Abstract
Background
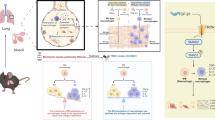
MUC1 is a membrane-tethered mucin expressed on the surface of epithelial and hematopoietic cells. Previous studies have established that MUC1 attenuates airway inflammation in response to Pseudomonas aeruginosa (Pa) through suppression of Toll-like receptor (TLR) signaling. Here, we elucidate the mechanism through which the MUC1 cytoplasmic tail (CT) inhibits TLR5 signaling in response to Pa and its flagellin in primary normal human bronchial epithelial (NHBE) cells.
Methods
NHBE and human and mouse macrophages were stimulated with Pa or flagellin and transforming growth factor-α (TGF-α) and tumor necrosis factor-α (TNF-α) levels in cell culture supernatants were measured by ELISA. NHBE cells were stimulated with Pa, flagellin, or TNF-α and MUC1-CT, and epidermal growth factor receptor (EGFR) levels were measured by immunoblotting. NHBE cells were stimulated with Pa and MUC1-CT/TLR5 and MUC1-CT/EGFR association were detected by co-immunoprecipitation.
Results
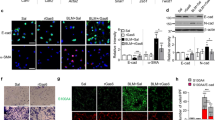
Stimulation of NHBE cells with Pa and flagellin each increased release of the EGFR ligand, TGF-α, from NHBE cells. Both stimuli also activated EGFR tyrosine phosphorylation in these same cells. By contrast, stimulation of NHBE cells with Pa failed to induce TNF-α release, whereas stimulation of human or mouse macrophages with Pa promoted TNF-α release. Stimulation of NHBE cells with recombinant TNF-α increased both MUC1 and EGFR protein levels, and stimulation of these cells with Pa enhanced MUC1-CT tyrosine phosphorylation and increased MUC1-CT/TLR5 and MUC1-CT/EGFR protein association, in an EGFR-dependent manner.
Conclusions
These results indicate that in response to Pa or flagellin, EGFR associates with and tyrosine phosphorylates MUC1-CT in primary NHBE cells, leading to increased MUC1-CT association with TLR5. Based on prior studies in tumor cells, increased MUC1-CT/TLR5 association in NHBE cells is predicted to competitively inhibit Pa/flagellin-stimulated TLR5 activation, reduce TLR5-dependent cell signaling, and down-regulate airway inflammation. Given that MUC1 is a universal suppressor of TLR signaling, the results from this study suggest that abnormal interactions between MUC1 and EGFR or TLRs may lead to the development of chronic inflammatory diseases. Thus, this is an important finding from the clinical point of view.





Similar content being viewed by others
Abbreviations
- AEC:
-
Airway epithelial cell
- CFU:
-
Colony forming unit
- CT:
-
Cytoplasmic tail
- EGFR:
-
Epidermal growth factor receptor
- ELISA:
-
Enzyme-linked immunosorbent assay
- HRP:
-
Horseradish peroxidase
- IL:
-
Interleukin
- Mac:
-
Macrophage
- IB:
-
Immunoblot
- IP:
-
Immunoprecipitation
- NK-κB:
-
Nuclear factor-κB
- NHBE:
-
Normal human bronchial epithelial
- Pa:
-
Pseudomonas aeruginosa
- PAK:
-
Pseudomonas aeruginosa strain K
- PAMPs:
-
Pathogen-associated molecular patterns
- PI3K:
-
Phosphoinositide 3-kinase
- TACE:
-
Tumor necrosis factor-α converting enzyme
- TGF-α:
-
Transforming growth factor-α
- TLR:
-
Toll-like receptor
- TNF-α:
-
Tumor necrosis factor-α
References
Zhuo H, Yang K, Lynch SV, Dotson RH, Glidden DV, Singh G, Webb WR, Elicker BM, Garcia O, Brown R, Sawa Y, Misset B, Wiener-Kronish JP. Increased mortality of ventilated patients with endotracheal Pseudomonas aeruginosa without clinical signs of infection. Crit Care Med. 2008;36(9):2495–503.
Chawla K, Vishwanath S, Manu MK, Lazer B. Influence of Pseudomonas aeruginosa on exacerbation in patients with bronchiectasis. J Glob Infect Dis. 2015;7(1):18–22.
Sethi S, Evans N, Grant BJ, Murphy TF. New strains of bacteria and exacerbations of chronic obstructive pulmonary disease. N Engl J Med. 2002;347(7):465–71.
Basu S, Fenton MJ. Toll-like receptors: function and roles in lung disease. Am J Physiol Lung Cell Mol Physiol. 2004;286(5):L887–92.
Zhang Z, Louboutin JP, Weiner DJ, Goldberg JB, Wilson JM. Human airway epithelial cells sense Pseudomonas aeruginosa infection via recognition of flagellin by Toll-like receptor 5. Infect Immun. 2005;73(11):7151–60.
Ojielo CI, Cooke K, Mancuso P, Standiford TJ, Olkiewicz KM, Clouthier S, Corrion L, Ballinger MN, Toews GB, Paine R 3rd, Moore BB. Defective phagocytosis and clearance of Pseudomonas aeruginosa in the lung following bone marrow transplantation. J Immunol. 2003;171(8):4416–24.
Cohen TS, Prince AS. Activation of inflammasome signaling mediates pathology of acute Pseudomonas aeruginosa pneumonia. J Clin Invest. 2013;123(4):1630–7.
Lu W, Hisatsune A, Koga T, Kato K, Kuwahara I, Lillehoj EP, Chen W, Cross AS, Gendler SJ, Gewirtz AT, Kim KC. Cutting edge: enhanced pulmonary clearance of Pseudomonas aeruginosa by Muc1 knockout mice. J Immunol. 2006;176(7):3890–4.
Kato K, Lu W, Kai H, Kim KC. Phosphoinositide 3-kinase is activated by MUC1 but not responsible for MUC1-induced suppression of toll-like receptor 5 signaling. Am J Physiol Lung Cell Mol Physiol. 2007;293(3):L686–92.
Umehara T, Kato K, Park YS, Lillehoj EP, Kawauchi H, Kim KC. Prevention of lung injury by Muc1 mucin in a mouse model of repetitive Pseudomonas aeruginosa infection. Inflamm Res. 2012;61(9):1013–20.
Kato K, Lillehoj EP, Park YS, Umehara T, Hoffman NE, Madesh M, Kim KC. Membrane-tethered muc1 mucin is phosphorylated by epidermal growth factor receptor in airway epithelial cells and associates with TLR5 to inhibit recruitment of myD88. J Immunol. 2012;188:2014–22.
Gendler SJ. MUC1, the renaissance molecule. J Mammary Gland Biol Neoplasia. 2001;6(3):339–53.
Wang H, Lillehoj EP, Kim KC. Identification of four sites of stimulated tyrosine phosphorylation in the MUC1 cytoplasmic tail. Biochem Biophys Res Commun. 2003;310(2):341–6.
Ueno K, Koga T, Kato K, Golenbock DT, Gendler SJ, Kai H, Kim KC. MUC1 mucin is a negative regulator of toll-like receptor signaling. Am J Respir Cell Mol Biol. 2008;38(3):263–8.
Choi S, Park YS, Koga T, Treloar A, Kim KC. TNF-alpha is a key regulator of MUC1, an anti-inflammatory molecule, during airway Pseudomonas aeruginosa infection. Am J Respir Cell Mol Biol. 2011;44(2):255–60.
Daigneault M, Preston JA, Marriott HM, Whyte MK, Dockrell DH. The identification of markers of macrophage differentiation in PMA-stimulated THP-1 cells and monocyte-derived macrophages. PLoS One. 2010;5(1):e8668.
Zhang, X, Goncalves, R, Mosser, DM The isolation and characterization of murine macrophages. Curr Protoc Immunol 2008, Chapter 14: Unit 14.1.
Yu H, Zhou X, Wen S, Xiao Q. Flagellin/TLR5 responses induce mucus hypersecretion by activating EGFR via an epithelial cell signaling cascades. Exp Cell Res. 2012;318(6):723–31.
Koga T, Kuwahara I, Lillehoj EP, Lu W, Miyata T, Isohama Y, Kim KC. TNF-alpha induces MUC1 gene transcription in lung epithelial cells: its signaling pathway and biological implication. Am J Physiol Lung Cell Mol Physiol. 2007;293(3):L693–701.
Raoust E, Balloy V, Garcia-Verdugo I, Touqui L, Ramphal R, Chignard M. Pseudomonas aeruginosa LPS or flagellin are sufficient to activate TLR-dependent signaling in murine alveolar macrophages and airway epithelial cells. PLoS One. 2009;4(10):e7259.
Li Y, Ren J, Yu W, Li Q, Kuwahara H, Yin L, Carraway KL 3rd, Kufe D. The epidermal growth factor receptor regulates interaction of the human DF3/MUC1 carcinoma antigen with c-Src and beta-catenin. J Biol Chem. 2001;276(38):35239–42.
Schroeder JA, Thompson MC, Gardner MM, Gendler SJ. Transgenic MUC1 interacts with epidermal growth factor receptor and correlates with mitogen-activated protein kinase activation in the mouse mammary gland. J Biol Chem. 2001;276(16):13057–64.
Bitler BG, Goverdhan A, Schroeder JA. MUC1 regulates nuclear localization and function of the epidermal growth factor receptor. J Cell Sci. 2010;123(Pt 10):1716–23.
Kyo Y, Kato K, Park YS, Gajhate S, Umehara T, Lillehoj EP, Suzaki H, Kim KC. Anti-inflammatory role of MUC1 mucin during nontypeable Haemophilus influenzae infection. Am J Respir Cell Mol Biol. 2012;46(2):149–56.
Li Y, Dinwiddie DL, Harrod KS, Jiang Y, Kim KC. Anti-inflammatory effect of MUC1 during respiratory syncytial virus infection of lung epithelial cells in vitro. Am J Physiol Lung Cell Mol Physiol. 2010;298(4):L558–63.
Takeyama K, Dabbagh K, Lee HM, Agusti C, Lausier JA, Ueki IF, Grattan KM, Nadel JA. Epidermal growth factor system regulates mucin production in airways. Proc Natl Acad Sci U S A. 1999;96(6):3081–6.
Kohri K, Ueki IF, Shim JJ, Burgel PR, Oh YM, Tam DC, Dao-Pick T, Nadel JA. Pseudomonas aeruginosa induces MUC5AC production via epidermal growth factor receptor. Eur Respir J. 2002;20(5):1263–70.
Shao MX, Ueki IF, Nadel JA. Tumor necrosis factor alpha-converting enzyme mediates MUC5AC mucin expression in cultured human airway epithelial cells. Proc Natl Acad Sci USA. 2003;100(20):11618–23.
Gooz M. ADAM-17: the enzyme that does it all. Crit Rev Biochem Mol Biol. 2010;45(2):146–69.
Menon BB, Kaiser-Marko C, Spurr-Michaud S, Tisdale AS, Gipson IK Suppression of toll-like receptor-mediated innate immune responses at the ocular surface by the membrane-associated mucins MUC1 and MUC16. Mucosal Immunol. 2015.
Sheng YH, Triyana S, Wang R, Das I, Gerloff K, Florin TH, Sutton P, McGuckin MA MUC1 and MUC13 differentially regulate epithelial inflammation in response to inflammatory and infectious stimuli. Mucosal Immunol. 2012.
Williams MA, Bauer S, Lu W, Guo J, Walter S, Bushnell TP, Lillehoj EP, Georas SN. Deletion of the mucin-like molecule muc1 enhances dendritic cell activation in response to toll-like receptor ligands. J Innate Immun. 2010;2(2):123–43.
Kondo T, Kawai T, Akira S. Dissecting negative regulation of Toll-like receptor signaling. Trends Immunol. 2012;33(9):449–58.
Hisatsune A, Nakayama H, Kawasaki M, Horie I, Miyata T, Isohama Y, Kim KC, Katsuki H. Anti-MUC1 antibody inhibits EGF receptor signaling in cancer cells. Biochem Biophys Res Commun. 2011;405(3):377–81.
Kharbanda A, Rajabi H, Jin C, Tchaicha J, Kikuchi E, Wong KK, Kufe D. Targeting the oncogenic MUC1-C protein inhibits mutant EGFR-mediated signaling and survival in non-small cell lung cancer cells. Clin Cancer Res. 2014;20(21):5423–34.
Neeraja D, Engel BJ, Carson DD. Activated EGFR stimulates MUC1 expression in human uterine and pancreatic cancer cell lines. J Cell Biochem. 2013;114(10):2314–22.
Li X, Wang L, Nunes DP, Troxler RF, Offner GD. Suppression of MUC1 synthesis downregulates expression of the epidermal growth factor receptor. Cancer Biol Ther. 2005;4(9):968–73.
Xu X, Bai L, Chen W, Padilla MT, Liu Y, Kim KC, Belinsky SA, Lin Y. MUC1 contributes to BPDE-induced human bronchial epithelial cell transformation through facilitating EGFR activation. PLoS One. 2012;7(3):e33846.
Acknowledgments
This work was supported by National institutes of Health Grant RO1 HL-047125. The authors thank Alec Hanss, Audriana Hurbon, and Nicole Morgan for technical assistance through their summer research program at the University of Arizona (Tucson, AZ).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no competing interests.
Additional information
Responsible Editor: Artur Bauhofer.
Rights and permissions
About this article
Cite this article
Kato, K., Lillehoj, E.P. & Kim, K.C. Pseudomonas aeruginosa stimulates tyrosine phosphorylation of and TLR5 association with the MUC1 cytoplasmic tail through EGFR activation. Inflamm. Res. 65, 225–233 (2016). https://doi.org/10.1007/s00011-015-0908-8
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00011-015-0908-8