Abstract
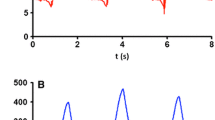
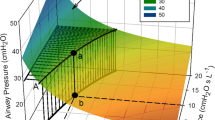
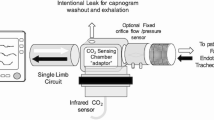
A new method for determination the static compliance of the respiratory system is described (“static compliance by automated single steps”-SCASS). In 12 ventilated patients pressure/volume (P/V) curves were determined by automated repetitive occlusion (6 s) at single volume steps and compared to the conventional syringe method (SM). All measurements were corrected for effects of temperature, humidity and pressure (THP). SM was found to be significantly influenced by intrapulmonary gas exchange causing an effective mean volume deficit of 217.4±65.7 ml (BTPS) at the end of the deflation. In contrast to that, the short duration of occlusion in SCASS minimize the gas exchange effects. The methodical differences between both methods result in overestimation of the inflation compliance in the uncorrected SM (SMuncorr: 83.4±12.6; SCASS: 76.0±11.9 ml/cmH2O.p<0.01) and underestimation of the deflation compliance resp. (SMuncorr: 58.3±7.5; SCASS: 79.1±15.0 ml/cmH2O.p<0.005). In contrast to the P/V curves by SM no significant hysteresis was found by SCASS. Gas exchange seems to be the main reason for the hysteresis. Even after correcting gas exchange and THP effects a significant hyseresis remained. The SCASS method avoids these problems and allows furthermore an accurate checking of leaks.
Article PDF
Similar content being viewed by others
References
Janney CD (1959) Super-syringe. Anesthesiology 20:709–711
Baum M, Benzer H, Blümel G, Bolcic J, Irsigler K, Tölle W (1971) Die Bedeutung der Oberflächenspannung in der Lunge beim experimentellen posttraumatischen Syndrom. Z Exp Chir 4:359–376
Benito S, Lemaire F, Mankikian B, Harf A (1985) Total respiratory compliance as a function of lung volume in patients with mechanical ventilation. Intensive Care Med 11:76–79
Falke KJ, Pontoppidan H, Kumar, Leith DE, Geffin B, Laver MB (1972) Ventilation with end-expiratory pressure in acute lung disease. Clin Invest 51:2315–2323
Matamis D, Lemaire F, Harf A, Brun-Buisson C, Ansquer JC, Atlan G (1984) Total respiratory pressure-volume curves in the adult respiratory distress syndrome. Chest 86:58–66
Suter PM, Fairly HB, Isenberg MD (1978) Effect of tidal volume and positive end-expiratory pressure on compliance during mechanical ventilation. Chest 73:158–162
Mankikian B, Lemaire F, Benito S, Brun-Buisson C, Harf A, Maillot JP, Becker J (1983) A new device for measurement of pulmonary pressure-volume curves in patients on mechanical ventilation. Crit Care Med 11:897–901
Gattinoni L, Mascheroni D, Basilico E, Foti G, Pesenti A, Avalli L (1987) Volume/pressure curve of total respiratory system in paralysed patients: artefacts and correction factors. Intensive Care Med 13:19–25
DallAva-Santucci J, Armagandis A, Brunet F, Dhainaut JF, Chelucci GL, Monsallier JF, Lockhart A (1988) Causes of error of presure-volume curves in paralyzed subjects. J Appl Physiol 64:42–49
Stokke T, Hensel I, Burchardi H (1981) Eine einfache Methode für die Bestimmung der funktionellen Residualkapazität während Beatmung. Anaesthesist 30:124–130
Burchardi H, Stokke T (1985) Pulmonary diffusing capacity for carbon monoxide by rebreathing in mechanically ventilated patients. Bull Eur Physiolpathol Respir 21:263–273
Pepe PE, Potkin PE, Reus DH, Hudson LD, Carrico CJ (1982) Clinical predictors of the adult respiratory distress syndrome. Am J Surg 144:124–129
Takala J, Keinänen O, Väisänen P, Kari A (1989) Measurement of gas exchange in intensive care: Laboratory and clinical validation of a new device. Crit Care Med 17:1041–1047
Bachofen H, Hildebrandt J (1971) Area analysis of pressure-volume hysteresis in mammalian lungs. J Appl Physiol 30:493–497
Wilcoxon F (1947) Individual comparisons by ranking methods. Biometrics 1:80–83
Suter PM, Fairly HB, Isenburg MD (1975) Optimum endexpiratory airway pressure in patients with acute pulmonary failure. N Engl J Med 292:284–289
Salmon RB, Primiano FP, Saidel GM, Niehwoehner DE (1981) Human lung pressure-volume relationships: alveolar collapse and airway closure. J Appl Physiol 51:353–362
Huang YC, Weinmann GG, Mitzner W (1988) Effect of tidal volume and frequency on the temporal fall in lung compliance. J Appl Physiol 65:2040–2045
Putensen C, Baum M, Koller W, Mutz G (1989) PEEP-Welle: Ein automatisiertes Verfahren zur bettseitigen Bestimmung der Volumen/Druck-Beziehung der Lunge beatmeter Patienten. Anaesthesist 38:214–219
Levy P, Similowski T, Corbeil C, Albala M, Pariente R, Milic-Emili J, Jonson B (1989) A method for studying the static volume-pressure curves of the respiratory system during mechanical ventilation. J Crit Care 4:83–89
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Sydow, M., Burchardi, H., Zinserling, J. et al. Improved determination of static compliance by automated single volume steps in ventilated patients. Intensive Care Med 17, 108–114 (1991). https://doi.org/10.1007/BF01691433
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1007/BF01691433