Abstract
Purpose
The aim of this work was to determine predictive factors for gastroduodenal (GD) toxicity in hepatocellular carcinoma (HCC) patients who were treated with radiotherapy (RT).
Patients and methods
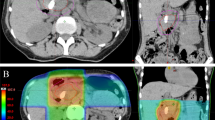
A total of 90 HCC patients who underwent esophagogastroduodenoscopy (EGD) before and after RT were enrolled. RT was delivered as 30–50 Gy (median 37.5 Gy) in 2–5 Gy (median 3.5 Gy) per fraction. All endoscopic findings were reviewed and GD toxicities related to RT were graded by the Common Toxicity Criteria for Adverse Events, version 3.0. The predictive factors for the ≥ grade 2 GD toxicity were investigated.
Results
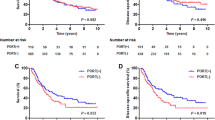
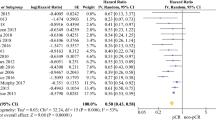
Endoscopic findings showed erosive gastritis in 14 patients (16 %), gastric ulcers in 8 patients (9 %), erosive duodenitis in 15 patients (17 %), and duodenal ulcers in 14 patients (16 %). Grade 2 toxicity developed in 19 patients (21 %) and grade 3 toxicity developed in 8 patients (9 %). V25 for stomach and V35 for duodenum (volume receiving a RT dose of more than x Gy) were the most predictive factors for ≥ grade 2 toxicity. The gastric toxicity rate at 6 months was 2.9 % for V25 ≤ 6.3 % and 57.1 % for V25 > 6.3 %. The duodenal toxicity rate at 6 months was 9.4 % for V35 ≤ 5.4 % and 45.9 % for V35 > 5.4 %. By multivariate analysis including the clinical factors, V25 for stomach and V35 for duodenum were the significant factors.
Conclusion
EGD revealed that GD toxicity is common following RT for HCC. V25 for the stomach and V35 for the duodenum were the significant factors to predict ≥ grade 2 GD toxicity.
Zusammenfassung
Ziel
Ziel der Studie war es, Vorhersagefaktoren für Magen-Darm-(GD-)Toxizität bei Patienten mit Leberzellkrebs (HCC) zu bestimmen, die eine Strahlenbehandlung (RT) erhalten hatten.
Patienten und Methoden
In die Studie wurden insgesamt 90 HCC-Patienten aufgenommen, die vor und nach einer RT einer Esophagogastroduodenoskopie (EGD) unterzogen wurden. Es wurden RT-Dosen zwischen 30–50 Gy (Median 37,5 Gy) in Einzeldosen zu je 2–5 Gy (Median 3,5 Gy) verabreicht. Alle endoskopischen Ergebnisse wurden überprüft und die GD-Toxizität in Bezug auf die RT wurde entsprechend den Kriterien der „Common Toxicity Criteria for Adverse Events Version 3.0“ eingestuft. Untersucht wurde die Vorhersagefaktoren für die GD-Toxizität ≥Stufe 2.
Ergebnisse
Die endoskopischen Befunde zeigten eine erosive Gastritis bei 14 Patienten (16 %), Magengeschwüre bei 8 Patienten (9 %), erosive Duodenitis bei 15 Patienten (17 %) und Duodenalgeschwüre bei 14 Patienten (16 %). Eine Stufe-2-Toxizität entwickelte sich bei 19 Patienten (21 %), eine Stufe-3-Toxizität bei 8 Patienten (9 %). V25 für den Magen und V35 für den Zwölffingerdarm hatten die höchsten Vorhersagefaktoren bei einer Toxizität ≥Stufe 2. Die Magentoxizitätsrate bei 6 Monaten betrug 2,9 % für V25 ≤ 6,3 % und 57,1 % für V25 > 6,3 %. Die Zwölffingerdarmtoxizitätsrate bei 6 Monaten war 9,4 % für V35 ≤ 5,4 % und 45,9 % für V35 > 5,4 %. Bei multivariaten Analysen inklusive klinischen Faktoren waren V25 für den Magen und V35 für den Zwölffingerdarm signifikante Faktoren.
Schlussfolgerung
Die EGD hat gezeigt, dass die GD-Toxizität nach einer RT für HCC verbreitet ist. V25 für den Magen und V35 für den Zwölffingerdarm waren signifikante Faktoren zur Vorhersage einer GD-Toxizität ≥Stufe 2.

Similar content being viewed by others
References
Chen LS, Lin HC, Hwang SJ et al (1996) Prevalence of gastric ulcer in cirrhotic patients and its relation to portal hypertension. J Gastroenterol Hepatol 11:59–64
Cheng SH, Lin YM, Chuang VP et al (1999) A pilot study of three-dimensional conformal radiotherapy in unresectable hepatocellular carcinoma. J Gastroenterol Hepatol 14:1025–1033
Chon YE, Seong J, Kim BK et al (2011) Gastroduodenal complications after concurrent chemoradiation therapy in patients with hepatocellular carcinoma: endoscopic findings and risk factors. Int J Radiat Oncol Biol Phys 81:1343–1351
Emami B, Lyman J, Brown A et al (1991) Tolerance of normal tissue to therapeutic irradiation. Int J Radiat Oncol Biol Phys 21:109–122
Geoffroy P, Duchateau A, Thiefin G et al (1987) Effects of propranolol and sucralfate on ethanol-induced gastric mucosal damage in chronic portal hypertensive rats. J Hepatol 5:162–166
Hosking SW, Kennedy HJ, Seddon I et al (1987) The role of propranolol in congestive gastropathy of portal hypertension. Hepatology 7:437–441
Huang J, Robertson JM, Ye H et al (2012) Dose-volume analysis of predictors for gastrointestinal toxicity after concurrent full-dose gemcitabine and radiotherapy for locally advanced pancreatic adenocarcinoma. Int J Radiat Oncol Biol Phys 83:1120–1125
Huang YJ, Hsu HC, Wang CY et al (2009) The treatment responses in cases of radiation therapy to portal vein thrombosis in advanced hepatocellular carcinoma. Int J Radiat Oncol Biol Phys 73:1155–1163
Kim DY, Park W, Lim DH et al (2005) Three-dimensional conformal radiotherapy for portal vein thrombosis of hepatocellular carcinoma. Cancer 103:2419–2426
Kim H, Lim do H, Paik SW et al (2009) Predictive factors of gastroduodenal toxicity in cirrhotic patients after three dimensional conformal radiotherapy for hepatocellular carcinoma. Radiother Oncol 93:302–306
Kitano S, Dolgor B (2000) Does portal hypertension contribute to the pathogenesis of gastric ulcer associated with liver cirrhosis? J Gastroenterol 35:79–86
Li B, Yu J, Wang L et al (2003) Study of local three-dimensional conformal radiotherapy combined with transcatheter arterial chemoembolization for patients with stage III hepatocellular carcinoma. Am J Clin Oncol 26:e92–e99
Milano MT, Chmura SJ, Garofalo MC et al (2004) Intensity-modulated radiotherapy in treatment of pancreatic and bile duct malignancies: toxicity and clinical outcome. Int J Radiat Oncol Biol Phys 59:445–453
Nakamura A, Shibuya K, Matsuo Y et al (2012) Analysis of dosimetric parameters associated with acute gastrointestinal toxicity and upper gastrointestinal bleeding in locally advanced pancreatic cancer patients treated with gemcitabine-based concurrent chemoradiotherapy. Int J Radiat Oncol Biol Phys 84:369–375
Oh D, Lim do H, Park HC et al (2010) Early three-dimensional conformal radiotherapy for patients with unresectable hepatocellular carcinoma after incomplete transcatheter arterial chemoembolization: a prospective evaluation of efficacy and toxicity. Am J Clin Oncol 33:370–375
Park HC, Seong J, Han KH et al (2002) Dose-response relationship in local radiotherapy for hepatocellular carcinoma. Int J Radiat Oncol Biol Phys 54:150–155
Seong J, Lee IJ, Shim SJ et al (2009) A multicenter retrospective cohort study of practice patterns and clinical outcome on radiotherapy for hepatocellular carcinoma in Korea. Liver Int 29:147–152
Siringo S, Burroughs AK, Bolondi L et al (1995) Peptic ulcer and its course in cirrhosis: an endoscopic and clinical prospective study. J Hepatol 22:633–641
Tokuuye K, Sumi M, Kagami Y et al (2000) Radiotherapy for hepatocellular carcinoma. Strahlenther Onkol 176:406–410
Yamada K, Izaki K, Sugimoto K et al (2003) Prospective trial of combined transcatheter arterial chemoembolization and three-dimensional conformal radiotherapy for portal vein tumor thrombus in patients with unresectable hepatocellular carcinoma. Int J Radiat Oncol Biol Phys 57:113–119
Yoon SM, Lim YS, Won HJ et al (2012) Radiotherapy plus transarterial chemoembolization for hepatocellular carcinoma invading the portal vein: long-term patient outcomes. Int J Radiat Oncol Biol Phys 82:2004–2011
Zamboglou C, Messmer MB, Becker G et al (2012) Stereotactic radiotherapy in the liver hilum. Basis for future studies. Strahlenther Onkol 188:35–41
Conflict of interest
On behalf of all authors, the corresponding author states that there are no conflicts of interest.
Author information
Authors and Affiliations
Corresponding author
Additional information
Hyunsik Yoon and Dongryul Oh contributed equally to the article.
Rights and permissions
About this article
Cite this article
Yoon, H., Oh, D., Park, H. et al. Predictive factors for gastroduodenal toxicity based on endoscopy following radiotherapy in patients with hepatocellular carcinoma. Strahlenther Onkol 189, 541–546 (2013). https://doi.org/10.1007/s00066-013-0343-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00066-013-0343-0