Abstract
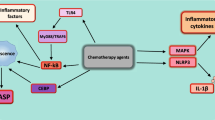
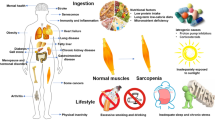
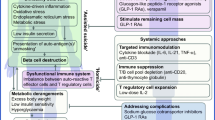
Patients with advanced cancer and cachexia typically demonstrate modestly increased rates of energy expenditure in the presence of diminished food intake due to anorexia and to gastrointestinal disturbances. Rates of glucose production by the liver, gluconeogenesis and glycolysis to lactate (Cori cycle) are increased, fat mobilisation and oxidation are accelerated. There is a redistribution of body proteins away from muscle towards visceral proteins, resulting in marked muscle protein loss. Cancer cachexia differs from simple starvation and demonstrates metabolic similarities to sepsis or polytrauma. The metabolic response in the patient with cancer is largely due to mediators released by the tumour or by the host; recently the role of cytokines such as tumour necrosis factor α (TNFα), interleukin-1 (IL-1) and-6 (IL-6) and interferon γ (INFγ) has been emphasized. Catabolic hormones such as glucocorticoids and adrenaline have also been implicated. Cytokines have the potential to reproduce experimentally the clinical syndrome of cancer cachexia. There is evidence of increased production of several of them in certain types of cancer. There are overlapping activities of the cytokines TNFα, IL-1, IFNγ and IL-6. The contribution of each of them to cancer cachexia remains unclear. Inhibition of cytokine activity using specific antibodies in cancer-bearing experimental animals demonstrated partial prevention of cachexia. A positive feedback between macrophage-derived IL-1 and tumour-derived IL-6 has been demonstrated recently in experimental cancer cachexia. Cytokines may support tumour growth by acting as growth factors.
Similar content being viewed by others
References
Aderka D, Fischer S, Levo Y, et al (1985) Cachectin/tumor necrosis factor production in human cancer. Lancet II:1190–1191
Akira S, Hirano T, Taga T, et al (1990) Biology of multifunctional cytokines: IL-6 and related molecules. FASEB J 4:2860–2867
American College of Physicians (1989) Parenteral nutrition in patients receiving cancer chemotherapy. Ann Intern Med 110:734–736
Arbeit JM, Lees DE, Corsey R, Brennan MF (1984) Resting energy expenditure in controls and cancer patients with localized and diffuse disease. Ann Surg 199:292–298
Axelrod L, Costa G (1980) Contribution of fat loss to weight loss in cancer. Nutr Cancer 2:81–83
Balkwill F, Osborne R, Burke F, et al (1987) Evidence for tumour necrosis factor/cachectin in cancer. Lancet II:1229–1231
Bodnar RJ, Pasternak GW, Mann PE et al (1989) Mediation of anorexia by human recombinant tumor necrosis factor through a peripheral action in the rat. Cancer Res 49:6280–6284
Bozzetti F, Pagnoni AM, Del Vecchio M (1980) Excessive caloric expenditure as a cause of malnutrition in patients with cancer. Surg Gynecol Obstet 150:229–234
Brennan MF (1977) Uncomplicated starvation versus cancer cachexia. Cancer Res 37:2359–2364
Carmichael MJ, Clague MB, Kier MJ, Johnston IDA (1980) Whole body protein turnover, synthesis and breakdown in patients with colorectal carcinoma. Br J Surg 67:736–769
Daly JM, Redmond HP, Gallagher H (1992) Perioperative nutrition in cancer patients. JPEN J Parenter Enteral Nutr 16 [Suppl 6]:100S-105S
Dempsey DT, Feurer ID, Knox LS, et al (1984) Energy expenditure in malnourished gastrointestinal cancer patients. Cancer 53:1265–1273
DeWys WD, Begg C, Lavin PT, et al (1980) Prognostic effect of weight loss prior to chemotherapy in cancer patients. Am J Med 69:491–497
Douglas RG, Shaw JHF (1990) Metabolic effects of cancer. Br J Surg 77:246–254
Eden E, Ekman L, Lindmark L, et al (1984) Whole-body tyrosine flux in relation to energy expenditure in weight-losing cancer patients. Metabolism 33:1020–1027
Fearon KCH, Hansell DT, Preston T, et al (1988) Influences of whole body protein turnover rate on resting energy expenditure in patients with cancer. Cancer Res 48:2590–2595
Gatanage T, Hwang C, Kohr W, et al (1990) Purification and characterization of an inhibitor (soluble tumor necrosis factor receptor) for tumor necrosis factor and lymphotoxin obtained from the serum ultrafiltrates of human cancer patients. Proc Natl Acad Sci USA 87:8781–8784
Gemlo BT, Palladino MA Jr, Jaffe HS, et al (1988) Circulating cytokines in patients with metastatic cancer treated with recombinant interleukin-2 and lymphokine-activated killer cells. Cancer Res 48:5864–5867
Hansell DT, Davies JWL, Burns HJG (1986) The relationship between resting energy expenditure and weight loss in benign and malignant disease. Ann Surg 203:240–245
Heber D, Cheblowski RT, Ishibushi DE, et al (1982) Abnormalities in glucose and protein metabolism in non-cachectic lung cancer patients. Cancer Res 42:4815–4819
Hyltander A, Körner U, Ludholm KG (1993) Evaluation of mechanisms behind elevated energy expenditure in cancer patients with solid tumours. Eur J Clin Invest 23:46–52
Jablons DM, McIntosh JK, Mule JJ, et al (1989) Induction of interferon β2/interleukin-6 (IL-6) by cytokine administration and detection of circulating IL-6 in the tumor-bearing state. Ann NY Acad Sci 577:157–166
Kien CL, Camitta BM (1987) Close association of accelerated rates of whole body protein turnover (synthesis and breakdown) and energy expenditure in children with newly diagnosed acute lymphatic leukaemia. JPEN J Parenter Enteral Nutr 11:129–134
Koea JB, Shaw JHF (1992) The effect of tumor bulk on the metabolic response to cancer. Ann Surg 3:282–288
Legaspi A, Jeevanandam M, Starnes HF, Brennan MF (1987) Whole body lipid and energy metabolism in the cancer patient. Metabolism 10:958–963
Long CL, Spenser JL, Kinney JM, Geiger JW (1971) Carbohydrate metabolism in normal man and effect of glucose infusion. J Appl Physiol 31:102–109
Lundholm K, Bylund AC, Holm J, et al (1976) Skeletal muscle metabolism in patients with malignant tumours. Eur J Cancer 12:465–473
McNamara MJ, Alexander R, Norton JA (1992) Cytokines and their role in the pathophysiology of cancer cachexia. JPEN J Parenter Enteral Nutr 16:50S-55S
Meguid MM, Debonis D, Meguid V, et al (1983) Nutritional support in cancer. Lancet II:230–231
Moldawer LL, Rogy MA, Lowry SF (1992) The role of cytokines in cancer cachexia. JPEN J Parenter Enteral Nutr 16:3S-49S
Rose D, Horowitz GD, Jeevanandam M, Brennan MF, Shives GT, Lowry SF (1983) Whole body protein kinetics during acute starvation and intravenous refeeding in normal man. Fed Proc 42:1070
Shaw JHF, Wolfe RR (1987) Fatty acids and glycerol kinetics in septic patients and in patients with gastrointestinal cancer: the response to glucose infusion and parenteral feeding. Ann Surg 205:368–376
Shaw JHF, Humberstone DM, Wolfe RR (1988) Energy and protein metabolism in sarcoma patients. Ann Surg 207:283–289
Spinas GA, Bloesch D, Keller U, Zimmerli W, Cammisuli S (1991) Pretreatment with ibubrofen augments circulating tumor necrosis factor-alpha, interleukin-6, and elastase during acute endotoxinemia. J Infect Dis 163:89–95
Strassmann G, Fong M, Kenney JS, et al (1992) Evidence for the involvement of interleukin-6 in experimental cancer cachexia. J Clin Invest 89:1681–1684
Uehara A, Sekiya C, Takasugi Y, et al (1989) Anorexia induced by interleukin-1: involvement of corticotropin-releasing factor. Am J Physiol 257:R613-R617
Vlassara H, Spiegel RJ, Doval DS, et al (1986) Reduced plasma lipoprotein lipase activity in patients with malignancy associated weight loss. Horm Metab Res 18:698–703
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Keller, U. Pathophysiology of cancer cachexia. Support Care Cancer 1, 290–294 (1993). https://doi.org/10.1007/BF00364965
Issue Date:
DOI: https://doi.org/10.1007/BF00364965