.05.031
Haghmorad D, Amini AA, Mahmoudi MB, Rastin M, Hosseini M, Mahmoudi M (2014) Pregnancy level of estrogen attenuates experimental autoimmune encephalomyelitis in both ovariectomized and pregnant C57BL/6 mice through expansion of Treg and Th2 cells. J Neuroimmunol 277(1–2):85–95. https://doi.org/10.1016/j.jneuroim.2014.10.004
Khan D, Ansar AS (2015) The immune system is a natural target for estrogen action: opposing effects of estrogen in two prototypical autoimmune diseases. Front Immunol 6:635. https://doi.org/10.3389/fimmu.2015.00635
Pernis A (2007) Estrogen and CD4+ T cells. Curr Opin Rheumatol 19:414–420. https://doi.org/10.1097/BOR.0b013e328277ef2a
Kovats S (2015) Estrogen receptors regulate innate immune cells and signaling pathways. Cell Immunol 294(2):63–69. https://doi.org/10.1016/j.cellimm.2015.01.018
Goldstein JD, Perol L, Zaragoza B, Baeyens A, Marodon G, Piaggio E (2013) Role of cytokines in thymus- versus peripherally derived-regulatory T cell differentiation and function. Front Immunol 4:155. https://doi.org/10.3389/fimmu.2013.00155
Manrique C, Lastra G, Habibi J, Mugerfeld I, Garro M, Sowers JR (2012) Loss of estrogen receptor α signaling leads to insulin resistance and obesity in young and adult female mice. Cardiorenal Med 2(3):200–210. https://doi.org/10.1159/000339563
Nagira K, Sasaoka T, Wada T et al (2006) Altered subcellular distribution of estrogen receptor α is implicated in estradiol-induced dual regulation of insulin signaling in 3T3-L1 adipocytes. Endocrinology 147(2):1020–1028. https://doi.org/10.1210/en.2005-0825
Nadal A, Alonso-Magdalena P, Soriano S, Ropero AB, Quesada I (2009) The role of oestrogens in the adaptation of islets to insulin resistance. J Physiol 587(Pt 21):5031–5037. https://doi.org/10.1113/jphysiol.2009.177188
Nakamura T, Imai Y, Matsumoto T et al (2007) Estrogen prevents bone loss via estrogen receptor α and induction of Fas ligand in osteoclasts. Cell 130(5):811–823. https://doi.org/10.1016/j.cell.2007.07.025
Yonezawa R, Wada T, Matsumoto N et al (2012) Central versus peripheral impact of estradiol on the impaired glucose metabolism in ovariectomized mice on a high-fat diet. Am J Physiol Endocrinol Metab 303(4):E445–E456. https://doi.org/10.1152/ajpendo.00638.2011
Sameshima A, Wada T, Ito T et al (2015) Teneligliptin improves metabolic abnormalities in a mouse model of postmenopausal obesity. J Endocrinol 227(1):25–36. https://doi.org/10.1530/JOE-15-0239
Ishikawa A, Wada T, Nishimura S et al (2020) Estrogen regulates sex-specific localization of regulatory T cells in adipose tissue of obese female mice. PLoS One 15(4):e0230885. https://doi.org/10.1371/journal.pone.0230885
Onogi Y, Wada T, Kamiya C et al (2017) PDGFRβ regulates adipose tissue expansion and glucose metabolism via vascular remodeling in diet-induced obesity. Diabetes 66(4):1008–1021. https://doi.org/10.2337/db16-0881
Wada T, Ishikawa A, Watanabe E et al (2017) Eplerenone prevented obesity-induced inflammasome activation and glucose intolerance. J Endocrinol 235(3):179–191. https://doi.org/10.1530/JOE-17-0351
Watanabe E, Wada T, Okekawa A et al (2020) Stromal cell-derived factor 1 (SDF1) attenuates platelet-derived growth factor-B (PDGF-B)-induced vascular remodeling for adipose tissue expansion in obesity. Angiogenesis 23(4):667–684. https://doi.org/10.1007/s10456-020-09738-6
Takahashi M, Miyatsuka T, Suzuki L et al (2020) Biphasic changes in β-cell mass around parturition are accompanied by increased serotonin production. Sci Rep 10(1):4962. https://doi.org/10.1038/s41598-020-61850-1
Kurashina T, Dezaki K, Yoshida M et al (2015) The β-cell GHSR and downstream cAMP/TRPM2 signaling account for insulinostatic and glycemic effects of ghrelin. Sci Rep 5:14041. https://doi.org/10.1038/srep14041
Phiel KL, Henderson RA, Adelman SJ, Elloso MM (2005) Differential estrogen receptor gene expression in human peripheral blood mononuclear cell populations. Immunol Lett 97(1):107–113. https://doi.org/10.1016/j.imlet.2004.10.007
Nishimura S, Manabe I, Nagasaki M et al (2009) CD8+ effector T cells contribute to macrophage recruitment and adipose tissue inflammation in obesity. Nat Med 15(8):914–920. https://doi.org/10.1038/nm.1964
Hull CM, Peakman M, Tree TIM (2017) Regulatory T cell dysfunction in type 1 diabetes: what’s broken and how can we fix it? Diabetologia 60(10):1839–1850. https://doi.org/10.1007/s00125-017-4377-1
Brooks-Worrell B, Narla R, Palmer JP (2013) Islet autoimmunity in phenotypic type 2 diabetes patients. Diabetes Obes Metab 15:4. https://doi.org/10.1111/dom.12167
Lu J, Zhang C, Li L, Xue W, Zhang C, Zhang X (2017) Unique features of pancreatic-resident regulatory T cells in autoimmune type 1 diabetes. Front Immunol 8:1235. https://doi.org/10.3389/fimmu.2017.01235
Choi B, Kim S-H (2018) Regulatory T cells promote pancreatic islet function and viability via TGF-β1 in vitro and in vivo. Korean J Clin Lab Sci 50(3):304–312. https://doi.org/10.15324/kjcls.2018.50.3.304
Sakaguchi S, Yamaguchi T, Nomura T, Ono M (2008) Regulatory T cells and immune tolerance. Cell 133(5):775–787. https://doi.org/10.1016/j.cell.2008.05.009
Zhong J, Rao X, Braunstein Z et al (2014) T-cell costimulation protects obesity-induced adipose inflammation and insulin resistance. Diabetes 63(4):1289–1302. https://doi.org/10.2337/db13-1094
Polanczyk MJ, Hopke C, Huan J, Vandenbark AA, Offner H (2005) Enhanced FoxP3 expression and Treg cell function in pregnant and estrogen-treated mice. J Neuroimmunol 170(1–2):85–92. https://doi.org/10.1016/j.jneuroim.2005.08.023
Tai P, Wang J, Jin H et al (2008) Induction of regulatory T cells by physiological level estrogen. J Cell Physiol 214(2):456–464. https://doi.org/10.1002/jcp.21221
Mohammad I, Starskaia I, Nagy T et al (2018) Estrogen receptor α contributes to T cell-mediated autoimmune inflammation by promoting T cell activation and proliferation. Sci Siganl 11(526):eaap9415
Shima T, Sasaki Y, Itoh M et al (2010) Regulatory T cells are necessary for implantation and maintenance of early pregnancy but not late pregnancy in allogeneic mice. J Reprod Immunol 85(2):121–129. https://doi.org/10.1016/j.jri.2010.02.006
Zheng Y, Josefowicz S, Chaudhry A, Peng XP, Forbush K, Rudensky AY (2010) Role of conserved non-coding DNA elements in the Foxp3 gene in regulatory T-cell fate. Nature 463(7282):808–812. https://doi.org/10.1038/nature08750
Gobert M, Lafaille JJ (2012) Maternal-fetal immune tolerance, block by block. Cell 150(1):7–9. https://doi.org/10.1016/j.cell.2012.06.020
Hsu P, Santner-Nanan B, Dahlstrom JE et al (2012) Altered decidual DC-SIGN+ antigen-presenting cells and impaired regulatory T-cell induction in preeclampsia. Am J Pathol 181(6):2149–2160. https://doi.org/10.1016/j.ajpath.2012.08.032
Polanczyk MJ, Hopke C, Vandenbark AA, Offner H (2007) Treg suppressive activity involves estrogen-dependent expression of programmed death-1 (PD-1). Int Immunol 19(3):337–343. https://doi.org/10.1093/intimm/dxl151
Fasching P, Stradner M, Graninger W, Dejaco C, Fessler J (2017) Therapeutic potential of targeting the Th17/Treg axis in autoimmune disorders. Molecules 22(1):134. https://doi.org/10.3390/molecules22010134
Chen RY, Fan YM, Zhang Q et al (2015) Estradiol inhibits Th17 cell differentiation through inhibition of RORgammaT transcription by recruiting the ERα/REA complex to estrogen response elements of the RORgammaT promoter. J Immunol 194(8):4019–4028. https://doi.org/10.4049/jimmunol.1400806
Kuzmicki M, Telejko B, Lipinska D et al (2014) The IL-6/IL-6R/sgp130 system and Th17 associated cytokines in patients with gestational diabetes. Endokrynol Pol 65(3):169–175. https://doi.org/10.5603/EP.2014.0023
Endo Y, Asou HK, Matsugae N et al (2015) Obesity drives Th17 cell differentiation by inducing the lipid metabolic kinase, ACC1. Cell Rep 12(6):1042–1055. https://doi.org/10.1016/j.celrep.2015.07.014
Zhang D, Jin W, Wu R et al (2019) High glucose intake exacerbates autoimmunity through reactive-oxygen-species-mediated TGF-β cytokine activation. Immunity 51(4):671–681. https://doi.org/10.1016/j.immuni.2019.08.001
Lee SH, Jhun J, Byun JK et al (2017) IL-17 axis accelerates the inflammatory progression of obese in mice via TBK1 and IKBKE pathway. Immunol Lett 184:67–75. https://doi.org/10.1016/j.imlet.2017.02.004
Zuniga LA, Shen WJ, Joyce-Shaikh B et al (2010) IL-17 regulates adipogenesis, glucose homeostasis, and obesity. J Immunol 185(11):6947–6959. https://doi.org/10.4049/jimmunol.1001269
Chung AS, Wu X, Zhuang G et al (2013) An interleukin-17-mediated paracrine network promotes tumor resistance to anti-angiogenic therapy. Nat Med 19(9):1114–1123. https://doi.org/10.1038/nm.3291
Zou W, Restifo NP (2010) T(H)17 cells in tumour immunity and immunotherapy. Nat Rev Immunol 10(4):248–256. https://doi.org/10.1038/nri2742
de la Paz Sanchez-Martinez M, Blanco-Favela F, Mora-Ruiz MD, Chavez-Rueda AK, Bernabe-Garcia M, Chavez-Sanchez L (2017) IL-17-differentiated macrophages secrete pro-inflammatory cytokines in response to oxidized low-density lipoprotein. Lipids Health Dis 16(1):196. https://doi.org/10.1186/s12944-017-0588-1
Kalabay L, Cseh K, Pajor A et al (2002) Correlation of maternal serum fetuin/α2-HS-glycoprotein concentration with maternal insulin resistance and anthropometric parameters of neonates in normal pregnancy and gestational diabetes. Eur J Endocrinol 147:6. https://doi.org/10.1530/eje.0.1470243
Yuan D, Wu BJ, Henry A, Rye KA, Ong KL (2019) Role of fibroblast growth factor 21 in gestational diabetes mellitus: a mini-review. Clin Endocrinol 90(1):47–55. https://doi.org/10.1111/cen.13881
Li SM, Wang WF, Zhou LH et al (2015) Fibroblast growth factor 21 expressions in white blood cells and sera of patients with gestational diabetes mellitus during gestation and postpartum. Endocrine 48(2):519–527. https://doi.org/10.1007/s12020-014-0309-8
Acknowledgements
The authors thank: P. Chambon (Institute for Genetics and Cellular and Molecular Biology, University of Strasbourg, Strasbourg, France) and Y. Imai (Division of Integrative Pathophysiology, Proteo-Science Center, Ehime University, Ehime, Japan) for providing ERα-floxed mice; T. So (Department of Molecular Cell Biology, University of Toyama, Toyama, Japan) and M. Hamaguchi (Department of Endocrinology and Metabolism, Kyoto Prefectural University, Kyoto, Japan) for their technical advice regarding experiments with immunology and flow cytometry; K. Dezaki (Iryo Sosei University, Fukushima, Japan) for the technical advice regarding isolation of pancreatic islet; and T. Matsushima (Department of Pathology, University of Toyama, Toyama, Japan) for technical assistance with immunohistochemistry. Some of the data were presented as abstracts at the 56th EASD Annual Meeting and the 72nd Annual Congress of the Japan Society of Obstetrics and Gynecology in 2020.
Authors’ relationships and activities
The authors declare that there are no relationships or activities that might bias, or be perceived to bias, their work.
Funding
The present study was funded by the Japan Society for the Promotion of Science (JSPS KAKENHI Grant Numbers JP15K09410, JP15K15599, JP18K08469, JP19H05011 and JP19K08997), a Grant for Research Activities of the First Bank of Toyama Scholarship Foundation, and a research grant from Mitsubishi Tanabe Pharma Corporation.
Author information
Authors and Affiliations
Contributions
TT helped design the study, performed experiments, analysed the data and wrote the manuscript; TW conceived and designed the study, performed experiments, analysed the data and wrote the manuscript; KU, SO, HI, and AO performed experiments and analysed the data; AI, TI, and YM performed experiments; AS, YO, MS, and AN analysed and interpreted the data; HT analysed and interpreted the data and edited the manuscript; SS helped design the study and critically reviewed the manuscript; TS supervise the study, analysed and interpretation of data, critically reviewed and edited the manuscript. All the authors have critically contributed to the revision of the article on important intellectual content. All the authors have approved the final version of this manuscript. TW and TS are the guarantors of this work.
Corresponding author
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
ESM
(PDF 1404 kb)
Rights and permissions
About this article
Cite this article
Tanaka, T., Wada, T., Uno, K. et al. Oestrogen receptor α in T cells controls the T cell immune profile and glucose metabolism in mouse models of gestational diabetes mellitus. Diabetologia 64, 1660–1673 (2021). https://doi.org/10.1007/s00125-021-05447-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00125-021-05447-x