Abstract
Aims/hypothesis
Macrophage-mediated renal injury plays an important role in the development of diabetic nephropathy. Colony-stimulating factor (CSF)-1 is a cytokine that is produced in diabetic kidneys and promotes macrophage accumulation, activation and survival. CSF-1 acts exclusively through the c-fms receptor, which is only expressed on cells of the monocyte–macrophage lineage. Therefore, we used c-fms blockade as a strategy to selectively target macrophage-mediated injury during the progression of diabetic nephropathy.
Methods
Obese, type 2 diabetic db/db BL/KS mice with established albuminuria were treated with a neutralising anti-c-fms monoclonal antibody (AFS98) or isotype matched control IgG from 12 to 18 weeks of age and examined for renal injury.
Results
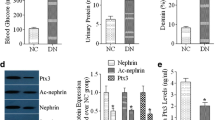
Treatment with AFS98 did not affect obesity, hyperglycaemia, circulating monocyte levels or established albuminuria in db/db mice. However, AFS98 did prevent glomerular hyperfiltration and suppressed variables of inflammation in the diabetic kidney, including kidney macrophages (accumulation, activation and proliferation), chemokine CC motif ligand 2 levels (mRNA and urine protein), kidney activation of proinflammatory pathways (c-Jun amino-terminal kinase and activating transcription factor 2) and Tnf-α (also known as Tnf) mRNA levels. In addition, AFS98 decreased the tissue damage caused by macrophages including tubular injury (apoptosis and hypertrophy), interstitial damage (cell proliferation and myofibroblast accrual) and renal fibrosis (Tgf-β1 [also known as Tgfb1] and Col4a1 mRNA).
Conclusions/interpretation
Blockade of c-fms can suppress the progression of established diabetic nephropathy in db/db mice by targeting macrophage-mediated injury.
Similar content being viewed by others
Introduction
Kidney macrophage accumulation is a feature of diabetic nephropathy that can predict patient decline in renal function [1]. Animal studies suggest that macrophages mediate renal injury in experimental models of diabetic nephropathy [2, 3]. Hyperglycaemia and AGE activate macrophages, resulting in the generation of reactive oxygen species [4] and secretion of proinflammatory cytokines (e.g. TNF-α, IL-1) and pro-fibrotic growth factors (e.g. TGF-β, platelet-derived growth factor) [3, 5, 6]. These macrophage responses exacerbate inflammation, promote tissue injury and stimulate fibrosis, thereby contributing to the development of diabetic nephropathy.
Strategies that reduce macrophage accumulation are reno-protective in inflammatory kidney diseases. For example, macrophage depletion reduces renal injury in rodent models of crescentic glomerulonephritis and renal allograft rejection [7, 8]. Similarly, genetic deficiency of molecules facilitating leucocyte recruitment (e.g. Icam1, Ccl2) and pharmacological blockade of chemokine CC motif receptors (CCR) 1 and 2 can reduce macrophage accumulation and renal injury in mouse models of diabetic nephropathy [6, 9–12]. However, these approaches are limited in that they do not target macrophages selectively, restricting the interpretation of these findings.
Recent studies show that macrophage accumulation in the kidney and other tissues can be selectively targeted using antibodies or pharmacological compounds that block c-fms signalling [13–16]. c-fms is a transmembrane receptor, which is present on monocyte–macrophages and osteoclasts and binds colony-stimulating factor (CSF)-1 with high affinity, resulting in receptor autophosphorylation and activation of signalling pathways such as phosphatidylinositol-3 kinase and extracellular signal-regulated kinase (ERK) [17]. CSF-1-induced c-fms signalling regulates the proliferation, survival and function of monocytes and fully differentiated macrophages [18–20]. Furthermore, c-fms-mediated and integrin-mediated signalling are important in the regulation of macrophage adhesion and motility [21, 22], which facilitate macrophage transmigration. Treatment with a neutralising c-fms monoclonal antibody (mAb) suppressed macrophage accumulation in mouse models of renal injury, including unilateral ureteric obstruction and renal allograft rejection [13, 14]. Similarly, an inhibitor of the c-fms receptor kinase prevented kidney macrophage accumulation in a model of ureteric obstruction [15]. These separate strategies both indicate that c-fms is a valid therapeutic target for specifically preventing macrophage-mediated renal injury.
Levels of CSF-1 are increased in human and experimental glomerulonephritis and correlate with kidney macrophage proliferation [23]. Studies in glomerulonephritis, ureteric obstruction and diabetic nephropathy have shown that glomerular podocytes and damaged tubules are major sites of CSF-1 production in the injured kidney. Since the development of diabetic nephropathy is thought to be dependent on macrophage-mediated injury [24], we evaluated whether specific targeting of macrophages by c-fms blockade would be effective in reducing renal inflammation and injury in established diabetic nephropathy. This was done using a neutralising c-fms antibody to treat type 2 diabetic nephropathy in db/db mice after the onset of albuminuria.
Methods
Treatment antibodies
AFS98 is a rat anti-mouse c-fms mAb (IgG2a) which neutralises the activity of c-fms by preventing the binding of CSF-1 [13]. AFS98 and an irrelevant control mAb (GL117, IgG2a) were produced from hybridomas and determined to be endotoxin-free before therapeutic use [13].
Animal model
Obese (db/db) and lean db/+ heterozygote control mice were created by breeding pairs of C57BL/KS db/+ mice obtained from Jackson Laboratories (Bar Harbor, ME, USA) and genotyped by PCR for the mutated leptin receptor. Mice were bred in-house at Monash Medical Centre (Clayton, Australia) and maintained on a normal diet under standard animal house conditions. Groups of obese male db/db mice (n = 12) were selected for equivalent hyperglycaemia and albuminuria at 12 weeks of age and were given intraperitoneal injections of anti-c-fms mAb (AFS98, 25 mg/kg) or control mAb (GL117, 25 mg/kg) every second day for 6 weeks. Mice were fasted for 3 h every 2 weeks and assessed for body weight, blood glucose by tail vein blood sampling (Medisense glucometer; Abbott Laboratories, Bedford, MA, USA) and urinary albumin excretion. At 18 weeks, mice were killed and serum creatinine, HbA1c and blood monocytes (flow cytometry) were measured and tissues collected and weighed. Additional control groups of 18-week-old non-diabetic db/+ mice (n = 13) and 12-week-old untreated diabetic db/db mice (n = 8) were also examined. Tissues were fixed in 4% (vol./vol.) neutral buffered formalin, methyl Carnoy’s fixative (60% methanol, 30% chloroform, 10% glacial acetic acid; vol./vol.) or 2% (wt/vol.) paraformaldehyde–lysine–periodate (PLP), or they were snap-frozen and stored at −80°C. These studies were approved by the Monash Medical Centre Animal Ethics Committee in accordance with the Australian Code of Practice for the Care and Use of Animals for Scientific Purposes, 7th edition (2004).
Biochemical analysis
Urine was collected from mice housed in metabolism cages for 18 h. Urine albumin and chemokine CC motif ligand 2 (CCL2) levels were measured with ELISA kits (Bethyl Laboratories, Montgomery, TX, USA and BD OptEIA, BD Biosciences, San Diego, CA, USA respectively). Whole mouse blood was collected by cardiac puncture in anaesthetised mice and stored as serum or heparinised plasma. HbA1c and serum and urine creatinine were measured by HPLC [25].
Histopathology analysis
Formalin-fixed sections (2 μm) were stained with periodic acid-Schiff’s reagent to assess structure and counterstained with haematoxylin to identify nuclei. Glomerular volume and mesangial matrix fraction were assessed by image analysis (Image Pro Plus; Media Cybernetics, Silver Spring, MD, USA) and cellularity was assessed by counting the total number of nuclei in 20 hilar glomerular cross-sections (gcs) per animal. Tubular atrophy was assessed by counting the number of injured (dilated, atrophied, necrotic) tubular cross sections in ten cortical fields (magnification, ×250) as a percentage of total tubular cross sections. Tubular hypertrophy was assessed by measuring the cross-sectional area of 100 transversely sectioned proximal convoluted tubules (magnification, ×400) per animal, using computer image analysis. All scoring was performed on blinded slides.
Antibodies
The primary antibodies used in this study were: (1) rabbit anti-phospho-p38 mitogen-activated protein kinase (MAPK; Thr180/Tyr182), rabbit anti-phospho-p44/42 (Thr202/204), rabbit anti-phospho c-Jun amino-terminal kinase (JNK)1/2 (Thr183/Thy185), rabbit anti-phospho activating transcription factor (ATF)-2 (Thr 69/71) and rabbit anti-cleaved caspase 3 (ASP175; all from Cell Signaling Technology, Beverly, MA, USA); (2) rabbit anti-Wilm’s tumour antigen 1 (WT1; Santa Cruz Biotechnology, Santa Cruz, CA, USA); (3) rat anti-mouse Ki-67 (TEC-3; Dako, Carpinteria, CA, USA); (4) mouse anti-α-tubulin and fluorescein-conjugated anti-α-smooth muscle actin (SMA; Sigma, St Louis, MO, USA); (5) goat anti-collagen IV (Southern Biotechnology, Birmingham, AL, USA); and (6) rat anti-CD68 and rat anti-CD169 (Serotec, Oxford, UK). Normal rabbit and goat serum or isotype-matched irrelevant IgGs were used as negative controls.
Immunohistochemistry
Immunostaining for α-SMA and collagen IV was performed on 4 µm sections fixed in methyl Carnoy’s solution. Immunostaining for cleaved caspase-3, Ki-67 and WT1 was performed on 4 μm formalin-fixed paraffin sections. Immunostaining for CD68 and CD169 was performed on 5 μm PLP-fixed cryostat sections [9]. For retrieval of antigens (except α-SMA, collagen IV, CD68 and CD169) sections were heated in a microwave oven (800 W, 12 min) or pressure cooker (high setting 20 min, full pressure 5 min) in 10 mmol/l sodium citrate buffer (pH 6.0). Antigens were then labelled by overnight incubation with primary antibody followed by biotinylated secondary antibodies (Vector Laboratories, Burlingame, CA, USA), and detection was performed using a standard peroxidase-ABC system (Vector) and development with 3,3-diaminobenzidine (DAB; Sigma) [9]. For detection of FITC-conjugated anti-α-SMA mAb, sections were incubated with peroxidase-conjugated sheep anti-fluorescein IgG (Roche Biochemicals, Mannheim, Germany) prior to DAB development [3].
For double labelling of proliferating macrophages, CD68 immunostaining was first performed with DAB development. These sections were then microwaved in citrate buffer and incubated sequentially with Ki-67 mAb, a biotinylated secondary antibody and alkaline phosphatase-conjugated ABC complexes (Vector). They were then developed with nitroblue tetrazolium (NBT) chromogen and bromochloroindolyl phosphate (BCIP) substrate (Roche).
Quantitation of immunohistochemistry
Immunostained cells were counted as glomerular+ cells/gcs or interstitial+ cells/mm2 in each animal. CD68+, CD169+, KI-67+ cells and WT1 were counted in 25 hilar gcs or 50 cortical fields (magnification, ×400). Cleaved caspase-3+ apoptotic cells and proliferating CD68+KI-67+ macrophages were counted in 50 gcs and the entire cortical interstitium. α-SMA immunostaining was assessed by image analysis in the periglomerular area (between Bowman’s capsule and surrounding tubules) around 25 hilar gcs (magnification, ×400) and expressed as the percentage of staining around the perimeter of Bowman’s capsule. Glomerular collagen IV was assessed as the percentage of area stained in 20 hilar gcs/animal. Tubulo-interstitial collagen IV was assessed by measuring the area stained and counting the number of tubular cross-sections per field (ten fields at ×250 magnification), excluding glomeruli and blood vessels. The ratio of collagen IV/tubules was standardised as the percentage of area stained:100 tubular cross-sections. This method was applied to account for the occurrence of significant tubular hypertrophy with diabetes, leading to a reduction in tubular density (and tubular basement membrane collagen staining) per field.
Western blotting
Frozen half kidneys were homogenised and sonicated in lysis buffer as previously described [26]. Lysate proteins were separated on a 4% to 20% (wt/vol.) SDS-PAGE gel and electro-blotted on to nitrocellulose membranes. Membranes were then blocked for 1 h with Odyssey blocking buffer (LI-COR, Lincoln, NB, USA) and incubated overnight with primary antibody in Odyssey buffer at 4°C. Blots were then washed with Tris-buffered saline/0.1% (vol./vol.) Tween-20 and incubated for 1 h with secondary antibody (goat anti-rabbit Alexa Fluor 680 [Invitrogen, Carlsbad, CA, USA] or donkey anti-mouse IRDye 800 [Rockland, Gilbertsville, PA, USA]). After washing, protein bands were detected using an image detection system (Odyssey Infrared; LI-COR). α-Tubulin was used as a loading control. Densitometry analysis was performed using an analyser (Gel-Pro Analyzer 3.0; Media Cybernetics). Results were expressed as the integrated optical density relative to tubulin.
Real-time PCR
Total RNA was extracted from whole kidney samples using RiboPure reagent (Ambion, Austin, TX, USA) and reverse-transcribed using a kit (Superscript First-Strand Synthesis kit; Invitrogen) with random primers. Real-time PCR was performed on Rotor-Gene 3000 (Corbett Research, Sydney, NSW, Australia) with thermal cycling conditions of 37°C for 10 min and 95°C for 5 min, followed by 50 cycles of 95°C for 15 s, 60°C for 20 s and 68°C for 20 s. The primer pairs and carboxyfluorescein-labelled minor groove binder probes used are indicated in the Electronic supplementary material (ESM) Table 1. The relative amount of mRNA was calculated using the comparative C t (ΔΔC t) method. All specific amplicons were normalised against 18S rRNA, which was amplified in the same reaction as an internal control using commercial assay reagents (Applied Biosystems, Foster City, CA, USA).
Statistical analysis
Statistical differences between two groups were analysed by the unpaired Student’s t test. Differences between multiple groups were analysed by one way ANOVA with Tukey’s multiple comparison post test. Correlations were performed using Pearson’s correlation coefficient. Data were recorded as mean ± SEM and p < 0.05 was considered significant. All analyses were performed using GraphPad Prism 5.0 (GraphPad, San Diego, CA, USA).
Results
Kidney levels of CSF-1 are increased in db/db mice during early diabetic renal injury
In contrast to non-diabetic db/+ controls, diabetic db/db mice showed signs of renal injury as early as 12 weeks of age, indicated by an elevated rate of urine albumin excretion (db/db 252 ± 44 μg/24 h vs db/+ 18 ± 4 μg/24 h, p < 0.0001). This development of renal injury in db/db mice was associated with a 36-fold increase in the relative level of kidney expression of Csf1 mRNA:18s rRNA (db/db 36.1 ± 5.6 vs db/+ 1.0 ± 0.2, p < 0.0001) and a rise in CD68+ glomerular macrophages (db/db 1.35 ± 0.10 vs db/+ 0.60 ± 0.13 cells/gcs, p < 0.0001), suggesting that kidney production of CSF-1 may contribute to the onset and progression of diabetic nephropathy by promoting renal inflammation.
c-fms antibody treatment reduces renal hypertrophy, but not obesity, diabetes or circulating monocytes in db/db mice
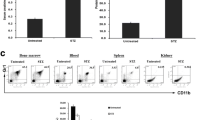
Diabetic db/db mice experienced mild weight loss between weeks 12 and 18 due to worsening hyperglycaemia, which was equivalent in mice treated with control or anti-c-fms (AFS98) mAb (Fig. 1). HbA1c levels in db/db mice at 18 weeks also demonstrated that AFS98 had no impact on hyperglycaemia during the treatment period (Fig. 1). Similarly, the peripheral monocyte count was equivalent in db/db mice receiving AFS98 or control mAb (65 ± 11 vs 64 ± 17 cells/µl, respectively, p = 0.9) at 18 weeks, suggesting that AFS98 treatment does not deplete circulating monocytes. In addition, diabetic db/db mice developed significant hepatomegaly, visceral adiposity and renal hypertrophy, but only renal hypertrophy was reduced with AFS98 treatment (Table 1).
c-fms antibody reduces macrophage accumulation in diabetic kidneys
Control diabetic db/db mice (receiving control mAb) showed a 2.4-fold increase in immunostaining for total (CD68+) glomerular macrophages and a tenfold increase in activated (CD169+) glomerular macrophages at 18 weeks of age, compared with non-diabetic db/+ controls (Table 2). AFS98 treatment reduced the total number of glomerular macrophages by 60% in db/db mice, but the number of glomerular CD169+ macrophages remained similar to control db/db mice (Table 2). The effect of AFS98 was more pronounced on kidney interstitial macrophages. The number of CD68+ and CD169+ interstitial macrophages were increased by 20% and 86%, respectively, at 18 weeks of age in diabetic db/db mice compared with db/+ mice (Table 2). AFS98 treatment not only prevented this increase, but also reduced CD68+ and CD169+ interstitial macrophages to about 30% of normal levels (Table 2, Fig. 2a, b). Double immunostaining for CD68 and Ki-67 demonstrated that glomerular and interstitial macrophage proliferation (CD68+Ki-67+ cells) was increased in control diabetic db/db mice compared with normal db/+ mice (Fig. 2c–f). Kidney macrophage proliferation in diabetic db/db mice was significantly reduced with AFS98 treatment (Fig. 2e, f); however, only about 5% of glomerular and 1% of interstitial macrophages were found to be proliferating in diabetic db/db kidneys.
c-fms antibody suppresses diabetic glomerular hyperfiltration without altering albuminuria
At 18 weeks of age, control diabetic db/db mice showed a threefold increase in creatinine clearance compared with db/+ mice, indicating significant glomerular hyperfiltration. Treatment with AFS98 prevented this hyperfiltration (Fig. 3a). Albuminuria was well established in diabetic db/db mice at the initiation of treatment (week 12; Fig. 3b), which coincided with loss of glomerular podocytes (Fig. 3c). Albuminuria continued to rise during treatment without further reduction in podocytes; however, AFS98 treatment did not alter the development of albuminuria or podocyte number (Fig. 3b, c).
c-fms antibody reduces tubular injury in diabetic db/db mice
Histological morphometric analysis of diabetic db/db glomeruli identified hypertrophy, hypercellularity and an increase in the mesangial matrix fraction, which were unaffected by AFS98 treatment (Table 3). However, immunostaining indicated that the glomerular deposition of collagen IV was partially reduced with AFS98 treatment (Table 3). Compared with db/+ mice, the kidneys of control diabetic db/db mice showed tubular hypertrophy with increased tubular apoptosis and proliferation. AFS98 treatment reduced tubular hypertrophy in db/db mice, which appeared to account for the reduction in overall kidney size (Fig. 4, Table 3). AFS98 treatment also normalised tubular apoptosis and reduced tubular proliferation in diabetic kidneys (Table 3). At this early stage of diabetic nephropathy, tubular atrophy was not prominent and was indistinguishable between the db/db groups. Consequently, other markers of tubular injury, namely urinary CCL2 and kidney Kim1 (also known as Havcr1) mRNA levels, were evaluated. The control diabetic db/db mice showed a twofold increase in urinary CCL2 and a threefold increase in whole kidney Kim1 mRNA, compared with db/+ mice. Both these markers of tubular injury were normalised with AFS98 treatment (Fig. 4). Interstitial macrophage accumulation showed a significant correlation with markers of tubular injury, including tubular hypertrophy (r = 0.56, p = 0.0079), tubular apoptosis (r = 0.51, p = 0.016), urinary CCL2 (r = 0.73, p = 0.0001) and kidney Kim1 mRNA (r = 0.60, p = 0.0007).
Obesity and hyperglycaemia are unaffected by AFS98 treatment. The body weight profiles (a) show that diabetic db/db mice treated with control mAb (triangles) and AFS98 mAb (inverted triangles) maintained a similar degree of obesity during the study compared with non-diabetic db/+ controls (circles). b The fasting blood glucose levels showed that both groups of db/db mice developed a similar hyperglycaemia profile, whereas db/+ mice maintained normal blood glucose levels. c HbA1c measured at 18 weeks demonstrated that hyperglycaemia had been equivalent in both groups of diabetic db/db mice during the study. Data are means ± SEM; n = 12–13. ***p < 0.001
AFS98 treatment reduces macrophages in diabetic kidneys. Immunostaining identified many interstitial CD68+ macrophages (brown) in the kidneys of diabetic db/db mice treated with a control mAb; this was markedly reduced by treatment with b AFS98 mAb. Magnification, ×400. c, d Proliferating kidney macrophages (arrows) were detected by dual immunostaining for CD68 (brown) and KI-67 (blue) in a c glomerulus and the d interstitium of diabetic db/db mice treated with control mAb. Magnification, ×1,000. At 18 weeks of age, AFS98 treatment had reduced the number of proliferating macrophages in e glomeruli and the f interstitium of diabetic db/db mice compared with those receiving control mAb. Data are means ± SEM; n = 12–13. *p < 0.05, **p < 0.01, ***p < 0.001
AFS98 treatment reduces glomerular hyperfiltration but not albuminuria. a Assessment of creatinine clearance at 18 weeks of age identified glomerular hyperfiltration in db/db mice treated with control mAb compared with non-diabetic db/+ controls; this was prevented by treatment with AFS98. b Compared with non-diabetic db/+ mice (circles), the urine albumin excretion rate was markedly elevated at 12 to 18 weeks in db/db mice receiving control mAb (triangles) and was unaffected by AFS98 treatment (inverted triangles). c Podocyte numbers were significantly reduced in diabetic mice (black bars) at week 12 compared with non-diabetic controls (white bars) and were similarly diminished at week 18 of diabetes in mice treated with AFS98 or control mAb (G117). Data are means ± SEM; n = 12–13. ***p < 0.001
AFS98 treatment reduces tubular damage. a Morphometric analysis of the transverse cross-sectional area of proximal convoluted tubules showed that diabetic db/db mice receiving control mAb had significant hypertrophy compared with normal db/+ mice at 18 weeks of age, which was reduced by AFS98 treatment. Tubular injury in db/db mice treated with control mAb was identified by increases in b tubular apoptosis, c urine excretion of CCL2:creatinine and d kidney levels of Kim1 vs 18S RNA compared with db/+ mice at 18 weeks of age. Injury was prevented by AFS98 treatment. Data are means ± SEM; n = 12–13. *p < 0.05, **p < 0.01, ***p < 0.001
c-fms antibody reduces renal fibrosis in diabetic db/db mice
Control diabetic db/db kidneys displayed greater numbers of apoptotic and proliferating interstitial cells and an increased accumulation of periglomerular α-SMA+ myofibroblasts and tubulo-interstitial deposition of collagen IV, compared with db/+ kidneys. AFS98 treatment reduced the number of proliferating interstitial cells, the accumulation of periglomerular myofibroblasts and the tubulo-interstitial deposition of collagen IV in diabetic db/db mice (Table 3, Fig. 5). In support of these findings, we found that kidney mRNA levels of Col4a1 and Tgf-β1 (also known as Tgfb1) were increased approximately threefold in control diabetic db/db compared with db/+ mice, but were normalised by AFS98 treatment (Fig. 5). Interstitial macrophage accumulation correlated significantly with the number of proliferating interstitial cells (r = 0.81, p < 0.0001), periglomerular α-SMA staining (r = 0.48, p = 0.0257), tubulo-interstitial collagen IV staining (r = 0.66, p = 0.0022) and kidney Tgf-β1 mRNA levels (r = 0.50, p = 0.0195).
AFS98 treatment reduces tubulo-interstitial fibrosis. Immunostaining for α-SMA (brown) (a–c) showed that its production was confined to blood vessels in a non-diabetic db/+ kidney. Periglomerular and interstitial levels of α-SMA were seen in accumulating myofibroblasts in a diabetic kidney from b a db/db mouse receiving control mAb; levels were reduced in c a diabetic db/db mouse treated with AFS98 mAb. Magnification, ×400. d–f Immunostaining identified collagen IV deposition (brown) in the tubular and glomerular basement membranes and the mesangium of d non-diabetic db/+ mice. Additional collagen IV deposition was found in the expanded mesangium and interstitial areas of a diabetic kidney from e a diabetic db/db mouse given control mAb; deposition was reduced in f a diabetic db/db mouse treated with AFS98 mAb. Magnification, ×250. g Quantitation of the kidney area staining for α-SMA and collagen IV (h) verified that AFS98 reduces interstitial myofibroblasts and collagen IV accumulation. i Diabetic db/db mice receiving control mAb had increased kidney levels of Tgf-β1 mRNA and j Col4a1 compared with non-diabetic db/+ mice; increases were prevented by AFS98 treatment. Data are means ± SEM; n = 12–13. *p < 0.05, **p < 0.01, ***p < 0.001
c-fms antibody attenuates activation of pro-inflammatory mechanisms
Compared with db/+ mice, control diabetic db/db mice showed a 2.3-, 1.5- and 3.8-fold increase in kidney levels of phospho-ERK, phospho-p38 MAPK and phospho-JNK by western blotting, respectively (Fig. 6). AFS98 treatment of db/db mice did not alter the kidney levels of phospho-ERK or phospho-p38 MAPK, but did reduce the levels of phospho-JNK and phosphorylation of the downstream transcription factor, ATF2. In addition, kidney mRNA levels of Tnf-α and Ccl2 were increased by threefold in control diabetic db/db compared with db/+ mice, this increase being prevented by AFS98 treatment (Fig. 7). Kidney interstitial macrophage accumulation correlated with kidney levels of phospho-ATF2 (r = 0.56, p = 0.0066) and the mRNA levels of Tnf-α (r = 0.71, p = 0.0002) and Ccl2 (r = 0.50, p = 0.0203).
Effects of AFS98 treatment on MAPK signalling in diabetic kidneys. a Representative western blots show the kidney levels of phospho-ERK, phospho-p38, phospho-JNK, phospho-ATF2 and α-tubulin (loading control) in db/+ mice and diabetic db/db mice receiving control mAb and AFS98. b–e Densitometry analysis demonstrated that kidney levels of each of the above proteins were increased in untreated diabetic db/db mice compared with db/+ mice. The elevated kidney levels of b phospho-ERK and c phospho-p38 in diabetic db/db mice given control mAb were not different from those of mice given AFS98 treatment. However, the elevated kidney levels of d phospho-JNK and e phospho-ATF2 in db/db mice receiving control mAb were reduced by AFS98 treatment. Data are means ± SEM; n = 12–13. *p < 0.05, **p < 0.01, ***p < 0.001
AFS98 treatment suppresses gene transcription of proinflammatory cytokines. Diabetic db/db mice receiving control mAb had a threefold increase in kidney mRNA levels of a Tnf-α and b Ccl2 compared with db/+ mice; increases were prevented by AFS98 treatment. Data are means ± SEM; n = 12–13. **p < 0.01, ***p < 0.001
Discussion
This study demonstrates that CSF-1 plays a significant role in the development of type 2 diabetic nephropathy through its interaction with macrophage c-fms.
AFS98 treatment did not affect the obesity or progression of diabetes in db/db mice. Previous studies indicate that macrophage infiltration into adipose tissue promotes insulin resistance in insulin-sensitive tissues, leading to type 2 diabetes [27–29]. Consequently, c-fms antibody blockade could have reduced the accumulation of adipose macrophages, thereby restoring insulin sensitivity and lowering hyperglycaemia. However, since the fasting blood glucose profile and HbA1c levels were unaffected by AFS98 treatment, we did not explore whether this treatment altered adipose macrophages in our db/db mice.
Our primary outcome was that AFS98 treatment reduced kidney macrophages in diabetic db/db mice. Both direct and indirect mechanisms facilitating macrophage accumulation were affected. As expected, AFS98 suppressed local macrophage proliferation in diabetic kidneys; however, given that only 1% to 5% of total kidney macrophages were proliferating at week 18, it is likely that our c-fms blocking strategy contributed to the reduction in kidney macrophages by additional mechanisms. AFS98 did not cause any significant difference in apoptosis of interstitial cells at week 18; however, it did reduce the interstitial macrophage numbers to 30% of normal levels, suggesting that this treatment may decrease the duration of macrophage survival. AFS98 treatment may also have indirectly suppressed macrophage recruitment by reducing production of CCL2 in diabetic kidneys. In addition, c-fms blockade may inhibit monocyte–macrophage migration through regulation of macrophage adhesion and motility [21, 22] and by preventing kidney macrophages from producing their own monocyte/macrophage chemoattractants, including CSF-1. Indeed, CSF-1 can be a potent chemoattractant for cells expressing high levels of c-fms [30] and may also serve to recruit monocytes from the circulation [31].
It was surprising that AFS98 reduced the number of activated (CD169+) macrophages in the interstitium, but not in the glomeruli of diabetic db/db mice. One explanation is that circulating immune complexes, capable of activating macrophages, accumulate in the glomeruli, but not in the interstitium of diabetic db/db kidneys [2]. In this study, we detected glomerular deposition of IgG and C3 by immunofluorescence in db/db mice, with no difference between control and treated groups (data not shown). Renal biopsy studies have also identified glomerular deposits of immune complexes in diabetic patients [32]. Another possibility is that the activation of glomerular macrophages is regulated indirectly by the effects of the diabetic milieu on mesangial cells or podocytes through cytokine secretion or cell–cell interactions and that these are unaffected by AFS98. Indeed the differing microenvironments of the glomerulus and the tubulo-interstitium can influence the macrophage phenotype [9], which may be an important feature of diabetic nephropathy.
Our second main finding was that renal hyperfiltration was prevented by AFS98 treatment, suggesting a role for macrophages in this process. AFS98 reduced hypertrophy of the kidney and proximal tubules, which may have resulted in reduced tubular re-absorption. In diabetic kidneys, tubular re-absorption is usually increased, a finding thought to be the dominant cause of hyperfiltration operating through a tubulo-glomerular feedback mechanism [33]. Therefore, macrophages may stimulate diabetic hyperfiltration by promoting processes that increase tubular re-absorption. In addition, tubules are known to secrete creatinine [34], which also may be increased by macrophage-mediated injury during diabetes, contributing to the apparent increase in creatinine clearance.
Although treatment with AFS98 reduced renal inflammation and hyperfiltration, it had no effect on levels of established albuminuria in db/db mice. Several factors may account for this. Our analysis showed that irreversible podocyte loss had occurred in diabetic glomeruli during the establishment of albuminuria prior to treatment. c-fms blockade was unable to repair this damage. AFS98 treatment was also unable to reduce the number of activated glomerular macrophages, which may be critical for promoting albuminuria. In addition, albuminuria before treatment may have reached a level that caused sufficient ongoing injury to the kidney to be self-sustaining and therefore not reversible by anti-c-fms therapy. These concepts are supported by a previous study, which similarly showed that intervention treatment with a CCR1 antagonist was able to reduce interstitial inflammation, but not albuminuria in an accelerated model of type 2 diabetes [11]. This study and ours both suggest that interstitial macrophages are not important for the maintenance of overt albuminuria in diabetic kidney disease. It is also noteworthy that the protection from hyperfiltration achieved with AFS98 did not affect the albuminuria level in these diabetic mice. One possible interpretation is that AFS98 treatment also induced an increase in glomerular permeability to albumin. However, this finding could also be explained by AFS98 reducing tubular re-absorption of filtered albumin.
Our third important finding was that AFS98 treatment protected diabetic db/db kidneys from tubulo-interstitial damage, which included a reduction in tubular injury (hypertrophy, proliferation, apoptosis and mRNA levels of Kim1) and interstitial fibrosis (interstitial myofibroblast accumulation and tubulo-interstitial deposition of collagen IV). These results provide convincing evidence that macrophages promote tubular injury and interstitial fibrosis in diabetic kidneys, a concept proposed by previous studies [3,11]. In the current analysis, we noted that c-fms blockade was associated with a reduction in kidney mRNA levels of inflammatory cytokines (Tnf-α, Ccl2), a profibrotic cytokine (Tgf-β1) and Col4a1. Production of these mediators is known to be regulated by intracellular MAPK signalling, which is induced by elements of the diabetic milieu. Our examination of MAPK activation in the diabetic kidneys found that AFS98 treatment caused significant attenuation of JNK signalling and reduced activation of the downstream transcription factor ATF2. These results suggest that the effects of c-fms blockade are at least partly mediated by a reduction in JNK activity, which presumably regulates the functions of macrophages and other renal cells. Other studies have indicated that the activation of JNK following c-fms signalling is critical for the development, proliferation and survival of macrophages [35]. In addition, JNK signalling stimulates macrophage production of proinflammatory mediators such as TNF-α and IL-1, which can cause injury to other renal cells or further exacerbate the inflammatory response [36]. Indeed, recent evidence in non-diabetic kidney disease suggests that the activation of macrophages and their potential to cause renal injury are partly dependent on JNK signalling [37]. However, it is also possible that the reduction of kidney JNK signalling in AFS98-treated mice is due to the depletion of macrophages and their ability to induce JNK signalling in other renal cells. Other studies have shown that JNK signalling can promote apoptosis of tubular cells [38, 39], the formation of myofibroblasts [40, 41] and TGF-β-induced matrix production [42]. Therefore, JNK signalling may be an important therapeutic target for inhibiting macrophage-mediated injury in diabetic nephropathy.
In conclusion, this study shows that specific targeting of macrophages with a neutralising c-fms antibody can suppress the development of inflammation, tissue injury and fibrosis in the kidneys of a mouse model of type 2 diabetes with established albuminuria. This evidence supports the concept that macrophages play a critical role in the development of diabetic nephropathy. In addition, our findings indicate that the development of inhibitors of c-fms or JNK signalling may provide a strategy for protecting diabetic kidneys against macrophage-mediated injury.
Abbreviations
- ATF:
-
Activating transcription factor
- CCL2:
-
Chemokine CC motif ligand 2
- CCR:
-
Chemokine CC motif receptor
- CSF:
-
Colony-stimulating factor
- DAB:
-
3,3-Diaminobenzidine
- ERK:
-
Extracellular signal-regulated kinase
- gcs:
-
Glomerular cross-section
- JNK:
-
c-Jun amino-terminal kinase
- mAb:
-
Monoclonal antibody
- MAPK:
-
Mitogen-activated protein kinase
- PLP:
-
Paraformaldehyde–lysine–periodate
- SMA:
-
Smooth muscle actin
- WT1:
-
Wilm’s tumour antigen 1
References
Nguyen D, Ping F, Mu W, Hill P, Atkins RC, Chadban SJ (2006) Macrophage accumulation in human progressive diabetic nephropathy. Nephrology (Carlton) 11:226–231
Chow F, Ozols E, Nikolic-Paterson DJ, Atkins RC, Tesch GH (2004) Macrophages in mouse type 2 diabetic nephropathy: correlation with diabetic state and progressive renal injury. Kidney Int 65:116–128
Chow FY, Nikolic-Paterson DJ, Atkins RC, Tesch GH (2004) Macrophages in streptozotocin-induced diabetic nephropathy: potential role in renal fibrosis. Nephrol Dial Transplant 19:2987–2996
Urata Y, Yamaguchi M, Higashiyama Y et al (2002) Reactive oxygen species accelerate production of vascular endothelial growth factor by advanced glycation end products in RAW264.7 mouse macrophages. Free Radic Biol Med 32:688–701
Rashid G, Korzets Z, Bernheim J (2006) Advanced glycation end products stimulate tumor necrosis factor-alpha and interleukin-1 beta secretion by peritoneal macrophages in patients on continuous ambulatory peritoneal dialysis. Isr Med Assoc J 8:36–39
Chow FY, Nikolic-Paterson DJ, Ozols E, Atkins RC, Tesch GH (2005) Intercellular adhesion molecule-1 deficiency is protective against nephropathy in type 2 diabetic db/db mice. J Am Soc Nephrol 16:1711–1722
Duffield JS, Tipping PG, Kipari T et al (2005) Conditional ablation of macrophages halts progression of crescentic glomerulonephritis. Am J Pathol 167:1207–1219
Jose MD, Ikezumi Y, van Rooijen N, Atkins RC, Chadban SJ (2003) Macrophages act as effectors of tissue damage in acute renal allograft rejection. Transplantation 76:1015–1022
Chow FY, Nikolic-Paterson DJ, Ozols E, Atkins RC, Rollin BJ, Tesch GH (2006) Monocyte chemoattractant protein-1 promotes the development of diabetic renal injury in streptozotocin-treated mice. Kidney Int 69:73–80
Chow FY, Nikolic-Paterson DJ, Ma FY, Ozols E, Rollins BJ, Tesch GH (2007) Monocyte chemoattractant protein-1-induced tissue inflammation is critical for the development of renal injury but not type 2 diabetes in obese db/db mice. Diabetologia 50:471–480
Ninichuk V, Khandoga AG, Segerer S et al (2007) The role of interstitial macrophages in nephropathy of type 2 diabetic db/db mice. Am J Pathol 170:1267–1276
Kanamori H, Matsubara T, Mima A et al (2007) Inhibition of MCP-1/CCR2 pathway ameliorates the development of diabetic nephropathy. Biochem Biophys Res Commun 360:772–777
Le Meur Y, Tesch GH, Hill PA et al (2002) Macrophage accumulation at a site of renal inflammation is dependent on the M-CSF/c-fms pathway. J Leukoc Biol 72:530–537
Jose MD, Le Meur Y, Atkins RC, Chadban SJ (2003) Blockade of macrophage colony-stimulating factor reduces macrophage proliferation and accumulation in renal allograft rejection. Am J Transplant 3:294–300
Ma FY, Liu J, Kitching AR, Manthey CL, Nikolic-Paterson DJ (2009) Targeting renal macrophage accumulation via c-fms kinase reduces tubular apoptosis but fails to modify progressive fibrosis in the obstructed rat kidney. Am J Physiol Renal Physiol 296:F177–F185
Hamilton JA (2008) Colony-stimulating factors in inflammation and autoimmunity. Nat Rev Immunol 8:533–544
Pixley FJ, Stanley ER (2004) CSF-1 regulation of the wandering macrophage: complexity in action. Trends Cell Biol 14:628–638
Tushinski RJ, Oliver IT, Guilbert LJ, Tynan PW, Warner JR, Stanley ER (1982) Survival of mononuclear phagocytes depends on a lineage-specific growth factor that the differentiated cells selectively destroy. Cell 28:71–81
Tushinski RJ, Stanley ER (1985) The regulation of mononuclear phagocyte entry into S phase by the colony stimulating factor CSF-1. J Cell Physiol 122:221–228
Irvine KM, Burns CJ, Wilks AF, Su S, Hume DA, Sweet MJ (2006) A CSF-1 receptor kinase inhibitor targets effector functions and inhibits pro-inflammatory cytokine production from murine macrophage populations. FASEB J 20:1921–1923
Pixley FJ, Lee PS, Condeelis JS, Stanley ER (2001) Protein tyrosine phosphatase phi regulates paxillin tyrosine phosphorylation and mediates colony-stimulating factor 1-induced morphological changes in macrophages. Mol Cell Biol 21:1795–1809
Caveggion E, Continolo S, Pixley FJ et al (2003) Expression and tyrosine phosphorylation of Cbl regulates macrophage chemokinetic and chemotactic movement. J Cell Physiol 195:276–289
Isbel NM, Nikolic-Paterson DJ, Hill PA, Dowling J, Atkins RC (2001) Local macrophage proliferation correlates with increased renal M-CSF expression in human glomerulonephritis. Nephrol Dial Transplant 16:1638–1647
Tesch GH (2007) Role of macrophages in complications of type 2 diabetes. Clin Exp Pharmacol Physiol 34:1016–1019
Johns BA, Broten T, Stranieri MT, Holahan MA, Cook JJ (2001) Simple high-performance liquid chromatographic method to analyze serum creatinine has several advantages over the Jaffé picric acid reaction as demonstrated with a cimetidine dose response in rhesus monkeys. J Chromatogr B Biomed Sci Appl 759:343–348
Lim AK, Nikolic-Paterson DJ, Ma FY et al (2009) Role of MKK3-p38 MAPK signalling in the development of type 2 diabetes and renal injury in obese db/db mice. Diabetologia 52:347–358
Weisberg SP, McCann D, Desai M, Rosenbaum M, Leibel RL, Ferrante AW Jr (2003) Obesity is associated with macrophage accumulation in adipose tissue. J Clin Invest 112:1796–1808
Xu H, Barnes GT, Yang Q et al (2003) Chronic inflammation in fat plays a crucial role in the development of obesity-related insulin resistance. J Clin Invest 112:1821–1830
Arkan MC, Hevener AL, Greten FR et al (2005) IKK-beta links inflammation to obesity-induced insulin resistance. Nat Med 11:191–198
Pierce JH, Di Marco E, Cox GW et al (1990) Macrophage-colony-stimulating factor (CSF-1) induces proliferation, chemotaxis, and reversible monocytic differentiation in myeloid progenitor cells transfected with the human c-fms/CSF-1 receptor cDNA. Proc Natl Acad Sci U S A 87:5613–5617
Wang JM, Griffin JD, Rambaldi A, Chen ZG, Mantovani A (1988) Induction of monocyte migration by recombinant macrophage colony-stimulating factor. J Immunol 141:575–579
Cavallo T, Pinto JA, Rajaraman S (1984) Immune complex disease complicating diabetic glomerulosclerosis. Am J Nephrol 4:347–354
Thomson SC, Vallon V, Blantz RC (2004) Kidney function in early diabetes: the tubular hypothesis of glomerular filtration. Am J Physiol Renal Physiol 286:F8–F15
Schwartz GJ, Furth SL (2008) Glomerular filtration rate measurement and estimation in chronic kidney disease. Pediatr Nephrol 22:1839–1848
Himes SR, Sester DP, Ravasi T, Cronau SL, Sasmono T, Hume DA (2006) The JNK are important for development and survival of macrophages. J Immunol 176:2219–2228
Chan ED, Winston BW, Jarpe MB, Wynes MW, Riches DW (1997) Preferential activation of the p46 isoform of JNK/SAPK in mouse macrophages by TNF alpha. Proc Natl Acad Sci U S A 94:13169–13174
Ikezumi Y, Hurst L, Atkins RC, Nikolic-Paterson DJ (2004) Macrophage-mediated renal injury is dependent on signaling via the JNK pathway. J Am Soc Nephrol 15:1775–1784
Ma FY, Flanc RS, Tesch GH et al (2007) A pathogenic role for c-Jun amino-terminal kinase signaling in renal fibrosis and tubular cell apoptosis. J Am Soc Nephrol 18:472–484
Wang L, Matsushita K, Araki I, Takeda M (2002) Inhibition of c-Jun N-terminal kinase ameliorates apoptosis induced by hydrogen peroxide in the kidney tubule epithelial cells (NRK-52E). Nephron 91:142–147
Liu S, Xu SW, Kennedy L et al (2007) FAK is required for TGFbeta-induced JNK phosphorylation in fibroblasts: implications for acquisition of a matrix-remodeling phenotype. Mol Biol Cell 18:2169–2178
Liu Q, Mao H, Nie J et al (2008) Transforming growth factor-beta 1 induces epithelial–mesenchymal transition by activating the JNK-Smad3 pathway in rat peritoneal mesothelial cells. Perit Dial Int 28(Suppl 3):S88–S95
Hocevar BA, Brown TL, Howe PH (1999) TGF-beta induces fibronectin synthesis through a c-Jun N-terminal kinase-dependent, Smad4-independent pathway. EMBO J 18:1345–1356
Acknowledgements
We thank E. Ozols, N. Gibson and P. Frost for their technical assistance. The study was funded by the National Health and Medical Research Council of Australia, Kidney Health Australia and Eli Lilly.
Duality of interest
The authors report that there is no duality of interest associated with this manuscript.
Author information
Authors and Affiliations
Corresponding author
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Lim, A.K.H., Ma, F.Y., Nikolic-Paterson, D.J. et al. Antibody blockade of c-fms suppresses the progression of inflammation and injury in early diabetic nephropathy in obese db/db mice. Diabetologia 52, 1669–1679 (2009). https://doi.org/10.1007/s00125-009-1399-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00125-009-1399-3