Abstract
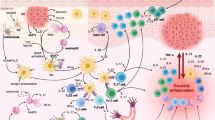
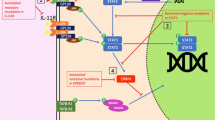
Interleukin (IL)-17 is a 30- to 35-kDa homodimeric polypeptide cytokine cloned in 1993 and originally named cytotoxic T lymphocyte-associated antigen-8 (CTLA-8). Sequencing the human genome resulted in the discovery of an additional five members of the IL-17 family that were consecutively named IL-17B to IL-17F. IL-17A is exclusively produced by a newly identified CD4+ T-helper subset that was recently named Th17. Differentiation of these cells from naïve CD4+ T cells requires both TGF-β and IL-6. IL-15 and, especially, IL-23 are required for these cells’s survival and efficient IL-17 production. IL-17 binding to an IL-17 receptor expressed on epithelial, endothelial, and fibroblastic stromal cells triggers the activation of transcription factor NF-κB and mitogen-activated protein kinase (p-38), which in turn results in the secretion of IL-1, TNF-α, IL-6, IL-8, or prostaglandin E2. The IL-17 family plays a key role in the regulation of immune and inflammatory response, in the homeostasis of several tissues, and the progression of autoimmune diseases. In addition, IL-17 exerts synergistic effects with TNF-α and IL-1 in the induction of joint inflammation and cartilage and joint destruction. Given these properties, it is not surprising that in certain pathological conditions, for example rheumatoid arthritis, Th17 cells emerge as a new pathological cell type that, by IL-17 production and release, contributes to their pathogeneses.
Similar content being viewed by others
Author information
Authors and Affiliations
Corresponding author
About this article
Cite this article
Paradowska, A., Maśliński, W., Grzybowska-Kowalczyk, A. et al. The function of interleukin 17 in the pathogenesis of rheumatoid arthritis. Arch. Immunol. Ther. Exp. 55, 329–334 (2007). https://doi.org/10.1007/s00005-007-0032-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00005-007-0032-8