Abstract
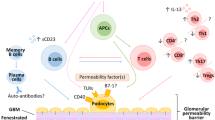
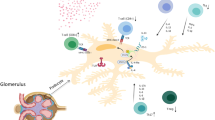
Idiopathic nephrotic syndrome (INS) is a multifactorial disease, characterized by proteinuria, hypoalbuminemia, edema and hyperlipidemia. Studies in humans and animal models have associated INS with changes in the immune response. The purpose of this article is to review clinical and experimental findings showing the involvement of the immune response in the pathogenesis of INS. The role of the immune system in INS has been shown by clinical and experimental studies. However, the pattern of immune response in patients with INS is still not clearly defined. Many studies show changes in the dynamics of T lymphocytes, especially the regulatory T cells. Alternatively, there are other reports regarding the involvement of the complement system and B lymphocytes in the pathophysiology of INS. Indeed, none of the immunological biomarkers evaluated were undeniably linked to changes in glomerular permeability and proteinuria. On the other hand, some studies suggest a link between urinary chemokines, such as IL-8/CXCL8 and MCP-1/CCL2, and changes in glomerular permeability and/or the deterioration of glomerulopathies. To understand the pathophysiology of INS, longitudinal studies are clearly needed. The characterization of the profile of the immune response might help the development of specific and individualized therapies, leading to clinical improvement and better prognosis.


Similar content being viewed by others
References
Schachter AD. The pediatric nephrotic syndrome spectrum: clinical homogeneity and molecular heterogeneity. Pediatr Transpl. 2004;8:344–8.
D’Agati VD, Kaskel FJ, Falk RJ. Focal segmental glomerulosclerosis. N Engl J Med. 2011;365:2398–411.
Souto MFO, Teixeira MM, Penido MGMG, Simões e Silva AC. Fisiopatologia da Síndrome Nefrótica em crianças e adolescentes. Arch Latin Nefr Ped. 2008;8:1–10.
Fodor P, Saitúa MT, Rodriguez E, González B, Schlesinger L. T-cell dysfunction in minimal-change nephrotic syndrome of childhood. Am J Dis Child. 1982;136:713–7.
Araya C, Diaz L, Wasserfall C, Atkinson M, Mu W, Johnson R, et al. T regulatory cell function in idiopathic minimal lesion nephrotic syndrome. Pediatr Nephrol. 2009;24:1691–8.
Araya CE, Wasserfall CH, Brusko TM, Mu W, Segal MS, Johnson RJ, et al. A case of unfulfilled expectations cytokines in idiopathic minimal lesion nephrotic syndrome. Pediatr Nephrol. 2006;21(603–610):3.
Shalboub RJ. Pathogenesis of lipoid nephritis: a disorder of T cell function. Lancet. 1974;304:556–60.
Savin VJ, Sharma R, Sharma M, McCarthy ET, Swan SK, Ellis E, et al. Circulating fator associated with increased glomerular permeability to albumin in recurrent focal segmental glomerulosclerosis. N Engl J Med. 1996;334:878–83.
Gitlin D, Janeway CA, Farr LE. Studies of the metabolism of plasma proteins in the nephrotic syndrome. I. Albumin, γ-globulin and immunoglobulin. J Clin Invest. 1956;35:44–56.
Lagrue G, Branellec A, Blanc C, Xheneumont S, Beaudoux F, Sobel A, et al. A vascular permeability factor in lymphocyte culture supernatants from patients with nephrotic syndrome II: pharmacological and physicochemical properties. Biomedicine. 1975;23:73–5.
Giangiacomo J, Cleary TG, Cole BR, Hoffstein P, Robson AM. Serum immunoglobulins in the nephrotic syndrome. A possible cause of minimal change nephrotic syndrome. N Engl J Med. 1975;293:08–12.
Herrod HG, Stapleton FB, Trouy RL, Roy S. Evaluation of T lymphocyte subpopulations in children with nephrotic syndrome. Clin Exp Immunol. 1983;52:581–5.
Boulton JJM, Tulloch I, Dore B, Mclay A. Changes in the glomerular capillary wall induced by lymphocyte products and serum of nephrotic patients. Clin Nephrol. 1983;20:72–7.
Yokoyama H, Kida H, Tani Y, Abe T, Tomosugi N, Koshino Y, et al. Immunodynamics of minimal change nephrotic syndrome in adults T and B lymphocyte subsets and serum immunoglobulin levels. Clin Exp Immunol. 1985;61:601–7.
Beaman M, Oldfield S, Maclennan ICM, Michael J, Adu D. Hypogammaglobulinaemia in nephrotic rats is attributable to hypercatabolism of IgG. Clin Exp Immunol. 1988;74:425–30.
Moorthy AV, Zimmerman SW, Burkholder PM. Inhibition of lymphocyte blastogenesis by plasma of patients with minimal change nephrotic syndrome. Lancet. 1976;1:1160–2.
Kausman JY, Kitching AR. A new approach to idiopathic nephrotic syndrome. J Am Soc Nephrol. 2007;18:2621–2.
Hashimura Y, Nozu K, Kanegane H, Miyawaki T, Hayakawa A, Yoshikawa N, et al. Minimal change nephrotic syndrome associated with immune dysregulation, polyendocrinopathy, enteropathy, X-linked syndrome. Pediatr Nephrol. 2009;24:1181–6.
Lagrue G, Branellec A, Xheneumont S, Weil B. Lymphokine ‘skin reactive factor’ (SRF) and the nephrotic syndrome. Bibl Anat. 1975;13:331–4.
Tanaka R, Yoshikawa N, Nakamura H, Ito H. Infusion of peripheral blood mononuclear cell products from nephrotic children increases albuminuria in rats. Nephron. 1992;60:35–41.
Riyuzo MC, Soares V. Revisão: Papel do infiltrado inflamatório na fibrose túbulo-intersticial e evolução das glomerulopatias. J Bras Nefrol. 2002;24:40–7.
Le Berre L, Herve C, Buzelin F, Usal C, Soulillou JP, Dantal J. Renal macrophage activation and Th2 polarization precedes the development of nephrotic syndrome in Buffalo/Mna rats. Kidney Int. 2005;68:2079–90.
Cao Q, Wang Y, Zheng D, Sun Y, Wang YA, et al. IL-10/TGF-β-modified macrophages induce regulatory t cells and protect against adriamycin nephrosis. J Am Soc Nephrol. 2010;21:933–42.
Kuncio GS, Neilson EG, Haverty T. Mechanisms of tubulointerstitial fibrosis. Kidney Int. 1991;39:550–6.
Benz K, Büttner M, Dittrich K, Campean V, Dötsch J, Amann K. Characterization of renal immune cell infiltrates in children with nephrotic syndrome. Pediatr Nephrol. 2010;25:1291–8.
Lai K-W, Wei Ch-L, Tan L-K, Tan P-H, Chiang GSC, Lee CGL, et al. Overexpression of interleukin 13 induces minimal-change-like nephropathy in rats. J Am Soc Nephrol. 2007;18:1476–85.
Lee VWS, Wang Y, Qin X, Wang Y, Zheng G, Mahajan D, et al. Adriamycin nephropathy in severe combined immunodeficient (SCID) mice. Nephrol Dial Transpl. 2006;21:3293–8.
Vielhauer V, Berning E, Eis V, Kretzler M, Segerer S, Strutz F, et al. CCR1 blockade reduces interstitial inflammation and fibrosis in mice with glomerulosclerosis and nephrotic syndrome. Kidney Int. 2004;66:2264–78.
Wu H, Wang Y, Tay Y-C, Zheng G, Shang C, Alexander S, et al. DNA vaccination with naked DNA encoding MCP-1 and RANTES protects against renal injury in Adriamycin nephropathy. Kidney Int. 2005;67:2178–86.
Wang Y, Wang YP, Tay Y-C, Harris DCH. Progressive adriamycin nephropathy in mice: sequence of histologic and immunohistochemical events. Kidney Int. 2000;58:1797–804.
Rossmann P, Matousovic K, Bohdanecká M. Experimental adriamycin nephropathy: fine structure, morphometry, glomerular polyanion and cell membrane antigens. J Pathol. 1993;169:99–108.
Muñoz M, Rincón J, Pedreañez A, Viera N, Hernández-Fonseca JP, Mosquera J. Proinflammatory role of angiotensin II in a rat nephrosis model induced by Adriamycin. J Renin Angiotensin Aldosterone Syst. 2001; doi:10.1177/14703203114100922011.
Van Goor H, Van Der Horst MLC, Atmosoerodjo J, Joles JA, Van To A, Grond J. Renal apolipoproteins in nephrotic rats. Am J Pathol. 1993;142:1804–12.
Erwig LP, Kluth DC, Rees AJ. Macrophage heterogeneity in renal inflammation. Nephrol Dial Transpl. 2003;18:1962–5.
Eardley KS, Cockwell P. Macrophages and progressive tubulointerstitial disease. Kidney Int. 2005;68:437–55.
Wang Y, Wang YP, Zheng G, Lee VWS, Ouyang L, Chang DHH, et al. Ex vivo programmed macrophages ameliorate experimental chronic inflammatory renal disease. Kidney Int. 2007;72:290–9.
Schnaper HW, Aune TM. Identification of the lymphokine soluble immune response suppressor in urine of nephrotic children. J Clin Invest. 1985;76:341–9.
Sasdelli M, Rovinetti C, Cagnoli L, Beltrandi E, Barboni F, Zucchelli P. Lymphocyte subpopulations in minimal-change nephropathy. Nephron. 1980;25:72–6.
Fiser RT, Arnold WC, Charlton RK, Steele RW, Childress SH, Shirkey B. T-lymphocyte subsets in nephrotic syndrome. Kidney Int. 1991;40:913–6.
Lama G, Luongo I, Tirino G, Borriello A, Carangio C, Salsano ME. T-lymphocyte populations and cytokines in childhood nephrotic syndrome. Am J Kidney Dis. 2002;39:958–65.
Wang Y, Wang Y, Feng X, Bao S, Yi S, Kairaitis L, et al. Depletion of CD4 T cells aggravates glomerular and interstitial injury in murine adriamycin nephropathy. Kidney Int. 2001;59:975–84.
Wang Y, Wang YP, Tay Y-C, Harris DCH. Role of CD8 cells in the progression of murine adriamycin nephropathy. Kidney Int. 2001;59:941–9.
Tejani AT, Butt K, Trachtman H, Suthanthiran M, Rosenthal CJ, Khawar MR. Cyclosporine-A induced remission of relapsing nephrotic syndrome in children. Kidney Int. 1988;33:729–34.
Okuyama S, Komatsuda A, Wakui H, Aiba N, Fujishima N, Iwamoto K, et al. Up-regulation of TRAIL mRNA expression in peripheral blood mononuclear cells from patients with minimal-change nephrotic syndrome. Nephrol Dial Transpl. 2005;20:539–44.
Musial K, Ciszak L, Kosmaczewska A, Szteblich A, Frydecka I, Zwolińska D. Zeta chain expression in T and NK cells in peripheral blood of children with nephrotic syndrome. Pediatr Nephrol. 2010;25:119–27.
Wu H, Wang YM, Wang Y, Hu M, Zhang GY, Knight JF, et al. Depletion of gama–delta T cells exacerbates murine adriamycin nephropathy. J Am Soc Nephrol. 2007;18:1180–9.
Wang YM, Hu M, Wang Y, Polhill T, Zhang GY, Wang Y, et al. Regulatory T cells in renal disease. Int J Clin Exp Med. 2008;1:294–304.
Rubio-Cabezas O, Minton JA, Caswell R, Shield JP, Deiss D, Sumnik Z, et al. Clinical heterogeneity in patients with FOXP3 mutations presenting with permanent neonatal diabetes. Diabetes Care. 2009;32:111–6.
Apostolou I, Von Boehmer H. In vivo instruction of suppressor commitment in naive T cells. J Exp Med. 2004;199:1401–8.
Chen W, Jin W, Hardegen N, Lei KJ, Li L, Marinos N, et al. Conversion of peripheral CD4+CD25− naïve T cells to CD4+CD25+ regulatory T cells by TGF-beta induction of transcription factor FOXP3. J Exp Med. 2003;198:1875–86.
Le NT, Chao N. Regulating regulatory T cells. Bone Marrow Transpl. 2007;39:01–9.
Wang YM, Zhang GY, Wang Y, Hu M, Wu H, Watson D, et al. Foxp3-transduced polyclonal regulatory T cells protect against chronic renal injury from adriamycin. J Am Soc Nephrol. 2006;17:697–706.
Mahajan D, Wang Y, Qin X, Wang Y, Zheng G, Wang YM, et al. CD4+CD25+ regulatory T cells protect against injury in an innate murine model of chronic kidney disease. J Am Soc Nephrol. 2006;17:2731–41.
Shao XS, Yang XQ, Zhao XD, Li Q, Xie YY, Wang XG, et al. The prevalence of Th17 cells and FOXP3 regulate T cells (Treg) in children with primary nephrotic syndrome. Pediatr Nephrol. 2009;24:1683–90.
Pereira RL, Reis VO, Semedo P, Buscariollo BN, Donizetti-Oliveira C, Cenedeze MA, et al. Invariant natural killer T cell agonist modulates experimental focal and segmental glomerulosclerosis. PLoS One. 2012;. doi:10.1371/journal.pone.0032454.
Sellier-Leclerc AL, Duval A, Riveron S, Macher MA, Deschenes G, Loirat C, et al. A humanized mouse model of idiopathic nephrotic syndrome suggests a pathogenic role for immature cells. J Am Soc Nephrol. 2007;18:2732–9.
Garin EH, Blanchard DK, Matsushima K, Djeu JY. IL-8 production by peripheral blood mononuclear cells in nephrotic patients. Kidney Int. 1994;45:1311–7.
Neuhaus TJ, Wadhwa M, Callard R, Barratt TM. Increased IL-2, IL-4 and interferon-gamma (IFN-γ) in steroid-sensitive nephrotic syndrome. Clin Exp Immunol. 1995;100:475–9.
Yap HK, Cheung W, Murugasu B, Sim SK, Seah CC, Jordan SC. Th1 and Th2 cytokine mRNA profiles in childhood nephrotic syndrome: evidence for increased IL-13 mRNA expression in relapse. J Am Soc Nephrol. 1999;10:529–37.
Kemper MJ, Meyer-Jark T, Lilova M, Müller-Wiefel DE. Combined T- and B-cell activation in childhood steroid-sensitive nephrotic syndrome. Clin Nephrol. 2003;60:242–7.
Valanciuté A, Le SG, Solhonne B, Pawlak A, Grimbert P, Lyonnet L, et al. NF-kappa-B p65 antagonizes IL-4 induction by c-maf in minimal change nephrotic syndrome. J Immunol. 2004;172:688–98.
Kanai T, Yamagata T, Momoi MY. Macrophage inflammatory protein-1b and interleukin-8 associated with idiopathic steroid sensitive nephrotic syndrome. Pediatr Int. 2009;51:443–7.
Bricio T, Molina A, Egido J, Gonzalez E, Mampaso F. IL-1-like production in adriamycin-induced nephrotic syndrome in the rat. Clin Exp Immunol. 1992;87:117–21.
Wang Y, Chen J, Chen L, Tay Y-C, Rangan GK, Harris DCH. Induction of monocyte chemoattractant protein-1 in proximal tubule cells by urinary protein. J Am Soc Nephrol. 1997;8:1537–45.
Rangan GK, Wang Y, Tay YC, Harris DCH. Inhibition of nuclear factor-κB activation reduces cortical tubulointerstitial injury in proteinuric rats. Kidney Int. 1999;56:118–34.
Wang LM, Chi HJ, Wang LN, Nie L, Zou YH, Zhao TN, et al. Expression of interleukin 6 in rat model of doxorubicin induced nephropathy. Chin J Contemp Pediatr. 2010;12:912–4.
Kerpen HO, Bhat JG, Kantor R, Gauthier B, Rai KR, Schacht RG, et al. Lymphocyte subpopulations in minimal change nephrotic syndrome. Clin Immunol Immunopathol. 1979;14:130–6.
Pescovitz MD, Book BK, Sidner RA. Resolution of recurrent focal segmental glomerulosclerosis proteinuria after rituximab treatment. N Engl J Med. 2006;354:1961–3.
Ahmed MS, Wong CF. Rituximab and nephrotic syndrome: a new therapeutic hope? Nephrol Dial Transpl. 2008;23:11–7.
Takei T, Nitta K. Rituximab and minimal change nephrotic syndrome: a therapeutic option. Clin Exp Nephrol. 2011;15:641–7.
Sarma JV, Ward PA. The complement system. Cell Tissue Res. 2011; doi:10.1007/s00441-010-1034-0.
David S, Biancone L, Caserta C, Bussolati B, Cambi V, Camussi G. Alternative pathway complement activation induces proinflammatory activity in human proximal tubular epithelial cells. Nephrol Dial Transpl. 1997;12:51–6.
Rangan GK, Pippin JW, Couser WG. C5b-9 regulates peritubular myofibroblast accumulation in experimental focal segmental glomerulosclerosis. Kidney Int. 2004;66:1838–48.
He C, Imai M, Song H, Quigg RJ, Tomlinson S. Complement inhibitors targeted to the proximal tubule prevent injury in experimental nephrotic syndrome and demonstrate a key role for C5b-91. J Immunol. 2005;174:5750–7.
Rangan GK, Pippin JW, Coombes JD, Couser WG. C5b-9 does not mediate chronic tubulointerstitial disease in the absence of proteinuria. Kidney Int. 2005;67:492–503.
Eddy AA. Interstitial nephritis induced by protein overload proteinuria. Am J Pathol. 1989;135:719–73.
Bao L, Haas M, Pippin J, Wang Y, Miwa T, Chang A, et al. Focal and segmental glomerulosclerosis induced in mice lacking decay-accelerating factor in T cells. J Clin Invest. 2009;119:1264–74.
Turnberg D, Lewis M, Moss J, Xu Y, Botto MH, Cook T. Complement activation contributes to both glomerular and tubulointerstitial damage in adriamycin nephropathy in mice. J Immunol. 2006;177:4094–102.
Matsuo S, Nishikage H, Yoshida F, Nomura A, Piddlesden SJ, Morgan BP. Role of CD59 in experimental glomerulonephritis in rats. Kidney Int. 1994;46:191–200.
Turnberg D, Botto M, Warren J, Morgan BP, Walport MJ, Cook HT. CD59a deficiency exacerbates accelerated nephrotoxic nephritis in mice. J Am Soc Nephrol. 2003;14:2271–9.
Ransohoff RM. Chemokines and chemokine receptors: standing at the crossroads of immunobiology and neurobiology. Immunity. 2009;31(5):711–21.
Vianna HR, Bouissou CMMS, Tavares MS, Teixeira MM, Simões e Silva AC. Inflamação na doença renal crônica: papel de citocinas. J Bras Nefrol. 2011;33:351–64.
Pereira AB, Rezende NA, Teixeira Junior AL, Teixeira MM, Simões e Silva AC. Citocinas e quimiocinas no transplante renal. J Bras Nefrol. 2009;31:286–96.
Vianna HR, Soares CMBM, Silveira KD, Elmiro GS, Mendes PM, Tavares MS, et al. Cytokines in chronic kidney disease: potential link of MCP-1 and dyslipidemia in glomerular diseases. Pediatr Nephrol. 2013;28:463–9.
Pereira AB, Teixeira AL, Rezende NA, Pereira RM, Miranda DM, Oliveira EA, et al. Urinary chemokines and anti-inflammatory molecules in renal transplanted patients as potential biomarkers of graft function: a prospective study. Int Urol Nephrol. 2012;44:1539–48.
Garin EH, Laflam P, Chandler L. Anti-interleukin 8 antibody abolishes effects of lipoid nephrosis cytokine. Pediatr Nephrol. 1998;12:381–5.
Souto MFO, Teixeira AL, Russo RC, Penido M-GMG, Silveira KD, Teixeira MM, Simões e Silva AC. Immune mediators in idiopathic nephrotic syndrome: evidence for a relation between interleukin 8 and proteinuria. Pediatr Res. 2008;64:637–42.
Roberts WG, Palade GE. Increased microvascular permeability and endothelial fenestration induced by vascular endothelial growth factor. J Cell Sci. 1995;108:2369–79.
Simon M, Gröne HJ, Jöhren O, Kullmer J, Plate KH, Risau W. Expression of vascular endothelial growth factor and its receptors in human renal ontogenesis and in adult kidney. Am J Physiol. 1995;268:240–50.
Webb NJA, Watson CJ, Roberts ISD, Bottomley MJ, Jones CA, Lewis MA, et al. Circulating vascular endothelial growth factor is not increased during relapses of steroid-sensitive nephrotic syndrome. Kidney Int. 1999;55:1063–71.
Laflam PF, Garin EH. Effect of tumor necrosis factor-α and vascular permeability growth factor on albuminuria in rats. Pediatr Nephrol. 2005;21:177–81.
Strehlau J, Schachter AD, Pavlakis M, Singh A, Tejani A, Strom TB. Activated intrarenal transcription of CTL-effectors and TGF-1 in children with focal segmental glomerulosclerosis. Kidney Int. 2002;61:90–5.
Ruiz-Ortega M, Lorenzo Ó, Rupérez M, Blanco J, Egido J. Systemic infusion of angiotensin II into normal rats activates nuclear factor-κB and AP-1 in the kidney role of AT1 and AT2 receptors. Am J Pathol. 2001;158:1743–56.
Wei C, El Hindi S, Li J, Fornoni A, Goes N, Sageshima J, et al. Circulating urokinase receptor (suPAR) as a cause of focal segmenter glomerulosclerosis. Nat Med. 2011;17:952–60.
Maas RJ, Deegens JK, Wetzels JF. Serum suPAR in patients with FSGS: trash or treasure? Pediatr Nephrol. 2013;28:1041–8.
Mosmann TR, Cherwinski H, Bond MW, Giedlin MA, Coffman RL. Two types of murine helper T cell clone. I. Definition according to profiles of lymphokine activities and secreted proteins. J Immunol. 1986;175:05–14.
Del Prete GF, De Carli M, Mastromauro C, Biagiotti R, Macchia D, Falagiani P, Ricci M, Romagnani S. Purified protein derivative of Mycobacterium tuberculosis and excretory-secretory antigen(s) of Toxocara canis expand in vitro human T cells with stable and opposite (type 1 T helper or type 2 T helper) profile of cytokine production. J Clin Invest. 1991;88:346–50.
Abbas AK, Murphy KM, Sher A. Functional diversity of helper T lymphocytes. Nature. 1986;383:787–93.
Hurtado A, Johnson RJ. Hygiene hypothesis and prevalence of glomerulonephritis. Kidney Int. 2005;68 (Supplement):62–7.
Odobasic D, Kitching AR, Tipping PG, Holdsworth SR. CD80 and CD86 costimulatory molecules regulate crescentic glomerulonephritis by different mechanisms. Kidney Int. 2005;68:584–94.
Lee VWS, Harris DCH. Adriamycin nephropathy: a model of focal segmental glomerulosclerosis. Nephrology. 2011;16:30–8.
Tovar AR, Murguía F, Cruz C, Hernández-Pando R, Aguilar-Salinas CA, Pedraza-Chaverri J, et al. A soy protein diet alters hepatic lipid metabolism gene expression and reduces serum lipids and renal fibrogenic cytokines in rats with chronic nephrotic syndrome. J Nutr. 2002;132:2562–9.
Kim SY, Lim AY, Jeon SK, Lee IS, Choue R. Effects of dietary protein and fat contents on renal function and inflammatory cytokines in rats with adriamycin-induced nephrotic syndrome. Mediat Inflamm. 2011; doi:10.1155/2011/945123.
Acknowledgments
This study was partially supported by CNPq (Conselho Nacional de Desenvolvimento Científico e Tecnológico, Brazil) and FAPEMIG (Fundação de Amparo à Pesquisa do Estado de Minas Gerais, Brazil) by the Grant INCT-MM (Instituto Nacional de Ciência e Tecnologia—Medicina Molecular: FAPEMIG: CBB-APQ-00075-09/CNPq 573646/2008-2). Dr. AC Simões e Silva received a research productivity grant from CNPq.
Author information
Authors and Affiliations
Corresponding author
Additional information
Responsible Editor: John Di Battista.
Rights and permissions
About this article
Cite this article
de Fátima Pereira, W., Brito-Melo, G.E.A., Guimarães, F.T.L. et al. The role of the immune system in idiopathic nephrotic syndrome: a review of clinical and experimental studies. Inflamm. Res. 63, 1–12 (2014). https://doi.org/10.1007/s00011-013-0672-6
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00011-013-0672-6