Abstract
Chronic exposure to high levels of particulate matter (PM) is correlated to a higher prevalence of cardio-metabolic disturbances. Adipose tissue represents a pivotal regulator of metabolic homeostasis, and its dysfunction is associated with health issues in PM-exposed models. This review discusses the adaptive changes of white (WAT) and brown (BAT) adipose tissue in response to fine particulate matter (PM2.5), investigating the underlying pathophysiology. In exposed models, PM2.5 increases oxidative stress and impairs mitochondria functionality and biogenesis in WAT and BAT. Chronic exposure also upregulates the main apoptotic/pro-inflammatory pathways and promotes the infiltration of monocytes and the accumulation of activated macrophages. Oxidative stress and inflammation are responsible for the inhibition of insulin signal transduction and glucose uptake in both the adipose tissues. The increased inflammatory status also suppresses the metabolic activity of brown adipocytes, promoting the whitening. Altogether, this evidence suggests the shift of WAT and BAT toward an inflammatory and metabolic dysfunctional phenotype. Although the underlying mechanisms remain to be clarified, the development of inflammation in lungs, gut, and hypothalamus seems to have a pivotal role in the alteration of adipose tissue homeostasis. The potential consequences on systemic cardio-metabolic health render the relationship PM-adipose tissue a key issue to investigate.
Graphical abstract

Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Particulate matter (PM) is a component of air pollution containing a complex mixture of solid and liquid particles, derived from human activities and natural sources. Variability in size, shape, and chemical composition is responsible for differing toxicity of inhaled PM [1]. Chronic exposure to airborne PM has a profound impact on human health, especially in the early stages of life and frail subjects [2, 3]. In humans and animals, the chronic inhalation of fine PM (PM2.5; mean diameter of particles ~2.5 μm) is associated with the development of insulin resistance [4], metabolic syndrome [5], and diabetes [2, 6,7,8]. The functional impairment of tissues such as the brain, liver, and adipose tissue, secondary to PM2.5 exposure, is likely implicated in the development of such dysmetabolic conditions [9,10,11].
Growing evidence suggests that PM2.5 inhalation negatively influences both white and brown adipose tissue (WAT and BAT, respectively) [12, 13]. In addition, the development of dysfunction in both the adipose tissues is associated with the worsening of health conditions in humans and animals undergoing chronic PM exposure [12, 14,15,16,17,18,19,20,21,22,23,24,25,26,27,28].
Considering these findings, the investigation of adipose tissue response to PM2.5 can represent a crucial step for understanding the health consequences of prolonged PM2.5 exposure. This review discusses the adaptive and pathological responses of BAT and WAT of rodents undergoing PM2.5 exposure.
Adipose tissue is an important regulator of metabolic homeostasis
Adipose tissue is an ensemble of different cell types comprising adipocytes, immune, vascular, and stromal cells. Adipocytes express a highly adaptive biological profile [29] as they can activate specific pathways in response to surrounding environmental changes and varying nutritional conditions [29, 30]. The crosstalk between adipose tissue and organs such as the brain, liver, and skeletal muscle helps to coordinate an articulated network, which is critical for the control of systemic metabolic health [30,31,32].
WAT is primarily intended to store the energy surplus in the form of triglycerides (TGs) [30]. The tight inter-communication between adipocytes and resident immune cells regulates inflammatory balance and insulin sensitivity in WAT [30, 32,33,34]. Factors such as energy excess, toxicants, and pro-inflammatory agents can disrupt this equilibrium leading to the development of inflammation and metabolic dysfunction [30]. The spillage of pro-inflammatory/diabetogenic mediators such as interleukin 1β (IL-1β), interleukin 6 (IL-6), tumor necrosis factor-α (TNFα), and C–C motif chemokine ligand-2 (CCL2) from dysfunctional WAT worsens gluco-metabolic health [35,36,37].
BAT promotes the conversion of stored fats into energy through the sympathetic-mediated activation of uncoupling protein (UCP)-1 [34, 38]. Brown adipocytes increase energy expenditure and improve insulin sensitivity by stimulating glucose and fatty free acids (FFAs) oxidation [34, 38, 39]. White and brown adipocytes can mutually interconvert given appropriate stimuli [40]: physical activity stimulates the browning [34, 40]; in contrast, obesity is correlated with increased whitening [38, 41]. The whitening of brown adipocytes is characterized by decreased mitochondrial fitness and marks dysfunction as white-shifted adipocytes are prone to develop a pro-inflammatory/apoptotic phenotype [34, 42]
Airborne particulate matter
Airborne PM is a collection of microscopic particles of different sizes, consisting of carbonaceous particles with adsorbed chemicals [43]. Transition metals (Fe, Cu, Ni) account for the larger fraction of inorganic molecules constituting PM. Endotoxins, polycyclic aromatic hydrocarbons (PAHs), and quinones [44, 45] typically represent the organic fraction of PM. Differences in size, shape, and chemical composition are responsible for the toxicity of specific subclasses of inhaled PM [1, 43].
In the respiratory compartment, PM dissolves in the aqueous lining, coming into direct contact with alveolar cells [1]. Alveolar macrophages sequester particles of various size shifting towards an activated phenotype [46]; the PM-induced activation of macrophages is critical for the increase of local and systemic inflammation [1, 47,48,49].
The finest fraction of PM (~0.2 μm) enters systemic circulation by crossing the alveolar (or gastrointestinal; GI) barrier and could be internalized in tissues via endocytosis-mediated mechanisms [1, 46, 47, 49,50,51,52,53]. Larger particles can reach extrapulmonary organs transported by alveolar macrophages [53]. Also, organic/inorganic fractions of PM, as well as materials adsorbed to the surface of inhaled particles can pass into circulation and accumulate in central/peripheral tissues [43].
PM2.5 exposure increases oxidative stress and impairs mitochondria and endoplasmic reticulum
In isolated cells, PM elicits its cytotoxic activity by altering membrane stability and stimulating the production of reactive oxygen species (ROS) [1]. Both the carbonaceous nuclei and adsorbed organic/inorganic chemicals play a critical role in this respect [43]. Reactive constituents of PM (metals, PAHs, quinones) propel the production of ROS by inducing Fenton’s reactions and/or stimulating the oxidation of other organic macromolecules (Fig. 1) [4, 5]. PM can also generate ROS by interfering with the activity of the mitochondrial respiratory chain [54].
Intracellular pathways conducive to inflammation and insulin resistance are upregulated in adipose tissue of PM2.5-exposed animals. PM2.5 enhances ROS production. PM2.5 constituents (e.g., endotoxins) and pro-inflammatory cytokines stimulate the NF-κB pathway. ROS are responsible for the impairment of ER and mitochondria. ER stress and ROS upregulate JNK, p38, and ERK and suppress AMPK. NF-kB and JNK enable pro-inflammatory/apoptotic response and downregulate insulin signaling. Mitochondrial dysfunction impairs substrate oxidation and insulin sensitivity. AKT, Protein kinase B; AMPK, AMP-activated protein kinase; ASK, apoptosis signal-regulating kinase 1; CCL2, chemokine C–C motif ligand 2; ER, endoplasmic reticulum; ERK, extracellular signal-regulated kinase; IL-6, interleukin 6; IR, insulin receptor; ILR; interleukin receptor; IRS, insulin receptor substrate; JNK 1, 2; NF-κB, nuclear factor kappa-light-chain-enhancer of activated B cells; p38, p38 mitogen-activated protein kinase; PM, particulate matter; ROS, reactive oxygen species; TLR4, Toll-like receptor 4; TGs, triglycerides; TNFα, tumor necrosis factor-α; TNFR, tumor necrosis factor receptor. **These pathways are not demonstrated in adipose tissue
The upregulation of superoxide anions and markers such as superoxide dismutase (SOD), nuclear factor erythroid 2-related factor (Nrf)-2, and heat shock 70 kDa protein-1 (HSP72) provides supporting evidence for increased ROS in WAT and BAT of PM2.5-exposed animals [23, 55]. Chiefly, HSP72 represents a hallmark of functional derangement under PM exposure, since its expression correlates with inflammation and insulin resistance [56, 57]. ROS act as co-factors in the induction of mitochondria and endoplasmic reticulum (ER) functional impairment [58].
Mitochondria are essential for energy production. In adipose tissue, they regulate lipid metabolism, insulin sensitivity, and the secretion of key adipokines [59, 60]. The proper functioning of mitochondria in WAT and BAT warrants systemic gluco-metabolic homeostasis [34, 42, 61, 62].
PM2.5 and its chemical constituents can impair mitochondria [53]. Also, pro-inflammatory mediators and ER stress can negatively impact mitochondrial functionality (Fig. 1) [9, 23, 55, 61,62,63]. Studies in rodents demonstrate that mitochondrial function and biogenesis are compromised upon prolonged PM2.5 exposure [1, 54, 64] (Fig. 1). In WAT and BAT of mice undergoing either inhalation or intratracheal instillation of PM2.5, the expression of mitochondrial biogenetic markers–peroxisome proliferator activated receptor gamma coactivator 1-(PGC-1)α and UCP-1–was significantly suppressed [23, 25, 28, 65, 66]. Similarly, a reduction in mitochondrial number and size was observed in BAT and WAT of PM2.5-exposed rodents [23, 65, 66]. These changes were associated with the increase in superoxide anion and Nrf-2 in both WAT and BAT [23, 65], suggesting a causal role of ROS in the alteration of mitochondrial biogenesis/functionality and vice versa (Fig. 1).
ER represents a pivotal structure for adipocyte metabolic health [67, 68]. ER dysfunction is responsible for the development of chronic inflammation in adipose tissue [68]. ROS enhances the unfolded protein response (UPR), which represents a cellular self-protection mechanism and a reliable indicator of ER dysfunction [58, 69, 70].
In mice exposed to chronic PM2.5 inhalation, Mendez et al. observed a significant increase in ER stress in WAT, as demonstrated by the induction of the UPR activator–binding immunoglobulin protein (BiP) [71]. In addition, the long-term exposure to high PM2.5 concentrations was found to activate the UPR pathway by upregulating the expression of regulated IRE1-dependent mRNA decay and the constitutive elements of ER-associated degradation pathways [71].
PM2.5 triggers inflammation and insulin resistance
In WAT of PM2.5-exposed animals, mitochondrial and ER impairment is associated with insulin resistance and inflammation [23, 65, 71]. This finding is in accordance with evidence from non-exposed models [61, 68] and indicates that mitochondrial and ER dysfunction can upregulate the molecular pathways conducive to inflammation and insulin resistance in the adipose tissue of PM2.5-exposed animals [72] (Fig. 1).
JNK is a cell regulator, enabled by a variety of stressors [73]; its activation induces apoptosis and suppresses the insulin signal in adipocytes [73,74,75]. PM2.5 exposure was demonstrated to augment JNK expression in organs critical for metabolic regulation such as liver and adipose tissue [17, 25, 76]. Pan et al. showed a significant increase in pJNK in the visceral WAT (vWAT) of both lean and ob/ob mice undergoing PM2.5 inhalation, compared to non-exposed [25].
The activation of p38 mitogen-activated protein kinase (p38) and extracellular signal-regulated kinase (ERK) inhibits insulin signaling [77, 78] and promotes the whitening of brown adipocytes [79, 80]. In human observational studies, the expression of p38 and ERK in vWAT was correlated with the concentration of PM [81]. In lean and db/db mice PM2.5 inhalation increased p38 and ERK expression [25]. Interestingly, in high-fat diet (HFD)-fed PM2.5-exposed rodents, the inhibition of monocyte recruitment efficiently prevented the activation of p38 in WAT, suggesting that the immune-mediated inflammation is involved in the activation of the p38 pathway [18].
The 5′-AMP-activated protein kinase (AMPK) enables the translocation of the glucose transporter (GLUT)-4 to plasma membrane and promotes glucose and FFAs oxidation [82]. In WAT, AMPK suppresses the nuclear factor kappa-light-chain-enhancer of activated B-cells (NF-κB) and the adipocyte pro-inflammatory shift [17, 25, 83, 84] (Fig. 1). In animal models, PM2.5 intratracheal instillation significantly reduced phosphorylated AMPK (pAMPK) in the subcutaneous WAT (sWAT) of lean mice [28]. In contrast, the pharmacological activation of AMPK effectively prevented the PM2.5-induced whitening in BAT.
The protein kinase B (AKT) mediates the transduction of insulin signal [85]. Reduced phosphorylation of AKT473 (pAKT) is associated with inflammation and insulin resistance in WAT [86]. In response to PM2.5, the expression of pAKT and GLUT-4 significantly decreased in vWAT and BAT of lean [23, 28, 87] and diabetes-susceptible mice (KKay) [26]. In contrast, the administration of antioxidants or the conditional ablation of CCR2 was sufficient to revert these metabolic changes [18, 28]. This and similar evidence suggests that the macrophage-dependant inflammation/ROS production is implicated in the development of insulin resistance in adipose tissue of PM2.5-exposed animals [23, 88] (Fig. 2).
Adipocyte-macrophage interplay in adipose tissue under PM2.5 exposure. A tight adipocyte-macrophage interplay is instrumental for the development of WAT and BAT metabolic dysfunction. Macrophage- and adipocyte-released pro-inflammatory cytokines stimulate the recruitment of circulating monocytes. Activated macrophages enhance ROS production and inflammatory response in WAT, increasing adipocyte stress. Stressed/apoptotic adipocytes release pro-inflammatory mediators, sparking a vicious cycle resulting in the development of adipose tissue dysfunction. CCL2, C–C motif chemokine ligand 2; FFAs, fatty free acids; IL-6, interleukin 6; O2−, superoxide anion; TNFα, tumoral necrosis factor
The accumulation of macrophages is a recognized mark of adipose tissue inflammation and metabolic dysfunction [30]. In animal models, PM2.5 exposure was shown to upregulate vascular adhesion molecules and augmented monocytes in mesenteric blood vessels of both HFD-fed and lean mice [12, 18, 19]. Also, an increased number of activated macrophages in vWAT and BAT is reported by numerous investigations [12, 18, 21, 25,26,27, 71, 88].
The M1-polarization of macrophages is another feature indicating the inflammatory switch of WAT in PM2.5-exposed animals [12, 19]. M1 macrophages accumulate in vWAT of obese animals and generate pro-inflammatory/pro-fibrotic signals [89]. On the contrary, M2 macrophages buffer fluctuations of energy substrates and improve insulin sensitivity [30, 89]. Early findings suggest the M1-shift under PM2.5 exposure [12, 19, 90]. For example, in vitro studies showed that high concentrations of PM2.5, through ROS-dependent mechanisms, drive the M1-polarization of macrophages in WAT [90]; in addition, PM2.5 exposure was shown to suppress the anti-inflammatory IL-10 and the M2-specific markers–macrophage-galactose-type lectin and galactose-N-acetyl-galactosamine–specific lectin–in lean [19] and obese animals [12].
PM2.5 stimulates adipocyte hypertrophy and WAT mass expansion
Adipocyte hypertrophy and WAT mass expansion have been observed in both lean [19, 25, 28, 71, 91] and obese rodents [12, 25] undergoing chronic PM2.5 exposure. Observational data in humans substantiate this finding by showing that chronic PM exposure is associated with higher abdominal adiposity [13, 92]. Interestingly, in rodent studies, PM2.5-induced WAT mass expansion occurs independently of changes in food intake [25, 28].
Hypertrophy can cause white adipocyte stress and dysfunction [30, 34]. The excessive adipocyte enlargement induces the compression of blood vessels, causing the development of ischemic areas in the context of WAT [34, 93]; chronic hypoxia stimulates the activation of apoptosis and stress/inflammatory pathways, promoting the shifting of WAT toward a dysfunctional phenotype [30, 34, 94] (Figs. 1, 2, and 3).
Model showing the potential mechanisms responsible for adipose tissue dysfunction under PM2.5 exposure. PM2.5-induced alveolar inflammation is responsible for the release of pro-inflammatory mediators into circulation. PM2.5 also alters microbiota composition and compromises epithelial integrity, allowing the leakage of pro-inflammatory molecules. Circulating cytokines, LPS, and other byproducts fuel inflammation and insulin resistance in WAT and stimulate the whitening of brown adipocytes. PM2.5-induced hypothalamic inflammation contributes to increase inflammation and insulin resistance in WAT. CCL2, C–C motif chemokine ligand 2; ICAM, intercellular adhesion molecule 1; LPS, lipopolysaccharide FFAs, free fatty acids. IL-6, interleukin 6; IL-1β, interleukin 1β; O2−, superoxide anion; OxFFAs, oxidized free fatty acids; OxPLs, oxidized phospholipids; PM, particulate matter; TLR, Toll-like receptor. TNFα, tumoral necrosis factor
Although the underlying mechanisms are unclear, early studies suggest that chronic exposure to PM2.5 enhances adipo- and lipogenesis in WAT [28, 71]. In PM2.5- instilled mice, adiposyte hypertropy and WAT expansion were associated with the upregulation of the pro-adipogenic factors – peroxisome proliferator-activated receptor (PPAR)γ – and – cAMP response element-binding protein (CREB/P)α – [28]. In addition, a significant upregulation of key-enzymes in the synthesis of fatty acid (acetyl-CoA carboxylase, ACC) and TGs synthesis (diglyceride acyltransferase-2, DGAT2) was reported in WAT of PM2.5-exposed mice [71]. A decrease in energy expenditure, resulting from hypothalamic dysfunction and BAT whitening, can also account for the augmented TGs storage in white adipocytes [20, 21, 25, 26, 71, 95].
On the other hand, adipocyte hypertrophy, in the absence of an energy surplus, suggests the existence of maladaptive mechanisms enhancing TGs accumulation [34]. ER and mitochondrial dysfunction can impair glucose/lipid oxidation, stimulating TGs storage and adipocyte hypertrophy independently from changes in energy intake/expenditure [34, 42, 62, 67]. In PM2.5 exposed rodents, for instance, the impairment in mitochondrial biogenesis was associated with WAT mass expansion and adipocyte hypertrophy [25, 28]. Likewise, ER stress was associated with the upregulation of lipogenic markers in WAT in exposed models [71].
One final aspect is that oxidative stress/inflammation can directly inhibit the oxidation of substrates in adipocytes, stimulating TGs storage and hypertrophy [96] (Fig. 2). Supporting this insight, the deletion of the antioxidant transcription factor Nrf-2 was found to exacerbate adipocyte hypertrophy upon PM2.5 intratracheal instillation [91]; conversely, the administration of a concentrated antioxidant (e.g., hydroxytyrosol) efficiently reverted adipocytes hypertrophy and vWAT mass expansion [28].
PM2.5 exposure induces the whitening of brown adipocytes
Growing evidence reveals that BAT loss and the whitening of brown adipocytes occur in animals chronically exposed to PM2.5 [23]. Brown adipocytes of PM2.5-exposed rodents display a higher number of lipid droplets than filtered-air-exposed controls [17], which indicates an initial phase of whitening. PM2.5 exposure reduced mitochondrial size and number in BAT of PM2.5-exposed [23, 65, 66]. The UCP-1 expression was found to decrease in BAT of PM2.5-exposed KKay [26], ApoE-/- [65] and lean mice [17, 23, 28]. Also, chronic exposure to PM2.5 suppressed PGC-1α and glucose uptake in BAT [20, 21, 23], while stimulating the expression of markers of whitening (e.g., homeobox-C9 and insulin-like growth factor-binding protein-3) [23, 65].
Persistent PM2.5 inhalation induces the upregulation of p38, TNFα, and IL-6 [26] and the accumulation of macrophages in BAT [21]. Interestingly, macrophage accumulation was associated with the impairment of glucose uptake, indicating that BAT metabolic dysfunction might be dependent upon inflammation. This occurrence is also suggested by evidence in non-exposed models; macrophages infiltration in WAT is demonstrated to prevent the browning of adipocyte precursors [97], and the overexpression of TNFα and CCL2 in BAT is associated with the downregulation of UCP-1 and PGC-1α [98]. In contrast, the inhibition of p38 and JNK promotes the browning of white adipocytes [79, 80]. In addition, the suppression of WAT browning is probably mediated by the activation of the protein apoptosis signal-regulating kinase 1 (ASK1), a JNK inducer (Fig. 1) [99]. Notably, ASK1 represents a key player in the induction of inflammatory response in alveolar cells upon PM2.5 exposure [54].
Role of other tissues in WAT and BAT dysfunction under PM2.5 exposure
In humans and animals, PM2.5 exerts its negative effects by perturbing cell and tissue homeostasis. In animal models, 2-μm particles have been shown to reach parenchymatous organs such as the kidney, liver, and spleen, likely transported by alveolar macrophages [53]. Therefore, PM2.5 may reach the adipose tissue milieu and exert an in loco toxic effect.
In addition, existing evidence suggests that pro-inflammatory mediators and other biomolecules released by inflamed tissues including the lungs, the GI tract, and the hypothalamus may be responsible for WAT and BAT dysfunction, in PM2.5-exposed models (Figs. 3 and 4).
Synoptic scheme showing the potential influence of adipose tissue dysfunction on systemic health under PM2.5. Lung- and gut-derived pro-inflammatory mediators and other biomolecules trigger WAT inflammation and metabolic dysfunction. The development of hypothalamic inflammation increases WAT inflammatory response and insulin resistance. Soluble mediators secreted by dysfunctional WAT worsen whole-body metabolic homeostasis and affect the functionality of central/peripheral tissues. BAT, brown adipose tissue; CCL2, C–C motif chemokine ligand 2; IL-6, interleukin 6; IL-12, interleukin 12; OxFFAs, oxidized free fatty acids; OxPLs, oxidized phospholipids; PM, particulate matter; SNS, sympathetic nervous system; TNFα, tumoral necrosis factor
Alveolar-derived pro-inflammatory mediators may affect BAT and WAT
The activation of alveolar macrophages, following PM2.5 inhalation, is responsible for the systemic increase of IL-1β, IL-6, TNFα, and interferon-γ [9, 10, 12, 100]. In experimental models, both the treatment with antioxidants and the induction of SOD expression in the lungs efficaciously inhibited inflammation in periaortic adipose tissue and mitigated insulin resistance in endothelial cells [101, 102], suggesting that lungs inflammation can impair the functionality of distant tissues.
Under chronic PM2.5 exposure, lung-released inflammatory mediators can affect adipose tissue metabolic and inflammatory homeostasis. IL-6 was demonstrated to impair insulin signaling and GLUT4 in pre-adipocytes [103]. In mature adipocytes, TNFα inhibited IRS-1 and stimulated IL-6 expression [104, 105]. TNFα also enhances ROS production [96, 106] and suppresses mitochondrial biogenesis and brown adipocytes growth [107, 108]. IL-1β activates NF-κB and inhibits IRS-1 and pAKT, in WAT [109, 110]. Finally, IL-6 and IL-1β can suppress BAT thermogenetic activity and the browning of white adipocytes [111,112,113].
Other organic byproducts derived from the interaction airways-PM2.5 may enhance inflammation in adipose tissue. For example, PM-carried endotoxins as well as ROS and organic byproducts released into circulation trigger WAT inflammation by activating the toll-like receptor (TLR) downstream cascade [72, 88, 114] (Figs. 1 and 2).
Alteration of the gut-microbiota lining can induce WAT and BAT dysfunction
The lower GI tract can be directly exposed to PM, following the consumption of foods carrying high levels of particles [51]. Evidence suggests that up to 1014 particles per day can be ingested by consuming a typical western diet, with an overall GI absorption of about 1% [51, 115]. Besides, the muco-ciliary clearance in the upper airways redirects inhaled PM2.5 toward the GI tract [116]. Since PM2.5 is less readily absorbed [51], it migrates as far as the lower gut [117], interfering with gut-microbiota homoeostasis.
The loss of integrity of colonocytes-microbiota lining represents a potential trigger for WAT dysfunction [118, 119]. Indeed, the leakage of intraluminal LPS, oxidized FFAs, and other pro-inflammatory mediators stimulates adipogenesis and WAT inflammation [96, 106, 118, 120,121,122,123,124]. In addition, gut-derived LPS impairs BAT thermogenic activity by downregulating UCP-1 and the β3-adrenergic signaling [125,126,127]. On the contrary, the inhibition of mucosal inflammation in the gut is followed by decreased inflammation and insulin resistance in WAT [128].
In experimental models, PM2.5 exposure was shown to negatively influence gut-microbiota homeostasis [116, 129]. PM2.5 induced a switch in the gut microbiota toward a pro-inflammatory phenotype and augmented the proportion of oxidized FFAs within the gut lumen [130,131,132]. In mice treated with oral gavage of a PM2.5 solution, gut epithelial cells exhibited molecular and morphologic features of dysfunction and death [117]. Also, PM2.5 exposure worsened gut permeability by altering the expression of thigh-junctions and by increasing inflammation of the mucosal lining [117, 132,133,134] (Figs. 2 and 3). Noteworthy, in PM2.5 intratracheal-instilled mice, the decrease in gut-microbiota diversity was correlated with white adipocytes hypertrophy and the suppression of UCP-1 in BAT [28].
Hypothalamic inflammation is associated with insulin resistance and inflammation in WAT
The hypothalamus is a brain structure critical for the integration of multiple peripheral signals to ensure metabolic flexibility and systemic homeostasis. In particular, the mediobasal hypothalamus directly modulates lipogenesis, substrate oxidation and insulin sensitivity of WAT [135, 136].
PM2.5 could affect brain functionality by (i) upregulating circulating pro-inflammatory mediators [137]; (ii) inducing inflammation of the olfactory bulb [137]; and (iii) altering gut microbiota ecosystem and the gut-brain crosstalk [137, 138].
PM2.5 exposure is followed by an intense microglia activation and increased expression of the inhibitor of nuclear factor kappa-B kinase subunit-β (IKKβ), TNFα, and IL-6 in the hypothalamus [139,140,141]. PM2.5 was also shown to upregulate NF-κB and the expression of pro-inflammatory genes in the paraventricular nucleus [141], a region involved in the control of energy balance and sympathetic activation. Interestingly, this neuro-inflammatory setting was accompanied by the accumulation of activated macrophages and the suppression of insulin signaling in vWAT [139]. Of note, either the blockage [139] or the ablation [27] of IKKβ in the hypothalamus effectively prevented macrophages accumulation, the expression of pro-inflammatory mediators, and insulin resistance in vWAT. Altogether, these findings strongly suggest that WAT dysfunction, under PM2.5, could be driven by hypothalamic inflammation (Fig. 3) [139,140,141,142,143,144,145].
Conclusion and future directions
Current animal studies demonstrate that PM2.5 exposure significantly increases inflammation in both WAT and BAT. Mitochondrial impairment, insulin resistance, and the whitening of brown adipocytes indicate the development of metabolic dysfunction.
While the underlying mechanisms are not fully elucidated, PM2.5-driven alterations in the lungs, the gut, and the hypothalamus appear to play an important role in driving inflammation and dysmetabolism in both WAT and BAT.
Noteworthy, the perturbation of adipose tissue homeostasis, under PM2.5 exposure, may worsen systemic cardio-metabolic health and the functionality of central/peripheral organs (Fig. 4).
Further investigations should be aimed to (i) investigate the accumulation of PM2.5 in adipose tissue and mechanisms of damage in adipocytes; (ii) characterize the activation of lipolysis/lipogenesis as well as the release of adipose tissue-specific mediators (adiponectin, FFAs, diacylglycerols, ceramides); and (iii) estimate the effect of adipose tissue dysfunction on gluco-metabolic balance in exposed models.
Literature search methods
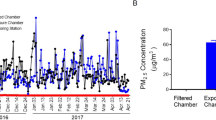
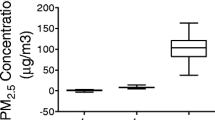
The research has been carried out on Medline, Scopus and Embase by restricting the language to English. The search strategy was assessed by alternatively combining the keywords “adipose tissue,” “adipocyte,” “metabolism,” “obesity” with “PM,” “fine particulate matter,” and “air pollution.” Data strictly pertaining to experimental evidence investigating the effect of fine particulate matter (PM; 2.5 μm, in diameter) on WAT and BAT have been retrieved. In order to describe the pathophysiological mechanisms underlying BAT and WAT dysfunction, we have restricted our research to controlled studies on animals undergoing direct exposure in a confined chamber or intratracheal instillation (a validated method to replicate airborne PM exposure in animal models) [146] of PM2.5.
Availability of data and material
Not applicable.
Code availability
Not applicable.
Change history
27 April 2022
A Correction to this paper has been published: https://doi.org/10.1007/s00109-022-02200-8
Abbreviations
- ACC:
-
Acetyl-CoA Carboxylase
- AKT:
-
Protein kinase B
- AMPK:
-
AMP-activated protein kinase
- ASK1:
-
Apoptosis signal-regulating kinase 1
- BAT:
-
Brown adipose tissue
- CCL2:
-
C-C motif chemokine ligand 2
- CCR-2:
-
C-C chemokine receptor type 2
- CREB/Pα:
-
CAMP response element-binding protein
- DGAT2:
-
Diglyceride acyltransferase-2
- ER:
-
Endoplasmic reticulum
- FFAs:
-
Fatty free acids
- GI:
-
Gastrointestinal
- GLUT4:
-
Glucose transporter 4
- BiP:
-
Binding immunoglobulin protein
- HFD:
-
High fat diet
- HSP72:
-
Heat shock protein 70 kilodaltons
- IKK:
-
Inhibitor of nuclear factor kappa-B kinase subunit-β
- IL-1β:
-
Interleukin 1 beta
- IL-10:
-
Interleukin 10
- IL-6:
-
Interleukin 6
- JNK:
-
C-Jun N-terminal kinase
- LPS:
-
Lipopolysaccharide
- NF-κB:
-
Nuclear factor kappa-light-chain-enhancer of activated B cells
- Nrf-2:
-
Nuclear factor erythroid 2-related factor 2
- OxPLs:
-
Oxidized phospholipids
- p38MAPK:
-
P38 Mitogen-activated protein kinases
- PAHs:
-
Polycyclic aromatic hydrocarbons
- PGC-1α:
-
Peroxisome proliferator-activated receptor gamma coactivator 1
- PM:
-
Particulate matter
- PPARγ :
-
Peroxisome proliferator-activated receptor
- ROS:
-
Reactive oxygen species
- SOD:
-
Superoxide dismutase
- TGs:
-
Triglycerides
- TLR:
-
Toll-like receptor
- TNF:
-
Tumor necrosis factor
- UCP:
-
Uncoupling protein
- UPR:
-
Unfolded protein response
- WAT:
-
White adipose tissue
References
Øvrevik J, Refsnes M, Låg M, Holme JA, Schwarze PE (2015) Activation of proinflammatory responses in cells of the airway mucosa by particulate matter: oxidant- and non-oxidant-mediated triggering mechanisms. Biomolecules 5:1399–1440
Pearson JF, Bachireddy C, Shyamprasad S, Goldfine AB, Brownstein JS (2010) Association between fine particulate matter and diabetes prevalence in the U.S. Diabetes Care 33:2196–2201
Pope CA, Ezzati M, Dockery DW (2009) Fine-particulate air pollution and life expectancy in the United States. N Engl J Med 360:376–386
Alderete TL, Habre R, Toledo-Corral CM, Berhane K, Chen Z, Lurmann FW, Weigensberg MJ, Goran MI, Gilliland FD (2017) Longitudinal associations between ambient air pollution with insulin sensitivity β-cell unction and adiposity in Los Angeles Latino Children. Diabetes 66:1789–1796
Chen JC, Schwartz J (2008) Metabolic syndrome and inflammatory responses to long-term particulate air pollutants. Environ Health Perspect 116:612–617
Lao XQ, Guo C, Chang LY et al (2019) Long-term exposure to ambient fine particulate matter (PM 2.5) and incident type 2 diabetes: a longitudinal cohort study. Diabetologia 62:759–769
He D, Wu S, Zhao H, Qiu H, Fu Y, Li X, He Y (2017) Association between particulate matter 2.5 and diabetes mellitus: a meta-analysis of cohort studies. J Diabetes Investig 8:687–696
Weinmayr G, Hennig F, Fuks K, Nonnemacher M, Jakobs H, Möhlenkamp S, Erbel R, Jöckel KH, Hoffmann B, Moebus S (2015) Long-term exposure to fine particulate matter and incidence of type 2 diabetes mellitus in a cohort study: effects of total and traffic-specific air pollution. Environ Health 14:53
Kido T, Tamagawa E, Bai N et al (2011) Particulate matter induces translocation of IL-6 from the lung to the systemic circulation. Am J Respir Cell Mol Biol 44:197–204
Tsai DH, Amyai N, Marques-Vidal P, Wang JL, Riediker M, Mooser V, Paccaud F, Waeber G, Vollenweider P, Bochud M (2012) Effects of particulate matter on inflammatory markers in the general adult population. Part Fibre Toxicol 9:24
Tsai DH, Riediker M, Berchet A, Paccaud F, Waeber G, Vollenweider P, Bochud M (2019) Effects of short- and long-term exposures to particulate matter on inflammatory marker levels in the general population. Environ Sci Pollut Res 26:19697–19704
Sun Q, Yue P, Deiuliis JA et al (2009) Ambient air pollution exaggerates adipose inflammation and insulin resistance in a mouse model of diet-induced obesity. Circulation 119:538–546
Guo Q, Xue T, Jia C, Wang B, Cao S, Zhao X, Zhang Q, Zhao L, Zhang JJ, Duan X (2020) Association between exposure to fine particulate matter and obesity in children: a national representative cross-sectional study in China. Environ Int 143:105950
Kim HJ, Park JH, Min JY, Min KB, Seo YS, Yun JM, Kwon H, Kim JI, Cho B (2017) Abdominal adiposity intensifies the negative effects of ambient air pollution on lung function in Korean men. Int J Obes 41:1218–1223
Jeong SM, Park JH, Kim HJ, Kwon H, Hwang SE (2020) Effects of abdominal obesity on the association between air pollution and kidney function. Int J Obes 44:1568–1576
Zhao Y, Qian Z, Wang J, Vaughn MG, Liu YQ, Ren WH, Dong GH (2013) Does obesity amplify the association between ambient air pollution and increased blood pressure and hypertension in adults? Findings from the 33 Communities Chinese Health Study. Int J Cardiol 168:e148–e150
Song Y, Qi Z, Zhang Y, Wei J, Liao X, Li R, Dong C, Zhu L, Yang Z, Cai Z (2020) Effects of exposure to ambient fine particulate matter on the heart of diet-induced obesity mouse model. Sci Total Environ 732:139304
Liu C, Xu X, Bai Y et al (2014) Air pollution-mediated susceptibility to inflammation and insulin resistance: Influence of CCR2 pathways in mice. Environ Health Perspect 122:17–26
Xu X, Yavar Z, Verdin M et al (2010) Effect of early particulate air pollution exposure on obesity in mice: Role of p47phox. Arterioscler Thromb Vasc Biol 30:2518–2527
Rajagopalan S, Park B, Palanivel R et al (2020) Metabolic effects of air pollution exposure and reversibility. J Clin Invest 130:6034–6040
Palanivel R, Vinayachandran V, Biswal S et al (2020) Exposure to air pollution disrupts circadian rhythm through alterations in chromatin dynamics. iScience 23:101728
Sun Q, Wang A, Jin X et al (2005) Long-term air pollution exposure and acceleration of atherosclerosis and vascular inflammation in an animal model. J Am Med Assoc 294:3003–3010
Xu X, Liu C, Xu Z, Tzan K, Zhong M, Wang A, Lippmann M, Chen LC, Rajagopalan S, Sun Q (2011) Long-term exposure to ambient fine particulate pollution induces insulin resistance and mitochondrial alteration in adipose tissue. Toxicol Sci 124:88–98
Wang Y, Li R, Chen R et al (2020) Ambient fine particulate matter exposure perturbed circadian rhythm and oscillations of lipid metabolism in adipose tissues. Chemosphere 251:126392
Pan K, Jiang S, Du X et al (2019) AMPK activation attenuates inflammatory response to reduce ambient PM 2.5 -induced metabolic disorders in healthy and diabetic mice. Ecotoxicol Environ Saf 179:290–300
Liu C, Bai Y, Xu X et al (2014) Exaggerated effects of particulate matter air pollution in genetic type II diabetes mellitus. Part Fibre Toxicol 11:27
Chen M, Qin X, Qiu L, Chen S, Zhou H, Xu Y, Hu Z, Zhang Y, Cao Q, Ying Z (2018) Concentrated ambient PM2.5 -induced inflammation and endothelial dysfunction in a murine model of neural IKK2 deficiency. Environ Health Perspect 126:027003
Wang N, Ma Y, Liu Z, Liu L, Yang K, Wei Y, Liu Y, Chen X, Sun X, Wen D (2019) Hydroxytyrosol prevents PM2.5-induced adiposity and insulin resistance by restraining oxidative stress related NF-κB pathway and modulation of gut microbiota in a murine model. Free Radic Biol Med 141:393–407
Maurizi G, Petäistö T, Maurizi A, Della Guardia L (2018) Key-genes regulating the liposecretion process of mature adipocytes. J Cell Physiol 233:3784–3793
Maurizi G, Della Guardia L, Maurizi A, Poloni A (2018) Adipocytes properties and crosstalk with immune system in obesity-related inflammation. J Cell Physiol 233:88–97
Maurizi G, Babini L, Della Guardia L (2018) Potential role of microRNAs in the regulation of adipocytes liposecretion and adipose tissue physiology. J Cell Physiol 233:9077–9086
Kusminski CM, Bickel PE, Scherer PE (2016) Targeting adipose tissue in the treatment of obesity-associated diabetes. Nat Rev Drug Discov 15:639–660
Boden G (2011) Obesity insulin resistance and free fatty acids. Curr Opin Endocrinol Diabetes Obes 18:139–143
Giordano A, Frontini A, Cinti S (2016) Convertible visceral fat as a therapeutic target to curb obesity. Nat Rev Drug Discov 15:405–424
Della Guardia L, Codella R (2021) Exercise tolls the bell for key mediators of low-grade inflammation in dysmetabolic conditions. Cytokine Growth Factor Rev 62:83–93
Guilherme A, Virbasius JV, Puri V, Czech MP (2008) Adipocyte dysfunctions linking obesity to insulin resistance and type 2 diabetes. Nat Rev Mol Cell Biol 9:367–377
Han MS, White A, Perry RJ, Camporez JP, Hidalgo J, Shulman GI, Davis RJ (2020) Regulation of adipose tissue inflammation by interleukin 6. Proc Natl Acad Sci USA 117:2751–2760
Kozak LP, Koza RA, Anunciado-Koza R (2010) Brown fat thermogenesis and body weight regulation in mice: Relevance to humans. Int J Obes 34:S23–S27
Chondronikola M, Volpi E, Børsheim E et al (2014) Brown adipose tissue improves whole-body glucose homeostasis and insulin sensitivity in humans. Diabetes 63:4089–4099
Severinsen MCK, Schéele C, Pedersen BK (2020) Exercise and browning of white adipose tissue – a translational perspective. Curr Opin Pharmacol 52:18–24
Lapa C, Arias-Loza P, Hayakawa N, Wakabayashi H, Werner RA, Chen X, Shinaji T, Herrmann K, Pelzer T, Higuchi T (2017) Whitening and impaired glucose utilization of brown adipose tissue in a rat model of type 2 diabetes mellitus. Sci Rep 7:16795
Kotzbeck P, Giordano A, Mondini E et al (2018) Brown adipose tissue whitening leads to brown adipocyte death and adipose tissue inflammation. J Lipid Res 59:784–794
Gali NK, Yang F, Jiang SY, Chan KL, Sun L, Ho KF, Ning Z (2015) Spatial and seasonal heterogeneity of atmospheric particles induced reactive oxygen species in urban areas and the role of water-soluble metals. Environ Pollut 198:86–96
Dong J, Chi Y, Ephraim A, Nzihou A, Millán LMR (2020) Particulate matter. In: Nzihou A (ed) Handbook on Characterization of Biomass Biowaste and Related By-products. Springer, Cham. https://doi.org/10.1007/978-3-030-35020-8_14
Liu L, Urch B, Poon R et al (2015) Effects of ambient coarse fine and ultrafine particles and their biological constituents on systemic biomarkers: a controlled human exposure study. Environ Health Perspect 123:534–540
Champion JA, Mitragotri S (2006) Role of target geometry in phagocytosis. Proc Natl Acad Sci USA 103:4930–4934
Nelin TD, Joseph AM, Gorr MW, Wold LE (2012) Direct and indirect effects of particulate matter on the cardiovascular system. Toxicol Lett 208:293–299
An Z, Jin Y, Li J, Li W, Wu W (2018) Impact of particulate air pollution on cardiovascular health. Curr Allergy Asthma Rep 18:15
Shimada A, Kawamura N, Okajima M, Kaewamatawong T, Inoue H, Morita T (2006) Translocation pathway of the intratracheally instilled ultrafine particles from the lung into the blood circulation in the mouse. Toxicol Pathol 34:949–957
Su R, Jin X, Li H, Huang L, Li Z (2020) The mechanisms of PM2.5 and its main components penetrate into HUVEC cells and effects on cell organelles. Chemosphere 241:125127
Lomer MCE, Hutchinson C, Volkert S, Greenfield SM, Catterall A, Thompson RPH, Powell JJ (2004) Dietary sources of inorganic microparticles and their intake in healthy subjects and patients with Crohn’s disease. Br J Nutr 92:947–955
Chin MT (2015) Basic mechanisms for adverse cardiovascular events associated with air pollution. Heart 101:253–256
Furuyama A, Kanno S, Kobayashi T, Hirano S (2009) Extrapulmonary translocation of intratracheally instilled fine and ultrafine particles via direct and alveolar macrophage-associated routes. Arch Toxicol 83:429–437
Soberanes S, Urich D, Baker CM et al (2009) Mitochondrial complex III-generated oxidants activate ASK1 and JNK to induce alveolar epithelial cell death following exposure to particulate matter air pollution. J Biol Chem 284:2176–2186
Costa Beber LC, da Silva MOAF, dos Santos AB, Mai AS, Goettems-Fiorin PB, Frizzo MN, Hirsch GE, Ludwig MS, Heck TG (2020) The association of subchronic exposure to low concentration of PM2.5 and high-fat diet potentiates glucose intolerance development by impairing adipose tissue antioxidant defense and eHSP72 levels. Environ Sci Pollut Res 27:32006–32016
Gasparotto J, Chaves PR, da Boit MK et al (2018) Obese rats are more vulnerable to inflammation, genotoxicity and oxidative stress induced by coal dust inhalation than non-obese rats. Ecotoxicol Environ Saf 165:44–51
Costa-Beber LC, Goettems-Fiorin PB, dos Santos JB, Friske PT, Frizzo MN, Heck TG, Hirsch GE, Ludwig MS (2021) Ovariectomy enhances female rats’ susceptibility to metabolic oxidative, and heat shock response effects induced by a high-fat diet and fine particulate matter. Exp Gerontol 145:111215
Ogborn DI, McKay BR, Crane JD, Parise G, Tarnopolsky MA (2014) The unfolded protein response is triggered following a single, unaccustomed resistance-exercise bout. Am J Physiol Regul Integr Comp Physiol 307:R664–R669
Hu F, Liu F (2011) Mitochondrial stress: a bridge between mitochondrial dysfunction and metabolic diseases? Cell Signal 23:1528–1533
Periasamy M, Maurya SK, Sahoo SK, Singh S, Reis FCG, Bal NC (2017) Role of SERCA pump in muscle thermogenesis and metabolism. Compr Physiol 7(3):879–890
de Mello AH, Costa AB, Engel JDG, Rezin GT (2018) Mitochondrial dysfunction in obesity. Life Sci 192:26–32
Kusminski CM, Scherer PE (2012) Mitochondrial dysfunction in white adipose tissue. Trends Endocrinol Metab 23:435–443
Gao CL, Zhu C, Zhao YP, Chen XH, Ji CB, Zhang CM, Zhu JG, Xia ZK, Tong ML, Guo XR (2010) Mitochondrial dysfunction is induced by high levels of glucose and free fatty acids in 3T3-L1 adipocytes. Mol Cell Endocrinol 320:25–33
Daiber A, Kuntic M, Hahad O, Delogu LG, Rohrbach S, Di Lisa F, Schulz R, Münzel T (2020) Effects of air pollution particles (ultrafine and fine particulate matter) on mitochondrial function and oxidative stress – Implications for cardiovascular and neurodegenerative diseases. Arch Biochem Biophys 696:108662
Xu Z, Xu X, Zhong M et al (2011) Ambient particulate air pollution induces oxidative stress and alterations of mitochondria and gene expression in brown and white adipose tissues. Part Fibre Toxicol 8:20
Xu X, Rao X, Wang TY et al (2012) Effect of co-exposure to nickel and particulate matter on insulin resistance and mitochondrial dysfunction in a mouse model. Part Fibre Toxicol 9:40
Rosen ED, Spiegelman BM (2006) Adipocytes as regulators of energy balance and glucose homeostasis. Nature 444:847–853
Zhang K, Kaufman RJ (2008) From endoplasmic-reticulum stress to the inflammatory response. Nature 454:455–462
Han J, Kaufman RJ (2014) Measurement of the unfolded protein response to investigate its role in adipogenesis and obesity. Methods Enzymol 538:135–150
Hentilä J, Ahtiainen JP, Paulsen G, Raastad T, Häkkinen K, Mero AA, Hulmi JJ (2018) Autophagy is induced by resistance exercise in young men but unfolded protein response is induced regardless of age. Acta Physiol 224:e13069
Mendez R, Zheng Z, Fan Z, Rajagopalan S, Sun Q, Zhang K (2013) Exposure to fine airborne particulate matter induces macrophage infiltration, unfolded protein response and lipid deposition in white adipose tissue. Am J Transl Res 5:224–234
Yoda Y, Tamura K, Shima M (2017) Airborne endotoxin concentrations in indoor and outdoor particulate matter and their predictors in an urban city. Indoor Air 27:955–964
Solinas G, Becattini B (2017) JNK at the crossroad of obesity insulin resistance and cell stress response. Mol Metab 6:174–184
Vallerie SN, Hotamisligil GS (2010) The role of JNK proteins in metabolism. Sci Transl Med 2:60rv5
Zhang X, Xu A, Chung SK, Cresser JHB, Sweeney G, Wong RLC, Lin A, Lam KSL (2011) Selective inactivation of c-Jun NH2-terminal kinase in adipose tissue protects against diet-induced obesity and improves insulin sensitivity in both liver and skeletal muscle in mice. Diabetes 60:486–495
Zheng Z, Xu X, Zhang X et al (2013) Exposure to ambient particulate matter induces a NASH-like phenotype and impairs hepatic glucose metabolism in an animal model. J Hepatol 58:48–54
Zarubin T, Han J (2005) Activation and signaling of the p38 MAP kinase pathway. Cell Res 15:11–18
Hemi R, Yochananov Y, Barhod E, Kasher-Meron M, Karasik A, Tirosh A, Kanety H (2011) p38 mitogen-activated protein kinase-dependent transactivation of ErbB receptor family: a novel common mechanism for stress-induced IRS-1 serine phosphorylation and insulin resistance. Diabetes 60:1134–1145
Zhang S, Cao H, Li Y et al (2018) Metabolic benefits of inhibition of p38α in white adipose tissue in obesity. PLoS Biol 16:e2004225
Matesanz N, Nikolic I, Leiva M et al (2018) p38α blocks brown adipose tissue thermogenesis through p38δ inhibition. PLoS Biol 16:e2004455
Hassan L, Pecht T, Goldstein N, Haim Y, Kloog I, Yarza S, Sarov B, Novack V (2019) The effects of ambient particulate matter on human adipose tissue. J Toxicol Environ Heal Part A Curr Issues 82:564–576
Mihaylova MM, Shaw RJ (2011) The AMPK signalling pathway coordinates cell growth autophagy and metabolism. Nat Cell Biol 13:1016–1023
Soeder KJ, Snedden SK, Cao W, Della Rocca GJ, Daniel KW, Luttrell LM, Collins S (1999) The β3-adrenergic receptor activates mitogen-activated protein kinase in adipocytes through a G(i)-dependent mechanism. J Biol Chem 274:12017–12022
Long MH, Zhang C, Xu DQ, Fu WL, Gan XD, Li F, Wang Q, Xia WX (2020) PM2.5 aggravates diabetes via the systemically activated IL-6-mediated STAT3/SOCS3 pathway in rats’ liver. Env Pollut 256:113342
Guo S (2014) Insulin signaling resistance and metabolic syndrome: insights from mouse models into disease mechanisms. J Endocrinol 220:T1–T23
Osborn O, Olefsky JM (2012) The cellular and signaling networks linking the immune system and metabolism in disease. Nat Med 18:363–374
Liu C, Xu X, Bai Y, Zhong J, Wang A, Sun L, Kong L, Ying Z, Sun Q, Rajagopalan S (2017) Particulate Air pollution mediated effects on insulin resistance in mice are independent of CCR2. Part Fibre Toxicol 14:6
Kampfrath T, Maiseyeu A, Ying Z et al (2011) Chronic fine particulate matter exposure induces systemic vascular dysfunction via NADPH oxidase and TLR4 pathways. Circ Res 108:716–726
Oh DY, Morinaga H, Talukdar S, Bae EJ, Olefsky JM (2012) Increased macrophage migration into adipose tissue in obese mice. Diabetes 61:346–354
Zhao Q, Chen H, Yang T, Rui W, Liu F, Zhang F, Zhao Y, Ding W (2016) Direct effects of airborne PM2.5 exposure on macrophage polarizations. Biochim Biophys Acta Gen Subj 1860:2835–2843
Jiang M, Li D, Piao J et al (2020) Real-ambient exposure to air pollution exaggerates excessive growth of adipose tissue modulated by Nrf2 signal. Sci Total Environ 730:138652
An R, Ji M, Yan H, Guan C (2018) Impact of ambient air pollution on obesity: a systematic review. Int J Obes 42:1112–1126
Sun K, Tordjman J, Clément K, Scherer PE (2013) Fibrosis and adipose tissue dysfunction. Cell Metab 18:470–477
Lindhorst A, Raulien N, Wieghofer P, Eilers J, Rossi FMV, Bechmann I, Gericke M (2021) Adipocyte death triggers a pro-inflammatory response and induces metabolic activation of resident macrophages. Cell Death Dis 12:579
Campolim CM, Weissmann L, Ferreira CKO, Zordão OP, Dornellas APS, de Castro G, Zanotto TM, Boico VF, Quaresma PGF, Lima RPA et al (2020) Short-term exposure to air pollution (PM2.5) induces hypothalamic inflammation, and long-term leads to leptin resistance and obesity via Tlr4/Ikbke in mice. Sci Rep 10:10160
Lin Y, Berg AH, Iyengar P et al (2005) The hyperglycemia-induced inflammatory response in adipocytes: the role of reactive oxygen species. J Biol Chem 280:4617–4626
Estève D, Boulet N, Volat F et al (2015) Human white and brite adipogenesis is supported by msca1 and is impaired by immune cells. Stem Cells 33:1277–1291
Alcalá M, Calderon-Dominguez M, Bustos E, Ramos P, Casals N, Serra D, Viana M, Herrero L (2017) Increased inflammation oxidative stress and mitochondrial respiration in brown adipose tissue from obese mice. Sci Rep 7:16082
Lucchini FC, Wueest S, Challa TD, Item F, Modica S, Borsigova M, Haim Y, Wolfrum C, Rudich A, Konrad D (2020) ASK1 inhibits browning of white adipose tissue in obesity. Nat Commun 11:1642
Marchini T, Wolf D, Michel NA et al (2016) Acute exposure to air pollution particulate matter aggravates experimental myocardial infarction in mice by potentiating cytokine secretion from lung macrophages. Basic Res Cardiol 111:44
Haberzettl P, Jin L, Riggs DW, Zhao J, O’Toole TE, Conklin DJ (2021) Fine particulate matter air pollution and aortic perivascular adipose tissue: Oxidative stress leptin and vascular dysfunction. Physiol Rep 9:e14980
Haberzettl P, O’Toole TE, Bhatnagar A, Conklin DJ (2016) Exposure to fine particulate air pollution causes vascular insulin resistance by inducing pulmonary oxidative stress. Environ Health Perspect 124:1830–1839
Lagathu C, Bastard JP, Auclair M, Maachi M, Capeau J, Caron M (2003) Chronic interleukin-6 (IL-6) treatment increased IL-6 secretion and induced insulin resistance in adipocyte: prevention by rosiglitazone. Biochem Biophys Res Commun 311:372–379. https://doi.org/10.1016/j.bbrc.2003.10.013
Almuraikhy S, Kafienah W, Bashah M et al (2016) Interleukin-6 induces impairment in human subcutaneous adipogenesis in obesity-associated insulin resistance. Diabetologia 59:2406–2416
Rotter V, Nagaev I, Smith U (2003) Interleukin-6 (IL-6) Induces insulin resistance in 3T3-L1 adipocytes and is, like IL-8 and tumor necrosis factor-α, overexpressed in human fat cells from insulin-resistant subjects. J Biol Chem 278:45777–45784
Chen XH, Zhao YP, Xue M et al (2010) TNF-α induces mitochondrial dysfunction in 3T3-L1 adipocytes. Mol Cell Endocrinol 328:63–69
Houstis N, Rosen ED, Lander ES (2006) Reactive oxygen species have a causal role in multiple forms of insulin resistance. Nature 440:944–948
Valladares A, Álvarez AM, Ventura JJ, Roncero C, Benito M, Porras A (2000) p38 mitogen-activated protein kinase mediates tumor necrosis factor-α-induced apoptosis in rat fetal brown adipocytes. Endocrinology 141:4383–4395
Bing C (2015) Is interleukin-1β a culprit in macrophage-adipocyte crosstalk in obesity? Adipocyte 4:149–152
Gao D, Madi M, Ding C, Fok M, Steele T, Ford C, Hunter L, Bing C (2014) Interleukin-1β mediates macrophage-induced impairment of insulin signaling in human primary adipocytes. Am J Physiol Endocrinol Metab 307:E289–E304
van den Berg SM, van Dam AD, Rensen PCN, de Winther MPJ, Lutgens E (2017) Immune modulation of brown(ing) adipose tissue in obesity. Endocr Rev 38(1):46–68
García MDC, Pazos P, Lima LDC (2018) Regulation of energy expenditure and brown/beige thermogenic activity by interleukins: new roles for old actors. Int J Mol Sci 19:2569
Goto T, Naknukool S, Yoshitake R et al (2016) Proinflammatory cytokine interleukin-1β suppresses cold-induced thermogenesis in adipocytes. Cytokine 77:107–114
Behbod B, Urch B, Speck M et al (2013) Endotoxin in concentrated coarse and fine ambient particles induces acute systemic inflammation in controlled human exposures. Occup Environ Med 70:761–767
Lomer MCE, Thompson RPH, Powell JJ (2002) Fine and ultrafine particles of the diet: influence on the mucosal immune response and association with Crohn’s disease. Proc Nutr Soc 61:123–130
Möller W, Häußinger K, Winkler-Heil R, Stahlhofen W, Meyer T, Hofmann W, Heyder J (2004) Mucociliary and long-term particle clearance in the airways of healthy nonsmoker subjects. J Appl Physiol 97:2200–2206
Mutlu EA, Engen PA, Soberanes S et al (2011) Particulate matter air pollution causes oxidant-mediated increase in gut permeability in mice. Part Fibre Toxicol 8:19
Cheru L, Saylor CF, Lo J (2019) Gastrointestinal barrier breakdown and adipose tissue inflammation. Curr Obes Rep 8:165–174
Bleau C, Karelis AD, St-Pierre DH, Lamontagne L (2015) Crosstalk between intestinal microbiota, adipose tissue and skeletal muscle as an early event in systemic low-grade inflammation and the development of obesity and diabetes. Diabetes Metab Res Rev 31:545–561
Cani PD, Amar J, Iglesias MA et al (2007) Metabolic endotoxemia initiates obesity and insulin resistance. Diabetes 56:1761–1772
De La Serre CB, Ellis CL, Lee J, Hartman AL, Rutledge JC, Raybould HE (2010) Propensity to high-fat diet-induced obesity in rats is associated with changes in the gut microbiota and gut inflammation. Am J Physiol Gastrointest Liver Physiol 299(2):G440–G448
Hersoug LG, Møller P, Loft S (2018) Role of microbiota-derived lipopolysaccharide in adipose tissue inflammation, adipocyte size and pyroptosis during obesity. Nutr Res Rev 31:153–163
Lee BC, Lee J (2014) Cellular and molecular players in adipose tissue inflammation in the development of obesity-induced insulin resistance. Biochim Biophys Acta Mol Basis Dis 1842:446–462
Velloso LA, Folli F, Saad MJ (2015) TLR4 at the crossroads of nutrients gut microbiota and metabolic inflammation. Endocr Rev 36:245–271
Valladares A, Roncero C, Benito M, Porras A (2001) TNF-α inhibits UCP-1 expression in brown adipocytes via ERKs - opposite effect of p38MAPK. FEBS Lett 493:6–11
Nøhr MK, Bobba N, Richelsen B, Lund S, Pedersen SB (2017) Inflammation downregulates UCP1 expression in brown adipocytes potentially via SIRT1 and DBC1 interaction. Int J Mol Sci 18:1006
Okla M, Zaher W, Alfayez M, Chung S (2018) Inhibitory effects of Toll-like receptor 4 NLRP3 inflammasome and interleukin-1β on white adipocyte browning. Inflammation 41:626–642
Luck H, Tsai S, Chung J et al (2015) Regulation of obesity-related insulin resistance with gut anti-inflammatory agents. Cell Metab 21:527–542
Kish L, Hotte N, Kaplan GG et al (2013) Environmental particulate matter induces murine intestinal inflammatory responses and alters the gut microbiome. PLoS One 8:e62220
Wang W, Zhou J, Chen M, Huang X, Xie X, Li W, Cao Q, Kan H, Xu Y, Ying Z (2018) Exposure to concentrated ambient PM2.5 alters the composition of gut microbiota in a murine model. Part Fibre Toxicol 15:17
Liu Y, Wang T, Si B, Du H, Liu Y, Waqas A, Huang S, Zhao G, Chen S, Xu A (2021) Intratracheally instillated diesel PM2.5 significantly altered the structure and composition of indigenous murine gut microbiota. Ecotoxicol Environ Saf 210:111903
Feng J, Cavallero S, Hsiai T, Li R (2020) Impact of air pollution on intestinal redox lipidome and microbiome. Free Radic Biol Med 151:99–110
Baek KI, Qian Y, Chang CC, O’Donnell R, Soleimanian E, Sioutas C, Li R, Hsiai TK (2020) An embryonic zebrafish model to screen disruption of gut-vascular barrier upon exposure to ambient ultrafine particles. Toxics 8:107
Mutlu EA, Comba IY, Cho T et al (2018) Inhalational exposure to particulate matter air pollution alters the composition of the gut microbiome. Environ Pollut 240:817–830
Cavalcanti-de-Albuquerque JP, Bober J, Zimmer MR, Dietrich MO (2019) Regulation of substrate utilization and adiposity by Agrp neurons. Nat Commun 10:311
Steculorum SM, Ruud J, Karakasilioti I et al (2016) AgRP neurons control systemic insulin sensitivity via myostatin expression in brown adipose tissue. Cell 165:125–138
Shou Y, Huang Y, Zhu X, Liu C, Hu Y, Wang H (2019) A review of the possible associations between ambient PM2.5 exposures and the development of Alzheimer’s disease. Ecotoxicol Environ Saf 174:344–352
Zhu X, Ji X, Shou Y, Huang Y, Hu Y, Wang H (2020) Recent advances in understanding the mechanisms of PM2.5-mediated neurodegenerative diseases. Toxicol Lett 329:31–37
Liu C, Fonken LK, Wang A et al (2014) Central IKKβ inhibition prevents air pollution mediated peripheral inflammation and exaggeration of type II diabetes. Part Fibre Toxicol 11:53
Bai KJ, Chuang KJ, Chen CL, Jhan MK, Hsiao TC, Cheng TJ, Chang LT, Chang TY, Chuang HC (2019) Microglial activation and inflammation caused by traffic-related particulate matter. Chem Biol Interact 311:108762
Ying Z, Xu X, Bai Y et al (2014) Long-term exposure to concentrated ambient PM2.5 increases mouse blood pressure through abnormal activation of the sympathetic nervous system: a role for hypothalamic inflammation. Environ Health Perspect 122:79–86
Pan B, Chen M, Zhang X et al (2021) Hypothalamic-pituitary-adrenal axis mediates ambient PM2.5 exposure-induced pulmonary inflammation. Ecotoxicol Environ Saf 208:111464
Li H, Cai J, Chen R et al (2017) Particulate matter exposure and stress hormone levels: a randomized double-blind crossover trial of air purification. Circulation 136:618–627
Li R, Sun Q, Lam SM et al (2020) Sex-dependent effects of ambient PM2.5 pollution on insulin sensitivity and hepatic lipid metabolism in mice. Part Fibre Toxicol 17:14
MohanKumar SMJ, Campbell A, Block M, Veronesi B (2008) Particulate matter oxidative stress and neurotoxicity. Neurotoxicology 29:479–488
Driscoll KE, Costa DL, Hatch G, Henderson R, Oberdorster G, Salem H, Schlesinger RB (2000) Intratracheal instillation as an exposure technique for the evaluation of respiratory tract toxicity: uses and limitations. Toxicol Sci 55:24–35
Acknowledgments
We thank Adrien T Stanley and Claudia G Liberini for proofreading the manuscript.
Funding
Open access funding provided by Università degli Studi di Milano within the CRUI-CARE Agreement.
Author information
Authors and Affiliations
Contributions
All authors contributed toward this study. Lucio Della Guardia: conceptualization, data collection, and writing of the manuscript. Andrew C. Shin: supervision and editing of the manuscript. All authors read and approved the final version of the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
The original online version of this article was revised: The published article should be Open Access.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Della Guardia, L., Shin, A.C. White and brown adipose tissue functionality is impaired by fine particulate matter (PM2.5) exposure. J Mol Med 100, 665–676 (2022). https://doi.org/10.1007/s00109-022-02183-6
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00109-022-02183-6