Abstract
Purpose
To compare the effect on the incidence of motor block by reducing the concentration of ropivacaine from 0.2% to 0. 125% in parturient-controlled epidural analgesia (PCEA) for labour.
Methods
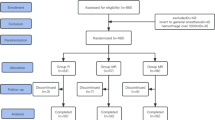
Randomized, controlled and double-blind trial involving parturients in early labour who received demand-only PCEA regimen (bolus 5 ml, lockout 10 min, maximum volume per hour of 20 ml) with either 0.2% (R0.2 group, n = 25) or 0. 125% (R0. 125 group, n=25) ropivacaine. Pain scores, the degree of motor block, the rate of drug consumption, the proportion of good to total PCEA demands and the overall satisfaction scores were documented,
Results
Fewer parturients in the R0. 125 group had lower limb motor block (4 vs 11, P < 0.05) although the degree of block was mild in all the affected parturients. The ratio of good to total PCEA demands was more favourable in the R0.2% group (median 0.72 vs 0.52, P < 0.01) although the hourly rate of ropivacaine consumption, the degree of pain relief, the maternal-fetal outcome and the overall satisfaction scores were similar. Conclusion: Both ropivacaine 0.2% and 0. 125% provided comparably effective analgesia but motor block occurred more commonly in the 0.2% group.
Résumé
Objectif
Comparer l’effet, sur l’incidence du blocage moteur, de la réduction de la concentration de ropivacaïne de 0,2 % à 0, 125 % pendant l’analgésie épidurale contrôlée par la patiente (AECP) en travail obstétrical.
Méthode
On a procédé à un essai randomisé, contrôlé et à double inconnu auprès de parturientes, au début de leur travail, qui ont reçu un régime d’AECP sur demande seulement (un bolus de 5 ml, une période réfractaire de 10 min, un volume maximal de 20 ml à l’heure) avec, soit de la ropivacaïne à 0,2 % (groupe R0.2, n = 25), soit à 0, 125 % (groupe R0. 125, n = 25). On a documenté: les scores de douleur, l’intensité du blocage moteur, la fréquence de la prise de médicament, la proportion de demandes efficaces sur les demandes totales d’AECP et l’indice de satisfaction globale.
Résultats
Peu de patientes du groupe R0. 125 ont eu un blocage moteur des membres inférieurs (4 vs 11, P < 0,05) bien que le blocage n’ait pas été important chez les parturientes touchées. La proportion de demandes efficaces sur les demandes totales d’AECP a été meilleure dans le groupe R0.2 % (médiane de 0,72 vs 0,52, P < 0,01), mais la fréquence horaire de consommation de ropivacaïne, le degré de soulagement de la douleur, l’évolution fœto-maternelle et la satisfaction globale ont été similaires.
Conclusion
La ropivacaïne 0,2 % et 0, 125 % produisent des effets analgésiques comparables, mais le blocage moteur survient plus souvent avec une concentration de 0,2 %.
Article PDF
Similar content being viewed by others
References
Eddleston JM, Holland JJ, Griffin RP, Corbett A, Horsman EL, Reynolds F. A double-blind comparison of 0.25% ropivacaine and 0.25% bupivacaine for extradural analgesia in labour. Br J Anaesth 1996; 76: 66–71.
Stienstra R, Jonker TA, Bourdrez P, Kuijpers JC, van Kleef JW, Lundberg U. Ropivacaine 0.25% versus bupivacaine 0.25% for continuous epidural analgesia in labor: a double-blind comparison. Anesth Analg 1995; 80: 285–9.
Sia AT, Chong JL. Epidural 0.2% ropivacaine for labour analgesia: parturient-controlled or continuous infusion? Anaesth Intensive Care 1999; 27: 154–8.
Cusick JF, Myklebust JB, Abram SE, Davidson A. Altered neural conduction with epidural bupivacaine. Anesthesiology 1982; 57: 31–6.
Liu SS, Moore JM, Luo AM, Trautman WJ, Carpenter RL. Comparison of three solutions of ropivacaine/fentanyl for postoperative patient-controlled epidural analgesia. Anesthesiology 1999; 90: 727–33.
Christiaens F, Verborgh C, Dierick A, Camu F. Effects of diluent volume of single dose of epidural bupivacaine in parturients during the first stage of labor. Reg Anesth Pain Med 1998; 23: 134–41.
Owen MD, D’Angela R, Geranchar JC, et al. 0.125% ropivacaine is similar to 0.125% bupivacaine for labor analgesia using patient-controlled epidural infusion. Anesth Analg 1998; 86: 527–31.
Paech MJ. Patient-controlled epidural analgesia in obstetrics. Int J Obstet Anesth 1996; 5: 115–25.
Ferrante FM, Rosinia FA, Gordon C, Datta S. The role of continuous background infusions in patientcontrolled epidural analgesia for labor and delivery. Anesth Analg 1994; 79: 80–4.
Gambling DR, Huber CJ, Berkowitz J, et al. Patient-controlled epidural analgesia in labour: varying bolus dose and lockout interval. Can J Anaesth 1993; 40: 211–7.
Gambling DR, Yu P, Cole C, McMorland GH, Palmer L. A comparative study of patient controlled analgesia (PCEA) and continuous infusion epidural analgesia (CIEA) in labour. Can J Anaesth 1988; 35: 249–54.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Sia, A.TH., Ruban, P., Chong, J.L. et al. Motor blockade is reduced with ropivacaine 0.125% for parturient-controlled epidural analgesia during labour. Can J Anesth 46, 1019–1023 (1999). https://doi.org/10.1007/BF03013195
Accepted:
Issue Date:
DOI: https://doi.org/10.1007/BF03013195