Abstract
Objective
To assess the effect of changes in tidal volume (V T) with a constant inspiratory flow and minute ventilation\((\dot V_E )\) on gas exchange and oxygen transport in acute respiratory distress syndrome (ARDS).
Design
A crossover study of threeV T in two study groups, using patients as their own controls.Setting: A medical-surgical intensive care unit in a tertiary care center.
Patients
Eight patients with ARDS and seven postoperative cardiac surgery patients with uncomplicated recoveries were studied during volume-controlled mechanical ventilation.
Interventions
During controlled mechanical ventilation, patients were first ventilated with aV T of 9–11 ml/kg.V T was then increased to 12–14 ml/kg (+25%) for 30 min and subsequently decreased to 6–8 ml/kg (−25%) for 30 min by adjusting the respiratory rate (RR) while the inspiratory flow rate,\(\dot V_E \), and inspiratory duty cycle (TL/TTOT) were kept constant. At the end, patients were ventilated with the baseline settings for another 30 min.
Measurements and results
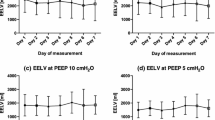
V E, carbon dioxide production\((\dot VCO_2 )\) and oxygen consumption\((\dot VO_2 )\) were measured continuously with a gas exchange monitor, and cardiac output and arterial and mixed venous blood samples were taken at the end of each 30-min period to assess CO2 removal and oxygen transport. Alveolar minute ventilation\(\dot V_A \) and the deadspace to tidal volume ratio (V D/V T) were calculated from the Bohr equation. Despite large changes inV T, arterial oxygenation (P aO2) and oxygen transport\((\dot DO_2 )\) were unchanged throughout the study. WhenV T was increased, physiologicalV D increased from 448±34 ml to 559±46 ml (mean±SE) in ARDS (P<0.001) and from 281±22 ml to 357±35 ml in CABG (P<0.05). With the smallV T,V D decreased to 357±22 ml in ARDS (P<0.01), and to 234±24 ml in CABG (P<0.05). In ARDS,V D/V T decreased from 0.57±0.03 to 0.55±0.03 (P<0.05) with the largeV T, and increased to 0.60±0.03 (P<0.01), whenV T was reduced. In CABG,V D/V T did not change significantly. ARDS patients had a higherP aCO2 than cardiac patients (P<0.001), and only minor changes inP aCO2 were observed (for ARDS and CABG respectively, baseline 5.9±0.3 kPa and 4.1±0.1 kPa, largeV T 5.7±0.3 kPa and 4.1±0.2 kPa, smallV T 6.2±0.3 kPa and 4.2±0.2 kPa;P<0.05).
Conclusions
Tidal volumes can be reduced to 6–8 ml/kg in ARDS patients without compromising oxygen transport, while adequate CO2 elimination can be maintained.
Article PDF
Similar content being viewed by others
References
MacNaughton PD, Evans TW (1992) Management of adult respiratory distress syndrome. Lancet 339: 469–472
Kolobow T, Moretti MP, Fumagalli R, Mascheroni D, Prato P, Chen V, Joris M (1987) Severe impairment of lung function induced by high peak airway pressure during mechanical ventilation. Am Rev Respir Dis 135: 312–315
Corbridge TC, Wood LDH, Crawford GP, Chudoba MJ, Janos J, Sznajder I (1990) Adverse effects of large tidal volume and low PEEP in canine acid aspiration. Am Rev Respir Dis 142: 311–315
Rouby J-J (1990) Pressure release ventilation. In: Vincent JL (ed) Update in intensive care and emergency medicine. Springer, Berlin, Heidelberg, New York, pp 185–191
Marcy TW, Marini JJ (1991) Inverse ratio ventilation in ARDS: rationale and implementation. Chest 100: 494–504
Snyder JV (1987) Ventilatory support: physiology and technique. In: Snyder JV, Pinsky MR (eds) Oxygen transport in the critically ill. Yearbook Medical Publishers, Chicago, pp 358–370
Kiiski R, Takala J, Kari A, Milic-Emili J (1992) The effect of tidal volume on gas exchange and oxygen transport in ARDS. Am Rev Respir Dis 146: 1131–1135
Murray JF, Matthay MA, Luce JM, Flick MR (1988) An expanded definition of the adult respiratory distress syndrome. Am Rev Respir Dis 138: 720–723
Kiiski R, Takala J, Eissa NT (1991) Measurement of alveolar ventilation and changes in dead space by indirect calorimetry: a clinical and laboratory validation. Crit Care Med 19: 1303–1309
Meriläinen PT (1987) Metabolic monitor. Int J Clin Monit Comp 4: 167–177
Takala J, Keinänen O, Väisänen P, Kari A (1989) Measurement of gas exchange in intensive care: laboratory and clinical validation of a new device. Crit Care Med 17: 1401–1047
Ronco JJ, Phang PT (1991) Validation of an indirect calorimeter to measure oxygen consumption in critically ill patients. J Crit Care 6: 36–41
Weissman C, Sardar A, Kemper M (1990) In-vitro evaluation of a compact metabolic measurement instrument. J Parenter Enteral Nutr 14: 216–221
Nunn JF (1987) Applied respiratory physiology. Butterworths, London, pp 249–250
Zar J (1984) Biostatistical analysis. Butterworths, London, pp 126–290
Marini JJ, Ravenscraft SA (1992) Mean airway pressure: physiologic determinants and clinical importance-Part 1: Physiologic determinants and measurements. Crit Care Med 20: 1461–1472
Leatherman JW, Lari RI, Iber C, Ney AL (1991) Tidal volume reduction in ARDS: effect on cardiac output and arterial oxygenation. Chest 99: 1227–1231
Cooper EA (1967) Physiological deadspace in passive ventilation. 2: Relationship with tidal volume, frequency, age, and minor upsets of respiratory health. Anaesthesia 22: 199–220
Severinghaus JW, Stupfel M (1957) Alveolar dead space as an index of distribution of blood flow in pulmonary capillaries. J Appl Physiol 10: 335–348
Darioli R, Perret C (1984) Mechanical controlled hypoventilation in status asthmaticus. Am Rev Respir Dis 129: 385–387
Hickling KG, Henderson SJ, Jackson R (1990) Low mortality associated with low volume, pressure limited ventilation with permissive hypercapnia in severe adult respiratory distress syndrome. Intensive Care Med 16: 372–377
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Kiiski, R., Kaitainen, S., Karppi, R. et al. Physiological effects of reduced tidal volume at constant minute ventilation and inspiratory flow rate in acute respiratory distress syndrome. Intensive Care Med 22, 192–198 (1996). https://doi.org/10.1007/BF01712236
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1007/BF01712236