Abstract
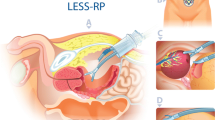
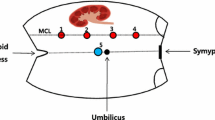
Port placement and docking of the da Vinci® Surgical System is fundamental in robotic-assisted laparoscopic radical prostatectomy (RALP). The aim of our study was to investigate learning curves for port placement and docking of robots (PPDR) in RALP. This manuscript is a retrospective review of prospectively collected data looking at PPDR in 526 patients who underwent RALP in our institute from April 2005 to May 2010. Data included patient-factor features such as body mass index (BMI), and pre-, intra- and post-operative data. Intra-operative information included operation time, subdivided into anesthesia, PPDR and console times. 526 patients underwent RALP, but only those in whom PPDR was performed by the same surgeon without laparoscopic and robotic experience (F.D.M.) were studied, totalling 257 cases. The PPDR phase revealed an evident learning curve, comparable with other robotic phases. Efficiency improved until approximately the 60th case (P < 0.001), due more to effective port placement than to docking of robotic arms. In our experience, conversion to open surgery is so rare that statistical evaluation is not significant. Conversion due to robotic device failure is also very rare. This study on da Vinci procedures in RALP revealed a learning curve during PPDR and throughout the robotic-assisted procedure, reaching a plateau after 60 cases.



Similar content being viewed by others
References
Heidenreich A, Aus G, Bolla M, Joniau S, Matveev VB, Schmid HP, Zattoni F (2008) EAU guidelines on prostate cancer. Eur Urol 53:68–80
Boccon-Gibod L (2006) Radical prostatectomy: open? Laparoscopic? Robotic? Eur Urol 49:598–609
Binder J, Kramer W (2001) Robotically-assisted laparoscopic radical prostatectomy. BJU Int 87:408–410
Artibani W, Grosso G, Novara G, Pecoraro G, Sidoti O, Sarti A, Ficarra V (2003) Is laparoscopic radical prostatectomy better than traditional retropubic radical prostatectomy? An analysis of peri-operative morbidity in two contemporary series in Italy. Eur Urol 44:401–406
Rassweiler J, Hruza M, Teber D, Su LM (2006) Laparoscopic and robotic assisted radical prostatectomy—critical analysis of the results. Eur Urol 49:612–624
Savera AT, Kaul S, Badani K, Stark AT, Shah NL, Menon M (2006) Robotic radical prostatectomy with the “veil of aphrodite” technique: histologic evidence of enhanced nerve sparing. Eur Urol 49:955–957
Ficarra V, Cavalleri S, Novara G, Aragona M, Artibani W (2007) Evidence from robot-assisted laparoscopic radical prostatectomy: a systematic review. Eur Urol 51:45–55
Ficarra V, Novara G, Fracalanza S, D’Elia C, Secco S, Iafrate M, Cavalleri S, Artibani W (2009) A prospective, non-randomized trial comparing robot-assisted laparoscopic and retropubic radical prostatectomy in one European institution. BJU Int 104:534–539
Menon M, Shrivastava A, Bhandari M, Satyanarayana R, Siva S, Agarwal PK (2009) Vattikuti Institute prostatectomy: technical modifications in 2009. Eur Urol 56:89–96
Pasticier G, Rietbergen JB, Guillonneau B, Fromont G, Menon M, Vallancien G (2001) Robotically assisted laparoscopic radical prostatectomy: feasibility study in men. Eur Urol 40:70–74
Guillonneau B (2005) Should we consider testing for skill in surgery? Eur Urol 47:480–481
Chang L, Satava RM, Pellegrini CA, Sinanan MN (2003) Robotic surgery: identifying the learning curve through objective measurement of skill. Surg Endosc 17:1744–1748
Kaul S, Shah NL, Menon M (2006) Learning curve using robotic surgery. Curr Urol Rep 7:125–129
Kumar U, Gill IS (2006) Learning curve in human laparoscopic surgery. Curr Urol Rep 7:120–124
Prasad SM, Maniar HS, Soper NJ, Damiano RJ Jr, Klingensmith ME (2002) The effect of robotic assistance on learning curves for basic laparoscopic skills. Am J Surg 183:702–707
Yohannes P, Rotariu P, Pinto P, Smith AD, Lee BR (2002) Comparison of robotic versus laparoscopic skills: is there a difference in the learning curve? Urology 60:39–45 [discussion 45]
Seymour NE, Gallagher AG, Roman SA, O’Brien MK, Bansal VK, Andersen DK, Satava RM (2002) Virtual reality training improves operating room performance: results of a randomized, double-blinded study. Ann Surg 236:458–463
Dindo D, Demartines N, Clavien PA (2004) Classification of surgical complications. A new proposal with evaluation in a cohort of 6336 patients and results of a survey. Ann Surg 240:205–213
Van Appledorn S, Bouchier-Hayes D, Agarwal D, Costello AJ (2006) Robotic laparoscopic radical prostatectomy: setup and procedural techniques after 150 cases. Urology 67:364–367
Martina GR, Giumelli P, Scuzzarella S, Remotti M, Caruso G, Lovisolo J (2005) Laparoscopic extraperitoneal radical prostatectomy—learning curve of a laparoscopy-naive urologist in a community hospital. Urology 65:959–963
Menon M, Shrivastava A, Tewari A, Sarle R, Hemal A, Peabody JO, Vallancien G (2002) Laparoscopic and robot assisted radical prostatectomy: establishment of a structured program and preliminary analysis of outcomes. J Urol 168:945–949
Menon M, Tewari A, Baize B, Guillonneau B, Vallancien G (2002) Prospective comparison of radical retropubic prostatectomy and robot-assisted anatomic prostatectomy: the Vattikuti Urology Institute experience. Urology 60:864–868
Touijer K, Guillonneau B (2006) Teaching laparoscopic urologic oncology. The Memorial Sloan-Kettering Center experience. Actas Urol Esp 30:464–468
Stelzer MK, Abdel MP, Sloan MP, Gould JC (2009) Dry lab practice leads to improved laparoscopic performance in the operating room. J Surg Res 154:163–166
Lehnert M, Richter B, Beyer PA, Heller K (2006) A prospective study comparing operative time in conventional laparoscopic and robotically assisted Thal semifundoplication in children. J Pediatr Surg 41:1392–1396
Delaney CP, Lynch AC, Senagore AJ, Fazio VW (2003) Comparison of robotically performed and traditional laparoscopic colorectal surgery. Dis Colon Rectum 46:1633–1639
Murphy DG, Bjartell A, Ficarra V, Graefen M, Haese A, Montironi R, Montorsi F, Moul JW, Novara G, Sauter G, Sulser T, van der Poel H (2010) Downsides of robot-assisted laparoscopic radical prostatectomy: limitations and complications. Eur Urol 57:735–746
Herman MP, Raman JD, Dong S, Samadi D, Scherr DS (2007) Increasing body mass index negatively impacts outcomes following robotic radical prostatectomy. JSLS 11:438–442
Cestari A, Buffi NM, Scapaticci E, Lughezzani G, Salonia A, Briganti A, Rigatti P, Montorsi F, Guazzoni G (2010) Simplifying patient positioning and port placement during robotic-assisted laparoscopic prostatectomy. Eur Urol 57:530–533
Pick DL, Lee DI, Skarecky DW, Ahlering TE (2004) Anatomic guide for port placement for daVinci robotic radical prostatectomy. J Endourol 18:572–575
Conflict of interest
None.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Dal Moro, F., Secco, S., Valotto, C. et al. Specific learning curve for port placement and docking of da Vinci® Surgical System: one surgeon’s experience in robotic-assisted radical prostatectomy. J Robotic Surg 6, 323–327 (2012). https://doi.org/10.1007/s11701-011-0315-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11701-011-0315-2