Abstract
Introduction
Studies assessing outcomes between laparoscopic and robotic bariatric metabolic surgery (BMS) have been limited by the relatively small percentage of robotic cases. However, in recent years, the number of robotic BMS cases has doubled. We report the largest US study comparing robotic versus laparoscopic outcomes in BMS over the longest time period (5 years).
Methods
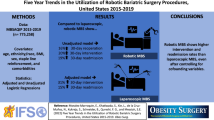
Analysis of the MBSAQIP database was undertaken. This included information on 791,423 patients from 2015–2019 in the USA. Within this retrospective case–control study, 13.7% of SG and 16.6% of RYGB cases were done robotically.
Setting
USA, MBSAQIP database.
Results
Robotic BMS increased mean operative time by 26 min for SG and 40 min for RYGB. However, this did not increase the 30-day venous thromboembolism (VTE) or organ dysfunction complications between the 2 groups. Robotic SG had slightly higher risks of multiple infectious complications (OR 1.26 to 1.76). Robotic RYGB had slightly lower infectious complications and transfusion requirements. Robotic BMS had higher 30-day readmission rates and 30-day reoperative rates for both SG and RYGB.
Conclusions
Both robotic SG and RYGB were found to have significantly longer operative times than laparoscopic SG and RYGB. Potential outcome benefits from robotic BMS can include a reduction in infectious complications and transfusion requirements with robotic RYGB cases. SGs were found to have slightly higher infectious complications.
Graphical abstract



Similar content being viewed by others
References
“Adult Obesity Facts.” Centers for Disease Control and Prevention, Centers for Disease Control and Prevention, 30 Sept. 2021, https://www.cdc.gov/obesity/data/adult.html. Accessed 15 Mar 2022.
Wilson EB, Sudan R. The evolution of robotic bariatric surgery. World J Surg. 2013;37(12):2756–60. https://doi.org/10.1007/s00268-013-2125-3.
Buchs NC, Pugin F, Azagury DE, et al. Robotic revisional bariatric surgery: a comparative study with laparoscopic and open surgery. Int J Med Robot Comput Assist Surg. 2014;10(2):213–7. https://doi.org/10.1002/rcs.1549.
Bailey JG, et al. Robotic versus laparoscopic Roux-en-Y gastric bypass in obese adults ages 18 to 65 years: a systematic review and economic analysis. Surg Endosc. 2014;28:414–26. https://doi.org/10.1007/s00464-013-3217-8.
Li K, et al. Robotic versus laparoscopic bariatric surgery: a systematic review and meta-analysis. Obes Surg. 2016;26:3031–44. https://doi.org/10.1007/s11695-016-2408-5.
Alizadeh RF, et al. Robotic versus laparoscopic sleeve gastrectomy: a MBSAQIP analysis. Surg Endosc. 2018;33:917–22. https://doi.org/10.1007/s00464-018-6387-6.
Rogula T, et al. Does robotic Roux-en-Y gastric bypass provide outcome advantages over standard laparoscopic approaches? Obes Surg. 2018;28(9):2589–96. https://doi.org/10.1007/s11695-018-3228-6.
Smeenk RM, Van’t Hof G, Elsten E, et al. The results of 100 robotic versus 100 laparoscopic gastric bypass procedures: a single high volume centre experience. Obes Surg. 2016;26:1266–73. https://doi.org/10.1007/s11695-015-1933-y.
Ahmad A, Carleton JD, Ahmad ZF, et al. Laparoscopic versus robotic-assisted Roux-en-Y gastric bypass: a retrospective, single-center study of early perioperative outcomes at a community hospital. Surg Endosc. 2016;30:3792–6. https://doi.org/10.1007/s00464-01.
Wood MH, et al. A comparison of outcomes between the traditional laparoscopic and totally robotic Roux-en-Y gastric bypass procedures. J Robotic Surg. 2014;8:29–34. https://doi.org/10.1007/s11701-013-0416-1.
Moon RC, et al. Robotic Roux-en-Y Gastric Bypass, is it safer than laparoscopic bypass? Obes Surg. 2016;26:1016–20. https://doi.org/10.1007/s11695-015-1884-3.
Sebastian R, Howell MH, Chang KH, et al. Robot-assisted versus laparoscopic Roux-en-Y gastric bypass and sleeve gastrectomy: a propensity score-matched comparative analysis using the 2015 = 2016 MBSAQIP database. Surg Endosc. 2018;33(5):1600–12. https://doi.org/10.1007/s00464-018-6422-7.
Magouliotis DE, Tasiopoulou VS, Sioka E, et al. Robotic versus laparoscopic sleeve gastrectomy for morbid obesity: a systematic review and meta-analysis. Obes Surg. 2017;17(1):245–53. https://doi.org/10.1007/s11695-016-2444-1.
Acevedo E Jr, Mazzei M, Zhao H, et al. Outcomes in conventional laparoscopic versus robotic-assisted primary bariatric surgery: a retrospective, case–controlled study of the MBSAQIP database. Surg Endosc. 2019;34(3):1353–65. https://doi.org/10.1007/s00464-019-06915-7.
Tatarian T, Yang J, Wang J, et al. Trends in the utilization and perioperative outcomes of primary robotic bariatric surgery from 2015 to 2018: a study of 46,764 patients from the MBSAQIP data, egistry. Surg Endosc. 2020;35(7):3915–22. https://doi.org/10.1007/s00464-020-07839-3.
Dudash M, Kuhn J, Dove J, et al. The longitudinal efficiency of robotic surgery: an MBSAQIP propensity matched 4-year comparison of robotic and laparoscopic bariatric surgery. Obes Surg. 2020;30(10):3706–13. https://doi.org/10.1007/s11695-020-04712-z.
Pokala B, Samuel S, Yanala U, et al. Elective robotic-assisted bariatric surgery: Is it worth the money? A national database analysis. Am J Surg. 2020;220(6):1445–50. https://doi.org/10.1016/j.amjsurg.2020.08.040.
Chao GF, Montgomery JR, Abou Azar S, et al. Venous thromboembolism: risk factors in the sleeve gastrectomy era. Surg Obes Relat Dis. 2021;17(11):1905–11. https://doi.org/10.1016/j.soard.2021.06.022.
Dreifuss NH, Mangano A, Hassan C, et al. Robotic revisional bariatric surgery: a high-volume center experience. Obes Surg. 2021;31(4):1656–63. https://doi.org/10.1007/s11695-020-05174-z.
Ayloo SM, Choudhury N. Robotic revisional bariatric surgery: single-surgeon case series. Int J Med Robot Comput Assist Surg. 2015;11(3):284–9. https://doi.org/10.1002/rcs.1622.
“Prospective Robotic-Assisted Revisional Bariatric Study - Full Text View.” Full Text View - ClinicalTrials.gov, https://clinicaltrials.gov/ct2/show/NCT04506190. Accessed 15 Mar 2022.
Kim MS, Kim WJ, Hyung WJ, et al. Comprehensive learning curve of robotic surgery: discovery from a multicenter prospective trial of robotic gastrectomy. Ann Surg. 2019;273(5):949–56. https://doi.org/10.1097/SLA.0000000000003583.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Statement of Informed Consent
This study was determined not to meet the criteria for human subject research. As such, informed consent was not obtained from patients for this MBSAQIP database review.
Statement of Human and Animal Rights
No human or animal subjects were used for research.
Conflict of Interest
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Key Points
• From 2015 to 2019 the percentage of SG and RYGB done laparoscopically has been decreasing. Over the same time period the percentage of these surgeries done robotically has doubled.
• Robotic SG and RYGB are associated with significantly longer operative times than the laparoscopic counterparts.
• Robotic SG is associated with higher risk for infectious complications.
• Robotic RYGB is associated with lower infectious complications and transfusion requirements.
• Patients have a higher 30-day readmissions and reoperations for both robotic SG and RYGB
Rights and permissions
About this article
Cite this article
Wesley Vosburg, R., Haque, O. & Roth, E. Robotic vs. Laparoscopic Metabolic and Bariatric Surgery, Outcomes over 5 Years in Nearly 800,000 Patients. OBES SURG 32, 2341–2348 (2022). https://doi.org/10.1007/s11695-022-06082-0
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11695-022-06082-0



