Abstract
Interferon-alpha (IFN-α) is a potent anti-viral cytokine, critical to the host immune response against viruses. IFN-α is first produced upon viral detection by pathogen recognition receptors. Following its expression, IFN-α embarks upon a complex downstream signalling cascade called the JAK/STAT pathway. This signalling pathway results in the expression of hundreds of effector genes known as interferon stimulated genes (ISGs). These genes are the basis for an elaborate effector mechanism and ultimately, the clearance of viral infection. ISGs mark an elegant mechanism of anti-viral host defence that warrants renewed research focus in our global efforts to treat existing and emerging viruses. By understanding the mechanistic role of individual ISGs we anticipate the discovery of a new “treasure trove” of anti-viral mediators that may pave the way for more effective, targeted and less toxic anti-viral therapies. Therefore, with the aim of highlighting the value of the innate type 1 IFN response in our battle against viral infection, this review outlines both historic and recent advances in understanding the IFN-α JAK/STAT pathway, with a focus on new research discoveries relating to specific ISGs and their potential role in curing existing and future emergent viral infections.
Similar content being viewed by others
IFN
Almost 60 years ago, Isaacs and Lindenmann first described IFNs as key molecules that block viral infection [1]. Since then the IFN family of primordial cytokines have been continually defined as having a pivotal role in host immunity and first-line innate defence against viral pathogens. IFNs also display anti-proliferative and immunomodulatory properties. Owing to these important characteristics, research into IFN signalling mechanisms has expanded exponentially over the past decade.
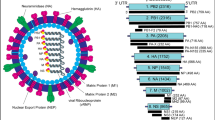
There are three main classes of IFN—type I, type II and type III. The IFNs are grouped into families based on their structural homology, chromosomal location and interaction with their various receptor chains. Type I IFNs include IFN-α (of which there are 13 human subtypes), as well as IFN-β, IFN-ε, IFN-κ and IFN-ω [2]. IFN-α genes are coded by numerous gene clusters on chromosome 9. IFN-α interacts with a common cell-surface receptor, known as type I IFN receptor (IFNAR). IFNAR is a heteromeric receptor that is made up of two subunits: IFNAR1 and IFNAR2 [3]. By binding this receptor, type I IFNs commence an intracellular signalling cascade that results in downstream effector mechanisms. During the last decade, a new appreciation for the role of IFNs, specifically type 1, in targeting viral infection, has emerged. Therefore, this review details new advances in this field, with a specific focus on the IFN-α JAK/STAT pathway and its related anti-viral effector ISGs.
Function of IFN
While type I IFNs have diverse roles, they are essential to eliminate viral infection. This has long been proven in studies using IFNAR-deficient mice, that show increased susceptibility to viral infections, as a direct result of impaired IFN signalling [4]. Similarly, it has been shown that humans with genetic defects resulting in STAT1 deficiency have impaired viral defence and consequently a higher susceptibility to viral infection. [5]. Type I IFNs enable viral clearance by activating anti-viral responses in the infected and surrounding cells, while also activating effector immune cells. They also facilitate viral clearance by upregulating the expression of MHC class I and co-stimulatory molecules, such as CD86, on the surface of dendritic cells (DCs) [6]. This results in increased viral recognition and subsequent activation of Th1 cells, that stimulates expression of several key cytokines (IFN-γ, IL-2, IL-10, TGF-β), responsible for both maximising the killing efficacy of macrophages, as well as increased differentiation of CD8+ T-cells, famous for their cytotoxic effects [7]. Furthermore, type I IFNs also trigger apoptosis, leading to the death of virally infected cells [8].
Viral induction of IFN
Recognition via pathogen recognition receptors (PRRs)
IFNs are initially produced following the detection of viral RNA, DNA or protein by intracellular PRRs. These PRRs are the ‘guards’ of the immune system and function to recognise these viral pathogen associated molecular patterns (PAMPs). Recognition and binding of PAMPs induces activation of innate immune signalling cascades, which result in the generation of anti-viral, type I IFNs and a spectrum of pro-inflammatory cytokines. Specific examples of PRRs specialised to recognise viral PAMPs are Toll-like receptors (TLRs) and Retinoic acid-inducible gene (RIG)-1-like receptors (RLRs) [9] (Fig. 1).
Schematic of PRR pathways (RLRs and TLRs) involved in detecting viral antigen. a The binding of viral PAMPS to RLRs results in the phosphorylation of IRF3 and IRF7, which, when translocated to the nucleus, promote type-1 IFN expression. b The binding of viral PAMPS to the endosomal TLRs (TLR3, TLR7, TLR8 and TLR9) results in IRF and NFκB activation, which promote the expression of both type-1 IFNs and pro-inflammatory cytokines involved in viral defense
TLRs are a family of PRRs expressed both on the plasma cell surface, as well as intracellular endosomal membranes. The endosomal TLRs (TLR3, TLR7, TLR8 and TLR9) are especially important in the recognition of viral PAMPs [10]. TLR7 recognises single stranded RNA (ssRNA) and TLR9 recognises unmethylated CpG DNA. The binding of viral PAMPs to these PRRs results in the phosphorylation of cytoplasmic IFN regulatory factor 7 (IRF7). IRF7 then translocates to the nucleus, where it facilitates the expression of type 1 IFNs through gene transcription. Likewise, TLR3 is activated by double stranded (ds) viral RNA, resulting in the phosphorylation of IRF3 which, like IRF7, translocates to the nucleus, also facilitating the expression of type 1 IFNs [11]. It is thought that IRF1, 3, 5 and 7 are important in the induction of IFN-α, whereas IRF3, cooperating with NF-κB and ATF-2/c-Jun, together form a transcriptionally active “enhanceosome complex” that enhances IFN-β gene expression [12, 13].
Another family of PRRs important in the recognition of viruses are the RLRs, a group of cytoplasmic PRRs involved in cytosolic surveillance for viral PAMPs. There are three members of the RLR family. RIG-1, Melanoma differentiation-associated protein 5 (MDA5) and Laboratory of genetics and physiology 2 (LGP2). Binding of RLRs to viral PAMPs leads to the activation of the mitochondrial bound adaptor protein, IFN-β promoter stimulator (IPS)-1. IPS-1 goes on to activate NFκB, IRFs and MAPK, resulting in the transcription of pro-inflammatory cytokines as well as type-1 IFNs [14, 15].
Interestingly, components of innate immune signalling pathways, required for type I IFN production, can also be regulated by type I IFNs themselves in a positive feedback loop. In fact, several PRRs and PRR signalling adaptors, most notably IRF7, are induced by type I IFNs, which enables the type I IFN production to be maintained or possibly enhanced [16, 17].
IFN-α, once expressed by the mechanisms outlined above, enters a downstream signalling cascade which is responsible for its effector functions, with the key pathway for IFN-α being the JAK/STAT signalling cascade.
Signal transduction via JAK/STAT
JAK/STAT pathway
The JAK/STAT signalling pathway is responsible for transmitting extracellular chemical signals to the nucleus and thereby facilitating the transcription of specific genes (Fig. 2). There are three components of the JAK/STAT pathway: (1) the cell receptor, (2) JAK proteins and (3) STAT proteins. There are four members of the JAK family [JAK 1, 2, 3 and tyrosine kinase (Tyk) 2] and seven STATs (1–4, 5a, 5b and 6) [18]. STAT proteins contain an SH2 domain, which is critical for their binding to phosphorylated receptor residues [19]. IFNAR1 and IFNAR2 subunits are permanently associated with Tyk2 and JAK1, which, when activated, are classically known to recruit STAT1 and STAT2 [20].
Schematic of classical, anti-viral IFN-α signalling. Upon type-1 IFN receptor engagement, JAKs become auto-phosphorylated and subsequently phosphorylate receptor residues, providing docking sites for STAT1 and STAT2. This binding results in phosphorylation of the STAT proteins. This leads to the formation of the ISGF3 complex following interaction of STAT1 and STAT2 with IRF9. This ISGF3 complex translocates to the nucleus, where it binds to ISRE promoter element. ISRE binding facilitates the transcription of multiple ISGs—a selection of which are discussed in this review, including Mx1, Mx2, PKR, OAS, viperin and tetherin
The binding of IFN-α to JAK proteins increases their kinase activity, leading to the phosphorylation of tyrosine residues on the receptor tail [21]. This phosphorylation results in the creation of a phosphotyrosine-based motif which allows for a more accessible binding site for STAT1 and STAT2. Upon binding, STATs are then also phosphorylated by JAKs. This phosphorylation leads to the formation of a heterodimer of phosphorylated STAT1 and STAT2. Cytoplasmic IRF9 binds to the STAT1:STAT2 heterodimer, forming a complex known as IFN-stimulated gene factor 3 (ISGF3). The ISGF3 complex then translocates from the cytoplasm into the nucleus, where it binds to a DNA sequence called the IFN-stimulated response element (ISRE). This binding triggers transcription of ISGs [22], which are responsible for the effector properties of IFN-α.
The anti-viral response
IFN stimulated genes (ISGs)
ISGs carry out a broad range of effector functions (Table 1). In fact, “ISG research” has now begun to elucidate how IFN-α re-programs the host’s cellular biology, resulting in a state of enhanced anti-viral defence.
The first ISGs were identified almost 30 years ago and since then IFN-α itself has been shown to regulate the expression of >500 ISGs [23]. As expected, with this number of induced genes, IFN-α acts to initiate many different effector functions. Some ISGs act as PRRs to increase viral recognition and immune cell recruitment, whilst others directly target the viral life cycle, stopping further viral infection [24]. As well as these “effector” ISGs, numerous ISGs are involved in the control of the actual IFN response. These “regulatory” ISGs are essential in returning normal balance to cellular homeostasis post-infection (Fig. 3).
“Effector” vs. “regulatory” effects of ISGs produced in response to type-1 IFNs. Type-1 IFNs stimulates the transcription of hundreds of ISGs. These ISGs can be broadly split into two categories: (1) anti-viral or “effector” ISGs and (2) “regulatory” ISGs. Anti-viral ISGs are critical in the defense against viruses, whereas regulatory ISGs ensure that the anti-viral response is controlled and prevents an over-zealous events, that could potentially damage to the host
Anti-viral effector ISGs
In an attempt to arrest viral activity, several ISGs target the complex and multi-faceted viral life cycle.
Inhibition of viral entry
Myxovirus resistance (Mx) genes are arguably the most extensively studied ISGs involved in viral inhibition. There are two Mx proteins encoded by Mx1 and Mx2 genes, often called MxA and MxB, respectively.
Mx1 acts on viruses at the early, post-entry, pre-replication stage. Its recently documented protein structure has led to new insights into its proposed mechanism of action [25]. Studies on Mx1 suggest that it is involved in trapping viral nucleocapsids as they enter the cell and therefore preventing them from reaching their target cellular destination. Indeed, recent research has shown Mx1 to be a key component of the anti-viral defence against the influenza-A virus in human cells [26]. Mx1 contains a GTPase domain which is important in self-oligomerisation and structure [27]. This GTPase activity also plays a role in directing “trapped” viral components to sites within the cell, where they are subsequently degraded [28].
Mx2 has recently been identified as an anti-viral effector protein. Studies showed that expression of Mx2 was linked to significant resistance against HIV. The same studies also showed that the presence of Mx2 is required for the full anti-viral efficacy of IFN-α against HIV. Mx2 functions in a similar manner to Mx1, by targeting and isolating viral components, thereby preventing the downstream pathway of the virus life cycle [29, 30].
Another family of proteins involved in early stage viral inhibition is the IFN inducible transmembrane (IFITM) family. There are four members in this family, IFITM1, IFITM2, IFITM3, IFITM5. Initially in 2009, IFITMs were shown to be strong inhibitors of Influenza A virus [31]. However, more recent research has given deeper insight into IFITM function. IFITMs have been shown to exhibit broad anti-viral activity against several viruses, including HCV and HIV [32, 33]. IFITM proteins are located primarily in late endosomes and lysosomes and as a result, are most active against viruses that utilise these pathways to penetrate the host cell environment [34]. IFITM1 is effective in inhibition of SARS coronavirus and Ebola, whereas IFITM3 is most effective against Influenza. A recent genome-wide association study (GWAS), supports the role of IFITM in Influenza and elegantly links polymorphisms in the IFITM3 gene with increased severity and likelihood of hospital admission of Influenza patients [35]. Fascinating new research has highlighted the anti-viral effects of IFITM3, specifically its effect on HIV-1. It was shown that the V3 loop of the HIV envelope protein determines the overall anti-viral effect of IFITM3 [36].
The Tripartite motif (TRIM) family of proteins also acts on the early stages of viral invasion. This is a large family of ~60 human genes [37]. TRIM5α is one of the most widely studied TRIM proteins and was identified as an inhibitor of early HIV-1 infection. TRIM5α has been shown to bind to the viral capsid of HIV in monkeys, where it results in accelerated capsid shell disassembly [38]. Electron microscopy has been used to investigate the anti-viral role of TRIM5α, using HIV-1 as the infecting agent. TRIM5α was found to mimic the viral capsid via a hexagonal lattice formation, thus enabling virion binding [39, 40]. TRIM5α is thought to function using two main mechanisms against HIV-1 infection: (1) it hastens the uncoating of the virion, thereby preventing viral reverse transcription and (2) its E3-ligase activity leads to enhanced degradation via the proteasome [41, 42].
Clinical studies have shown that another TRIM member, TRIM22, also plays a role in viral defence; with higher TRIM22 levels correlating with lower viral load in HIV-1 patients [43]. TRIM22 has also been implicated in other viral infections, including hepatitis B and influenza A [44–46].
Inhibition of protein synthesis
A large number of ISGs target viral translation and replication. Some of the most widely studied ISGs in this area include ISG15, 2′-5′-oligo-adenylate synthetase (OAS) and protein kinase R (PKR).
ISG15 is a ubiquitin-like protein and is among the most widely expressed ISGs induced by IFN-α. It can exist as a free molecule, both intracellularly and extracellularly, as well as conjugated to other proteins. This process of conjugation is known as ISGylation and involves the covalent attachment of ISG15 to target proteins [47]. For example, ISGylation of IRF3 creates a more stable IRF3, leading to more sustained activity and subsequently increased type I IFN production [48]. Interestingly, research on the anti-viral effects of ISG15 shows contrasting results between mice and humans. Studies using ISG15 knockout mice show an increased susceptibility to viral infections, such as influenza A and B, Herpes-simplex 1 virus (HSV-1) and Sindbus virus, suggesting a key role in anti-viral defence [49]. However, a study with ISG15-deficient humans shows no apparent increased susceptibility to viral infection, but does demonstrate a key role for ISG15 in anti-mycobacteria immunity [50]. While another group report that in humans, ISG15 reduces viral resistance and is involved in IFN-α/β signalling regulation by sustaining USP18 levels [51] (discussed further in section “USP18”).
The 2′-5′-OAS family of proteins were first identified as IFN-induced proteins capable of inhibiting cellular protein synthesis. There are four OAS genes in humans, OAS1, OAS2, OAS3 and OASlike (OASL) [52]. OAS proteins are characterised by their ability to synthesize 2′,5′-linked phosphodiester bonds, which go on to form unique 2′-5′-oligomers from ATP. These unique oligomers activate a latent form of RNaseL, which ultimately results in both viral and cellular RNA cleavage [53], thereby resulting in potent anti-viral activity through the degradation of viral RNA, as well as apoptosis of the infected host cell. The degree of anti-viral effector function via OAS genes has been investigated using RNaseL deficient mice. These mice were shown to have increased susceptibility to RNA viruses, including picornaviridae, reoviridae and flaviviridae [54]. Human studies have also reinforced the role of OAS in anti-viral defence, with immunisation trials showing that polymorphisms in the OAS1 gene significantly correlate with a poor response to the vaccine for yellow fever [55].
Whilst the RNaseL activity of the OAS proteins has been well characterised, it was recently suggested that the OAS proteins have additional anti-viral mechanisms [56, 57]. Recent research has focused on the OASL protein, which has shown evidence of both anti-viral and pro-viral activity. A study using an OASL deletion mutant discovered that it plays a role in suppressing replication of vesicular stomatitis virus by enhancing the RIG-I pathway [58]. However, another investigation found that OASL can suppress IRF7, a key transcription factor for type I IFN induction. It is, therefore, thought that OASL may have a dual function that depends on the viral phase [59]. Gaining a deeper understanding of OAS proteins and their full array of anti-viral/pro-viral effects may reveal novel targets for anti-viral treatment.
Similar to OAS, the PKR family was first identified based on its ability to interfere with protein synthesis in dsRNA treated cells [60]. PKR belongs to a family of tyrosine kinases that respond to intracellular environmental stress. It is constitutively expressed throughout the body in small amounts, however, it is upregulated in response to type I and type III IFNs. PKR carries out its anti-viral effector mechanisms by phosphorylating the eukaryotic translation initiation factor (eIF2α). EIF2α phosphorylation, leads to sequestration of eIF2b, a guanine nucleotide exchange factor which facilitates the recycling of GDP to GTP. By preventing the conversion of GDP to GTP, translation is halted [61]. Therefore, in short, PKR acts to phosphorylate eIF2α, which in turn inhibits translation of both cellular and viral RNA in virally infected cells.
The anti-viral role of PKR has been investigated using transgenic mice with deletions in PKR. These mice were found to be more susceptible to viral infections (VSV and influenza) and exhibited significantly impaired anti-viral responses [62]. PKR’s anti-viral role has also been affirmed in studies where its inhibition enhances HCV (genotype 1a) replication. In addition, by suppressing PKR activity, phosphorylation of STAT1 and NFκB activation are both decreased [63]. Interestingly, recent research has shown that the anticancer drug sunitinib (a potent tyrosine kinase inhibitor), prevents anti-viral innate immune responses mediated by PKR in cell cultures and in mice. Further human studies are necessary to elucidate if patients receiving this drug are at increased risk of viral infections [64]. Recent research efforts identified a key defence role for PKR against SARS coronavirus. This study aimed to identify pro-viral and anti-viral host effects using siRNA screening methods. They found that PKR was the strongest host anti-viral “hit” against SARS and confirmed their results in vitro using PKR knockdown cell assays. This study confirmed the strong anti-viral effects of PKR and hypothesised similar effects against other coronaviruses [65]. Future work into this area of anti-viral ISGs will enhance our understanding of the complex interplay between host and virus, thus revealing where our research efforts should focus in terms of anti-viral therapeutic design and development.
Inhibition of viral egress
Although most ISGs target viruses at the “pre-replication” stage, several ISGs have also been found to target viruses “post-translation”, before the viral proteins exit the infected cell. Two such examples are virus inhibitory protein endoplasmic reticulum associated IFN inducible (viperin) and tetherin.
Viperin is a highly expressed ISG, with broad anti-viral effects. A key mechanism of viperin is its ability to inhibit the enzyme Farnesyl diphosphate synthase (FPPS), which when decreased, interferes with cell membrane fluidity. Some viruses, such as influenza A, bud from lipid rafts, which require this membrane fluidity. A viperin-mediated decrease in FPPS thus prevents viral budding [66]. In addition, viperin has recently been found to also interfere with earlier viral life-cycle stages. For example, it has been shown to inhibit RNA replication in HCV through binding to the non-structural(NS)5A/human vesicle-associated membrane protein-associated protein subtype A (VP-A) complex, and thereby interfere with the stability and functionality of the HCV replication complex [67]. By suggesting that viperin exerts its effects at the early replication phase of viral invasion, this research suggests that viperin’s mechanism of action is multi-faceted, complex and undeniably critical in host anti-viral defence. Further work elucidating the nuances of such mechanisms is eagerly awaited.
Tetherin is a protein encoded by the BST2 gene. Like viperin, it prevents viral proteins leaving infected cells. Tetherin has a unique topology, with both ends of the protein embedded in the cellular membrane by transmembrane anchors. Studies have shown that it is this unique topology, rather than the amino acid sequence, that confers tetherin’s ability to restrict viral egress [68]. Initially identified in 2009, tetherin was noted for its ability to trap HIV-1 on the plasma membrane using its anchors, thereby preventing the virus egressing [68]. In recent years, studies using mice with single nucleotide polymorphisms (SNPs) in tetherin show significant increases in disseminated retroviral infection [69]. Tetherin’s anti-viral effects span a number of viral families, including filoviruses (Ebola and Marburg virus), paramyxovirus (Nipah virus), arenaviruses (Lassa and Machupo), as well as gamma-herpesvirus (Kaposi’s sarcoma-associated herpesvirus) [70–72].
Exciting new research, looking at the specific relationship between tetherin and HIV-1, focused on the viral protein U (Vpu) protein, which is known to target tetherin for degradation, as part of HIV-1’s immune evasion tactics. This study showed that mutations in Vpu made the HIV-1 virus more susceptible to antibody-dependant cell-mediated cytotoxicity (ADCC). These results suggest that tetherin serves as a link between innate and adaptive immune defence against viruses and may therefore represent a much more important role in host viral defence that was previously thought [73].
Negative regulators of IFN
Due to type I IFNs maximising PRR recognition of pathogens and strongly inducing immune effector mechanisms, their uncontrolled production has the potential to be detrimental to the host. In fact, the severe side-effects of exogenous IFN-α during HCV therapy, including flu-like symptoms and neuropsychiatric disorders, highlight the need to control its signalling responses [74]. For this reason, the human IFN response has several intracellular “check-points”, including induction of the regulatory proteins suppressor of cytokine signaling (SOCS) and ubiquitin specific peptidase (USP)18.
SOCS proteins
SOCS proteins are mainly induced by cytokines and function in a negative feedback loop that regulates signal transduction. SOCS proteins classically target the JAK/STAT pathway by binding phosphorylated tyrosine residues of the receptor chain and/or JAKs. By doing so, they inhibit STAT receptor binding and halt the propagation of downstream signalling [75]. SOCS proteins can even result in the degradation of the activated JAK/STAT complex through its ubiquitination and proteosomal degradation [76]. Studies have shown the regulatory power of SOCS proteins upon the anti-viral IFN-α signalling pathway. Overexpression of SOCS1 and SOCS3 can completely abrogate both 2′,5′-OAS and MxA mRNA expression. These studies implicate SOCS proteins as potential causes of IFN-α resistance in the treatment of viruses, such as HCV [77]. Furthermore, SOCS can be targeted by viruses as part of an elegant immune evasion mechanism, as seen with HIV-1, which targets SOCS3, resulting in a dampened host anti-viral state [78]. SOCS proteins are paramount in both determining the host susceptibility to viral infection as well as the response to certain anti-viral treatments. Understanding this unique regulatory system is therefore critical in the efforts to develop novel anti-viral immunotherapeutics.
USP18
USP18 belongs to the deubiquitinating protease family of enzymes and is involved in a process known as deISGlyation. ISGylation, as outlined earlier, is a pathway similar to that of ubiquitinisation and involves the covalent attachment of ISG15 to target proteins. USP18 targets this pathway by removing the covalently attached ISG15 proteins, thus reversing the process (hence the name, deISGlyation) [79]. This has been supported by studies using USP18 knockout mice, which have dramatically increased levels of ISGylation that correspond with hypersensitivity to type 1 IFNs and increased viral resistance [80]. Recently, USP18 has been shown to bind the intracellular domain of the IFNAR2, thereby inhibiting JAK1 binding and disrupting downstream IFN-α signalling. Together, these findings suggest that USP18’s regulatory activity may be specific to the signalling of type 1 IFNs [81]. Indeed, important clinical implications result from IFN-α desensitisation, as high levels of USP18 mRNA predict a poorer response to IFN-α treatment in HCV [82].
The future of ISGs
Biomedical research is increasingly looking towards novel immunotherapies that utilise the body’s own natural defences to control disease and infection. Type 1 IFN signalling and the resultant expression of ISGs is a superb example of an elegant immune mechanism of host defence. Gaining a better understanding of this pathway and the function of individual ISGs, will increase the likelihood of novel therapeutic development, aimed at enhancing our key primordial host effector functions. IFN-α has been used therapeutically for over two decades against HCV and was even trialled for HIV more than 20 years ago [83, 84]. However, viral immune evasion strategies result in poor clinical outcomes, with up to 50% of HCV (genotype 1) positive individuals not responding to IFN-α treatment [85]. Research into HCV has implicated degradation of the JAK/STAT pathway as a possible explanation for the poor IFN-α response seen in these patients [86]. Therefore, increased understanding of the IFN-α JAK/STAT signalling pathway is essential for our ambition to identify novel, more targeted, less toxic and overall more effective anti-viral treatments. ISG-based anti-viral strategies may well represent exciting new therapeutic targets going forward. Indeed, recent research endeavours have expanded our knowledge greatly and the future strategies are likely to show application of this new knowledge to clinical trials and much needed development of novel agents against both existing and emerging viruses.
Conclusions
IFN-α and the production of ISGs is critical for host defence against viruses. The expression of the various effector and regulatory ISGs ultimately determines how the host responds to viral infection. Novel research has led to paradigm shifts in our understanding of these innate immune anti-viral mechanisms of action. Through this research, we stand to gain an enriched understanding of viral invasion and indeed, evasion mechanisms and thus elicit new modes of harnessing this anti-viral activity via immunotherapeutic intervention.
References
Isaacs A, Lindenmann J (1957) Virus interference. I. The interferon. Proc R Soc Lond B Biol Sci 147:258–267
van Pesch V, Lanaya H, Renauld J-C, Michiels T (2004) Characterization of the murine alpha interferon gene family. J Virol 78:8219–8228. doi:10.1128/JVI.78.15.8219-8228.2004
Uzé G, Schreiber G, Piehler J, Pellegrini S (2007) The receptor of the type I interferon family. In: Pitha PM (ed) Interferon 50th anniv. Springer, Berlin, pp 71–95
Müller U, Steinhoff U, Reis LF et al (1994) Functional role of type I and type II interferons in antiviral defense. Science 264:1918–1921
Jouanguy E, Zhang S-Y, Chapgier A et al (2007) Human primary immunodeficiencies of type I interferons. Biochimie 89:878–883. doi:10.1016/j.biochi.2007.04.016
Simmons DP, Wearsch PA, Canaday DH et al (2012) Type I interferon drives a distinctive dendritic cell maturation phenotype that allows continued class II MHC synthesis and antigen processing. J Immunol Baltim Md 188:3116–3126. doi:10.4049/jimmunol.1101313
Cella M, Salio M, Sakakibara Y et al (1999) Maturation, activation, and protection of dendritic cells induced by double-stranded RNA. J Exp Med 189:821–829
Castelli JC, Hassel BA, Wood KA et al (1997) A study of the interferon antiviral mechanism: apoptosis activation by the 2-5A system. J Exp Med 186:967–972
Garland Science—Book: Janeway’s Immunobiology + 7. http://www.garlandscience.com/product/isbn/0815341237. Accessed 7 Sept 2016
Thompson MR, Kaminski JJ, Kurt-Jones EA, Fitzgerald KA (2011) Pattern recognition receptors and the innate immune response to viral infection. Viruses 3:920–940. doi:10.3390/v3060920
Xagorari A, Chlichlia K (2008) Toll-like receptors and viruses: induction of innate antiviral immune responses. Open Microbiol J 2:49–59. doi:10.2174/1874285800802010049
Grandvaux N, Servant MJ, tenOever B et al (2002) Transcriptional profiling of interferon regulatory factor 3 target genes: direct involvement in the regulation of interferon-stimulated genes. J Virol 76:5532–5539
Tamura T, Yanai H, Savitsky D, Taniguchi T (2008) The IRF family transcription factors in immunity and oncogenesis. Annu Rev Immunol 26:535–584. doi:10.1146/annurev.immunol.26.021607.090400
Gack MU (2014) Mechanisms of RIG-I-like receptor activation and manipulation by viral pathogens. J Virol 88:5213–5216. doi:10.1128/JVI.03370-13
Platanias LC (2005) Mechanisms of type-I- and type-II-interferon-mediated signalling. Nat Rev Immunol 5:375–386. doi:10.1038/nri1604
Levy DE, Marié I, Smith E, Prakash A (2002) Enhancement and diversification of IFN induction by IRF-7-mediated positive feedback. J Interferon Cytokine Res Off J Int Soc Interferon Cytokine Res 22:87–93. doi:10.1089/107999002753452692
Hertzog PJ, Williams BRG (2013) Fine tuning type I interferon responses. Cytokine Growth Factor Rev 24:217–225. doi:10.1016/j.cytogfr.2013.04.002
Aaronson DS, Horvath CM (2002) A road map for those who don’t know JAK-STAT. Science 296:1653–1655. doi:10.1126/science.1071545
Levy DE, Darnell JE (2002) Stats: transcriptional control and biological impact. Nat Rev Mol Cell Biol 3:651–662. doi:10.1038/nrm909
Decker T, Müller M, Stockinger S (2005) The yin and yang of type I interferon activity in bacterial infection. Nat Rev Immunol 5:675–687. doi:10.1038/nri1684
Brooks AJ, Dai W, O’Mara ML et al (2014) Mechanism of activation of protein kinase JAK2 by the growth hormone receptor. Science 344:1249783. doi:10.1126/science.1249783
Schneider WM, Chevillotte MD, Rice CM (2014) Interferon-stimulated genes: a complex web of host defenses. Annu Rev Immunol 32:513–545. doi:10.1146/annurev-immunol-032713-120231
de Veer MJ, Holko M, Frevel M et al (2001) Functional classification of interferon-stimulated genes identified using microarrays. J Leukoc Biol 69:912–920
Schoggins JW, Rice CM (2011) Interferon-stimulated genes and their antiviral effector functions. Curr Opin Virol 1:519–525. doi:10.1016/j.coviro.2011.10.008
Gao S, von der Malsburg A, Paeschke S et al (2010) Structural basis of oligomerization in the stalk region of dynamin-like MxA. Nature 465:502–506. doi:10.1038/nature08972
Xiao H, Killip MJ, Staeheli P et al (2013) The human interferon-induced MxA protein inhibits early stages of influenza A virus infection by retaining the incoming viral genome in the cytoplasm. J Virol. doi:10.1128/JVI.02220-13
Klockow B, Tichelaar W, Madden DR et al (2002) The dynamin A ring complex: molecular organization and nucleotide-dependent conformational changes. EMBO J 21:240–250. doi:10.1093/emboj/21.3.240
Haller O, Kochs G (2011) Human MxA protein: an interferon-induced dynamin-like GTPase with broad antiviral activity. J Interferon Cytokine Res Off J Int Soc Interferon Cytokine Res 31:79–87. doi:10.1089/jir.2010.0076
Kane M, Yadav SS, Bitzegeio J et al (2013) MX2 is an interferon-induced inhibitor of HIV-1 infection. Nature 502:563–566. doi:10.1038/nature12653
Goujon C, Moncorgé O, Bauby H et al (2013) Human MX2 is an interferon-induced post-entry inhibitor of HIV-1 infection. Nature 502:559–562. doi:10.1038/nature12542
Brass AL, Huang I-C, Benita Y et al (2009) The IFITM proteins mediate cellular resistance to influenza A H1N1 virus, West Nile virus, and dengue virus. Cell 139:1243–1254. doi:10.1016/j.cell.2009.12.017
Wilkins C, Woodward J, Lau DT-Y et al (2013) IFITM1 is a tight junction protein that inhibits hepatitis C virus entry. Hepatol Baltim Md 57:461–469. doi:10.1002/hep.26066
Lu J, Pan Q, Rong L et al (2011) The IFITM proteins inhibit HIV-1 infection. J Virol 85:2126–2137. doi:10.1128/JVI.01531-10
Feeley EM, Sims JS, John SP et al (2011) IFITM3 inhibits influenza A virus infection by preventing cytosolic entry. PLoS Pathog 7:e1002337. doi:10.1371/journal.ppat.1002337
Everitt AR, Clare S, Pertel T et al (2012) IFITM3 restricts the morbidity and mortality associated with influenza. Nature 484:519–523. doi:10.1038/nature10921
Wang Y, Pan Q, Ding S et al (2017) The V3-loop of HIV-1 Env determines viral susceptibility to IFITM3 impairment of viral infectivity. J Virol. doi:10.1128/JVI.02441-16
Ozato K, Shin D-M, Chang T-H, Morse HC (2008) TRIM family proteins and their emerging roles in innate immunity. Nat Rev Immunol 8:849–860. doi:10.1038/nri2413
Stremlau M, Owens CM, Perron MJ et al (2004) The cytoplasmic body component TRIM5alpha restricts HIV-1 infection in Old World monkeys. Nature 427:848–853. doi:10.1038/nature02343
Diaz-Griffero F (2011) Caging the beast: TRIM5α binding to the HIV-1 core. Viruses 3:423–428. doi:10.3390/v3050423
Ganser-Pornillos BK, Chandrasekaran V, Pornillos O et al (2011) Hexagonal assembly of a restricting TRIM5alpha protein. Proc Natl Acad Sci USA 108:534–539. doi:10.1073/pnas.1013426108
Towers GJ (2007) The control of viral infection by tripartite motif proteins and cyclophilin A. Retrovirology 4:40. doi:10.1186/1742-4690-4-40
Rold CJ, Aiken C (2008) Proteasomal degradation of TRIM5α during retrovirus restriction. PLoS Pathog 4:e1000074. doi:10.1371/journal.ppat.1000074
Singh R, Gaiha G, Werner L et al (2011) Association of TRIM22 with the type 1 interferon response and viral control during primary HIV-1 infection. J Virol 85:208–216. doi:10.1128/JVI.01810-10
Hattlmann CJ, Kelly JN, Barr SD (2012) TRIM22: a diverse and dynamic antiviral protein. Mol Biol Int 2012:e153415. doi:10.1155/2012/153415
Gao B, Duan Z, Xu W, Xiong S (2009) Tripartite motif-containing 22 inhibits the activity of hepatitis B virus core promoter, which is dependent on nuclear-located RING domain. Hepatol Baltim Md 50:424–433. doi:10.1002/hep.23011
Di Pietro A, Kajaste-Rudnitski A, Oteiza A et al (2013) TRIM22 inhibits influenza A virus infection by targeting the viral nucleoprotein for degradation. J Virol 87:4523–4533. doi:10.1128/JVI.02548-12
Zhao C, Collins M, Hsiang T-Y, Krug RM (2013) Interferon-induced ISG15 pathway: an ongoing virus–host battle. Trends Microbiol 21:181–186. doi:10.1016/j.tim.2013.01.005
Shi H-X, Yang K, Liu X et al (2010) Positive regulation of interferon regulatory factor 3 activation by Herc5 via ISG15 modification. Mol Cell Biol 30:2424–2436. doi:10.1128/MCB.01466-09
Lenschow DJ, Lai C, Frias-Staheli N et al (2007) IFN-stimulated gene 15 functions as a critical antiviral molecule against influenza, herpes, and Sindbis viruses. Proc Natl Acad Sci USA 104:1371–1376. doi:10.1073/pnas.0607038104
Bogunovic D, Byun M, Durfee LA et al (2012) Mycobacterial disease and impaired IFN-γ immunity in humans with inherited ISG15 deficiency. Science 337:1684–1688. doi:10.1126/science.1224026
Speer SD, Li Z, Buta S et al (2016) ISG15 deficiency and increased viral resistance in humans but not mice. Nat Commun. doi:10.1038/ncomms11496
Hovanessian AG, Justesen J (2007) The human 2′-5′oligoadenylate synthetase family: unique interferon-inducible enzymes catalyzing 2′-5′ instead of 3′-5′ phosphodiester bond formation. Biochimie 89:779–788. doi:10.1016/j.biochi.2007.02.003
Clemens MJ, Vaquero CM (1978) Inhibition of protein synthesis by double-stranded RNA in reticulocyte lysates: evidence for activation of an endoribonuclease. Biochem Biophys Res Commun 83:59–68
Zhou A, Paranjape J, Brown TL et al (1997) Interferon action and apoptosis are defective in mice devoid of 2′,5′-oligoadenylate-dependent RNase L. EMBO J 16:6355–6363. doi:10.1093/emboj/16.21.6355
Bonnevie-Nielsen V, Field LL, Lu S et al (2005) Variation in antiviral 2′,5′-oligoadenylate synthetase (2′5′AS) enzyme activity is controlled by a single-nucleotide polymorphism at a splice-acceptor site in the OAS1 gene. Am J Hum Genet 76:623–633. doi:10.1086/429391
Kristiansen H, Scherer CA, McVean M et al (2010) Extracellular 2′-5′ oligoadenylate synthetase stimulates RNase L-independent antiviral activity: a novel mechanism of virus-induced innate immunity. J Virol 84:11898–11904. doi:10.1128/JVI.01003-10
Choi UY, Kang J-S, Hwang YS, Kim Y-J (2015) Oligoadenylate synthase-like (OASL) proteins: dual functions and associations with diseases. Exp Mol Med 47:e144. doi:10.1038/emm.2014.110
Zhu J, Zhang Y, Ghosh A et al (2014) Antiviral activity of human OASL protein is mediated by enhancing signaling of the RIG-I RNA sensor. Immunity 40:936–948. doi:10.1016/j.immuni.2014.05.007
Lee MS, Kim B, Oh GT, Kim Y-J (2013) OASL1 inhibits translation of the type I interferon-regulating transcription factor IRF7. Nat Immunol 14:346–355. doi:10.1038/ni.2535
Meurs E, Chong K, Galabru J et al (1990) Molecular cloning and characterization of the human double-stranded RNA-activated protein kinase induced by interferon. Cell 62:379–390
Roberts WK, Hovanessian A, Brown RE et al (1976) Interferon-mediated protein kinase and low-molecular-weight inhibitor of protein synthesis. Nature 264:477–480. doi:10.1038/264477a0
Balachandran S, Roberts PC, Brown LE et al (2000) Essential role for the dsRNA-dependent protein kinase PKR in innate immunity to viral infection. Immunity 13:129–141
Zhang L, Alter HJ, Wang H et al (2013) The modulation of hepatitis C virus 1a replication by PKR is dependent on NF-κB mediated interferon beta response in Huh7.5.1 cells. Virology 438:28–36. doi:10.1016/j.virol.2013.01.015
Jha BK, Polyakova I, Kessler P et al (2011) Inhibition of RNase L and RNA-dependent protein kinase (PKR) by sunitinib impairs antiviral innate immunity. J Biol Chem 286:26319–26326. doi:10.1074/jbc.M111.253443
de Wilde AH, Wannee KF, Scholte FEM et al (2015) A kinome-wide small interfering RNA screen identifies proviral and antiviral host factors in severe acute respiratory syndrome coronavirus replication, including double-stranded RNA-activated protein kinase and early secretory pathway proteins. J Virol 89:8318–8333. doi:10.1128/JVI.01029-15
Wang X, Hinson ER, Cresswell P (2007) The interferon-inducible protein viperin inhibits influenza virus release by perturbing lipid rafts. Cell Host Microbe 2:96–105. doi:10.1016/j.chom.2007.06.009
Helbig KJ, Eyre NS, Yip E et al (2011) The antiviral protein viperin inhibits hepatitis C virus replication via interaction with nonstructural protein 5A. Hepatol Baltim Md 54:1506–1517. doi:10.1002/hep.24542
Perez-Caballero D, Zang T, Ebrahimi A et al (2009) Tetherin inhibits HIV-1 release by directly tethering virions to cells. Cell 139:499–511. doi:10.1016/j.cell.2009.08.039
Barrett BS, Smith DS, Li SX et al (2012) A single nucleotide polymorphism in tetherin promotes retrovirus restriction in vivo. PLoS Pathog 8:e1002596. doi:10.1371/journal.ppat.1002596
Jouvenet N, Neil SJD, Zhadina M et al (2009) Broad-spectrum inhibition of retroviral and filoviral particle release by tetherin. J Virol 83:1837–1844. doi:10.1128/JVI.02211-08
Sakuma T, Noda T, Urata S et al (2009) Inhibition of Lassa and Marburg virus production by tetherin. J Virol 83:2382–2385. doi:10.1128/JVI.01607-08
Mansouri M, Viswanathan K, Douglas JL et al (2009) Molecular mechanism of BST2/tetherin downregulation by K5/MIR2 of Kaposi’s sarcoma-associated herpesvirus. J Virol 83:9672–9681. doi:10.1128/JVI.00597-09
Arias JF, Heyer LN, von Bredow B et al (2014) Tetherin antagonism by Vpu protects HIV-infected cells from antibody-dependent cell-mediated cytotoxicity. Proc Natl Acad Sci USA 111:6425–6430. doi:10.1073/pnas.1321507111
Manns MP, Wedemeyer H, Cornberg M (2006) Treating viral hepatitis C: efficacy, side effects, and complications. Gut 55:1350–1359. doi:10.1136/gut.2005.076646
Piganis RAR, De Weerd NA, Gould JA et al (2011) Suppressor of cytokine signaling (SOCS) 1 inhibits type I interferon (IFN) signaling via the interferon alpha receptor (IFNAR1)-associated tyrosine kinase Tyk2. J Biol Chem 286:33811–33818. doi:10.1074/jbc.M111.270207
Tamiya T, Kashiwagi I, Takahashi R et al (2011) Suppressors of cytokine signaling (SOCS) proteins and JAK/STAT pathways. Arterioscler Thromb Vasc Biol 31:980–985. doi:10.1161/ATVBAHA.110.207464
Vlotides G, Sörensen AS, Kopp F et al (2004) SOCS-1 and SOCS-3 inhibit IFN-alpha-induced expression of the antiviral proteins 2,5-OAS and MxA. Biochem Biophys Res Commun 320:1007–1014. doi:10.1016/j.bbrc.2004.06.051
Akhtar LN, Benveniste EN (2011) Viral exploitation of host SOCS protein functions. J Virol 85:1912–1921. doi:10.1128/JVI.01857-10
Malakhov MP, Malakhova OA, Kim KI et al (2002) UBP43 (USP18) specifically removes ISG15 from conjugated proteins. J Biol Chem 277:9976–9981. doi:10.1074/jbc.M109078200
Ritchie KJ, Hahn CS, Kim KI et al (2004) Role of ISG15 protease UBP43 (USP18) in innate immunity to viral infection. Nat Med 10:1374–1378. doi:10.1038/nm1133
François-Newton V, Magno de Freitas Almeida G, Payelle-Brogard B et al (2011) USP18-based negative feedback control is induced by type I and type III interferons and specifically inactivates interferon α response. PLOS One 6:22200. doi:10.1371/journal.pone.0022200
Chen L, Borozan I, Feld J et al (2005) Hepatic gene expression discriminates responders and nonresponders in treatment of chronic hepatitis C viral infection. Gastroenterology 128:1437–1444
Borden EC, Sen GC, Uze G et al (2007) Interferons at age 50: past, current and future impact on biomedicine. Nat Rev Drug Discov 6:975–990. doi:10.1038/nrd2422
Haas DW, Lavelle J, Nadler JP et al (2000) A randomized trial of interferon alpha therapy for HIV type 1 infection. AIDS Res Hum Retroviruses 16:183–190. doi:10.1089/088922200309278
Zeuzem S, Berg T, Moeller B et al (2009) Expert opinion on the treatment of patients with chronic hepatitis C. J Viral Hepat 16:75–90. doi:10.1111/j.1365-2893.2008.01012.x
Stevenson NJ, Bourke NM, Ryan EJ et al (2013) Hepatitis C virus targets the interferon-α JAK/STAT pathway by promoting proteasomal degradation in immune cells and hepatocytes. FEBS Lett 587:1571–1578. doi:10.1016/j.febslet.2013.03.041
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Raftery, N., Stevenson, N.J. Advances in anti-viral immune defence: revealing the importance of the IFN JAK/STAT pathway. Cell. Mol. Life Sci. 74, 2525–2535 (2017). https://doi.org/10.1007/s00018-017-2520-2
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00018-017-2520-2