Abstract
Background
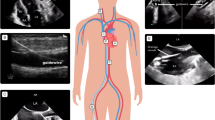
The American Society of Anesthesiologists (ASA) has published practice guidelines for the use of perioperative transesophageal echocardiography (TEE) but the role and impact of TEE performed by anesthesiologists outside the cardiac operating room (OR) is still poorly explored. We report our experience in the use of TEE in the noncardiac OR, the recovery room and in the intensive care unit (ICU) in a university hospital, and analyze the impact of TEE on clinical decision making.
Methods
Two hundred fourteen patients were included and TEE indications were classified prospectively according to the ASA guidelines. The examinations and data sheets were reviewed by two anesthesiologists with advanced training in TEE. For each examination, it was noted if TEE altered the management according to five groups: 1) changing medical therapy; 2) changing surgical therapy; 3) confirmation of a diagnosis; 4)positioning of an intravascular device; and 5) TEE used as a substitute to a pulmonary artery catheter.
Results
Eighty-nine (37%), 67 (31%) and 58 (27%) patients had category I, II and III indications. The impact was more significant in category I where TEE altered therapy 60% of the time compared with 31% and 21% for categories II and III (P < 0.001). The most frequent reason for changing management was a modification in medical therapy in 53 instances (45%).
Conclusion
Our results confirm a greater impact of TEE performed by anesthesiologists on clinical management for category I compared to category II and III indications in the noncardiac OR surgical setting and in the ICU.
Résumé
Contexte
L’American Society of Anesthesiologists (ASA) a publié lelignes directrices pour l’utilisation périopératoire de l’échocardiographie transœsophagienne (ETO), mais le rôle et l’impact de l’ETO réalisée par les anesthésiologistes à l’extérieur de la salle d’opération (SO) sont encore peu connus. Nous présentons notre expérience de l’usage de l’ETO dans une SO non cardiaque, dans la salle de réveil et à l’unité des soins intensifs (USI) d’un hôpital universitaire. Aussi, nous analysons l’impact de l’ETO sur la prise de décision en clinique.
Méthode
Deux cent quatorze sujets ont participé à l’étude et les indications d’ETO ont été classifiées prospectivement selon les lignes directrices de l’ASA. Les examens et les fiches techniques ont été passées en revue par deux anesthésiologistes de formation avancée en ETO. Pour chaque examen, on a noté si l’ETO modifiait le traitement en regard de cinq groupes: 1) modification de la thérapie médicale 2) modification de la thérapie chirurgicale 3) confirmation du diagnostic 4) installation d’une sonde intravasculaire 5) usage de l’ETO comme substitut d’un cathéter artériel pulmonaire.
Résultats
Quatre-vingt-neuf (37 %), 67 (31 %) et 58 (27 %) patients présentaient des indications de catégorie I, II et III. L’ETO a eu un impact plus significatif pour la catégorie I où elle modifiait la thérapie dans 60 % des cas comparativement à 31 % et à 21 % pour les catégories II et III (P < 0,001). C’est la modification de la thérapie médicale qui apparaît comme la raison principale de changement du traitement avec 53 cas (45 %).
Conclusion
Nos résultats confirment une plus grande répercussion de l’ETO réalisé par les anesthésiologistes sur le traitement clinique pour les indications de catégorie I comparées à celles de catégories II et III dans le contexte chirurgical d’une SO non cardiaque et de l’USI.
Article PDF
Similar content being viewed by others
References
American Society of Anesthesiologists and the Society of Cardiovascular Anesthesiologists Task Force on Transesophageal Echo cardiography. Practice guidelines for perioperative transesophageal echocardiography. A report by the American Society of Anesthesiologists and the Society of Cardiovascular Anesthesiologists Task Force on Transesophageal Echocardiography. Anesthesiology 1996; 84: 986–1006.
Suriani RJ, Neustein S, Shore-Lesserson L, Konstadt S. Intraoperative transesophageal echocardiography during noncardiac surgery. J Cardiothorac Vasc Anesth 1998; 12: 274–80.
Kolev N, Brase R, Swanevelder J, et al. The influence of transoesophageal echocardiography on intraoperative decision making. A European multicentre study. European Perioperative TOE Research Group. Anaesthesia 1998; 53: 767–73.
McLean AS. Transoesophageal echocardiography in the intensive care unit. Anaesth Intensive Care 1998; 26: 22–5.
Couture P, Denault AY, McKenty S, et al. Impact of routine use of intraoperative transesophageal echocardiography during cardiac surgery. Can J Anesth 2000; 47: 20–6.
Bernard F, Denault A, Babin D, et al. Diastolic dysfunction is predictive of difficult weaning from cardiopulmonary bypass. Anesth Analg 2001; 92: 291–8.
Couture P, Denault AY, Carignan S, Boudreault D, Babin D, Ruel M. Intraoperative detection of segmental wall motion abnormalities with transesophageal echocardiography. Can J Anesth 1999; 46: 827–31.
Girard F, Couture P, Boudreault D, Normandin L, Denault A, Girard D. Estimation of the pulmonary capillary wedge pressure from transesophageal pulsed Doppler echocardiography of pulmonary venous flow: influence of the respiratory cycle during mechanical ventilation. J Cardiothorac Vasc Anesth 1998; 12: 16–21.
Brandt RR, Oh JK, Abel MD, Click RL, Orszulak TA, Seward JB. Role of emergency intraoperative transesophageal echocardiography. J Am Soc Echocardiogr 1998; 11: 972–7.
Font VE, Obarski TP, Klein AL, et al. Transesophageal echocardiography in the critical care unit. Cleve Clin J Med 1991; 58: 315–22.
Foster E, Schiller NB. The role of transesophageal echocardiography in critical care: UCSF experience. J Am Soc Echocardiogr 1992; 5: 368–74.
Chenzbraun A, Pinto FJ, Schnittger I. Transesophageal echocardiography in the intensive care unit: impact on diagnosis and decision-making. Clin Cardiol 1994; 17: 438–44.
Oh JK, Seward JB, Khandheria BK, et al. Transesophageal echocardiography in critically ill patients. Am J Cardiol 1990; 66: 1492–5.
Pearson AC, Castello R, Labovitz AJ. Safety and utility of transesophageal echocardiography in the critically ill patient. Am Heart J 1990; 119: 1083–9.
Hwang JJ, Shyu KG, Chen JJ, Tseng YZ, Kuan P, Lien WP. Usefulness of transesophageal echocardiography in the treatment of critically ill patients. Chest 1993; 104: 861–6.
Alam M. Transesophageal echocardiography in critical care units: Henry Ford Hospital experience and review of the literature. Prog Cardiovasc Dis 1996; 38: 315–28.
Reichert CL, Visser CA, Koolen JJ, et al. Transesophageal echocardiography in hypotensive patients after cardiac operations. Comparison with hemodynamic parameters. J Thorac Cardiovasc Surg 1992; 104: 321–6.
Puybasset L, Saada M, Catoire P, Bonnet F. Contribution of transesophageal echocardiography in intensive care: a prospective assessment (French). Ann Fr Anesth Réanim 1993; 12: 17–21.
Khoury AF, Afridi I, Quinones MA, Zoghbi WA. Transesophageal echocardiography in critically ill patients: feasibility, safety, and impact on management. Am Heart J 1994; 127: 1363–71.
Vignon P, Mentec H, Terre S, Gastinne H, Gueret P, Lemaire F. Diagnostic accuracy and therapeutic impact of transthoracic and transesophageal echocardiography in mechanically ventilated patients in the ICU. Chest 1994; 106: 1829–34.
Gorcsan J 3rd, Edwards TD, Ziady GM, Katz WE, Griffith BP. Transesophageal echocardiography to evaluate patients with severe pulmonary hypertension for lung transplantation. Ann Thorac Surg 1995; 59: 717–22.
Heidenreich PA, Stainback RF, Redberg RF, Schiller NB, Cohen NH, Foster E. Transesophageal echocardiography predicts mortality in critically ill patients with unexplained hypotension. J Am Coll Cardiol 1995; 26: 152–8.
Sohn DW, Shin GJ, Oh JK, et al. Role of transesophageal echocardiography in hemodynamically unstable patients. Mayo Clin Proc 1995; 70: 925–31.
Cicek S, Demirilic U, Kuralay E, Tatar H, Ozturk O. Transesophageal echocardiography in cardiac surgical emergencies. J Card Surg 1995; 10: 236–44.
Poelaert JI, Trouerbach J, De Buyzere M, Everaert J, Colardyn FA. Evaluation of transesophageal echocardiography as a diagnostic and therapeutic aid in a critical care setting. Chest 1995; 107: 774–9.
Suriani RJ, Cutrone A, Feierman D, Konstadt S. Intraoperative transesophageal echocardiography during liver transplantation. J Cardiothorac Vasc Anesth 1996; 10: 699–707.
Slama MA, Novara A, Van de Putte P, et al. Diagnostic and therapeutic implications of transesophageal echocardiography in medical ICU patients with unexplained shock, hypoxemia, or suspected endocarditis. Intensive Care Med 1996; 22: 916–22.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Denault, A.Y., Couture, P., McKenty, S. et al. Perioperative use of transesophageal echocardiography by anesthesiologists: Impact in noncardiac surgery and in the intensive care unit. Can J Anesth 49, 287–293 (2002). https://doi.org/10.1007/BF03020529
Accepted:
Issue Date:
DOI: https://doi.org/10.1007/BF03020529