Abstract
Three-dimensional (3D) hydrogel models play a crucial role in tissue engineering for promoting tissue regeneration. A biomimetic microchannel network system in the 3D hydrogel model is necessary for optimal cellular function. This report describes the preparation of a biomimetic hydrogel scaffold with an internal microchannel network, using electrospinning techniques and the sacrificial template method for 3D cell culture. Microchannels and cavities were created within the gelatin methacryloyl (GelMA) hydrogel by sacrificing polyvinyl alcohol (PVA) electrospun fibers (>10 µm), resulting in the creation of microvessel-like channels. Mechanical characterizations, swelling properties, and biodegradation analysis were conducted to investigate the feasibility of a biomimetic microchannel network hydrogel scaffold for 3D cell culture applications. Compared to pure GelMA hydrogel, the hydrogel with microchannels promoted cell proliferation, adhesion, and endothelial tube formation. Moreover, the results confirmed that the biomimetic microchannel network scaffold had a major impact on the distribution and arrangement of human umbilical vein endothelial cells (HUVECs) and can enable the formation of artificial microvasculature by the culture of HUVECs and cell media perfusion.
摘要
目 的
三维(3D)水凝胶模型在组织工程中起到了促进组织再生的关键作用. 三维水凝胶模型中的仿生微通道网络系统是实现最佳细胞功能的必要条件. 本文旨在研究利用电纺技术和牺牲模板法制备具有内部微通道网络的仿生水凝胶支架, 用于三维内皮细胞培养形成功能性人工微血管.
创新点
1. 首次利用静电纺丝技术成功制备直径>10 μm的纤维材料, 作为形成微通道网络的牺牲材料; 2. 通过反复挤压的方式, 在高浓度甲基丙烯酰化明胶(GelMA)水凝胶内成功创建了微通道和空腔, 从而创建了微血管样通道; 3. 成功在微通道腔内形成内皮细胞单层, 并研究了3D水凝胶支架表面和支架内对人脐静脉内皮细胞(HUVECs)的活性、 增殖、 形态发生和血管再生的影响.
方 法
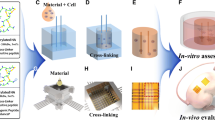
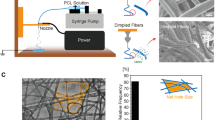
1. 以难挥发的去离子水和易挥发的六氟异丙醇(HFIP)为溶剂, 通过优化配比及电纺条件, 使其静电纺直径更大的纤维, 用于形成微通道结构的牺牲材料(图1); 2. 合成并研究高浓度的纯GelMA水凝胶和支架的理化性能和生物相容性. 通过力学性能、溶胀性能和降解性能等表征和对比, 筛选出最优性能的支架(图2~5); 3. 通过对支架表面和支架内的内皮细胞培养, 量化对比内皮细胞的形态发生以及细胞核铺展, 研究支架对人工微血管形成的影响(图6~8).
结 论
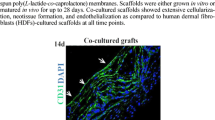
1. 在室温条件下, 聚乙烯醇(PVA)纤维能够被聚丁二酸丁二醇酯(PBS)溶液快速溶解; 2. 通过力学性能、溶胀性能和降解性能等测试, 与纯GelMA水凝胶相比, 含微通道网络的仿生GelMA水凝胶力学性能有所下降. 虽然微通道网络的存在降低了其各种性能, 但仍有利于HUVECs的生长和增殖, 且满足组织再生的周期, 特别适用于三维细胞培养和组织工程应用; 3. CCK-8毒性测试和对细胞的活-死染色结果显示, 三种支架均具有良好的生物相容性. 在培养7 d后, 材料表面细胞相互连接形成管状结构, HUVECs在浓度为25%的支架比15%和20%的支架细胞数量显著增加, 且有更明显的铺展和管状结构. 这表明其状态良好, 支持了含内部结构的GelMA水凝胶支架的生物相容性, 且此支架可作为生物医学领域的3D细胞培养, 应证了上述所提到的内含微结构的水凝胶亦适用于细胞附着与增殖. 4. 经过对细胞的4′,6-二脒基-2-苯基吲哚(DAPI)和微丝染色, 结果显示培养3 d后, 在支架通道内形成了稳定的内皮单细胞层, 细胞核分布均匀且沿着孔道主轴方向排布, 微丝清晰可见, 大多倾向于轴向分布. 其次, 微孔道通过接触引导影响HUVECs的细胞行为与形态, 从而促进HUVECs形成微血管. 发现微通道管腔3D微环境通过接触引导促进融合的内皮细胞单层的形成, 进一步表明了此支架作为体外微血管的再生的适用性. 最后, 通过量化对比, 微通道加速了微血管的再生.
Similar content being viewed by others
References
Atia L, Bi DP, Sharma Y, et al., 2018. Geometric constraints during epithelial jamming. Nature Physics, 14(6):613–620. https://doi.org/10.1038/s41567-018-0089-9
Aubin H, Nichol JW, Hutson CB, et al., 2010. Directed 3D cell alignment and elongation in microengineered hydrogels. Biomaterials, 31(27):6941–6951. https://doi.org/10.1016/j.biomaterials.2010.05.056
Bacakova L, Pajorova J, Bacakova M, et al., 2019. Versatile application of nanocellulose: from industry to skin tissue engineering and wound healing. Nanomaterials, 9(2):164. https://doi.org/10.3390/nano9020164
Bae H, Ahari AF, Shin H, et al., 2011. Cell-laden microengineered pullulan methacrylate hydrogels promote cell proliferation and 3D cluster formation. Soft Matter, 7(5):1903–1911. https://doi.org/10.1039/C0SM00697A
Bertassoni LE, Cecconi M, Manoharan V, et al., 2014. Hydrogel bioprinted microchannel networks for vascularization of tissue engineering constructs. Lab on a Chip, 14(13):2202–2211. https://doi.org/10.1039/c4lc00030g
Boakye MAD, Rijal NP, Adhikari U, et al., 2015. Fabrication and characterization of electrospun PCL-MgO-keratin-based composite nanofibers for biomedical applications. Materials, 8(7):4080–4095. https://doi.org/10.3390/ma8074080
Buchwald P, 2009. FEM-based oxygen consumption and cell viability models for avascular pancreatic islets. Theoretical Biology and Medical Modelling, 6:5. https://doi.org/10.1186/1742-4682-6-5
Bupphathong S, Quiroz C, Huang W, et al., 2022. Gelatin methacrylate hydrogel for tissue engineering applications–a review on material modifications. Pharmaceuticals, 15(2):171. https://doi.org/10.3390/ph15020171
Chamorro CI, Zeiai S, Reinfeldt Engberg G, et al., 2016. Minced tissue in compressed collagen: a cell-containing biotransplant for single-staged reconstructive repair. Journal of Visualized Experiments, 108:53061. https://doi.org/10.3791/53061
Chang WG, Niklason LE, 2017. A short discourse on vascular tissue engineering. NPJ Regenerative Medicine, 2:7. https://doi.org/10.1038/s41536-017-0011-6
Chen YC, Lin RZ, Qi H, et al., 2012. Functional human vascular network generated in photocrosslinkable gelatin methacrylate hydrogels. Advanced Functional Materials, 22(10):2027–2039. https://doi.org/10.1002/adfm.201101662
Cicha I, Detsch R, Singh R, et al., 2017. Biofabrication of vessel grafts based on natural hydrogels. Current Opinion in Biomedical Engineering, 2:83–89. https://doi.org/10.1016/j.cobme.2017.05.003
Daly AC, Pitacco P, Nulty J, et al., 2018. 3D printed microchannel networks to direct vascularisation during endochondral bone repair. Biomaterials, 162:34–46. https://doi.org/10.1016/j.biomaterials.2018.01.057
Davoodi E, Montazerian H, Zhianmanesh M, et al., 2022. Template-enabled biofabrication of thick 3D tissues with patterned perfusable macrochannels. Advanced Healthcare Materials, 11(7):2102123. https://doi.org/10.1002/adhm.202102123
Dogan E, Bhusal A, Cecen B, et al., 2020. 3D printing metamaterials towards tissue engineering. Applied Materials Today, 20:100752. https://doi.org/10.1016/j.apmt.2020.100752
Duval K, Grover H, Han LH, et al., 2017. Modeling physiological events in 2D vs. 3D cell culture. Physiology, 32(4):266–277. https://doi.org/10.1152/physiol.00036.2016
Edwards A, Jarvis D, Hopkins T, et al., 2015. Poly(ε-caprolactone)/keratin-based composite nanofibers for biomedical applications. Journal of Biomedical Materials Research Part B: Applied Biomaterials, 103(1):21–30. https://doi.org/10.1002/jbm.b.33172
Eke G, Mangir N, Hasirci N, et al., 2017. Development of a UV crosslinked biodegradable hydrogel containing adipose derived stem cells to promote vascularization for skin wounds and tissue engineering. Biomaterials, 129:188–198. https://doi.org/10.1016/j.biomaterials.2017.03.021
Enrico A, Voulgaris D, Östmans R, et al., 2022. 3D microvascularized tissue models by laser-based cavitation molding of collagen. Advanced Materials, 34(11):2109823. https://doi.org/10.1002/adma.202109823
Gao X, Ma SX, Xing XT, et al., 2022. Microvessels derived from hiPSCs are a novel source for angiogenesis and tissue regeneration. Journal of Tissue Engineering, 13:1–21. https://doi.org/10.1177/20417314221143240
Groebe K, Mueller-Klieser W, 1991. Distributions of oxygen, nutrient, and metabolic waste concentrations in multicellular spheroids and their dependence on spheroid parameters. European Biophysics Journal, 19(4):169–181. https://doi.org/10.1007/BF00196343
Gryka MC, Comi TJ, Forsyth RA, et al., 2019. Controlled dissolution of freeform 3D printed carbohydrate glass scaffolds in hydrogels using a hydrophobic spray coating. Additive Manufacturing, 26:193–201. https://doi.org/10.1016/j.addma.2018.12.014
Helary C, Bataille I, Abed A, et al., 2010. Concentrated collagen hydrogels as dermal substitutes. Biomaterials, 31(3):481–490. https://doi.org/10.1016/j.biomaterials.2009.09.073
Helary C, Abed A, Mosser G, et al., 2011. Synthesis and in vivo integration of improved concentrated collagen hydrogels. Journal of Tissue Engineering and Regenerative Medicine, 5(3):248–252. https://doi.org/10.1002/term.326
Helary C, Zarka M, Giraud-Guille MM, 2012. Fibroblasts within concentrated collagen hydrogels favour chronic skin wound healing. Journal of Tissue Engineering and Regenerative Medicine, 6(3):225–237. https://doi.org/10.1002/term.420
Hinton TJ, Jallerat Q, Palchesko RN, et al., 2015. Three-dimensional printing of complex biological structures by freeform reversible embedding of suspended hydrogels. Science Advances, 1(9):e1500758. https://doi.org/10.1126/sciadv.1500758
Hu KK, Shi H, Zhu J, et al., 2010. Compressed collagen gel as the scaffold for skin engineering. Biomedical Microdevices, 12(4):627–635. https://doi.org/10.1007/s10544-010-9415-4
Kenar H, Ozdogan CY, Dumlu C, et al., 2019. Microfibrous scaffolds from poly(L-lactide-co-ε-caprolactone) blended with xeno-free collagen/hyaluronic acid for improvement of vascularization in tissue engineering applications. Materials Science and Engineering: C, 97:31–44. https://doi.org/10.1016/j.msec.2018.12.011
Kim MS, Kim G, 2014. Three-dimensional electrospun polycaprolactone (PCL)/alginate hybrid composite scaffolds. Carbohydrate Polymers, 114:213–221. https://doi.org/10.1016/j.carbpol.2014.08.008
Kolesky DB, Truby RL, Gladman AS, et al., 2014. 3D bio-printing of vascularized, heterogeneous cell-laden tissue constructs. Advanced Materials, 26(19):3124–3130. https://doi.org/10.1002/adma.201305506
Kolesky DB, Homan KA, Skylar-Scott MA, et al., 2016. Three-dimensional bioprinting of thick vascularized tissues. Proceedings of the National Academy of Sciences of the United States of America, 113(12):3179–3184. https://doi.org/10.1073/pnas.1521342113
Kumar M, Sharma V, 2021. Additive manufacturing techniques for the fabrication of tissue engineering scaffolds: a review. Rapid Prototyping Journal, 27(6):1230–1272. https://doi.org/10.1108/rpj-01-2021-0011
Kurakula M, Koteswara Rao GSN, 2020. Moving polyvinyl pyrrolidone electrospun nanofibers and bioprinted scaffolds toward multidisciplinary biomedical applications. European Polymer Journal, 136:109919. https://doi.org/10.1016/j.eurpolymj.2020.109919
Li Y, Wang J, Wang Y, et al., 2021. Advanced electrospun hydrogel fibers for wound healing. Composites Part B: Engineering, 223:109101. https://doi.org/10.1016/j.compositesb.2021.109101
Liaw CY, Guvendiren M, 2017. Current and emerging applications of 3D printing in medicine. Biofabrication, 9(2):024102. https://doi.org/10.1088/1758-5090/aa7279
Lin RZ, Chen YC, Moreno-Luna R, et al., 2013. Transdermal regulation of vascular network bioengineering using a photopolymerizable methacrylated gelatin hydrogel. Biomaterials, 34(28):6785–6796. https://doi.org/10.1016/j.biomaterials.2013.05.060
Lovett ML, Nieland TJF, Dingle YTL, et al., 2020. Innovations in 3D tissue models of human brain physiology and diseases. Advanced Functional Materials, 30(44):1909146. https://doi.org/10.1002/adfm.201909146
Miller JS, Stevens KR, Yang MT, et al., 2012. Rapid casting of patterned vascular networks for perfusable engineered three-dimensional tissues. Nature Materials, 11(9):768–774. https://doi.org/10.1038/NMAT3357
Mota C, Puppi D, Chiellini F, et al., 2015. Additive manufacturing techniques for the production of tissue engineering constructs. Journal of Tissue Engineering and Regenerative Medicine, 9(3):174–190. https://doi.org/10.1002/term.1635
Moulisová V, Gonzalez-García C, Cantini M, et al., 2017. Engineered microenvironments for synergistic VEGF-integrin signalling during vascularization. Biomaterials, 126:61–74. https://doi.org/10.1016/j.biomaterials.2017.02.024
Nazarnezhad S, Baino F, Kim HW, et al., 2020. Electrospun nanofibers for improved angiogenesis: promises for tissue engineering applications. Nanomaterials, 10(8):1609. https://doi.org/10.3390/nano10081609
Nichol JW, Koshy ST, Bae H, et al., 2010. Cell-laden micro-engineered gelatin methacrylate hydrogels. Biomaterials, 31(21):5536–5544. https://doi.org/10.1016/j.biomaterials.2010.03.064
Pien N, Pezzoli D, van Hoorick J, et al., 2021. Development of photo-crosslinkable collagen hydrogel building blocks for vascular tissue engineering applications: a superior alternative to methacrylated gelatin?. Materials Science and Engineering: C, 130:112460. https://doi.org/10.1016/j.msec.2021.112460
Rademakers T, Horvath JM, van Blitterswijk CA, et al., 2019. Oxygen and nutrient delivery in tissue engineering: approaches to graft vascularization. Journal of Tissue Engineering and Regenerative Medicine, 13(10):1815–1829. https://doi.org/10.1002/term.2932
Rnjak-Kovacina J, Wray LS, Golinski JM, et al., 2014. Arrayed hollow channels in silk-based scaffolds provide functional outcomes for engineering critically sized tissue constructs. Advanced Functional Materials, 24(15):2188–2196. https://doi.org/10.1002/adfm.201302901
Roh TT, Chen Y, Paul HT, et al., 2019. 3D bioengineered tissue model of the large intestine to study inflammatory bowel disease. Biomaterials, 225:119517. https://doi.org/10.1016/j.biomaterials.2019.119517
Rouwkema J, Rivron NC, van Blitterswijk CA, 2008. Vascularization in tissue engineering. Trends in Biotechnology, 26(8):434–441. https://doi.org/10.1016/j.tibtech.2008.04.009
Ryma M, Genç H, Nadernezhad A, et al., 2022. A print-and-fiise strategy for sacrificial filaments enables biomimetically structured perfusable microvascular networks with functional endothelium inside 3D hydrogels. Advanced Materials, 34(28):2200653. https://doi.org/10.1002/adma.202200653
Shiwarski DJ, Hudson AR, Tashman JW, et al., 2021. Emergence of fresh 3D printing as a platform for advanced tissue biofabrication. APL Bioengineering, 5(1):010904. https://doi.org/10.1063/5.0032777
Song XY, Yu YL, Leng Y, et al., 2022. Expanding tubular microvessels on stiff substrates with endothelial cells and pericytes from the same adult tissue. Journal of Tissue Engineering, 13:1–17. https://doi.org/10.1177/20417314221125310
Therriault D, White SR, Lewis JA, 2003. Chaotic mixing in three-dimensional microvascular networks fabricated by direct-write assembly. Nature Materials, 2(4):265–271. https://doi.org/10.1038/nmat863
Toriello M, Afsari M, Shon HK, et al., 2020. Progress on the fabrication and application of electrospun nanofiber composites. Membranes, 10(9):204. https://doi.org/10.3390/membranes10090204
Tsai YL, Theato P, Huang CF, et al., 2020. A 3D-printable, glucose-sensitive and thermoresponsive hydrogel as sacrificial materials for constructs with vascular-like channels. Applied Materials Today, 20:100778. https://doi.org/10.1016/j.apmt.2020.100778
Türker E, Yildiz ÜH, Arslan Yildiz A, 2019. Biomimetic hybrid scaffold consisting of co-electrospun collagen and PLLCL for 3D cell culture. International Journal of Biological Macromolecules, 139:1054–1062. https://doi.org/10.1016/j.ijbiomac.2019.08.082
Uppuluri VNVA, Thukani Sathanantham S, Bhimavarapu SK, et al., 2022. Polymeric hydrogel scaffolds: skin tissue engineering and regeneration. Advanced Pharmaceutical Bulletin, 12(3):437–448. https://doi.org/10.34172/apb.2022.069
van den Bulcke AI, Bogdanov B, de Rooze N, et al., 2000. Structural and rheological properties of methacrylamide modified gelatin hydrogels. Biomacromolecules, 1(1):31–38. https://doi.org/10.1021/bm990017d
Wan XZ, Liu PC, Jin XX, et al., 2018. Electrospun PCL/keratin/auNPs mats with the catalytic generation of nitric oxide for potential of vascular tissue engineering. Journal of Biomedical Materials Research Part A, 106(12):3239–3247. https://doi.org/10.1002/jbm.a.36521
Wang Y, Kankala RK, Ou CW, et al., 2022. Advances in hydrogel-based vascularized tissues for tissue repair and drug screening. Bioactive Materials, 9:198–220. https://doi.org/10.1016/j.bioactmat.2021.07.005
Wittmer CR, Hu X, Gauthier PC, et al., 2011. Production, structure and in vitro degradation of electrospun honeybee silk nanofibers. Acta Biomaterialia, 7(10):3789–3795. https://doi.org/10.1016/j.actbio.2011.06.001
Xia P, Luo YX, 2022. Vascularization in tissue engineering: the architecture cues of pores in scaffolds. Journal of Biomedical Materials Research Part B: Applied Biomaterials, 110(5):1206–1214. https://doi.org/10.1002/jbm.b.34979
Xiao SN, Zhao TF, Wang JK, et al., 2019. Gelatin methacrylate (GelMA)-based hydrogels for cell transplantation: an effective strategy for tissue engineering. Stem Cell Reviews and Reports, 15(5):664–679. https://doi.org/10.1007/s12015-019-09893-4
Xu F, Dawson C, Lamb M, et al., 2022. Hydrogels for tissue engineering: addressing key design needs toward clinical translation. Frontiers in Bioengineering and Biotechnology, 10:849831. https://doi.org/10.3389/fbioe.2022.849831
Yamamura N, Sudo R, Ikeda M, et al., 2007. Effects of the mechanical properties of collagen gel on the in vitro formation of microvessel networks by endothelial cells. Tissue Engineering, 13(7):1443–1453. https://doi.org/10.1089/ten.2006.0333
Zhang YY, Chen H, Li JS, 2022. Recent advances on gelatin methacrylate hydrogels with controlled microstructures for tissue engineering. International Journal of Biological Macromolecules, 221:91–107. https://doi.org/10.1016/j.ijbiomac.2022.08.171
Zhao DK, Xu HQ, Yin J, et al., 2022. Inkjet 3D bioprinting for tissue engineering and pharmaceutics. Journal of Zhejiang University-SCIENCE A (Applied Physics & Engineering), 23(12):955–973. https://doi.org/10.1631/2023.A2200569
Zhao X, Lang Q, Yildirimer L, et al., 2016. Photocrosslinkable gelatin hydrogel for epidermal tissue engineering. Advanced Healthcare Materials, 5(1):108–118. https://doi.org/10.1002/adhm.201500005
Zhou Y, Fan YC, Chen Z, et al., 2022. Catechol functionalized ink system and thrombin-free fibrin gel for fabricating cellular constructs with mechanical support and inner micro channels. Biofabrication, 14(1):015004. https://doi.org/10.1088/1758-5090/ac2ef8
Zia AW, Liu R, Wu X, 2022. Structural design and mechanical performance of composite vascular grafts. Bio-Design and Manufacturing, 5(4):757–785. https://doi.org/10.1007/s42242-022-00201-7
Zohar B, Blinder Y, Mooney DJ, et al., 2018. Flow-induced vascular network formation and maturation in three-dimensional engineered tissue. ACS Biomaterials Science & Engineering, 4(4):1265–1271.
Acknowledgments
This work is supported by the National Natural Science Foundation of China (No. 31870934) and the Natural Science Foundation for Young Scientists of Shanxi Province (No. 202103021223100), China.
Author information
Authors and Affiliations
Contributions
Haoyu SUN, Yang LIU, Meiwen AN, Meiling WEN, and Li WANG designed the research. Haoyu SUN, Haiyang MA, Tian HOU, Wenjie TANG, and Qing YU processed the corresponding data. Haoyu SUN wrote the first draft of the manuscript. Meiling WEN helped to organize the manuscript. Meiwen AN revised and edited the final version.
Corresponding authors
Ethics declarations
Haoyu SUN, Haiyang MA, Li WANG, Yang LIU, Tian HOU, Wenjie TANG, Qing YU, Meiwen AN, and Meiling WEN declare that they have no conflict of interest.
Additional information
Electronic supplementary materials
Figs. S1–S5
Electronic Supplementary Materials
11582_2024_531_MOESM1_ESM.pdf
Biomimetic microchannel network with functional endothelium formed by sacrificial electrospun fibers inside 3D gelatin methacryloyl (GelMA) hydrogel models
Rights and permissions
About this article
Cite this article
Sun, H., Ma, H., Wang, L. et al. Biomimetic microchannel network with functional endothelium formed by sacrificial electrospun fibers inside 3D gelatin methacryloyl (GelMA) hydrogel models. J. Zhejiang Univ. Sci. A 25, 79–96 (2024). https://doi.org/10.1631/jzus.A23D0045
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1631/jzus.A23D0045