Abstract
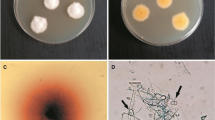
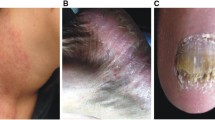
A 74-year-old healthy Japanese man had noticed an itchy lesion with two tiny thick brown scales on the fourth interdigital web of his right foot 3 months earlier. The brown fungus isolated from the scales had demonstrated brown, ellipsoidal, obovoid or clavate, 3-septate conidia. Morphologically, the fungus was identified as Curvularia sp., and was differentiated from other human pathogenic species of the genus, such as C. lunata, C. pallescens, C. trifolii, C. clavata, and C. brachyspora, by molecular analysis based on the DNA sequence data. The fungus grows well on keratotic materials (hairs, nails, and callus), which indicates that it might have the ability to infect the skin surface.









Similar content being viewed by others
References
Agrawal A, Singh SM (1995) Two cases of cutaneous phaeohyphomycosis caused by Curvularia pallescens. Mycoses 38:301–303
Anbu P, Gopinath SCB, Hilda A, Mathivanan N, Annadural G (2006) Secretion of keratinolytic enzymes and keratinolysis by Scopulariopsis brevicaulis and Trichophyton mentagrophytes: regression analysis. Can J Microbiol 52:1060–1069
Barde AK, Singh SM (1983) A case of onychomycosis caused by Curvularia lunata (Wakker) Boedijn. Mykosen 26:311–316
Berbee ML, Pirseyedi M, Hubbard S (1999) Cochliobolus phylogenetics and the origin of known, highly virulent pathogens, inferred from ITS and glyceraldehyde-3-phosphate dehydrogenase gene sequences. Mycologia 91:964–977
Berg D, Garcia JA, Schell WA, Perfect JR, Murray JC (1995) Cutaneous infection caused by Curvularia pallescens: a case report and review of the spectrum of disease. J Am Acad Dermatol 32:375–378
Bonduel M, Santos P, Turienzo CF, Chantada G, Paganini H (2001) Atypical skin lesions caused by Curvularia sp. and Pseudallescheria boydii in two patients after allogeneic bone marrow transplantation. Bone Marrow Transplant 27:1311–1313
de Hong GS, Guarro J, Gene J, Figueras MJ (2000) Atlas of clinical fungi, 2nd edn. CBS, Utrecht
Duvic M, Lowe L, Rios A, MacDonald E, Vance P (1987) Superficial phaeohyphomycosis of the scrotum in a patient with the acquired immunodeficiency syndrome. Arch Dermatol 123:1597–1599
Ellis MB (1966) Dematiaceous Hyphomycetes. VII: Curvularia, Brachysporium, etc. Mycol Pap 106:1–57
Fan YM, Huang WM, Li SF, Wu GF, Li W, Chen RY (2008) Cutaneous phaeohyphomycosis of foot caused by Curvularia clavata. Mycoses 52:544–546
Fernandez M, Noyola DE, Rossmann SN, Edwards MS (1999) Cutaneous phaeohyphomycosis caused by Curvularia lunata and a review of Curvularia infection in pediatrics. Pediatr Infect Dis J 18:727–731
Garg A, Sujatha S, Parija Garg J, SC Thappa DM (2008) Eumycetoma due to Curvularia lunata. Indian J Dermatol Venereol Leprol 74:515–516
Grieshop TJ, Yarbrough D III, Farrar WE (1993) Case report: phaeohyphomycosis due to Curvularia lunata involving skin and subcutaneous tissue after an explosion at a chemical plant. Am J Med Sci 305:387–389
Gugnani HC, Okeke CN, Sivanesan A (1990) Curvularia clavata as an aetiological agent of human skin infection. Lett Appl Microbiol 10:47–49
Harris JJ, Downham TF II (1978) Unusual fungal infections associated with immunologic hyporeactivity. Int J Dermatol 17:323–330
Hiromoto A, Nagano T, Nishigori C (2008) Cutaneous infection caused by Curvularia species in an immunocompetent patient. Br J Dermatol 158:1374–1375
Kamalam A, Ajithadass K, Sentamilselvi G, Thambiah AS (1992) Paronychia and black discoloration of a thumb nail caused by Curvularia lunata. Mycopathologia 118:83–84
Kiryu H, Suenaga Y (1985) A case of cutaneous Curvularia infection caused by Curvularia trifolii. In: Fukushiro R, Kagawa S, Kitamura K (eds) Typical cutaneous fungus disease—rare case (in Japanese). Proceedings of the 37th meeting of Japanese Society of Medical Mycology, Yokohama, pp 63–66
Lavoie SR, Espinel–Ingroff A, Kerkering T (1993) Mixed cutaneous phaeohyphomycosis in a cocaine user. Clin Infect Dis 17:114–116
Lopes JO, Jobim NM (1998) Dermatomycosis of the toe web caused by Curvularia lunata. Rev Inst Med Trop Sao Paulo 40:327–328
Mahgoub ES (1973) Mycetomas caused by Curvularia lunata, Madurella crisea, Aspergillus nidulans, and Nocardia brasiliensis in Sudan. Sabouraudia 11:179–182
Marcondes ND, Taira CL, Vandresen DC, Svidzinski TIE, Kadowaki MK, Peralta RM (2008) New feather-degrading filamentous fungi. Microb Ecol 56:13–17
Muhsin TM, Salih TH (2000) Exocellular enzyme activity of dermatophytes and other fungi isolated from ruminants in Southern Iraq. Mycopathologia 150:49–52
Rinaldi MG, Phillips P, Schwartz JG, Winn RE, Holt GR, Shagets FW, Elrod J, Nishioka G, Aufdemorte TB (1987) Human Curvularia infections: report of five cases and review of the literature. Diagn Microbiol Infect Dis 6:27–39
Rohwedder JJ, Simmons JL, Colfer H, Gatmaitan B (1979) Disseminated Curvularia lunata infection in a football player. Arch Intern Med 139:940–941
Sivanesen A (1987) Graminicolous species of Bipolaris, Curvularia, Drechslera, Exserohilum and their teleomorphs. Mycol Pap 158:1–261
Still JM Jr, Law EJ, Pereira GI, Singletary E (1993) Invasive burn wound infection due to Curvularia species. Burns 19:77–79
Swofford DL (2005) PAUP*. Phylogenetic analysis using parsimony (*and other methods), version 4. Sinauer Associates, Sunderland
Tamaki A, Nagano T, Nishikiori T (2006) A case of cutaneous phaeohyphomycosis caused by Curvularia sp. (in Japanese). Jpn J Dermatol 116:841
Tessari G, Formi A, Ferretto R, Solbiati M, Faggian G, Mazzucco A, Barba A (2003) Lethal systemic dissemination from a cutaneous infection due to Curvularia lunata in a heart transplant recipient. J Eur Acad Dermatol Venereol (JEADV) 17:440–442
Torda AJ, Jones PD (1997) Necrotizing cutaneous infection caused by Curvularia brachyspora in an immunocompetent host. Aust J Dermatol 38:85–87
White TJ, Bruns T, Lee S, Taylor J (1990) Amplification and direct sequencing of fungal ribosomal RNA genes for phylogenetics. In: Innis MA, Gelfand DH, Sninsky JJ, White TJ (eds) PCR protocols: a guide to methods and applications. Academic Press, New York, pp 315–322
Yvonne CW, de Nanassy J, Summerbell RC, Matlow AG, Richardson SE (1994) Fungal sternal wound infection due to Curvularia lunata in a neonate with congenital heart disease: case report and review. Clin Infect Dis 19:735–740
Acknowledgment
We thank Dr. M. Tuda (Professor Emeritus, Kyoto University, Japan) for his valuable comments on the morphological identification.
Author information
Authors and Affiliations
Corresponding author
About this article
Cite this article
Yanagihara, M., Kawasaki, M., Ishizaki, H. et al. Tiny keratotic brown lesions on the interdigital web between the toes of a healthy man caused by Curvularia species infection and a review of cutaneous Curvularia infections. Mycoscience 51, 224–233 (2010). https://doi.org/10.1007/s10267-009-0030-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10267-009-0030-2